Four years ago, when the heavy period bleeding which I’d had since adolescence suddenly became much worse, I never would have predicted that the cause of the bleeding would not be correctly diagnosed and treated until after I’d had an unnecessary surgery, a preventable major complication of another surgery, months of severe anemia and more. And yet many women may be at risk for similar problems without realizing it.
Heavy period bleeding (medically called menorrhagia) is a very common problem in women of reproductive age, affecting up to 30 percent of women. This type of bleeding can be very debilitating and difficult to deal with, as well as posing a diagnostic challenge for doctors to identify the underlying cause.
There are many possible causes of menorrhagia, including hormonal imbalances and dysfunction of the ovaries, fibroids, uterine polyps, adenomyosis, intrauterine devices (IUDs), and in rare cases, cancers of the reproductive system. One cause that is not often considered is a bleeding disorder. Up to 20 percent of women with menorrhagia may have von Willebrand’s disease, which is the most common of the so-called “mild” bleeding disorders (which include any bleeding disorder not classified as a severe hemophilia). The number of women with menorrhagia who have an undiagnosed bleeding disorder is even higher when platelet function disorders, another type of “mild” bleeding disorder, are included.
Studies have shown that gynecologists are not likely to consider a bleeding disorder as a possible cause when investigating menorrhagia, and are not likely to refer women with heavy period bleeding to a hematologist for further investigation, even when gynecological causes are ruled out. One study found that only four percent of physicians surveyed would consider von Willebrand’s disease as a possible diagnosis in women with menorrhagia, and only 3 percent of physicians would refer patients to a specialist.
Studies have also shown that women with undiagnosed bleeding disorders are more likely to be subjected to unnecessary surgical procedures, including hysterectomy, as a “fix” for the bleeding that doesn’t address the underlying problem. Menorrhagia is the major reason for approximately 300,000 hysterectomies per year in the U.S. Given the prevalence of undiagnosed bleeding disorders in this population, 60,000 or more hysterectomies per year could be performed in women whose menorrhagia could be addressed with treatment for their bleeding disorder instead of a major surgery. Women with von Willebrand’s disease are more likely to undergo a hysterectomy (26 percent of women with von Willebrand’s disease, compared to 9 percent of women in the control group) and to have the hysterectomy at a younger age.
In addition, undiagnosed bleeding disorders have a serious effect on women’s quality of life, and put women at risk for medical complications. Although women who have not experienced it, or men, who of course cannot experience it, may dismiss heavy period bleeding as simply a nuisance, it is far more than that. It can cause serious problems such as anemia, complications from childbirth and surgical procedures, lost work or school time, lifestyle issues, psychological disruptions, and have major effects on quality of life. The health-related quality of life for women with menorrhagia and a bleeding disorder was studied and found to be similar to that of HIV-positive men with severe hemophilia, underscoring the difficult symptoms and lifestyle issues that can result from these problems.
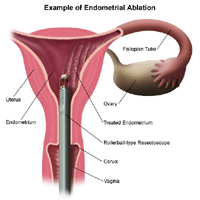
My own medical history reads like a clinical case study designed to educate doctors about the possible pitfalls of undiagnosed bleeding disorders, and judging by the numbers, there are many more women out there going through the same thing. After my son was born, the menorrhagia I’d had since I was a teenager worsened significantly. I had gynecological causes ruled out—no polyps, fibroids, or cancer. I already had been diagnosed with endometriosis, but that was not thought to be the cause of the bleeding. My gynecologist deemed the cause to be “hormonal” and spent two years trying to fix it with birth control pills, which didn’t work. At some point during those two years I asked for a referral to a hematologist, which I was told I didn’t need after a few preliminary blood clotting tests came back normal. I had an endometrial ablation, which also didn’t work, and caused my pelvic pain to worsen so severely that my first period after the ablation landed me in the ER (increased pelvic pain is a known risk with endometrial ablation).
I had enough of a history the first time I asked to warrant a referral. My history at that time included bleeding complications with my first laparoscopy for endometriosis, history of heavy periods with gynecological causes ruled out, easy bruising and bleeding gums. However, it took four more years of suffering with the symptoms of anemia, low ferritin, and heavy periods, one unnecessary surgical procedure (the ablation), and a preventable surgical complication that required a subsequent surgery (I had a major internal hemorrhage after excision surgery for endometriosis and removal of my left ovary and tube) and three more requests for hematology referrals, before I was finally referred to a hematologist and ultimately diagnosed with a bleeding disorder. And some studies show that the diagnostic delay from onset of bleeding symptoms can be up to 16 years! It is time for this to change. Gynecologists need to consider the possibility of bleeding disorders, and work with hematologists when appropriate, when trying to diagnose the underlying causes of menorrhagia.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.