Over 80 percent of American women use hormonal contraception at some point in their lives. Many women who have taken birth control pills, or used other hormonally-based birth control methods such as implants, patches, vaginal rings, and hormone-emitting IUDs are probably familiar with the common side effects like fatigue, loss of libido, mood effects, headaches and breast pain. However, many women may not be aware that taking almost any form of hormonal contraception increases their risk of developing blood clots, a condition that can range in severity from asymptomatic to fatal.
The risk of developing a blood clot varies depending on the type of hormonal birth control used. One might assume that the newer methods would be safer, but in fact, they are more dangerous. The newer birth control pills (formulations containing drospirenone, desogestrel, gestodene and dienogest) confer a higher risk of blood clots than older formulations (containing norethindrone acetate or levonorgestrel, as well as the newer norgestimate). And the risk from patches and vaginal rings are the highest of all. It seems that regulatory agencies are willing to lower safety for the sake of user convenience, something that most women using hormonal contraception probably would not agree with, if they knew they were being put at risk.
The overall risk is considered low, with about 1 in 10,000 reproductive age women per year developing a blood clot. However, the older birth control pills increase the risk by about four-fold, and the newer birth control pills by five to seven-fold compared to non-users of hormonal contraception. There has been a substantial increase in the incidence of blood clots for the period of 2001 to 2009, compared to the years prior, likely because of the increase in use of newer hormonal birth control pills and the vaginal ring (Nuvaring). And because approximately 20 million American women use hormonal contraception, these relatively small risks translate into significant numbers of cases each year.
Every woman who is using hormonal contraception deserves to know accurately what the risks are, in order to make an informed choice of method of contraception, yet these risks are not often being communicated by doctors. And considering that taking any form of hormonal birth control at all raises the risk of developing a blood clot, every woman on hormonal contraception should know what the warning signs are, and seek medical help if they experience those signs or symptoms. Knowing these warning signs could save your life. Described below are signs of blood clots in various locations in the body.
Blood Clots In Legs, Arms, and Lungs
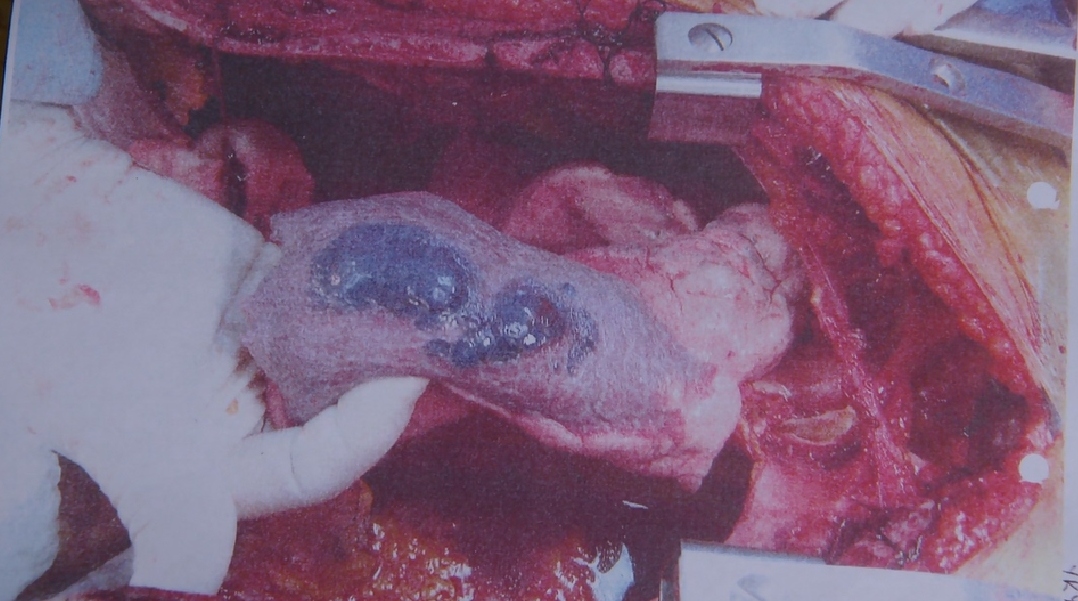
Blood clots can develop in any vein but most commonly develop in the leg, and sometimes in the arm. This type of blood clot is called a venous thromboembolism (VTE). These clots can break off from the spot where they initially form in the body, and travel to the lungs, causing a pulmonary embolism (PE), which is fatal in about 10 percent of cases within the first hour, and 30 percent of cases subsequently. Sometimes the VTE leading to the pulmonary embolism was asymptomatic or undiagnosed, and PE is the first indication of the presence of a blood clot. Even pulmonary embolism is often misdiagnosed at first.
Signs of VTE include pain or tenderness only in one leg or arm, swelling and/or red or blue discoloration of the affected limb or an area of the limb, and the leg or arm may be warm to the touch. Signs of a PE include sudden shortness of breath, chest pain that is sharp or stabbing and may get worse with deep breathing, rapid heartbeat, and cough (sometimes with bloody mucous). For information about how VTE and PE are diagnosed, see How is DVT Diagnosed? and How is PE Diagnosed?.
Blood Clots In the Veins of the Brain
Cerebral venous thrombosis (CVT), which is a type of stroke, is caused by blood clots in the veins of the brain. This condition is even more under recognized than DVT and PE, and comprises about one percent of all strokes. Using oral contraceptives has been shown to increase the risk of CVT up to 22-fold. This study is on the older side, performed before more widespread use of newer birth control pills, so the risk is likely even higher. In the past, this condition was fatal much more often, but now the diagnosis has been improving, and the mortality in various studies ranges from 5 to 30 percent. About 15 percent of patients who survive can have continued neurological impairment. CVT can be diagnosed using a combination of clinical signs and symptoms, and imaging such as MRI.
Signs and symptoms of CVT can vary depending on where the clot is in the brain. Headache is a common symptom, sometimes accompanied by nausea and vomiting. Seizures can also occur. In addition, neurological problems can be present, such as: paralysis or weakness on one side of the body, decreased vision on one side, difficulty speaking, or dizziness.
Blood Clots In Arteries
Like in veins, blood clots can form in almost any artery in the body. And similar to venous blood clots, clots that initially formed in one artery can break off and travel to arteries within almost any organ in the body. A blood clot in an artery in the brain causes a stroke (just like a blood clot in a vein in the brain), and a blood clot in an artery in the heart causes a heart attack. Hormonal contraception also increases the risk of these types of blood clots. In some cases larger strokes are preceded by smaller strokes, called transient ischemic attacks (TIA)—this occurs when a blood vessel is blocked temporarily by a blood clot. The incidence of stroke has increased significantly, especially in young people, from 1995 to 2008.
Symptoms of strokes caused by a blood clot in an artery are similar to those described above for CVT. Early treatment of a stroke results in significantly better outcomes; therefore the American Heart and Stroke Association has developed the following acronym to help people recognize the early warning signs: F.A.S.T.
- F: Face drooping
- A: Arm weakness
- S: Speech difficulty
- T: Time to call 911.
Warning signs of a heart attack in women include:
- Chest pain—can feel like uncomfortable pressure, squeezing, fullness or pain in the center of the chest.
- Pain or discomfort in one or both arms, back, neck, jaw or stomach.
- Shortness of breath with or without chest discomfort.
- Nausea, light-headedness, or breaking out in a cold sweat.
It should be noted, that women may experience the signs of a heart attack differently than men and diagnosing heart attacks in women is sometimes more complicated requiring great persistence on the part of the patient and the family. An example of this can be found here.
Other Factors That Increase Risk
An individual’s risk of getting a blood clot depends on a combination of genetic factors, acquired conditions, and environmental/lifestyle factors. Although many women may be familiar with the oft-cited risk factors of being overweight, smoking, and being over age 35, many women might be surprised to realize that some of the seemingly innocuous factors described below, or undiagnosed genetic conditions, can combine to increase the risk substantially.
Genetic Factors
Certain inherited conditions, known as inherited thrombophilias, can increase the risk of developing a blood clot. Many people with these inherited conditions have no signs or symptoms of a blood clotting disorder until an environmental or acquired risk factor or factors comes into the picture (such as a hormonal contraceptive), at which point their risk of developing a blood clot increases substantially. These inherited thrombophilias include antithrombin deficiency, protein C deficiency, protein S deficiency, Prothrombin (factor II) mutation, factor V Leiden mutation and hyperhomocysteinemia (which can be caused by MTHFR mutation). The effect of the increased risks from hormonal contraceptives and inherited thrombophilias is synergistic, meaning the risk is much larger than the risk of the two added together; for example, in hormonal contraceptive users carrying a factor V Leiden mutation, the risk of a blood clot is increased 35 fold. Inherited thrombophilias can be detected by genetic testing, but are not routinely screened for. More information about inherited thrombophilias can be found on the National Blood Clot Alliance website.
Acquired Conditions
The acquired condition that is most commonly associated with an increased risk for blood clotting is an autoimmune condition called anti-phospholipid syndrome (and less commonly anti-cardiolipin antibodies, or anti-B2 glycoprotein 1 antibodies). These antibodies can occur on their own, in the absence of other autoimmune diseases, or they can occur secondary to autoimmune diseases such as lupus. These conditions can cause other symptoms in addition to blood clots, such as miscarriage and migraine. Cancer, especially metastatic cancer, is also a recognized risk factor for thrombosis. Hyperhomocysteinemia can also be an acquired condition due to nutritional deficiencies, some chronic illnesses, and medications. Chronic inflammatory conditions such as Crohn’s disease also increases the risk of blood clots.
Environmental or Lifestyle Factors
Certain lifestyle factors are also known to increase the risk of blood clots, including:
- Obesity
- Immobility–prolonged inactivity, for example, bed rest, or taking long trips by plan or car
- Smoking
- Non-steroidal anti-inflammatory medications such as Advil
- Other medications such as certain psychiatric drugs
- Intense exercise
- Certain types of surgery
- Pregnancy
- Hormonal contraceptives
The risk of developing a blood clot also increases with increasing age.
It must be stressed that one does not need to have a genetic or acquired risk factor to develop a blood clot, or even to have a fatal blood clot. Following are just a few of many stories of young, healthy women who were seriously affected or died from blood clots while on hormonal contraception.
- Deadly Blood Clots from the NuvaRing: Erika’s Legacy
- Julia West Ross–Age 29
- Brittany Malone
- Megan Henry–Age 25–Pulmonary Embolisms
- Brain Grenade: Hormonal Contraceptives, Migraine, and Stroke
These women unfortunately did not realize that their choice of birth control was putting them at increased risk. For these women, knowing that they were at increased risk, and knowing the warning signs of a blood clot, could have saved their lives. That is why we are urging all women to become aware of these warning signs, investigate your personal risk, make smart, informed choices of birth control methods, and seek medical attention immediately if you are experiencing signs of a blood clot.
In Memory
This article was inspired by and written in memory of Karen Langhart, who tragically took her own life four years after her young, healthy, vibrant daughter Erika, died suddenly from bilateral massive pulmonary embolisms caused by the Nuvaring. Since Erika’s death, Karen had worked tirelessly to ensure that other families would not suffer the tragedy that hers did.
Hormones Matter will be covering this important topic in more detail in the coming months, so please follow this website, or follow us on Facebook and Twitter at and @HormonesMatter. If you have experience with contraceptive induced blood clots and would like to contribute a personal story or research article, please consider writing for Hormones Matter.












Smart Women’s Choice is the healthy alternative to hormone-containing birth control methods. A vaginal gel, it contains no hormones and no germicides. It works by immobilizing the sperm. If sperm cannot move from the vagina into the oviducts, the only place where fertilization can occur, then there can be no fertilization, hence no pregnancy. This method is 100% effective and produces ZERO side effects. It has been on the market for 20 months now and no pregnancies have been reported. People who purchased it once, purchased it again; clearly, they were satisfied. It is easy and pleasant to use, providing lubrication as well.
Safe and effective SWC is truly ‘Women’s Lib.’ Please tell us how YOU liked it! at ‘comments’ at
We appreciate it!