Hundreds of articles about the harmful effects of fluoroquinolone antibiotics (Cipro/ciprofloxacin, Levaquin/levofloxacin, Avelox/moxifloxacin and Floxin/ofloxacin) have been published in medical and scientific journals, yet most of the articles have been ignored by the medical community and downplayed by the FDA. I can only surmise that the ignorance around the dangers of fluoroquinolones is because they are used as antibiotics and antibiotics are “supposed” to be safe and only damage bacteria, while leaving human cells unscathed. Or maybe it is because of the constant repetition of the baseless statement that fluoroquinolones have an “excellent record of safety and tolerance;” a statement that is only true if delayed reactions, tolerance thresholds and epigenetic effects are not taken into consideration.
Regardless of the motivations of those who are ignoring how destructive fluoroquinolones are, valuable information about the safety (or rather, the dangers) of fluoroquinolones as a class of drugs, have been ignored. Warnings about the toxicity of fluoroquinolones have been noted in journal article after journal article, yet they are still some of the most popular antibiotics prescribed.
Caution, prudence and thoughtfulness should be exercised when prescribing drugs that are as dangerous and destructive as fluoroquinolones. Fluoroquinolones are chemo drugs that are being mis-prescribed as antibiotics. Before filling a prescription for a fluoroquinolone to treat a sinus infection, or to use prophylactically for traveler’s diarrhea, or putting in your child’s ear to treat an ear infection, I encourage you to note the cellular destruction done by fluoroquinolones. Neither the FDA nor the average doctor is properly warning patients about the dangers of fluoroquinolones. Unfortunately, it is up to patients to inform themselves and gain proper warnings about the consequences of these dangerous drugs.
Fluoroquinolones Damage DNA
Back in 1992, when fluoroquinolones were first gaining popularity, Scientists raised concerns about their safety in an article published by the Proceedings of the National Academy of Sciences of the United States:
“the interaction (of fluoroquinolones) with DNA is still of great concern because of the possible long-term genotoxicity of quinolone compounds, which are increasingly adopted as first-choice antibiotics for the treatment of many infections, and because it addresses the real mechanism of action of this class of molecules.”
Fluoroquinolones are topoisomerase interrupters, meaning that their mechanism of action is described as, “The bactericidal action of ciprofloxacin results from inhibition of the enzymes topoisomerase II (DNA gyrase) and topoisomerase IV (both Type II topoisomerases), which are required for bacterial DNA replication, transcription, repair, and recombination.” (Cipro warning label).
Very little, if any, concern over the possible genotoxic effects of fluoroquinolones were expressed to the public as they gained popularity and uses were expanded in the early 1990s. The warnings and concerns expressed by the scientists quoted were ignored.
It is noted in Molecular Pharmacology, “Delayed Cytotocicity and Cleavage of Mitochondrial DNA in Ciprofloxacin Treated Mammalian Cells” that fluoroquinolones “cause a selective loss of mitochondrial DNA (mtDNA)” and “The loss in mtDNA was associated with a delayed loss in mitochondrial function.” Additionally, it is stated that “ciprofloxacin induces reversible double-stranded breaks in nuclear DNA.” Studies have shown that both mitochondrial and nuclear DNA is adversely affected by fluoroquinolones, yet those studies have not gained traction in the medical community and have effectively been ignored.
The intergenerational effects of depleting DNA with fluoroquinolones is unknown at this time (I surmise that this is because these studies have been ignored, intergenerational studies are difficult to do, and funding for them is hard to come by). However, it is known that, “a number of human mitochondrial genetic diseases that are clinically discreet are being diagnosed at unexpected rates” (source). Additionally, in an article published in Nature in 2013 entitled, “Topoisomerases facilitate transcription of long genes linked to autism” it was noted that, “Our data suggest that chemicals or genetic mutations that impair topoisomerases, and possibly other components of the transcription elongation machinery that interface with topoisomerases, have the potential to profoundly affect the expression of long ASD (autism spectrum disorder) candidate genes.” Fluoroquinolones are topoisomerase interrupting chemicals.
Thus far, neither the increase in mitochondrial genetic diseases nor the link between topoisomerase interrupting drugs and autism have been acknowledged by the medical community, the FDA or the general public.
Fluoroquinolones Damage Mitochondria
The deleterious effects of fluoroquinolones on mitochondria have been noted repeatedly in journal articles, and even by the FDA.
In Science Translational Medicine, “Bactericidal Antibiotics Induce Mitochondrial Dysfunction and Oxidative Damage in Mammalian Cells,” it is noted that bactericidal antibiotics, including ciprofloxacin, a fluoroquinolone, “damage mammalian tissues by triggering mitochondrial release of reactive oxygen species (ROS).” Even the FDA acknowledges that fluoroquinolones cause mitochondrial damage. In their April 27, 2013 Pharmacovigilance Review, “Disabling Peripheral Neuropathy Associated with Systemic Fluoroquinolone Exposure,” the FDA notes that the mechanism for action through which fluoroquinolones induce peripheral neuropathy is mitochondrial toxicity. The report says:
“Ciprofloxacin has been found to affect mammalian topoisomerase II, especially in mitochondria. In vitro studies in drug-treated mammalian cells found that nalidixic acid and ciprofloxacin cause a loss of mitochondrial DNA (mtDNA), resulting in a decrease of mitochondrial respiration and an arrest in cell growth. Further analysis found protein-linked double-stranded DNA breaks in the mtDNA from ciprofloxacin-treated cells, suggesting that ciprofloxacin was targeting topoisomerase II activity in the mitochondria.”
Fluoroquinolones are very, very bad for mitochondria. As the engines of our cells, healthy mitochondria are very necessary for healthy cells. Mitochondrial dysfunction is connected with many chronic diseases, including autism, CFS/ME, fibromyalgia, Alzheimer’s Disease, Parkinson’s Disease,multiple sclerosis, etc.
Fluoroquinolones Alter Neurons
Fluoroquinolones downgrade GABA-A receptors and can lead to a variety of CNS related symptoms of fluoroquinolone toxicity such as “dizziness, confusion, tremors, hallucinations, depression, and, rarely, psychotic reactions have progressed to suicidal ideations/thoughts and self-injurious behavior such as attempted or completed suicide,” as well as “nervousness, agitation, insomnia, anxiety, nightmares or paranoia” (Cipro warning label).
It was concluded in an article in The Journal of Neurophysiology in 1991 that, “in the presence of an anti-inflammatory agent, the quinolone antibiotics decrease the affinity of GABAA receptors, the result being induction of epileptogenic neurotoxicities.”
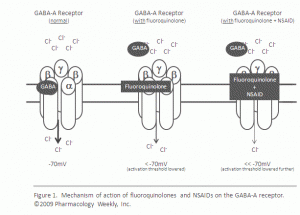
An article in Pharmacology Weekly that was published in 2009 notes that fluoroquinolones “modulate the activity of the gamma-aminobutyric acid (GABA)-A receptor” leading to the CNS side-effects of fluoroquinolones that include “tremors, restlessness, anxiety, confusion, paranoia, insomnia, etc.” and that “the presence of an NSAID or NSAID metabolite can significantly augment this effect and result in an even greater inhibition of GABA-A receptor activity” and lead to seizures, in addition to the other CNS effects listed. But, in 2015, people still are not systematically warned about the possibility of fluoroquinolone induced “nervousness, agitation, insomnia, anxiety, nightmares or paranoia” and NSAIDs are still prescribed concurrently with fluoroquinolones, despite documentation that the combination of fluoroquinolones and NSAIDs downgrade important neurotransmitters.
Though the symptoms that arise when GABA-A receptors are downgraded are noted on the warning labels for fluoroquinolones, nowhere on the warning label does it say that these effects can be long-lasting, or even permanent.
Generally, the effects of fluoroquinolones on neurotransmitters are ignored, and ensuing anxiety, insomnia and psychiatric illnesses are assumed to have nothing to do with the antibiotics that were prescribed for a sinus or urinary tract infection. The research and the warnings, have been ignored.
Fluoroquinolones Damage Cells
In The Journal of Medical Microbiology it was noted that:
“Dougherty & Saukkonen (1985) showed that inhibition of DNA synthesis by nalidixic acid, a DNA gyrase inhibitor, results in morphological changes consistent with a loss of membrane integrity and leakage of intracellular components. Similar results were presented by Wickens et al. (2000), who noticed a decrease of both membrane integrity and membrane potential after exposure of E. coli to CIP. One of the proposed explanations of this finding is that, as a result of processes induced by inhibition of DNA replication, cells lose their capacity to synthesize necessary components and to maintain the proper membrane structure (Dougherty & Saukkonen, 1985).”
Naladixic acid is the root component of all fluoroquinolones.
In case it needs to be said, cellular membrane integrity and keeping intracellular components inside cells, are important. It is important for cells as a whole, and for organelles within cells such as mitochondria. As the importance of the microbiome is being uncovered, the importance of the bacteria in our guts maintaining cellular integrity is slowly being realized as well.
Fluoroquinolones are Dangerous Drugs
The FDA warning label for Cipro/ciprofloxacin is 43 pages long. The serious and severe adverse effects listed on the warning label are due to the cellular destruction done by Cipro. Other fluoroquinolones (Levaquin and Avelox are popular) have similar safety/danger profiles.
Though no antibiotics are without consequence, the cellular destruction done by fluoroquinolones makes them far more dangerous than other antibiotics. Fluoroquinolones should be categorized as chemo drugs along with all other topoisomerase interrupters. Please be wary and cautious with fluoroquinolones, and don’t use them unless it is absolutely necessary.
Information about Fluoroquinolone Toxicity
Information about the author, and adverse reactions to fluoroquinolone antibiotics (Cipro/ciprofloxacin, Levaquin/levofloxacin, Avelox/moxifloxacin and Floxin/ofloxacin) can be found on Lisa Bloomquist’s site, www.floxiehope.com.
Participate in Research
Hormones MatterTM is conducting research on the side effects and adverse events associated with the fluoroquinolone antibiotics, Cipro, Levaquin, Avelox and others: The Fluoroquinolone Antibiotics Side Effects Study. The study is anonymous, takes 20-30 minutes to complete and is open to anyone who has used a fluoroquinolone antibiotic. Please complete the study and help us understand the scope of fluoroquinolone reactions.
Hormones MatterTM conducts other crowdsourced surveys on medication reactions. To take one of our other surveys, click here.
To sign up for our newsletter and receive weekly updates on the latest research news, click here.
What Else Can I Do To Help?
Hormones MatterTM is completely unfunded at this juncture and we rely entirely on crowdsourcing and volunteers to conduct the research and produce quality health education materials for the public. If you’d like help us improve healthcare with better data, get involved. Become an advocate, spread the word about our site, our research and our mission. Suggest a study. Share a study. Join our team. Write for us. Partner with us. Help us grow.
To support Hormones Matter and our research projects – Crowdfund Us.









Keep up the “good work” you do Lisa as it will eventually pay off and all these bad drugs will be taken off the market.
http://marcthavenot.com/donations/
Marc Thavenot was poisoned by a dangerous antibiotic called levaquin which damaged his immune and nervous system. He then was unable to fight off infections including Lyme Disease. He is unable to function or work and needs help to recover his health.
Hi, Lisa
I could not access the website on Pharmacology Weekly, published in 2009, that says that fluoroquinolones “modulate the activity of the gamma-aminobutyric acid (GABA)-A receptor” leading to the CNS side-effects of fluoroquinolones that include “tremors, restlessness, anxiety, confusion, paranoia, insomnia, etc.” and that “the presence of an NSAID or NSAID metabolite can significantly augment this effect and result in an even greater inhibition of GABA-A receptor activity”.
The link is not working.
Do you know how I can find it?
Hi Ana,
Unfortunately, the article went away when Pharmacology Weekly was sold or taken over by the folks who now have that url. I have never used the way back machine, but you may be able to access it with that, or some other web site that stores old urls. Luckily, I copied and pasted a decent portion of the article into the post https://floxiehope.com/2014/10/29/why-nsaids-suck-for-floxies-and-probably-everyone-else-too/. Here’s the excerpt (which was about half the total article):
What role do NSAIDs have in the predisposition for developing seizures while also taking a fluoroquinolone antibiotic?
Interestingly, the presence of an NSAID or NSAID metabolite can significantly augment this effect and result in an even greater inhibition of GABA-A receptor activity. It is, however, important to note that majority of this effect is related to an NSAID that is only available outside of the United States called fenbufen (Afiancen®, Bifene®, Cincopal®, Cinopal®, Lederfen®, Reugast®).9-11,14 It appears that the metabolite of fenbufen, 4-biphenylacetic acid (BPAA), augments the ability of the fluoroquinolone to inhibit GABA binding to the GABA-A receptor.9-11,14 It is important to note that BPPA itself does not inhibit GABA binding to the GABA-A receptor, but rather when BPAA and the fluoroquinolone come in close proximity they interact in such a way that it results in the ability of the fluoroquinolone antibiotic to inhibit GABA binding to a greater degree than by itself. It is possible that the interaction between a fluoroquinolone antibiotic and BPAA causes some other biologic effect that influences the activity of the GABA-A receptor. In fact, there is some evidence that some fluoroquinolones (mainly enoxacin and norfloxacin) can increase the activity of nuclear activator protein 1 (AP-1) DNA- and cyclic AMP responsive elements (CRE)-binding activities in both the hippocampus and cerebral cortex.14 It has been suggested that increased activity of AP-1 mediated gene expression is important for activity-dependent plasticity in these regions of the brain and thus contribute to the increased risk for seizures.14 Even though fenbufen has been the main NSAID implicated in this adverse drug reaction, other NSAIDs such as indomethacin, ketoprofen, naproxen, ibuprofen have also been shown to augment fluoroquinolone induced GABA-A receptor inhibition in animal studies.9
While the data most strongly implicate certain fluoroquinolone antibiotics and NSAIDs, CNS side effects and seizures have been reported with many of the fluoroquinolones, including the ones currently on the market.1-5 This is the reason that the product package inserts for the fluoroquinolone antibiotics not only list the above as potential side effects, but also describe the drug interaction with NSAIDs.1-5 As such, until further evidence suggests otherwise, it would be prudent, especially from a medical legal perspective, for healthcare providers to avoid the use of fluoroquinolones with or without NSAIDs in patients who are at greater risk for seizures (e.g., history of epilepsy, severe cerebral arteriosclerosis) or those with a lower seizure threshold (e.g., patients on medications known to do this, renal dysfunction).
I believe I was floxed, my question is that my dentist insist that I use fluoride toothpaste and that after a dental cleaning that I have fluoride application, is the dental fluoride ok, I am terrified to have a major relapse as I have been suffering for over 3 years know, may seem like a dumb question but I would really like to know
Thanks so much for all your work
Hi interesting site.
What is it specifically about these drugs that causes the issue that they share in common?
In other terms, what is it in the chemical structure that poses the risk?
Okay so they can damage mitochondria and other cells, but what is it specifically that does this (which is unique to these compounds) and what is the mode of action?
My interest for knowing is to find potentially dangerous traits across pharmaceutical drugs more generally that may not just be isolated to these drugs. If we can spot dangers in certain drugs then we may be able to premptively spot dangers with others.
Thank you for your time
Hi Nick,
Thank you very much for your interest in this matter! I suspect that the answer lies in the mechanism of action that is noted on the fluoroquinolone warning labels – “The bactericidal action of ciprofloxacin results from inhibition of the enzymes topoisomerase II (DNA gyrase) and topoisomerase IV (both Type II topoisomerases), which are required for bacterial DNA replication, transcription, repair, and recombination.” Fluoroquinolones, and other drugs with a quinoline core – like mefloquine and a few others – likely do the same kind of damage to mitochondrial DNA as what they do to bacterial DNA.
It’s also possible that the root of the problem is the fluorine, and that all fluorinated drugs (and other sources of fluorine in our environment) are leading to chronic illness.
This post goes over some other possibilities – http://www.hormonesmatter.com/fluoroquinolone-toxicity/.
I wish I had more certain answers for you. Having a dozen damage mechanisms is, unfortunately, less helpful than having one damage mechanism. At the end of the day, these are dangerous drugs that need to be studied more.
Regards,
Lisa Bloomquist