There are many misconceptions about the after effects of hysterectomy. There are a number of reasons for this. First and foremost, gynecologists are not honest with women. They present hysterectomy as merely the end of our ability to have children. A bonus is no more periods. Secondly, their professional society, ACOG, has a lot of influence on government and the media. Therefore, much of the information women find also misrepresents hysterectomy as benign. And last, but not least, most hysterectomized women fail to share the after effects. So it is no wonder secrecy abounds.
Over the years, I have written about many of the deleterious after effects of hysterectomy here, here, and here. Read the comments on any of these articles and see the thousands of women who have suffered. Among the least well recognized of these effects, however, are the figure changes that develop post-hysterectomy; changes that are related to both the anatomical effects of the surgery itself and the hormonal decline that ensues. Figure changes are hysterectomy’s best kept secret.
How Hysterectomy Changes a Woman’s Figure
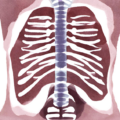
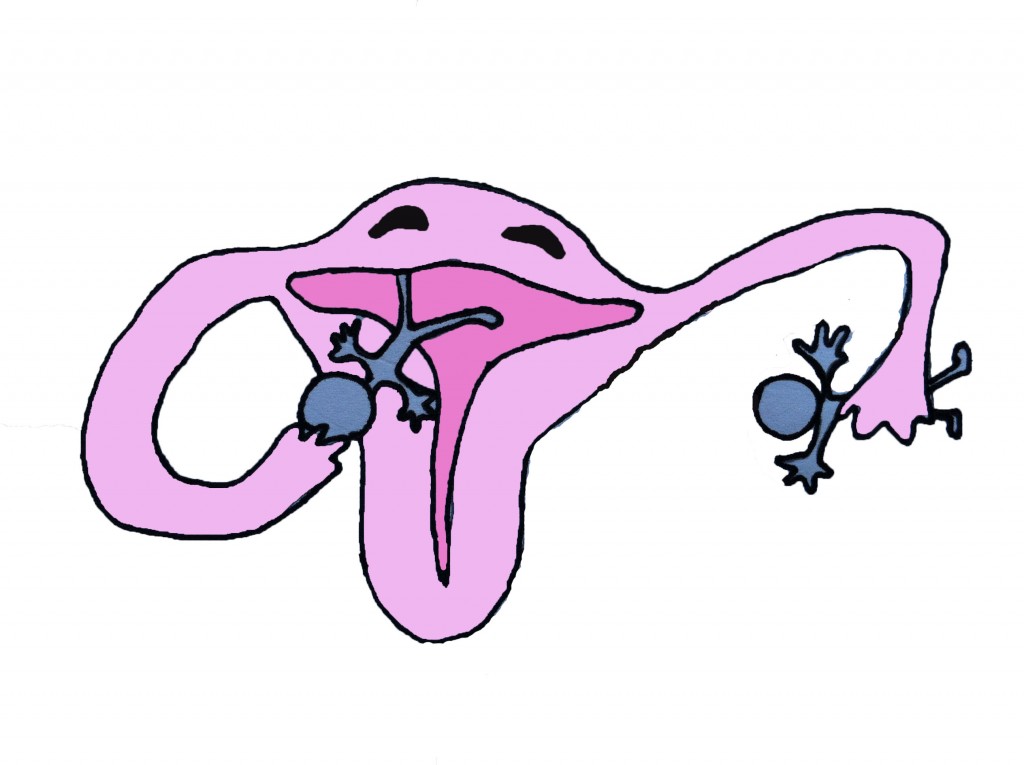
How does hysterectomy change a woman’s figure? The “bands” (medically known as “ligaments”) that suspend the uterus are also the support structures for our midsection. They keep the spine, hips, and rib cage where they belong. The severing of these ligaments causes our entire torso to collapse. The hips widen, the spine collapses, and the rib cage drops onto the hip bones. This causes a shortened and thickened midsection, protruding belly, and a loss of the curve in our lower backs.
These unnatural changes lead to back and hip problems, loss of mobility, poor circulation in extremities, and chronic pain. Nerve injuries are another source of pain and loss of mobility. “Hysterectomy cripple” is a term from an old gynecology textbook that reverberates in my head. Two of my articles and readers’ comments on this best kept secret can be found here and here. Some women also talk about these changes here.
Other Harms of Hysterectomy
The uterus is essential for a woman’s whole life to keep her healthy. So are the ovaries. And the Fallopian tubes. We were not made to be disassembled. Studies prove it. Yet gynecologists continue to treat the female sex organs as disposable.
Although hysterectomy’s best kept secret is figure changes, there are a number of other harms. Hysterectomy’s effects on the bladder and bowel are explained here. Many women report sexual dysfunction including loss of desire. Feelings of emotional emptiness are common. So is chronic fatigue. Even the ovaries (vital endocrine glands) don’t escape unscathed. Their impaired function causes a whole other set of problems related to the diminished supply of vital hormones. For many, these life altering changes cause break-ups of romantic relationships and families. The effects can also end careers leading to financial hardship and shattered lives. The societal effects are far-reaching.
It is one thing to have cancer and have to live with these trade-offs. But over 90% of these surgeries are unnecessary since less than 8% are done for cancer.
Why Do We Not Know About the Figure Changes?
How can we not know that hysterectomy causes figure changes? Shouldn’t we have noticed this in women who had hysterectomies? Yes and no. Women gain an average of 25 lbs. in the first year after hysterectomy according to the HERS Foundation. That can certainly mask figure changes. Not only that, the torso collapses gradually so is not immediately discernible. And women tend to dress differently in an attempt to hide their altered figures. For women we didn’t know before their hysterectomies, we have no “before” view. Conversely, how much does any woman really critique other women’s bodies anyway? Not so much. Nor can we count on women to divulge these changes just as they fail to share other effects. Proof of this association does not require studies as it is evident from diagrams of the female anatomy. Hence, the reason hysterectomy’s best kept secret is figure changes.
So Much Despair
I had a hysterectomy 13 years ago at age 49. The effects were immediate and severe – physically, mentally, and emotionally. I never could have imagined that a person could age so quickly or feel that their very heart and soul were ripped out! You can read my story here. I quickly realized that my gynecologist of 20 years was dishonest about the consequences. And my medical records show that he also lied about my diagnosis and treatment options.
The changes to my figure amplify the despair that has plagued me since that fateful day. Like the author of the book Misinformed Consent, I cannot bear to look at myself in the mirror. And I shudder to think how much more height I will lose from my already small frame. Even more unsettling is the recent onset of hip and leg pain and midsection discomfort. I fear that reduced blood flow is causing my hip joint to deteriorate (known as “avascular necrosis” or “osteonecrosis”). I know some hysterectomized women who had hip replacements in their 40s or 50s for this reason. Great… more worries about my future health. The thought of any medical treatment, especially surgery, terrifies me!
The Harm of Female Organ Removal
There is long-standing evidence of the harms of female organ removal. Yet, nothing is being done to stop the abuse. It affects almost half of U.S. women. The states’ medical boards don’t care, and neither do legislators. Even women’s health organizations don’t care. Their platform is “reproductive choice.” I guess I was naive to think any of them would care. Then along came the #MeToo movement. I thought this was our opening to make our voices heard. But no. People don’t seem to view this as a form of sexual abuse or harassment. Evidently, perpetrators of surgical crimes against women get a free pass.
The ACOG works hard lobbying Congress and the media to keep it that way. One only need look at the Advocacy menu on their website. Hysterectomy is a big money maker. So maximizing these surgeries and denying the harm is in gynecologists’ best interest. The recent increase in resident minimum requirements from 70 hysterectomies to 85 is evidence of this. There is no training for myomectomy, or removal of fibroids, despite fibroids being a common reason for a hysterectomy. A gynecologist petitioned the ACOG to mandate myomectomy training, to make this uterine-sparing option more accessible. The ACOG rejected his petition. Clearly, the Ob/Gyn specialty puts profits before women’s health.
One has to question why insurance companies continue to authorize and pay for so many unwarranted hysterectomies. What documentation are gynecologists submitting to get these authorizations? My insurance company refused to divulge what my gynecologist submitted to get authorization. I had an ovarian cyst yet my medical records show authorization for a “hysterectomy.” There was absolutely nothing wrong with my uterus or other ovary as proven by pre-op imaging and post-op pathology. He should have removed only the cyst.
Protect Yourself
Don’t allow yourself to be deceived or bullied by a gynecologist. If you do go into an operating room, protect yourself. Modify the consent form to explicitly state what can and cannot be done and removed. Have the surgeon(s) sign off on all revisions.
You certainly don’t want to endure a hysterectomy’s figure changes or any of the other negative effects. The HERS Foundation and Ovaries for Life are good resources for understanding the lifelong importance of the female organs.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, and like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Image by Tayeb MEZAHDIA from Pixabay.
This article was published originally on June 13, 2019.