This is the story of my wife’s decline in health following the surgical reconstruction of a torn left hip labrum. I am writing this for my wife because her health has declined so significantly over the past 5 years that she has become medically homebound and bedridden. She is too weak and unbalanced to walk, has become intolerant to light, to foods (she can only eat 10 different foods without having a reaction), to smells, and is in constant and extreme pain. She has also developed severe skin reactions that are destroying her lower extremities. After seeing more than 50 doctors with little to offer, we are posting her story here in the hope that someone will be able to help.
Post-surgical Development of Complex Regional Pain Syndrome
Megan is a 44 year old female who was athletic, very active, and physically fit her whole life. Prior to left hip labral reconstruction on 6/20/2017, Megan did not take a single prescription. She led a very healthy lifestyle, in which she enjoyed playing tennis, doing yoga, swimming, biking, snowboarding, running, hiking, camping, and backpacking regularly. Postoperatively, she developed left foot edema, redness, allodynia, hyperalgesia, diminished proprioception, and balance, and burning pain in her left foot. Despite diligently participating in physical therapy 3 times weekly, she was not able to fade off of her crutches. She continued to have severe lower extremity pain and was diagnosed with Complex Reginal Pain Syndrome (CRPS) on 11/1/2017. In December 2017, Megan participated in an FDA-approved clinical trial of neridronic acid (bisphosphonate) infusions for CRPS without relief. She developed flu-like symptoms, which got progressively worse after each infusion, but eventually resolved.
Skin Manifestations
By January 2018, Megan started to develop lesions on her left foot. Initially, they were pinpoint to large flat lesions. Some of them were extremely itchy. Overtime, the lesions and rash spread up her ankle and shin on her left leg.
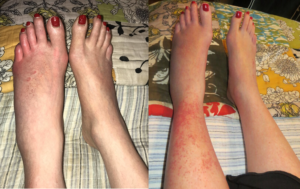
Over the next several months, while still attending physical therapy, Megan noted a lack of hair growth on her lower left leg, temperature discrepancies, in which the left foot was subjectively hot but objectively cooler than the right foot, blood pooling, and skin discoloration in her feet (dark red/purple) when standing, nail changes, and bilateral lower leg flushing following a warm shower. During this time, food sensitivities were also first observed – initially with beef and shrimp.
More Diagnoses But Little Help
In October 2018, Megan was evaluated by a physician at Brown Medical School, who is an expert with CRPS. He confirmed the diagnosis of CRPS (bilateral lower extremities) and in his provisional assessment of Megan, also diagnosed her with bilateral common peroneal neuralgia and bilateral foot drop. He also suspected Megan has mast cell activation syndrome (MCAS), orthostatic intolerance/dysautonomia (POTS), and hypermobile type Ehlers-Danlos Syndrome (hEDS) and was able to delineate which symptoms were consistent with CRPS and which were not. He did not attribute the blood pooling, the footdrop, flushing, lesions, rash, food intolerances and allergic-like reactions, dermographia, and other skin manifestations to CRPS. He recommended she be evaluated by another physician at the Steadman Clinic to assess for common peroneal nerve entrapment.
In October 2018, the Steadman doctor concluded that Megan did not have a common peroneal nerve entrapment. Instead, he noted irritations in the saphenous and obturator nerve distributions and diagnosed her with “bad luck”. He recommended Megan have an MRI of her lower back to ensure there is no central based pathology contributing to her bilateral symptoms. A lumbar MRI was conducted, which yielded no significant results.
Catastrophic Progression of Symptoms
All symptoms started after an orthopedic surgery on the left hip. Prior to the surgery on June 20th, 2017, there is no significant medical history. She had a clean bill of health prior to surgery – no prescriptions were taken, no known allergies. In April 2018, we learned the hospital that performed the surgery was not properly sterilizing the surgical instruments and operating rooms between surgeries, which resulted in numerous infections, injuries, and illnesses, per an investigation.
New symptoms, which have appeared in the last 24-36 months include: heavy sweating, bladder incontinence (especially after eating and some while sleeping), sudden urge to urinate, sudden urge to drink water, decreased vision, extremely dizzy, and feeling lightheaded when standing. Brain fog has been getting progressively worse. Food reactions and extreme sensitivity to stimuli have been getting progressively worse and more frequent. Menstrual cycles have been getting progressively worse – worst symptoms and highest pain are observed during the cycle. Food reactivity is more likely and worse while menstruating.
Current treatment approaches have not resulted in any lasting or significant improvement. Despite intervention, symptoms have gotten progressively worse. Megan has been medically homebound since 2019.
Large patches of skin peel, turn white, and flake off ankles, shins, and legs below the knees. Clusters of tiny “pin prick” lesions appear on tops of both feet and on legs, including thighs. There is a lace-like pattern of purple/brownish skin discoloration above the knees (Livedo Reticularis), which continues up the thighs. The lesions, rash, and discoloration have been progressing up both legs. Skin/tissue on feet appear purple, blue, red, pink, orange, discolored, and shiny in places. There is no hair growth on both legs below the knees. Toenails on both feet are thick, crumbly, extremely brittle, and yellowish/brown. There is little to no growth of toenails.
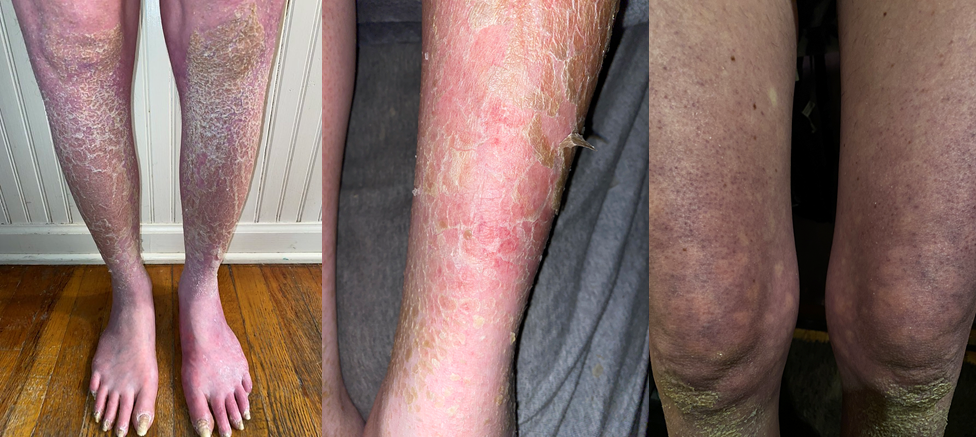
Feet and legs appear less reddish and flushed when elevated, however, they quickly turn purple upon standing. The purple discoloration fades when feet are elevated. Flushing is also present after showering and with temperature changes. Edema is present in both feet, ankles, shins, calves, and knees. An extremely painful, deep “itch” is felt in both feet and lower legs. Tremors are present throughout both legs. Standing upright elicits dizziness, tachycardia, presyncope/syncope, heart palpitations, and blurry vision (especially after eating).
Bilateral footdrop is present without a known cause. As a result, walking is exceedingly difficult, and assistance is required to move throughout the house. Balance, motor planning, proprioception, coordination, and gait have all been dramatically impacted. A wheelchair/transport chair is currently being utilized for community access.
Excruciating 9/10 pain in feet and lower legs. Hyperalgesia and allodynia observed. Socks, shoes, and any other clothing/materials are no longer tolerated below the knees due to pain. Severe 8/10 “deep bone pain” in lower legs and shins. Severe 8/10 joint pain in shoulders, hips, knees, hands, fingers, ankles, and wrists. Muscle spasms and tremors (lower back/body), stiffness, and weakness in legs and arms. It is now difficult to type and to write due to pain in wrists, hands, and fingers. Lights, sounds, touch, and weather/pressure changes cause significant 7/10 pain.
Diet is currently limited to about 10 foods (has decreased over time) due to allergic-like reactions that occur immediately after and while eating foods. The severe reactions have resulted in 3 trips to the emergency room. Foods frequently cause swelling to the face, eyes, and lips, dizziness, nausea, excessive eye dripping and tearing, excessive post-nasal drip, and an extremely painful deep itch with a rash and “pinpoint” lesions to appear on legs and feet. Eating also evokes sweating, extreme fatigue, and tachycardia. Only fresh food is consumed. Leftovers are frozen immediately. The family has not been able to cook inside for over 3 years due to serious respiratory distress, reactions, and irritations to eyes, ears, and throat caused by smoke, scents, and odors. In addition to scents, there is an extremely heightened sensitivity to light and sound. Socks, shoes, and any other clothing/materials are no longer tolerated below the knees.
Nutrient Deficiencies
Over the last year, we have learned that Megan suffers from several nutrient deficiencies, including thiamine, which was measured at only <6 nmols/L in December. After stumbling upon a case story about thiamine deficiency here, it is difficult not to wonder if low thiamine was responsible for her rapid decline in health following the surgery. Many of the symptoms she developed immediately following the surgery, the muscle weakness, edema, foot drop, proprioceptive difficulties are indicative of low thiamine. Over time, she developed an intolerance to most foods, which, from what I understand, is also common with thiamine deficiency. This then spiraled into other sensitivities (light, sound, and scent, etc.) and other sets of bizarre symptoms. In fact, as I do the research, I am learning that many of her ‘diagnoses’ are not independent diseases but could actually be manifestations of the low thiamine.
Of course, as her health declined and her ability to safely tolerate foods also declined, other deficiencies likely came into play. The skin issues may be related to deficiencies in vitamin A, which we have tested, and vitamins D and K, which we have not yet tested. She is also severely deficient in vitamins B12, C, and has low iron, copper, and zinc. Each of these can contribute to a wide variety of symptoms and compound her already poor health.
- Copper Deficiency 2/16/22
- Ferritin Deficiency 3/8/22, 8/12/22
- Zinc Deficiency 8/12/22
- Vitamin C Deficiency 8/12/22
- Vitamin A (Retinal) Deficiency 12/9/2022
- Vitamin B1 (Thiamine) Deficiency 12/9/2022
- Vitamin B12 (Cobalamin) Deficiency 12/9/2022
Current Symptoms
- General: heavy fatigue, migraines, low-grade fever, flushing, swollen lymph nodes, night waking, early waking, difficulty falling asleep, and daytime sleepiness
- Eyes: droopy eye lids, blurry vision, eye dripping, and excessive tearing
- Ears/Nose/Throat: hoarseness, stuffiness, sore throat, postnasal drip, heightened sense of smell, sinus pressure, ear ringing and buzzing, headache, migraines, sensitivity to loud noises, sores/ulcers on the roof of mouth and tongue, swelling of face/lips/throat, and lips/throat feeling “tingly”
- Heart: tachycardia, palpitations, swollen ankles/feet, edema, and blood “pooling” in legs
- Respiratory: shortness of breath/breathlessness, coughing, and wheezing
- Gastrointestinal Tract: bloating, cramping, acid reflux, alternating diarrhea and constipation, excess flatulence/gas, indigestion, nausea, and poor appetite
- Urinary Tract: the sudden urge to urinate, and mild bladder leakage/incontinence
- Musculoskeletal: muscle spasms, tremors, cramps, joint pain, joint stiffness, and muscle weakness
- Skin: rashes, hives/welts, hair loss, itching, swelling, skin peeling and flaking, livedo reticularis, excessive sweating, “pinpoint” lesions, flat-reddish lesions, and dermatographia
- Endocrine: cold intolerance, heat intolerance, urge to drink water, abnormally heavy/difficult menstrual periods, chills, and shaking
- Neurology: difficulty concentrating, difficulty thinking, difficulty balancing, brain fog, dizziness, light-headedness, tingling, and tremors
Previous Medical History
- Infected with Epstein-Barr/mononucleosis: 1993
- Pityriasis Rosea in 2011
- Infected with antibiotic resistant strep throat in 2012
- Left hip labral tear in 2016
- Right hip labral tear in 2016
- Erythema ab igne (due to heating pad) in 2017
- Left hip arthroscopy on 6/20/2017
- Femoral osteoplasty
- Mild acetabular rim trimming
- Minor shaving chondroplasty
- Acetabular labral reconstruction – transplanted labrum made from 11cm graft (cadaver tissue)
- Capsular closure
- Arthroscopic greater trochanteric bursectomy
- Windowing of IT band
- PRP injection
- FDA Clinical Trial of Neridronic Acid for CRPS 12/2017
Current Diagnoses
- Right hip labral tear, FAI/CAM Impingement, Bursitis, 2016
- Complex Regional Pain Syndrome (CRPS) 11/1/2017
- Suspected Ehlers-Danlos Hypermobile Type (hEDS) 10/1/2018
- Suspected Histamine Intolerance/Mast Cell Activation Syndrome (MCAS) 10/1/2018
- Bilateral Footdrop 10/1/2018
- Bilateral Common Perineal Neuralgia 10/1/2018
- Orthostatic Intolerance/Dysautonomia (POTS) 10/1/2018
- Alternaria Alternata allergy 11/13/19
- Secondary Polycythemia 1/5/2020
- Hashimoto’s Thyroiditis 9/14/2021
- Tinea Pedis Onychomycosis 12/2/2021 (misdiagnosed and overlooked for at least 2 years)
- Elevated Leukotriene 2/16/22
- Dysautonomia/Postural Orthostatic Tachycardia Syndrome (POTS) 9/6/2022
Current Medications
(updated 1/15/23)
| Morning (Before breakfast) |
Evening (Before dinner) |
Late Evening (Before bed) |
| Naltrexone (LDN) 4.5 mg | Vitamin C 1000 mg | Metoprolol 12.5 mg |
| Singulair (Montelukast) 10 mg | Zinc (sulfate) 25 mg | Neurontin (Gabapentin) 300 mg |
| Aspirin (NSAID) 81 mg | Copper 2 mg | Vitamin B1 (Thiamine) 100 mg* |
| Tagamet (Cimetidine) 200 mg | Iron 50 mg | Topical Terbinafine Cream (PRN) |
| Zrytec (Cetirizine) 10 mg | Tagamet (Cimetidine) 200 mg | |
| Synthroid (Levothyroxine) 50 mcg | Zrytec (Cetirizine) 10 mg | |
| Quercetin 500 mg | Quercetin 500 mg | |
| Neurontin (Gabapentin) 300 mg | Vitamin B1 (Thiamine) 100 mg* | |
| Vitamin B1 (Thiamine) 100 mg* |
*Vitamin B1 (Thiamine) started 12/23/22
Previous Medications
Short-term Prednisone (following ER Trip) provided significant relief of pain, skin rash, lesions, reduced swelling, and allowed more foods to be tolerated. Produced significant improvement of symptoms.
- Ketotifen – This medication was introduced and then discontinued due to potential side effects and lack of progress. Megan was taking 1 mg
- Cromolyn – This medication caused mouth ulcers (white spots) to occur, and it was discontinued. A nebulized form was prescribed but given without instructions as to how to introduce.
- Xifaxan – 10-day antibiotic course completed on 7/18/22 without improvement
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Photo by Sydney Rae on Unsplash.













Did you ever perform a test for fungal overgrowth (eg Metabolomix, urine; GI Effects, stool). My clinical experience from my functional medicine clinic is that fungal overgrowth including SIFO is vastly underrecognised as a contributing factor.
Also, did you do a SIBO test? 10 days of rifaxamin may not do the trick to clear SIBO. Methane? Hydrogen sulfide?
Wish you get better soon!
You are genuinely a great person for doing all this for Megan while taking care of her at the same time! I’m very sorry to hear that she’s been suffering, as I can’t imagine the physical and emotional pain she’s been going through. I can relate to her because I have developed some of her symptoms in the past several years (while the rest in the past decades), although mine are less severe. Sorry I wrote a long response, but I hope I can share my experience with you (and possibly other readers who are going through the same thing.)
I (39, Female) have had discoloration and livedo reticularis (especially during showers and when standing up), and dry skin in my lower limbs for more than 20 years; my face has always been reddish; scalp, ears flaky, and I have always had GI issues; I also have anxiety throughout my life. I had a severe infection in my left leg after falling down on a pile of dirt when I was in elementary school. It took me a long time to recover. During that time, I was in a non-English-speaking country. My mom and I just followed what the doctors told us to do. I don’t exactly recall my medication, but it involved antibiotics.
About five years ago, I started to develop hair loss and insomnia, but I thought it could be a result of my aging (or getting close to perimenopause). More recently, I developed many food intolerances, breathing issues (no mucus in the nose but always find it hard to breathe, post nasal drip which causes breathing problems whenever I sleep), bladder/urination issues, pulsatile tinnitus, tingling/numbness in parts of my face, and allodynia in some toes. On a bad day, my toes get electric shocks when touched. When it first started, it came and went. These days, the pain is constant whenever they are touched. But if I keep on touching them, the sensation will subside. I think it “teaches” my nerves to be ok with the touch. It always comes back, though. It just offers temporary relief for a day or two.
I went to a cardiologist some years ago and was diagnosed with chronic venous insufficiency. My ultrasound showed insignificant, minor plaques. I was asked to consider a laser procedure but chose to wear compressed stockings instead because I didn’t think it was the problem, as the discoloration resolves when I raise my legs. At that point, I still thought something was wrong with the veins deep in my legs. (It took me many years to realize that the problem might be skin-deep and that something was wrong in the capillaries underneath the skin. But the million-dollar question is what and why?)
Because of my recent symptoms, I went to a neurologist and was diagnosed with low-normal b12 levels and suspected of having small fiber neuropathy. I had a brain MRI (w/wo contrast), a CT scan of my temporal bones, and a variety of blood tests, all of which showed no MS/tumors in my brain or serious infections in my body, although I have high levels of igG, which I believe to be my antibodies of VZV. (I later went on to test all of my vitamins and found that I was low on vitamins D, B1, and high in beta-carotene, which is how I found this website as I looked up the causes for B1 deficiency. I never tested for Epstein-Barr virus, however.)
I researched a lot and came across a condition called erythromelalgia (EM). I then went to a rheumatologist regarding this info and was later diagnosed with Raynaud’s and possibly EM (since my redness and swelling don’t bring much pain). I don’t know that I have EM for a fact. But as I read a lot about it, I realized the problems in the mechanics are very similar, even though the cause could be entirely unrelated.
I realized that temperature, certain foods, and stress/anxiety always aggravate my discoloration, so anything like exercise and showers will help with the purplish color but aggravate the redness/swelling. (It took me years to realize that my redness/swelling and purpleness are different.) Too cold, the blood vessels constrict, so the skin turns purplish; too hot, they dilate, and the skin turns red and swells. But the problem is that what’s considered a normal temperature to a normal person is not “normal” to my body. I learned that this could be a nerve issue for some people. (In other words, their blood vessels don’t know when to dilate/constrict.) In my case, since my blood vessels consistently dilate when hot and constrict when cold and that balance is extremely delicate, I only can deduce that there is something wrong with how my nerves send signals to my brain or that my nervous system is on extremely high alert, hence, the sensitivity in temperature, stress, and food. I also learned that the problem, as mentioned earlier, might be only skin-deep. Because when I wear compression stockings, my discoloration is gone, but I always feel super nauseous. I think they do a good job of making the blood in the skin-deep blood vessels leave, but at the same time, it also makes the blood in the veins deep within my legs go too fast (because the problem is only in the capillaries under the skin, not deep within.) And because of constant constriction (whenever there is no dilation) in those capillaries, the skin is always dry there as the nutrients have difficulty reaching the tissues in the skin. The same thing also happens on my scalp and face. I once read a published paper about a man who had an accident where a bullet entered somewhere lower in his spine, but after the surgery, he has this blood pooling in his lower legs whenever he sits/stands. (Could there be something wrong with the nerves where Megan had her surgery?) As far as I know, the lower section of our spine is responsible for nerves in the legs. And I found massaging gently on the spots a few inches off each side of where the spine ends to be helpful for the discomfort and discoloration in my legs.
At the end of the visit, my rheumatologist recommended aspirin. However, it caused my toes to be redder and more swollen. I stopped it, and they got better. I feel that since aspirin dilates blood vessels and my blood vessels have trouble knowing when to constrict, more blood pools there. When I saw that Megan is also taking aspirin, I wanted to know what it was for.
In addition, menstruation always plays a role in how women perceive pain. The closer it gets to our period, the more pain we feel due to our hormones. Every one of my symptoms is worse as it gets closer to my period, and I believe it happens to many people as well. I think this is not something to be super concerned about, but it’s just that for Megan, her situation is difficult because her symptoms are more severe to begin with than the regular person’s. (However, after taking B-complex, I started to have very painful cramps during my period. But after adding vitamin D, iron, copper, selenium, and calcium, the cramps are back to minimal, although I am not sure which of these help as they are all in the same supplement.)
I understand that no one wants to take prescription drugs if they don’t have to. But I believe Megan’s many drugs have contributed to her nutrient deficiency, weakening her fragile body. I am not asking her not to take the drugs; it may be important that she does. But it is definitely the right call to add supplements. Although, judging by the condition of her body, it might take longer to see improvements. But trust that they will improve. It may also be hard to find the right mix of supplements for her due to her many symptoms and intolerances, but I highly recommend starting at super-low doses and adding one at a time. I did that because everything triggered something in me; I just had to pick one/a combo that relieved the most intense symptom.
The safest one has been B-complex; even vitamin D worsened my hair loss. But I needed it, and I realized combining B-complex and D eases the hair loss a little. Magnesium, however, triggers GI problems and redness in my legs. After taking B-complex (still at a low dose), I noticed my mood improved despite the period cramps. (After I developed so many symptoms, my anxiety and negativity were through the roof. And I had horrible insomnia and dry, painful skin.) And while my symptoms are still here, they (especially insomnia, dry skin, food intolerances, bladder issues, and hair loss) are a little less intense, and I think my mindset has much to do with it. I stopped giving my condition too much power/attention and kept reminding myself that things would improve. I also stopped looking for an answer obsessively because one thing led to another, and then another… this cycle never ends. I stopped looking at Google a few hours before my bedtime, letting my mind wind down. These days, I do what I can. I know it is hard, but it feels good to take your mind off the symptoms without worrying about what will happen next, and this is much needed for both you and her.
Lastly, finding a therapist specializing in helping chronically ill patients might benefit Megan, as I know it is extremely difficult and disheartening to deal with a chronic illness without knowing the cause or when it will improve.
Best of luck to you both!
Has malignancy been ruled out? I’m thinking along the lines of a paraneoplastic syndrome with acquired ichthyosis. See POEMS syndrome, see also monoclonal gammopathy which can cause neurological symptoms.
At this point I would say your wife has significant mitochondrial dysfunction. Without sufficient energy the body struggles to function, heal and recover. The many supplements suggested are likely having a limited benefit because metabolism is compromised due to insufficient mitochondrial energy to perform metabolism. In a severe case like this I would use PEMF, Frequency Specific Microcurrent (FSM) and red/green/violet Erchonia lasers in twice daily sessions to stimulate the brain, nervous system, lungs, heart, vascular system, and gut. Why those; the brain controls the body through the nervous system, the lungs absorb oxygen necessary for mitochondrial function, the heart and vascular deliver the oxygen and nutrients, and the gut is critical to nutrient absorption plus approx 70% of our immune function resides in the gut. PEMF improves cell membrane permeability to allow more nutrients and oxygen into the cells and toxins and wastes out. It also helps with blood and lymph circulation. FSM uses microcurrent to target specific tissues and issues. The combination of red/green/violet Erchonia lasers help stimulate all four complexes of the electron transport chain necessary for mitochondrial ATP production. Hope this helps.
Good bless you for being such a help to your wife.
My 2¢ on one thing: montelukast. I took that for allergies and while it helped greatly, I believe it lowered my immune system. I want to say it was three months into taking it that I had a bout of shingles on my face while in my mid-thirties.
Please make sure you read up on side effects of pharmacy products.
I am so sorry you are both going through this. I just have one thing to add- perhaps try another avenue to tackle the mast cell issues, such as quercetin for example- and not the stomach acid blocker. Two of my teens have mast cell/ EDS/ Pots- and one has very low iron, cholesterol, most nutrients and we found a huge cause was that she has malabsorption issues – low bile- low stomach acid- and the famotidine she was using for mast cell was making it much worse because it was lowering her always already low stomach acid. She started HCL with her protein foods and no longer needs to take iron, has gotten color back and energy is also improving.- it has taken ten years to get to this point and it was never mentioned. I was searching for reasons for low iron and saw a video saying a top cause was low stomach acid. Anyway I am unsure if there may have been some foreign invader that has attacked her stomach making it difficult for her to absorb anything and heal. There may be tests for stomach acid, I am not sure. Thiamine has been a great help to them, but they use higher doses. Sending healing thoughts.
Hi again! I’ve left a comment before but wanted to add something that might truly benefit her healing journey even further. I just wanted to encourage y’all to check out Dr, Pompas program. He is a genius and basically created an at home program to heal your body down to the cellular level so your body can fully start healing in other areas. Maybe just think about setting up a consultation and let him know your situation. It’s a five month protocol and has had a 98% success rate. He basically sends you a test to check the toxicity levels in your urine and depending on that, that’s where y’all will move forward if you like. Month one is a deinflame the body, months 2-4 is detoxing the body of toxins trapped in her cells, and the last month is detoxing the brain. He sends you all the info and supplements you need. One thing I love is it’s a one time payment, and you have access to a clinician 24/7 and have access to all his research and q&a with him for life. It’s not gonna send you down a $10,000 rabbit hole like I’ve experienced in my own health journey. I just want you better and for you and your family to enjoy life again fully together. I hope you guys are doing well and seeing progress. Sending so much love & prayers❤️
Oh, and here are a few links with photos of chronic venous insufficiency and DVT that you may want to review… they are identical to your wife’s photos. 🙁
https://www.clinicaladvisor.com/home/dermatologic-look-alikes/two-erythematous-leg-rashes/3/
https://provascularmd.com/stages-of-venous-insufficiency/
Many prayers for answers, restored health and healing for your wife! If I were in this situation, in addition to investigating thiamine, I would seek the help of a vascular or vein specialist and have them check for chronic venous insufficiency and/or Deep Vein Thrombosis. These two conditions are intertwined and can be caused by damage to veins during surgical procedures. Google for images of what these conditions look like in the legs/feet. Also, I took quercetin for a good while but have since learned that it chelates important nutrients like iron and zinc out of the body, and can cause nutritional deficiencies.
Hope this helps!
Hi,
I don’t know if this helps anyone but the documentary the
“The Bleeding Edge” is an eye opener and views some cases of patients health going downhill after surgeries done with various implant materials. If you had or are going to need hip surgery or metal, mesh put in your body please see this documentary.
Hope this helps some of you.
God Bless!
Barb
Briefly about me:
I have ME/CFS, MCAS. I very soft skin and am unfortunately hypermobile.
My condition has improved a lot with high dose vitamins.
Thiamine :
Benfotiamine 600mg – 400mg – 400mg
Sulbutimine : 600mg- 400mg – 200mg
I also take sulbutiamine through the skin (neck, arms, neck) when I am weak.
Riboflavine (supposed to always be deficient in ME/CFS) Has this been checked in your wife?
high dose 6 x 125mg
5-MTHF 5mg- 1mg – 1mg
Bitotin 100mg – 0 – 100mg
Magnesium chelate 1.200mg – 1.200mg – 1.200mg
Vitamin MK4 (Thorne) 15mg- 15mg – 15mg
Lugol’s solution 75mg – 75mg – 0
furthermore chromium, manganese, selenium, boron ,
sodium and Mg/Ca butyrate
Vitamin B12 (methylcobalmin 10mg/ adenosylcobalmin 10mg) in weekly alternation
Thiamine, ribovlavine and Lugol’s solution should be used very slowly until intracellular resistance is overcome.
This was very unpleasant for me. It was worth it.
There are some with ME/CFS , where it also comes to similar skin changes.
All the best for you and your wife.
I have many similarities to your wife (and some differences as well). My question to you is how they determined your wife had secondary polycythemia? Was a bone marrow biopsy done to rule out polycythemia vera?
Look into retinoic acid toxicity. Thre’s a common misconception that vitamin A is a vitamin which it might be if it’s in proper levels in the body but if it accumulates beyond the body’s capacity to excrete it then it can cause severe toxicity. This toxic level of retinoic acid causes many debilitating symptoms and develops into chronic diseases.
These two websites are an excellent source of information regarding vitamin A toxicity and the program how to correct this. The author of three ebooks by the name of Grant Genereux is priceless. The information then just might save thousands of lives of people like the woman described here and her incredible struggle with health issues.
https://ggenereux.blog/m
https://members.nutritiondetective.com/spaces/157
I’d like to know this as well. I have polycythemia also. I’m still being investigated for the type. I do not have the JAK 2 mutation but haven’t been tested for the EXON mutation yet. My oxygen saturation seems to be good at 96-99. I still need to have an ABG test and a few others. It’s confusing. I have many of the symptoms his wife has. Funny because I have been taking high doses of thiamine for about a year now and have been feeling pretty good. I still have bad days but I’m so much better than before. I also have what seems like mcas and dysautonomia. They are significantly better since I started thiamine. I made the mistake of adding nac to my protocol. After taking it for a month I crashed and all the symptoms came back. I stopped it and felt pretty normal again 2 days later. I wonder why? I was really hoping the NAC would help me even further. It’s hard to know what started all of these issues but it could have been when I got chronic strep and after years of taking antibiotics I had my tonsils removed at age 29. Then I got the epstein barr virus not long after. Do you have polycythemia or MCAS?
I’m assuming you have ruled out preexisting biofilm on the cadaver and/or the rods/pins that were used in the surgery..? Perhaps there were mold spores in the variety she has an allergy to on one of the foreign bodies they used. Perhaps that is why she tested positive for an allergy to that mold. There are some excellent youtube videos available on the best ways to test for it. These were my first thoughts, but this will be on my mind, and if I have any more, I will comment again. I understand it is out of desperation, but thank you for being vulnerable and sharing this heartbreaking story. I hope you find real answers.
This is something safe and easy to try that has a long track record of excellent results—methylene blue. Here is an article by Dr. Thomas Levy. This has turned around a lot of people with general mitochondrial issues.
https://orthomolecular.activehosted.com/index.php?action=social&chash=f7664060cc52bc6f3d620bcedc94a4b6.265&s=082503956821046a044f4c1d4b41183e
I used LDN for several years, as did two of my children. We were told by our doctor that it’s important to use it at night in order to generate the endorphins that are responsible for boosting the immune system.
Here is a wonderful interview with Dr. Bihari, the discoverer of LDN’s therapeutic benefits.
http://todayspractitioner.com/wp-content/uploads/2013/10/Bernard-Bihari-MD-Low-dose-Naltrexone-for-Normalizing-Immune-System-Function-athm_19_2_bihari_56_65.pdf
Best of luck to you!
May she emerge with restored health, knowing that you stood by her through it all! My humbly-offered, non-expert thoughts:
That antibiotic-resistant infection sets off my alarms. This scenario comes to mind: She was exposed to a resistant pathogen. She endured multiple bouts of heavy antibiotic usage, devastating her delicately balanced bio-flora without ever fully wiping out the pathogen. Doctors have only begun to wake up to the concept of the “human ecosystem”, so they never gave her bio-flora a second thought. Yogurt, if she was lucky. After a hip surgery and another bout of heavy antibiotic usage, her ecosystem was barren aside from the proven resistant pathogen (and possibly new ones) who found a fertile, empty ecosystem to colonize. Nature abhors a vacuum.
Meditate or pray or ponder on this possibility and consult someone who can think systemically. Personally, if it were my own body, I would give up on the conventional medicine that brought me to that place, and do whatever I could to ensure that my bio-flora was as diverse as possible. Perhaps an advanced round of antibiotics followed by heavy pre/pro-biotics, or maybe something more slow and steady. Seed Probiotics is one I’ve come across that seems to be more advanced in its formulation and theory, but anything’s better than what she’s probably got going on. My heart goes out to you both. I wish you the best.
Have you all considered that some of the prescribtion medications are known to deplete some of the nutrients in which she is low? For instance Cimetidine/Tagamet is known to deplete iron, zinc, and B12, that are reportedly low in this case, but can also deplete calcium, folate, and vitamin D.
Hss she done any tests for heavy metals? Especially mercury. I would definitely investigate.
I am no doctor and there appears to be many things happening, which makes it confusing to unravel. Firstly I would start with looking at the integrity of her cellular membranes in particular the level of lipids especially choline(vital for nerve impulses) and omega 3 and cholesterol(our brain is estimated to be up to 70% cholesterol). This aspect could also be causing inflammation. Secondly to understand what causes balance, prolapsed feet, and bone pain I would start to learn from Postural Resturation Institute, this is a neuro muscular problem, In essence everyone is right dominant regardless if they are left handed therefore it favours the right and sets up patterns of compensation which turns off muscles. Although both feet have prolapsed so muscles have turned off on both sides. PRI is about neuromuscular retraining, it involves becoming aware of our muscles by sensing the ground, these senses via our brain tell our muscles what to do. When these messages are altered our body structurally changes ie. the prolapsed feet, this is stemming from the hamstrings and the glutes turning off and our hips losing the ability to abduct and deduct when we walk. Both feet have prolapsed, I would be looking at PRI because the brain isn’t working telling muscles to fire and muscles are not firing and others are over compensating. This is all tied into the fight and flight and our breathing, holding us in these physical patterns. The PRI method is about neurological retraining and learning to identify the right muscles that should be engaging. There are many other layers going on and that is the challenge to understand each layer, peeling the onion one layer at a time. Below is a recording from one practitioner trained by PRI, (I like him because he was affected from a young age that altered his jaw alignment and that set up other compensations in the body causing lots of pain – I also have a misaligned jaw so my neuro messages were altered from a young age and compounded with my chronic illness, Vitamin B1 was part of the issue which PRI don’t go into or diet, when I took high dose B1 one neuromuscular problem resolved and that allowed me to identify a pattern in my muscles that kept me going to the chiropractor every couple of days with muscles tightening up in a pattern, twisting me. I also had a prolapsed left foot) I have coped for decades stretching but that is only a temporary solution. There are many practitioners trained in PRI, it is a very different approach, it addressess the neuro aspect, maybe you will find one that is experienced with chronic illnesses causing neuromuscular imbalances. Here is a short clip of one practitioner talking a little bit about it. But look up Postural Restoration Institute to find practitioners that speaks to you and your condition. https://www.youtube.com/watch?v=AaeSQq6-erk
I am so sorry to hear about your wife’s suffering.
I recently read an article talking about how plastic surgeons can help to repair nerve damage. Maybe that would help?
Unfortunately Gabapentin causes edema and weight gain in some people (but helps with pain). When I was taking gabapentin, I gained a ton of weight and had significant edema as well. I was able to wean off gabapentin (slowly) with alpha lipoic acid myo&chiro inositol. I have been off of gabapentin for about 8 months and I am slowly losing weight. Most of the edema is gone now.
L-lysine and liposomal vitamin C might help viral load management.
Maybe the facebook group iron protocol can help with ferritin deficiency which would help her cycles. Guessing her female hormones are involved as well….again, so sorry for her suffering.
Also I wanted to add I completely agree with you about the thiamin deficiency. It is sadly insanely over looked. Just be mindful of what type you are giving her HCL (while you still can take it alongside the benfotiamine) requires an insanely high dose for the proper amount to be bioavailable to the level she would need. Benfotiamine crosses the blood brain barrier (without depleting glutithione which HCL and most other forms can’t do) and bipasses a lot of transport pathways so it is absorbed at a higher dose. I had almost every symptom your wife has but wasn’t bed bound thankfully. I’m 24 and got insanely sick 5 years ago. Went without treatment and continued to decline especially after I had surgery and even more after having my daughter. I genuinely thought I was dying and I’m not one to like going to drs etc but I ended up going last year after I had a fear of having Alzheimer’s and dying; aswell as having a huge list similar to your wives that was unexplainable. I got diagnosed with mold toxicity, CIRS, MCAS, high histamine, and injured limbic system. And through doing my own research I believe thiamin deficiency aswell and have seen even more additional improvements after supplementing and as well as avoiding foods that deplete thiamin. I went from feeling like I was only existing waiting for death and now I’m almost me again. This may not apply to her at all but you just really never know, I would maybe do a mold and or parasite test just to be safe. It definitely sounds like her surgery as well as the meds have effected her but there could be a sneaky additional thing hiding there aswell like in my case that was depleting me of every more nutrients. I’m truly praying for y’all and hope y’all get the answers you deserve.
It sounds like a combination of CIRS, MCAS, high histamine, and an injured limbic system. I would highly recommend getting her on a great quality multi vitamin, desiccated liver supplement, vit D/K2 drops 5000IU per day, benfotiamin drops, b complex, methylation complete b-12 tablets, magnesium glycinate (300-400 mg a day) for at night before bed, vitamin c 1000 mg per day, glutithione, a good pre and probiotic do not take them together (wait about 30min after to taking prebiotic to take probiotic). ION gut support on top of pre and probiotic is amazing as well with encouraging greater cell to cell communication in the gut. Make sure she is getting adequate fats and protein, try and reach 30 g of protein per meal 80-90g per day, preferably grass fed grass finished beef, venison, or bison over chicken and fish. Depending on what she’s sensitive to an avocado smoothie twice a day morning and evening would be great. One whole avocado with 8-10oz of organic orange juice blended is one smoothie worth. Tastes amazing and will boost her fat/ fruit intake. I would minimize vegetables as they are harder to digest and tend to be higher in oxalates, etc which can actually inflame her more. Fruits, sweet potatoes, raw honey, pure maple syrup, raw A2 dairy from good source if she can tolerate , all as her carbs. Also pasture raised eggs again if she can tolerate. Have her drink a 6-8oz glass of water with 1/4 tsp of Redmond real salt twice a day (please don’t use any other source of salt). I would encourage alternating throughout the day between alkaline water and mountain valley spring water. No processed foods whatsoever, and only cook food in grass fed tallow. Maybe even consider taking tallow supplement as well to increase fats, a woman needs 50 g of fats a day minimum for hormones to even work. If she can handle dairy; ghee and butter are good options too again just must be sourced from A2 or it could further inflame her. If not just stick to tallow. Don’t be afraid of cholesterol, as your brain & nervous system have to have high amounts to function. As long as she’s staying away from processed foods and bad oils she’ll be good. Just please don’t cook her food in any veggie oil, canola, or seed oils when it comes to her food. Since she can’t workout to build a sweat to detox I would put her in a detox bath at home 2-3x a week. As hot of water as she can stand. Before she gets in mix in Bentonite clay, Ascorbic acid, magnesium flakes, mustard powder, epsom salt, baking soda, and essential oils of choice that will help her relax. If she can do it, stay in for 40 min. Let her take a book or tablet or whatever to enjoy her time. Also look into GUPTA brain retraining or other similar programs. To sum it up essentially when someone endures a trauma; it could be as small as something like the flu or food poisoning. Or from a surgery like in your wife’s case. Truly could begin with anything depending on the individual. It causes an injury to the limbic system which in turn can cause all kinds of issues with the body, and symptoms just like your describing and beyond, and again everyone’s symptoms can be so different and vary in severity. You can read peoples stories on their site or even watch videos on YouTube to feel encouraged. Her life may feel over it may feel like it can never get better but I’m telling you it’s not not and she will enjoy life again. It just takes commitment and diligence. Please don’t give up. She will have a life to deeply enjoy again. I would definitely get the GUPTA program asap and begin as it’s a process and will take time for her limbic system to heal. But it’s a one time payment no subscriptions. There is a community of people here to encourage you and know we love you and are praying for you. If there’s anything you need or even just any questions at all please please please feel free to reach out to me, this goes for your wife as well. I’m so so sorry y’all are going through this, but I know yall can do this. This season will pass and she will be herself again.?
Presumably your wife had general anaesthesia which is known to deplete B12 which will in turn exacerbate any folate deficiency, impair methylation and perhaps even cause her to fall into the methylfolate trap, I.e. folate deficiency leads to B12 deficiency.
Her deterioration in the lower extremities sounds very much as though she has impaired ability to synthesise DNA and an impaired metabolism. Her body simply no longer has the energy to absorb and process sufficient nutrition.
Do you have her latest CBCs? Unfortunately, doctors do not understand how to interpret them in order to diagnose and treat macrocytosis and microcytosis.
Certain aspects of her journey echo some of mine. I eventually determined that I had both damage and nutrient deficiencies (B2, B12 and B1) caused by fluoroquinolone antibiotics (Cipr0 once a year for about 20 years) and g@bapentin (took for over 20 years) as well as withdrawal or as they like to call it discontinuation syndrome from stopping g@bapentin over just 2 weeks as advised in literature. Did your wife ever take a fluoroquinolone antibiotic and/or g@bapentin or Lyric@? Dr. Gregory Russell-Jones (google B12 Oils RNB protocol) has determined that if one if deficient in B2 then they are likely deficient in B12. I restored my B12 by using his protocol. Maybe injections can work but he says we need the co-factors iodine, selenium, molybdenum to activate B2 so we can get B12 working. I also tested and was severely deficient in thiamine. Taking care of all of this has restored me to health except I am now tapering off a pain drug given to manage the extreme pain caused by the deficiencies (small fiber neuropathy.) The mainstream doctors were almost useless and even caused more damage. I think your wife can heal! It takes a long time to become B12 sufficient again. Dr. R-J advises not to take any more B1 than B2 by the way. It takes persistence and patience. I am so sorry for her horrific suffering. (BTW I have a hip labral tear which I suspect was partially from taking Cipr0 all those years.) There is a support group that aids in understanding Dr. Russell-Jones protocol and it is called Understanding B12 Deficiency. I found it incredibly useful. It is well moderated.
What would you look for/ask for in terms of testing for nutrient deficiencies?
Oh the fact that you went so deep and investigated your wife’s health shows that you are an amazing human. Really amazing.
I had 80% of these symptoms which I recovered from with many things but ultimately, what really did the real healing was pounding hard on TTFD, Benfothiamine and Sulbuthiamine. I took Thiamaxx + Thiamega combined every day and it felt like a miracle for me.
I also had a history of many surgeries (heart surgeries) because I was born with Heart Valve Aortic Stenosis. After every medication and procedure my health declined. I am 35 now and am seeing miracle in doing mega-mega dosing Thiamine + B Complex + magnesium.
Other things that I did:
Water Enemas
Lots of Coconut Water
Fruit + Orange Juice + Eggs & Meat diet
Red Light Therapy
Sauna
Cold Exposure
Grounding
EMF Shielding in my home (Cut off circuit breakers before going to sleep and shuting down Wifi).
Everything together + Mega Dosing Thiamine created a healing environment for my body.
On top of that the works of Dr Joe Dispenza was essential for deep inner emotional release and healing.
Here is my IG if you want to reach out: @gabrielbliss
This story is heartbreaking; I’m so sorry that you are living through this.
Were there any confounding variable that occurred around the time of the surgery? Any water damage to your home? It’s important to rule out CIRS (chronic inflammatory response syndrome) related to toxic mold and/or actinomycetes exposure. (see the work of Drs. Neil Nathan, Jill Crista, Ritchie Shoemaker for details).
Also, has she received any COVID shots? These have been shown to cause severe immunological, vascular, dermatological, neurological, and other problems – often in a relatively short timeframe.
Please keep us posted. <3
If she was diagnosed with b12 deficiency then she should be on injections. I deteriorated after general anesthesia, after following protocol from b12 society plus fixing other deficiencies I am almost back to normal.
They have discovered that sublingual B 12 is better absorbed than injections. That is on Pubmed.
Megan sounds so much like what I’ve gone thru. How lucky she is to have such a caring husband advocating for her. It’s so NEEDED, bc in her state, she may not be able to express her needs at times, as I too have experienced.
I too was labeled with (CRPS) Complex Regional Pain Syndrome by a few docs before discovering my thiamine deficiency (TD) (initially found in 2015: 6nmol/L (8-30 nmol/L lab norm);
yet no one told or treated me.
I was only asked if I was taking a multivitamin. No where near the doses one needs when left chronically deficient. In 2/2020 my thiamine deficiency was again lab documented on a regular blood B1 test (usually deficient on THIS test indicates CHRONIC DEFICIENCY).
Like Megan, I had MRI’s, cat scans, and lots of bloodwork, saw dozens of specialists to rule out other issues. None caught my thiamine deficiency until I suggested it to my neurologist, who was the ONE doctor who listened, encouraged me to be proactive and share research with him.
“Symptoms started after orthopedic surgery 6/20/17…” which many pharmaceuticals given during & after surgery along with the stressful surgery itself, has likely put her over her threshold into the thiamine deficient (and other deficiencies) state.
I suspect she MAY have been given prophylactic antibiotics during & after the surgery?
I suggest requesting her medical records to note meds used. Many are known to deplete thiamine.
Of important note is whether she got “jabbed” since this surgery? Or caught the “C” which may have also exacerbated her thiamine & other deficiencies as it did in me.
Her skin issues (our largest organ) are significant and I suspect due to untreated TD.
I had many skin issues, especially after contracting the “C,” which took me a good 6-8 weeks of supplementing to regain the progress made on my thiamine protocol.
Any added stressor sets me back, seemingly easier to deplete my thiamine which I blame because most of my multi organ system symptoms return, disappearing as I get my megadosing anti-inflammatory protocol in.
I see she was trialed on several meds which also seemed to worsen her health.
Wondering if she’s EVER received a fluoroquinolone antibiotic (there are about 60 generic versions).
I believe it’s what spiraled my health after I was treated with Levaquin, then began declining noting all Megan’s symptoms too, in myself!
However, gratefully I began researching on my own because Gabepentin made me much worse.
Sadly, collectively her symptoms scream thiamine deficiency from my own experience. Like her, seeing a “specialist” only seems to allow them to note their own specialty of symptoms which sadly overlooks her most important issue of underlying SEVERE THIAMINE DEFICIENCY (TD). Things seemingly to be worsening by much of the drug therapies instead of addressing the deficiencies (of which most docs have very little to no training in). My own excellent neurologist told me this, apologizing but telling me he’s learned so much from my case and NOW is testing all his patients for TD.
Pathetically sad, are the treatments which for me only “covered up some symptoms but worsened most,” so I stopped them slowly weaning off all, insisting on understanding the underlying cause instead of guessing and treating each symptom with another drug as my PCP continued trying to do.
I was Vit D deficient over a decade despite scripts, plenty of sun, and a diet rich in vit D. That should have been a huge clue to all doctors as to WHY I wasn’t absorbing vitamin(s), but as Chandler points out, Big Pharma and insurance companies dictates what our doctors can and cannot do.
Tagamet was taken off the market in most places, I’ve read.
PPI’s and anti acid meds decrease our needed stomach acidity to produce, absorb, and use vitamins, minerals, and nutrients.
If needed, on rare occasion of GI UPSET, indigestion, burning stomach (happened again recently after given a FQ antibiotic) I only use Famotadine for 3-4 days, then taking 3-1 pre/pro/postbiotics and gut enzymes to ease gut issues.
I use AA(Vit C) and magnesium citrate to ease my constipated days.
I support the gallbladder /Bile using TUDCA or Dr Berg’s gallbladder formula if I see pale, floating watery stools, indicating I need more bile.
I see she’s on thiamine 100 mg 3x/day which, in my opinion her symptoms indicate much higher doses needed.
Dosing, preferably starting intravenously then continued high dosing orally, which like me, once chronically deficient I’ll likely need for the rest of my life.
Off the bat here, I don’t see a mention of her methylation, glutathione, or electrolyte status.
For me, I support my methylation using SAM-e.
I take glutathione 500 mg 1-2 x/day since recently getting “floxed” again after a freak eye injury when I tripped 12/16/22.
In the mornings especially, as thiamine has “worn off” (average half life is 2-5 hours, I’ve read), I’m very unsteady, unbalanced, firmly using a cane to ambulate; very weak; brain fogged with severe nerve, muscle, joint, into my bones pain. Skin biopsies diagnosed my SEVERE SMALL FIBER NEUROPATHY (SFN) which I highly suspect Megan may have too. So severe it’s causing the serious breakdown in her legs. Her toe issues indicate probable candida which I had mildly too.
When deficient, the body cannot process sugar, carbs especially but many food sensitivities may ensue, unique to each person. This is why I journal my diet to learn what I do tolerate.
If so severe, it causes severe nerve damage that then may cause symptoms head to toe as I experience now too. I suspect her severe leg symptoms may be due to severe SFN??
Miraculously, I was making great progress following Elliot Overton’s anti-inflammatory neurological Thiamine protocol, until getting “floxed” again. I need to write that part of my long story too.
I take 2-3 doses of Benfotiamine/HCL (each capsule contains 150 mg Benfotamine with 50 mg hcl):
I now take 300mg Benfotiamine/hcl 3-4x/day
Lipothiamine 200mg 3 x/day
Plus a good multivitamin/BComplex which I alternate with taking B1, B2, B3, B12, and biotin/collagen separately in higher doses. I support my magnesium and potassium especially, but all others too for they, like the B vitamins all work closely together.
I’m reading a great book:
Fluoroquinolone Associated Disability (FQAD)- Pathogenesis, Diagnostics, Therapy and Diagnostic Citeria
Side effects of fluoroquinolones, written by Stefan Pieper.
This book sites thiamine therapy as well as many of the supplements I’m already taking. I’m slowly adding in others one at a time, starting low & always upping slowly to allow the body to rebalance and readjust.
I’m so saddened to hear of Megan’s suffering. I so empathize with you all. I wish I had an easy “one size fits all” answer here.
There is hope. I’d be completely bedridden, wheelchair bound if not for mega dosing thiamine while supporting it’s cofactor’s too. My thoughts stem from 30 years of nursing, and three years on thiamine protocol(s), always tweaking my plan according to research, and my journaling: rating symptoms,
noting vital signs, times/doses of supplements taken , diet intake/output.
Of note is your significant family history (like mine) also indicative of thiamine issues: thyroid disorders, degenerative diseases, cancers, histamine issues, MS (thought I had), cardiac disorders, many allergies, and food intolerances…
Well wishes to you. ❤️?
Has your wife ever taken or given a Fluoroquinolone Antibiotics such as Levaquin Cipro or Avelox? during surgery before or after? Have the skin lesions been biopsied for possible Cutaneous T-Cell Lymphomas?
It seems clear that she probably did not have any serious nutrient deficiencies before the surgery, which makes me think her body’s reaction to the surgery set off some destructive processes that have lead to the deficiencies and further symptoms.
Is she allergic to nickel? Any metal implants from the surgery? If so, what are they made of? Nickel allergy messed up my life so badly that I can’t even tolerate dietary nickel, and I have a small fear that I will one day be in a wreck or something and end up being operated on and given some sort of nickel-containing implant. Nickel is very common in stainless steel and even titanium alloys. Cobalt is another similar allergy. And some people with genetic issues cannot handle copper.
It also seems likely she could be having an immune reaction to the cadaver tissue.
I’d look into a parasite cleanse. I was deteriorating fast last year with multiple nutrient deficiencies, started having major autoimmune issues and ended up in liver failure I was on or tried many of the same medications listed. The first day I started working with a naturopath, she commented that it sounded like parasites even though I had three tests that were negative (apparently the majority of time those tests are false negatives). We took a few weeks to build my system back and then I started a cleanse. Within a week I saw liver flukes and after a few more weeks I saw whipworm and roundworm. I’m not 100% yet but I am no where as bad as I was 6 months ago!
This was my dad and was almost me ?. Unfortunately I learned too late and my dad passed with undiagnosed and untreated pernicious anemia, iron anemia and beri beri. A 230 pound 5’10” man that could physically do about anything was reduced to 5’3” 97 pounds skeleton ….while medicine watched and bilked very last dollar from Jaheim replacing joints and eventually placing a feeding tube when he could no longer swallow.
I sat at my hubs physical today while his b12 anemia and low red blood cells were marginalized and I thank god every day I learned better. We know his cause but I was astounded that the GP was utterly absent even with information I presented him to support what was happening.
Sad. Sad how many of us like Jane and others get left to essentially waste while they watch.
I was almost this. No one saved me. Not one doctor nor functional doctor seemed able to connect iron deficiency and B12 and B1 among others. I did finally save myself and thank the stars every day for content like this being shared and people willing to be vulnerable to share their stories.
I am so sorry to hear of all the symptoms and decline of health. Much of what your describe appears to have originated from the surgery so I would start looking there first. While I do not hold a MD I do work within the medical field. So for brainstorming I get a hold of any and all documentation relating to the original surgery. What are describing above sounds like your wife is having an internal reaction to either the donor tissue (if it was used), infection of the surgical area, or artificial implant reaction.
Appears her immune system is on hyper drive due to what maybe going on internally. Especially, when she used the steroids and it helped her condition really hints at her immune system is on high alert. Personally, I would work toward getting her immune system to calm down with a low inflammatory diet. Then review all the supplements you are taking some using high dose of some can cause others to decrease. Would it be possible to use a well rounded multivitamin to help keep everything in balance (not OTC multivitamins). Meal replacement powder drinks never worked for me personally and actually irritated my system. Look toward finding an integrative practitioner (review their education, first) since traditional medicine will probably continue to use steroids. Steroids are helpful for very short term incidents, but over use or long term are known to cause problems in the majority of people.
While working to get her immune system to calm down I would be on the hunt to find a surgeon who would review all the documentation you collected from the original provider. Make sure the new surgeon is outside of the original MDs umbrella of hospitals. Having an experienced MD who has no “tooth in this game” will be key. If she’s stable enough hopefully they would take an internal look at the original surgery.
I hope this helps and would provide another perspective. There are many within the healthcare system that truly want to help. Though like any occupation there are some that need to find another career. The patient then suffers because they are tumbled from provider to provider who only looks at their section of the body. That is one of the reasons I suggested an integrative provider since they are suppose to help in that department. GPs did that in the past, but sadly our system does not truly allow for that type of interaction anymore.
This is good advice.
I’ve made a note for myself to not use quercetin because of it’s thiamine antagonistic qualities.
I just wanted to relay this to you as well.
Linus I have also seen reports that quercetin is a thiamine antagonist. Quercetin is also a powerful antioxidant and is recommended to treat COVID symptoms and other inflammatory problems. I am wrestling as to whether to take it or not. How strong of an antagonist is it and if one takes megadoses of thiamine will this overcome the antagonistic effects? I don’t know and have not been able to find any answers.