Studies abound showing how the endogenous estrogens, estradiol mainly, improve memory and other cognitive functions. New research demonstrates there is an even more basic connection between the female reproductive organs – the uterus and ovaries – and the brain. The monthly menstrual cycle may control iron levels in body and also in the brain. Women who have a hysterectomy before reaching natural menopause may be at higher risk of neurodegenerative diseases such as Azheimer’s and Parkinson’s due to the increased peripheral and brain iron levels post hysterectomy.
Iron and Brain Health
Iron is an essential element for health. Both iron deficiency and excess are associated with brain pathology. In the developing brain, too little iron causes neurological impairment with significant cognitive and neuromuscular deficits. As we age, iron accumulation in the brain is also problematic and linked to neurodegenertive disorders. In part because women menstruate, they have naturally lower levels of peripheral (body) iron than men. Researchers believe that the menstrual flushing of excess iron may be in part responsible for delaying the brain iron accumulation that has been linked to early Alzheimer’s and Parkinson’s in men.
In a study published in the journal Neurobiology of Aging, researchers investigated what effect premenopausal hysterectomy had on brain iron levels. From a sample (n = 93) of healthy older, male and female volunteers, ages 47-80 years, researchers used a specialized MRI to image brain iron levels.
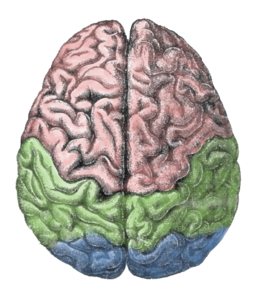
What they found was quite interesting. Women who had hysterectomy before reaching natural menopause had significantly higher iron levels in the white matter of the frontal cortex compared to women who reached menopause naturally. The hysterectomy group, also had higher iron levels in the other brain regions tested but those differences were not large enough to reach statistical significance. Brain iron levels in the hysterectomy group were similar to those of men, who have naturally higher iron levels in the brain and who often succumb to the neurodegenerative diseases at a much earlier age. The researchers speculated that the observed white matter iron accumulation could be a precusor to the grey matter iron accumulation observed in neurodegenerative diseases such as Alzheimer’s and Parkinson’s.
Brain Basics
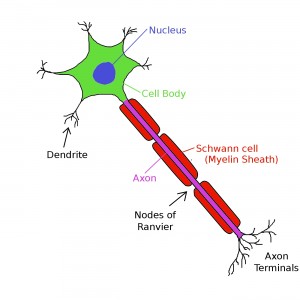
White matter in the brain consists of the oligodendrocytes – a type of cell that forms what is called the myelin sheath. Myelin is the insulation that protects the axons of the neuron (in the brain) or nerve (in the body) to allow rapid conduction or messaging across the brain or to the body. Myelin is like the plastic coating around the electrical wiring in your house. If the coating is too thick, conduction is blocked. If the coating is frayed or too thin, electrical sparks fly everywhere. Iron is a critical component of healthy myelin, too much or too little impairs signal conduction – brain messaging.
Grey matter, on the other hand, is where the unmyelinated portion of neurons – the dendrites and cell bodies – are located. These are brain regions responsible for learning, memory, emotion, sensory perception and motor control. Cells in this part of the brain rely on chemical signaling to translate information. After the dendrite receives and the cell body translates a message, it sends the signal down the myelinated axon to its target. Iron accumulation, either in the white or grey matter would impact brain function. Iron accumulation specifically in the frontal white matter region would impact all higher order cognitive function.
What This Means
The research is still in its early stages. An observed connection between menstrual blood loss and peripheral or brain iron stores though apparent, may not represent the total picture. It is quite likely that hormones associated with reproductive health, altered by the hysterectomy, also play a role in iron regulation. Initial research connecting the hyperandrogenic and metabolically dysregulated state of women with PCOS is associated with increased iron stores, as is general and cancer related inflammation, and genetics. Nevertheless, this study speaks to the critical need for more research about the long-term consequences of hysterectomy. Reproductive hormones regulate more than just reproduction. Removing the organs that synthesize these hormones has health consequences far beyond reproduction. It’s high time we begin addressing this.
If you have had a hysterectomy, be sure to take The Hysterectomy Survey.
Author’s note: I would like to thank David Wiseman Ph.D., M.R.Pharm.S.
Founder, International Adhesions Society (IAS) for introducing me to this exciting new research.










I was a victim of this surgery as well. I was lied to by the doctors and verbally berated for not agreeing with the surgery. They would not discharge me from the hospital until I had the surgery. It’s a long story. Is there any hope for me? The acupuncture did stave off the side effects but everything closed with the pandemic. Now all the hospital can say is “sorry and good bye”. Is there any hope because they removed my ovaries too. There has to be something.
My name is Oksana Sams and I had my Abdominal Hysterectomy in May 05, 2005 when I was 38 years old.
It changed my life forever after that I had to go though my process of divorced.
I was diagnosed with endometrioses and my left ovary was enlarge to 7cm, a Physician Assistant Natasha in family physician office of Marina Raikhel, MD in city of Lomita, CA 90717 send me to take a blood test CA-125 it came more then normal 35 units per milimitr Natasha told me the result so bad it could be a cancer and referred me to Louse H. Connolly, MD, Practice Limited Gynecology, who suggested me to do a hysterectomy. They both convinced me there was nothing could help me not to have the pain during my periods I had an awful pain each time during my period. I asked the Gynecologist to get a second opinion about my surgery she send me to Fikret Atamdede, MD, associate Professor Harbor/ UCLA Medical Center which confirmed the hysterectomy.
The day before surgery May 04, 2005 when I visit Doctor Louse Connolly in her offce, she called to the Professor Atamdede in my presents and started to argue with him about my health insurance payment for my surgery and told him that she would be primary recipient of the insurance money than she asked me not to cancel the surgery.
After she finished talking on the phone with him she apologized to me for this conversation I was shocked and understood that she did not consider me being present and understanding them. All that time those Doctors thought I do not understand very good English that why they used my confusion and just cheat me with the surgery. They used me to get my insurance money not for my health benefits at all just split money.
They did not want to treat me with alternative medications when I asked Doctor Connolly she told me it was so expensive medication. After my hysterectomy I had to stay in Torrance Memorial Hospital for 3 days only and in a bed for more then two weeks because my low belly was cut and was stitched. Each times I tried to stand up it hurted me badly.
The doctor Connolly visited me at Torrance Memorial Hospital one time only within three days my staying there when she took the staples of my belly.
In the same room where I was there is an African-American lady who had her surgery as well but her doctor visited her every day and make her feel better to prescribe her different electric massages her feet and her back.
In September 2005 I moved to Ukraine.
While living in Ukraine I visited my Gynecologist and specialists as well. They were shocked when they found about my surgery. They told me that in Ukraine doctors do not recommend to do surgery but a treatment of the endometrioses in my situation and Los Angeles Gynecologists made me disabled woman. I feel like that now. After I came to my city in Ukraine,I went as soon as possible to see an Ukrainian Gynecologist she started to treat my cervical erosion after my surgery ( before it become cervical cancer) for 6 months that was the result from the Hysterectomy which neither Doctor Connolly or Professor Atamdede form Los Angeles did not mentioned about it.
Thanks to my Ukrainian Gynocologist I felt her support and her attitude in opposite of the Gynocologist in USA who did not want to see me after surgery at all.
But now I think it would be better not to agreed to that surgery that destroyed my life and I feel my soul was taken out of me.
So I do not know if I can live with that in my mind. It psychological trauma for rest of my life as well as a physical damage for my body. Besides my hysterectomy they removed my left ovary. The removal the ovaries in women is the biological equivalent of castration in males and is a form of sterilization. Removal of the uterus renders the patient unable to bear children and has surgical risks as well as long-term effects, so the surgery is normally recommended when other treatment options are not available or have failed. The both doctors did not recommend me other treatment.
Removal of the uterus and ovaries at a young age (early forties and younger) may increase the risk of a heart attack, stroke, and (even when ovaries are not removed) the chances of experiencing an earlier menopause. Hysterectomy has also been associated with urinary problems, such as increased frequency of urination, incontinence, fistula, and urinary tract infections; sexual function problems, such as decrease in sexual sensations and lack of lubrication; depression or psychological stress (stemming from feelings associated with losing reproductive organs); hormone deficiencies (which may be caused by removal of the ovaries), or a decrease in blood supply to the ovaries. Normal ovarian function “protects” women from atherosclerosis which is a risk factor for sudden heart death.
I cannot get married any more and have a family. I did not realized how it could impact on my life. They just killed a women in me.
Do these studies make a distinction between full hysterectomies and supra-hysterectomies?
No, but recent studies published suggest that removal of the ovaries is detrimental to mitochondrial functioning.
http://www.hormonesmatter.com/hormones-hysterectomy-aging-brain/
http://www.hormonesmatter.com/lupron-estradiol-mitochondria-adverse-reactions/
http://www.hormonesmatter.com/tank-estradiol-lose-metabolic-flexibility-lupron-oophorectomy/
Thank you, Dr. Marrs, for this article! It makes sense that messing with “mother nature” alters normal physiology. Sadly though most in the medical profession choose to dismiss or ignore the harm of female organ removal.