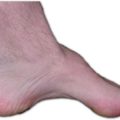
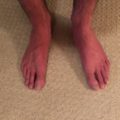
I am 41 years old and experiencing weird, scary, and upsetting symptoms that began a year and half ago. I have numbness in my feet that has moved up into my calf and super tight calves, ankles and feet. I have peripheral neuropathy, carpal tunnel symptoms, circulation issues without swelling and some sciatica like symptoms with achiness in my legs. I am exhausted all of the time, have no energy and symptoms of depression, but I am not depressed other than these health issues. I am overly irritable and always cold. My hair is falling out and I become dizzy when I standup from a sitting position.
In the past, I believe at some point I had insulin resistance but was never diagnosed. I did, however, have issues with my blood sugar. I was put on Metformin for 6 years, during which time I had a lot of stomach issues, nausea, and diarrhea. I was never a big drinker at all, nor did I use tobacco. I was under a ton of stress for many years though. Despite the stress, I was always healthy and worked out, ran on a treadmill, and was active. I worked as a nanny 55 hours a week.
My diet before metformin was not the greatest with lots of carbs and processed foods. I may have had a thiamine deficiency back then and but did not know about it. No one ever tested me for thiamine until recently. A lot of my symptoms started at a time where I was dealing with some heavy things, so I believe stress was definitely involved. For the past three years, I have not been on medication. Currently, I eat a low carb/keto diet and my A1c is 5.2 and insulin is 3.
Discovering Thiamine Deficiency
I started to experience these symptoms about a year and a half ago. I have tried many things to feel better and help with my symptoms and nothing has worked. Of the nutrient testing that I have had, my thiamine was low. It was 66nmol/L. The reference range was 78-185nmol/L. My vitamin D was barely above the deficiency range at 30ng/mL, my methylmalonic acid was on the low end of the range at 107nmol/L (range 87-318), and my vitamin B6 was high at 29.5ng/mL (range 2.1-21.7). Nothing was discussed regarding the other low vitamins and high B6. I was, however, told by my neurologist to take 100mg a day of vitamin B1/thiamine. She never indicated that this was the reason for my symptoms though.
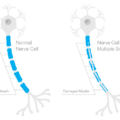
I began doing my own research and found that I had all of the classic symptoms of dry beriberi – thiamine deficiency that affects the nerves. In other words, my symptoms were related to thiamine deficiency. I began supplementing with Benfotiamine 600mg a day am taking magnesium (Optimum health) at 150×2= 300 at night. My FM doctor said my magnesium was at 4.5 and they like to see it at 5.3. I also take vitamin D3/K2. My vitamin d was on the low side.
When I began supplementing with thiamine at 100mg per day and the Benfotiamine, I notice I was not as tired or fatigued. I was feeling pretty weak there, and I feel better, but the nerve issues have not changed.
Six weeks after finding out I had a thiamine deficiency, I got bloodwork from my FM doctor and my thiamine was now too high, almost as if I wasn’t absorbing it. I should mention that the second test was a plasma test while the first test was done from the serum. From what I have learned, plasma thiamine measures are less accurate. Even so, should I be worried?
My FM doctor wants to test again for Lyme disease. Beyond that, I just don’t know what else to do to resolve the nerve issues. Thank you!
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Image by Daniel Reche from Pixabay.