Symptoms of pain related to the bladder, urinary urgency and/or frequency affect up to 12 million Americans and can range from uncomfortable to extremely debilitating. These symptoms can affect both men and women, although they are more common in women. Although these symptoms can be difficult to treat because there is no particular treatment that works for a majority of individuals, a range of treatment options do exist. With patient, physician, and sometimes other healthcare providers working together to explore options, relief from bladder symptoms can be achieved.
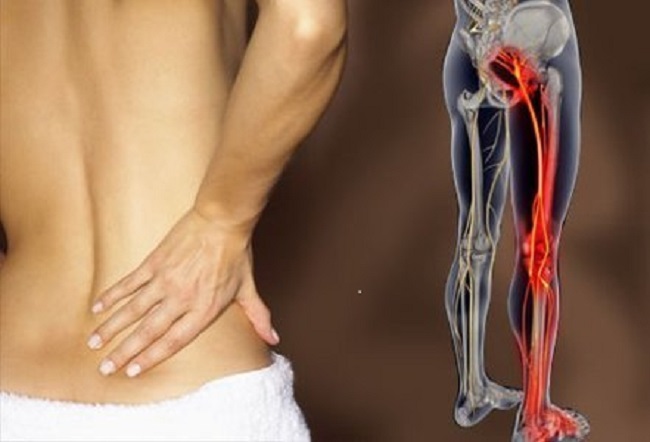
Symptoms of bladder pain syndrome – interstitial cystitis include recurring pelvic pain, pressure or discomfort. Pain may worsen with specific food or drinks, and with bladder filling. Pain can be specifically located in the bladder, urethra, or vagina, and/or more generally present in the lower abdomen, pelvis, and lower back. Pain with sexual intercourse is a common symptom. Urinary frequency (the need to urinate frequently) is often present and can be extreme, with some patients needing to urinate up to 60 times per day. Urinary urgency (a strong need to urinate) can also be present. This can also be accompanied by spasms.
Interstitial cystitis, the original name for this disease, had fairly strict diagnostic criteria that did not encompass all patients with this similar set of bladder symptoms, so other names have been proposed including painful bladder syndrome (PBS), bladder pain syndrome (BPS), and hypersensitive bladder syndrome. Some doctors now use the name interstitial cystitis to encompass all patients with bladder pain symptoms not from other causes (such as infection), and some doctors use the newer nomenclature such as bladder pain syndrome. Some doctors use the term interstitial cystitis to refer only to a subset of patients who have ulcerations in the wall of the bladder called Hunner’s ulcers. These differences can be confusing to patients.
Diagnosis of BPS can be challenging, since patients can present with a wide variety of symptoms, and the symptoms often overlap with other pelvic diseases such as endometriosis and adenomyosis. BPS is usually diagnosed through the clinical signs and symptoms of the patient, and by ruling out other conditions such as bladder infection and bladder cancer. In the past, cystoscopy with hydrodistention (slowing filling the bladder with fluid, then looking at the bladder wall using a camera scope), and the potassium sensitivity test, have been used to diagnose BPS, but these tests are no longer recommended because they can trigger additional pain in patients, and they are sometimes negative even in the presence of disease.
There is no cure for BPS, and treatments are directed at symptom control. The American Urological Association (AUA) recommends trying treatments in order from least invasive to most invasive. Treatments required for any individual may vary over the course of time, and sometimes multiple treatments at once may be used. The first line of treatments include education about normal bladder function, and self-care strategies to help manage bladder pain. An important self-care strategy for many BPS patients is to avoid dietary food triggers. There are some foods such as citrus, vinegar, tomatoes and coffee that are common triggers in individuals whose bladder pain is affected by diet; however, it is important to identify your own individualized food triggers, since they may be different for different individuals.
The second line treatments recommended by the AUA include manual physical therapy, and certain medications– both oral medications, and medications delivered via catheter to the bladder. Manual physical therapy should be performed by a pelvic floor physical therapist trained in manual therapy techniques, and Kegel exercises should be avoided. Oral medications include amitriptyline (an antidepressant sometimes used to treat pain), and antihistamines. Intravesical medications (delivered by catheter to the bladder directly) include heparin, lidocaine, and DMSO.
Third line treatments become more invasive, and include cystoscopy with hydrodistention, and surgical treatment of Hunner’s ulcers if found. Fourth line treatments include surgically implanted electrical nerve stimulators. Additional treatment possibilities include cyclosporine (an immunosuppressive drug), Botox injections, and surgery to remove the bladder. These options can have significant side effects and complications, so they are only undertaken when no other treatment strategies have worked. Pain management strategies should be used at all stages of treatment, and include over the counter and prescription painkillers, as well as stress management techniques and physical therapy.
Individuals with BPS may be more likely to have certain other diseases as well. It is highly associated with endometriosis, with some studies suggesting that up to 80 percent of patients with endometriosis also have BPS/IC. Individuals with allergies, migraines, or asthma may have a greater chance of developing BPS/IC. BPS/IC is also strongly associated with irritable bowel syndrome, and is also associated with vulvodynia, fibromyalgia, chronic fatigue syndrome, and lupus.
Recent research indicates that different pain syndromes often occur together in the same patient, often as well as other systemic diseases. As the relationships between various pain syndromes and different diseases become better understood, this may lead to new and better treatment options that are able to treat the whole individual rather than trying to treat each separate syndrome, in patients who have multiple diseases. One common frustration in patients with multiple diseases is that each specialist only looks at and treats their own clinical area, and then patients themselves have to coordinate care between specialists and different approaches, which may sometimes even conflict with each other. Many patients would welcome the change to treat and understand their body as one system, with the help of specialist health care providers who understand the relationships between different diseases and different parts of the body. Unfortunately, this type of integrated care delivery is currently only available to patients with certain life-threatening conditions such as cancer or heart disease, and only in the most advanced hospital systems. For now, patients with BPS/IC have to take charge of managing their own way through their treatment options.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
This article was published previously on Hormones Matter on September 11, 2014.