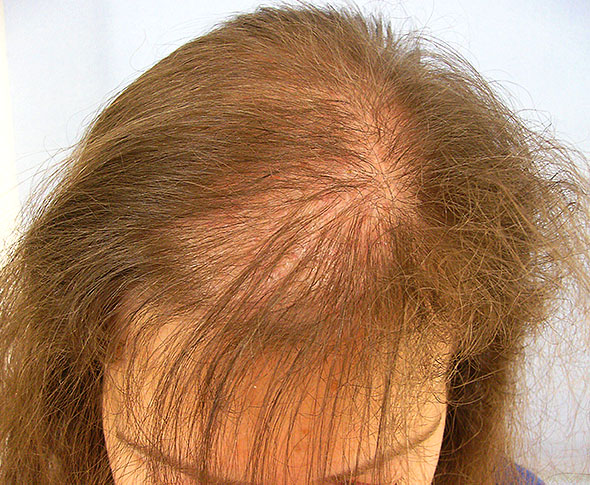
One of the core components of an HPV vaccine adverse reaction inevitably includes some degree of seemingly unexplainable but observable brain inflammation and white matter disintegration. The brain inflammation falls under a number of different names and diagnoses, some are regionally specific, cerebellar anomalies for example, while others demarcate a more diffuse injury including, acute disseminated encephalomyelitis (ADEM), myalgic encephalomyelitis (ME), sometimes known as chronic fatigue, multiple sclerotic (MS) type lesions and, the newest and perhaps more prescient among them, a set of conditions designated as Autoimmune/Inflammatory Syndrome Induced by Adjuvants or ASIA that denote chronic inflammation both centrally and peripherally relative to vaccine adjuvant exposure.
Is the Brain Immune Privileged?
Despite the observance of brain inflammation in many post HPV vaccine victims, many practitioners, and indeed, the FDA and CDC, seem loathe to recognize that an aluminum lipopolysaccharide adjuvanted virus vector might induce a neuro-inflammatory response, leaving patients with little recourse post injury. The difficulties attributing brain inflammation to a vaccine reaction stem from a long held belief that the blood brain barrier is stalwart in its protection against peripheral trespassers. The brain has long been considered, ‘immune privileged’ having little to no communication with peripheral immune function. Indeed, the perceived impenetrableness of the blood brain barrier is so extensive that brain-body separation might as well be complete, with a brain in bottle and a decapitated body.
Logically, we know this cannot be true. There must be crosstalk between the immune systems of brain/central nervous system and that of the body. How else could we survive if the two modalities were segregated so completely? It turns out, that logic may be prevailing. A decade of research suggests that the long held notion brain immune – privilege is completely and utterly incorrect. Indeed, the immune system not only guides early neurodevelopment (and so mom’s immune function matters) but communicates and affects brain morphological changes chronically. Likewise, signals from the brain continuously influence peripheral immune function.
The immune system appears to influence the nervous system during typical functioning and in disease. Chronic infection or severe illness may disrupt the balance of normal neural–immune cross-talk resulting in permanent structural changes in the brain during development, and/or contributing to pathology later in life. The diversity, promiscuity, and redundancy of “immune” signaling molecules allow for a complex coordination of activities and precise signaling pathways, fundamental to both the immune and nervous systems.
It should not be surprising then, that nutrient status and toxicant exposures in the periphery, in the body, affect central nervous system function and are capable of inducing brain inflammation and vice versa. And yet, it is; perhaps even more so than any of us realize.
Re -Thinking Brain Inflammation
When one reads through the definitions, research and case reports of ADEM, ME, MS or other instances of brain inflammation, the notion that biochemical lesions in the periphery are linked to observed neuro-inflammatory reactions is far from center stage. Nevertheless, if we can accept the premise what happens in and to the body does not stay in the body, then we can begin to re-frame our approach to brain inflammation. Specifically, we can look at inflammation more globally and ask not only what triggers inflammation, but allows inflammation to persist chronically, regardless of its location. If there is an on-going peripheral inflammatory response, is it not prudent to suspect that a similar response might be occurring within the central nervous system, even if our imaging tools are not yet capable of visualizing the inflammation; even if it is too premature to observe demyelination, neuronal, axonal swelling or other telltale signs of chronic brain inflammation? I think it is.
Vaccine Adjuvants: A Pathway to Brain Inflammation
With the HPV vaccine, and indeed, any vaccine, the deactivated viral vectors come with a cocktail of additional chemical toxicants and a metal adjuvant to boost the recipient’s immune response, as measured by the increase in post vaccine inflammatory markers. It is believed that without these adjuvants (and data back this up), the recipient’s immune response is insufficiently activated to merit ‘protection’ against the virus. The strength or size of the immune response is then equated with success and protection.
By this equation, an excessive immune response that continues chronically and is eventually labeled ‘autoimmune’ as innate systems begin to fail, is in some way not a failure or side effect, but an example of extreme success; the larger the immune response, the stronger the vaccine. And so, skewed as this observation may seem, within the current vaccine-paradigm there can be no ‘side-effects’, not really. By design, there should be inflammation, even brain inflammation; the more the better. Also by design, metal, lipid soluble, adjuvants cross the blood brain barrier and directly induce brain inflammation. To say vaccines don’t or somehow couldn’t induce brain inflammation is ignorant, if not, utterly negligent, and quite simply, defies logic. Again, for prudence and safety, shouldn’t we assume that an inflammatory reaction in the body might also ignite some concordant reaction in the central nervous system?
Why Aren’t We All Vaccine Injured?
What becomes apparent though, is even with exposure to the most toxic brew of vaccines, not all who receive vaccines are injured, at least observably. (I would argue, however, even those who appear healthy post vaccine, had we the tools to observe brain inflammation more accurately, would show a central inflammatory response, at least acutely, and likely, progressively). So what distinguishes those individuals who seem fine post vaccine, particularly post HPV vaccine, from those who are injured severely and sometimes mortally?
More and more, I think that the fundamental differences between vaccine reactors and non-reactors rest in microbial and mitochondrial health. Indeed, all vaccines, medications, and environmental toxicants damage mitochondria, often via multiple mechanisms, while altering microbial balance. Whether an individual can withstand those mitochondrial insults depends largely upon a balance struck among three variables: 1) heritable mitochondrial dysfunction, genetic and epigenetic; 2) the frequency and severity of toxicant exposures across the lifetime; and 3) nutrient status. Those variables then, through the mitochondria, influence the degree and chronicity of inflammation post vaccine. With the HPV vaccine in particular, the timing of the vaccine, just as puberty approaches and hormone systems come online, may confer additional and unrecognized risks to future reproductive health.
Mitochondria and Microbiota
The mitochondria, as we’ve written about on numerous occasions, control not only cellular energy, but cell life and death. Every cell in the body, including neurons in the brain, require healthy mitochondria to function appropriately. Healthy mitochondria are inextricably tied to nutrient concentrations, which demand not only dietary considerations but balanced gut microbiota. Gut bacteria synthesize essential nutrients from scratch and absorb and metabolize dietary nutrients that feed the mitochondria. Indeed, from an evolutionary perspective, mitochondria evolved from microbiota and formed the symbiotic relationship that regulate organismal health. Disturb gut bacteria and not only do we get an increase in pathogenic infections and chronic inflammation, but also, a consequent decrease in nutrient availability. This too can, by itself, damage mitochondria.
When the mitochondria are damaged, either by lack nutrients and/or toxicant exposure, they trigger cascades of biochemical reactions aimed at conserving energy and saving the cell for as long as reasonably possible. When survival is no longer possible, mitochondrial sequestration, and eventually, death ensue, often via necrosis rather than the more tightly regulated apoptosis. Where the mitochondria die, cells die, tissue dies and organ function becomes impaired. I should note, as steroid hormone production is a key function of mitochondria, hormone dysregulation, ovarian damage and reduced reproductive capacity may be specific marker of mitochondrial damage in young women.
Mitochondria and Inflammation
Mitochondria regulate immune system activation and inflammation and so inflammation is a sign of mitochondrial damage, even brain inflammation. Per a leading researcher in mitochondrial signaling:
The cell danger response (CDR) is the evolutionarily conserved metabolic response that protects cells and hosts from harm. It is triggered by encounters with chemical, physical, or biological threats that exceed the cellular capacity for homeostasis. The resulting metabolic mismatch between available resources and functional capacity produces a cascade of changes in cellular electron flow, oxygen consumption, redox, membrane fluidity, lipid dynamics, bioenergetics, carbon and sulfur resource allocation, protein folding and aggregation, vitamin availability, metal homeostasis, indole, pterin, 1-carbon and polyamine metabolism, and polymer formation.
The first wave of danger signals consists of the release of metabolic intermediates like ATP and ADP, Krebs cycle intermediates, oxygen, and reactive oxygen species (ROS), and is sustained by purinergic signaling.
After the danger has been eliminated or neutralized, a choreographed sequence of anti-inflammatory and regenerative pathways is activated to reverse the CDR and to heal.
When the CDR persists abnormally, whole body metabolism and the gut microbiome are disturbed, the collective performance of multiple organ systems is impaired, behavior is changed, and chronic disease results.
Reducing Inflammation
Instinctively, we think reducing inflammation pharmacologically, by blocking one of the many inflammatory pathways, is the preferred route of treatment. However, this may only add to the mitochondrial damage, further alter the balance of gut microbiota and ensure increased immune activation, while doing nothing to restore mitochondrial and microbial health. In emergent and acute cases, this may be warranted, where an immediate, albeit temporary, reduction in inflammation is required. The risk, however, is that short term gains in reduced inflammation are overridden by additional mitochondrial damage and increased risk of chronic and/or progressive inflammation. The whole process risks becoming a medical game of whack-a-mole; a boon to pharmaceutical sales, but devastating to those who live with the pain of a long-standing inflammatory condition.
In light of the the fact that damaged mitochondria activate inflammatory pathways and that vaccines, medications and environmental toxicants induce mitochondrial damage, perhaps we ought to begin looking at restoring gut microbial health and overall mitochondrial functioning. And as an aside, perhaps we ought to look at persistent inflammation not as an autoinflammatory reaction, but for what is it, an indication of on-going mitochondrial dysfunction.
We Need Your Help
Hormones Matter needs funding now. Our research funding was cut recently and because of our commitment to independent health research and journalism unbiased by commercial interests we allow minimal advertising on the site. That means all funding must come from you, our readers. Don’t let Hormones Matter die.
Yes, I’d like to support Hormones Matter.
This post was published originally on Hormones Matter on September 22, 2014.