Have you, or possibly your partner, ever wondered if there really was a link between your menstrual cycle and sexual attraction? Perhaps you have noticed that during certain times of the month something is not quite right and whatever it is, it seems to affect your ability to concentrate. Scientists have as well.
Evolution, the Menstrual Cycle, and Sexual Attraction
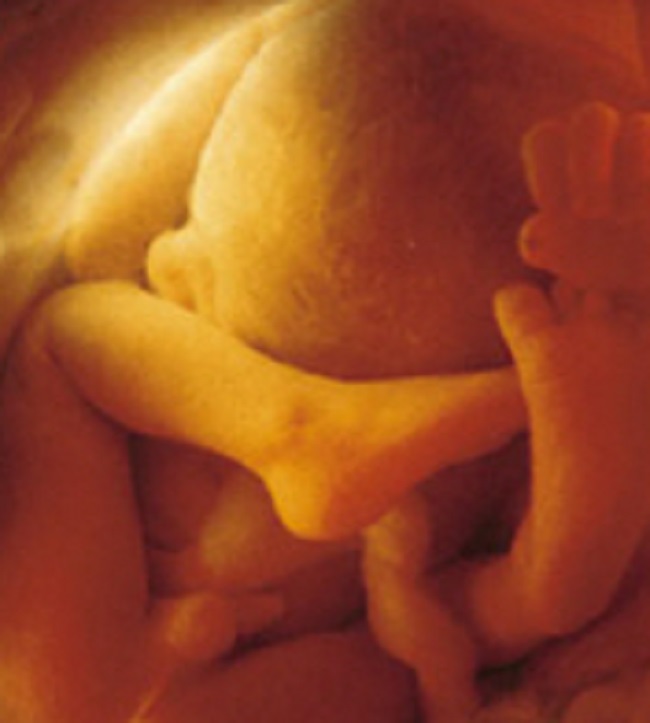
Since the dawn of humankind, women have been programmed to think and act in such a way that helps us find the perfect mate with the best genes to make the best babies; survival of the fittest. However, the conditions and interactions are not as clear-cut today as they were during caveman times. Women are educated and have careers. We work hard and we play harder. In other words, we might be too busy to think of finding a man and having children, at least on a conscious level.
Researchers have found that reproductive hormones are still at play when it comes to how we feel about certain situations, view the world, and interact with others. During the week before ovulation, women have improved memory, perhaps to signify the right time to find “The One,” but also to help you make better decisions and navigate your environment. Near ovulation, women may have a heightened sense of smell, possibly to sniff out potential toxins. Additionally, several studies have shown that women who are in the fertile window tend to dress and feel more attractive as compared to other times in their cycles. A major drawback to this process is that some women may be highly sensitive to to the cyclic rise and fall of their hormones and experience negative mood symptoms, increased food cravings, and susceptibility to stress, particularly during the premenstrual phase.
Oral Contraceptives and Sexual Attraction
What about the pill? Oral contraceptives (OCs) contain synthetic hormones that may also affect women’s social behavior and psychological functioning. In my own research, I have found that women who are on the pill show greater attraction toward current and potential mates across all phases of the cycle. Naturally, this could be due to the simple fact that women using OCs expect to have more sex than those who are not. However, we also found that an increase in androgens, a side effect of the pill, was significantly related to this increase in attraction.
Because of our genetic make-up, women must go through regular shifts in their cognitive abilities, moods, and behavior. In other words, we think, feel, and react differently based on what our hormones are doing. This may translate to women’s approach to relationships, sexual arousal, and motivation to seek out mates. But also, it affects how we work, talk to friends, and deal with our problems.
Does this mean women should plan their activities accordingly? That may be a tad extreme, but maybe it will help both men and women understand why sometimes we are just not in the mood.