In 2009, the US Preventive Services Task Force (USPSTF) released a statement in which they recommended against mammograms for women aged 40 to 49, which contrasted with the recommendation made seven years prior that women begin screening at the age of 40.
What’s a Mammogram?
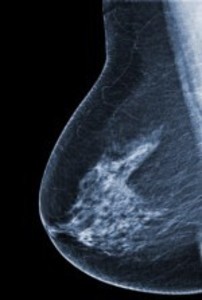
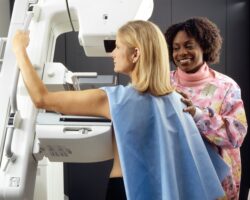
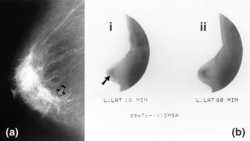
Mammograms are x-ray examinations that help doctors determine if there are any changes to the breast tissue that could not be felt during clinical breast examinations. It’s normal for breasts to change, but doctors specifically look for changes that may indicate the patient has breast cancer.
Doctors use mammograms to try to determine if lumps in the breasts are cancerous and compare findings to previous mammograms to identify physical changes in the breast.
Breast Changes May Be Hormonal
Of course, it’s important to note that changes in the breasts are not necessarily cancerous, and can actually be hormonal. The University of Maryland Medical Center refers to this as “fibrocystic change,” in which the breasts become lumpy and painful right before one’s menstrual period, a result of hormones being produced in the ovaries.
More than 50% of women experience fibrocystic changes during their menstrual cycle, which means a majority of women experience physical changes in their breasts regularly.
As a woman, it is helpful to be aware of cyclical changes that the breasts undergo, and if possible, keep track. Hormonal changes in the breast don’t usually begin until a woman is 30, symptoms may be impacted by hormonal drugs (such as hormone replacement therapy or birth control pills), and fibrocystic changes usually stop after menopause.
Understanding natural changes to the breasts can supplement a doctor’s knowledge during mammography screenings. Such knowledge may even help a woman better plan breast examinations according to her menstrual cycle, so doctors can identify new changes as opposed to recurring ones.
So Why Delay Mammography?
Even in 2002, the USPSTF stated there was little evidence that women benefited from screening for breast cancer sooner than 50 years of age. The report noted that negative consequences of mammograms include “anxiety, discomfort and cost associated with positive test results, many of which are false positive, and the diagnostic procedures they generate.”
In addition, since the breast is exposed to small doses of radiation during mammography, the repeated exposure can increase a woman’s risk of cancer. The risk of getting cancer is small, however, and the benefits of mammography usually outweigh the risks. But the USPSTF started to question whether the benefits outweigh the risks for women in their 40s.
Though mammograms can benefit those with breast cancer, the incidence of breast cancer in women in their 40s is much lower than it is for women in their 50s. Since most women are not likely to have breast cancer in their 40s, women in this age group are more likely to suffer adverse effects from the examination.
The USPSTF stated the decision to have a mammogram should be an individual one that takes into account family medical history and other pertinent information.
Decline in Mammograms among 40-year-old Women
The impact of these recommendations can be seen in recent data recorded by Mayo Clinic, which shows there have been 54,000 fewer mammograms among women in their 40s, or a 5.72% decline.
It’s difficult to determine whether this decrease in mammography among women in their 40s is good or not, as some experts still recommend screening as early as 40, including Mayo Clinic, which follows the recommendations given by the American Cancer Society.
Now What?
Women should identify any regular physical breast changes, continue to conduct self breast examinations along with clinical breast examinations, and openly discuss this information, as well as any possible genetic predisposition to breast cancer, with their doctors. Through discourse, women can decide what the best course of action is for their specific needs.








Hi Elena,
Do you have any thoughts on thermography as an alternative to mamography? Here is a really interesting podcast on the topic – http://fearlessparent.org/radio-blog-in-praise-of-thermography-episode-41/
Regards,
Lisa
I am definitely an advocate of regular mammogram checks after the age of 40. I had a baseline done at 40 and at 43 had another routine mammogram. They saw enough variation to warrant a second mammogram, biopsy, diagnosis Ductal carcinoma in situ (DCIS), lumpectomy and now awaiting start of localize radiation. DCIS is almost always detected through mammogram and not through breast examination. Ofcourse with no family history of cancer it was a shock to be diagnosed with cancer but without the mammogram i would have this mass growing of me.
It’s difficult when USPSTF states the benefits are smaller for women in their 40s.. But if you can prevent cancer, it seems to be worth the risk. They’ll probably collect more data and just reverse their decision again. I’m glad your mammogram prevented a more serious situation – thanks for your input.