The Mayo Clinic terms pain associated with sexual stimulation or vaginal contact as “sexual pain disorder,” and categorizes this as a type of female sexual dysfunction. More commonly we speak of “dyspareunia” to refer to pain with sex. It can present in a number of different ways; it may be internal or external, it may or may not prevent orgasm, and it may even occur after sexual activity.
Unfortunately, pain with sexual activity is rarely discussed or considered seriously. I’ve sat face to face with health care professionals who tell me that the primary cause of pain is that the women’s partner is too large for her. Sexual dysfunction in women is typically treated as either an inevitable “female problem” or an emotional disorder requiring antidepressants or anti-anxiety medications.
Pain is not uncommon, and it is treatable. Consider how many people suffer low back pain, headaches, or stomachaches. Imagine how much effort goes into diagnosing and treating these issues. Why then would we not be just as open about discussing and treating female sexual pain? Given the complexity of the anatomy, which I outline below, and the intersections of hormones, pregnancy and childbirth, postural habits, and the possibility of infection and trauma, it should be no surprise that many women experience pain or other dysfunction.
In my experience as a physical therapist, I find that while some women seek treatment, most either presume it is normal or don’t realize that there are treatment options. I can’t tell you how many times a woman will report “no” to sexual pain on my intake forms, then later during the evaluation report with surprise “I have had that pain my whole life, I thought it was normal!”
I will say now what I always tell these women: with the possible exception of disruption of a hymen or a significant size difference between partners, discomfort during sexual stimulation is never considered normal. And even in these situations pain is not inevitable, and should never be allowed to continue as this can result in further trauma and future discomfort.
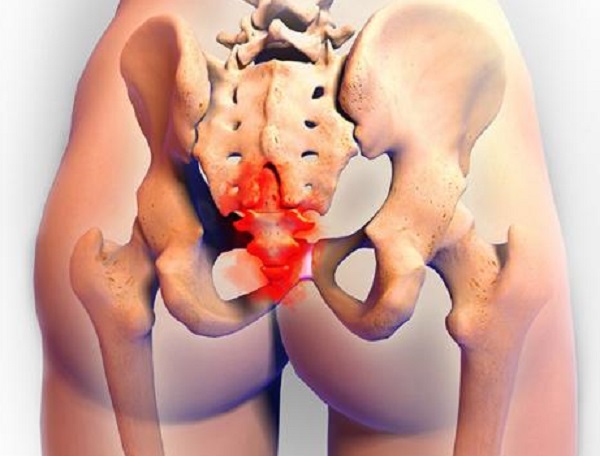
First, an overview of the anatomy. The external female genital area is composed of muscles known as the pelvic floor, as well as extensive nerves, glands, and other soft tissue. The muscles work to support of organs against gravity, for control of urination and bowel movements, and for sexual function. In the pelvic floor, there are three separate openings: the urethra, the vagina, and the anus. The clitoris, which is composed of highly sensitive erectile tissue, functions solely for sexual stimulation. It is covered by a “hood” of soft tissue externally, but also extends internally. The entirety of the labia, external clitoris, and vaginal opening are known as the vulva. Internally, the vagina extends to the uterus.

Clearly, this is a complex area, with many functions, and it makes sense that there might be many possible locations and causes for discomfort. Pain may be experienced with initial penetration or superficial stimulation, with deep penetration, with orgasm, or after orgasm. I will briefly overview some of the possible causes of each. In a subsequent article, I will address strategies for dealing with some of these causes, from the perspective of a physical therapist specializing in women’s health and pelvic rehabilitation.
A thorough examination by a gynecologist is always the first step in assessing pelvic pain, as not all causes of pain can be treated with physical therapy.
Superficial Sexual Pain
Sexual pain may be experienced with initial (shallow) penetration or with light touch to the vulva, perineum, or anus. It may feel like burning, stretching, or sharp stabbing discomfort. It may increase or dissipate if sexual activity continues. It may even be intense enough to prohibit all touch.
Decreased lubrication, related to hormone changes or lack of physiologic arousal, may cause pain with initial penetration (arousal includes increased blood flow to the genital area as well as increased lubrication). Thinning of vaginal tissues, known as atrophy, often occurs with hormone shifts associated with menopause, and may result in discomfort and light bleeding with penetration if adequate lubrication is not present.
Active infections can cause sensitivity and irritation of the vulva and vagina. These infections may be acute, or low-level and chronic. Even after infection has resolved, residual irritation or fascial restrictions within the tissues can cause pain.
Sensitivity to perfumes and dyes, such as in laundry detergent, pads, or tampons, can cause irritation and sensitivity. There are also skin conditions that may cause unusually fragile skin and pain to touch. Swelling of glands at the opening of the vagina may also occur and is frequently found in women with vulvar vestibulitis (pain and irritation at the opening of the vagina).
An intact hymen may be the cause of pain with initial penetration. However, given the variety of shape and thickness of the hymen, and the many activities that can change it over the course of a woman’s life from childhood to adulthood, pain with penetration during a woman’s first sexual encounter should not be presumed to be inevitable.
There may be atypical anatomy, such as thickened hymenal remnants or fascial bands that restrict the vaginal opening. There may also be scar tissue that is restricting the vaginal opening, due to trauma, tearing during childbirth or episiotomy.
Tightness of the muscles of the pelvic floor can cause pain with initial penetration. This pain may be right at the opening of the vagina or referred to other areas. In severe cases, this is known as vaginismus, which is an involuntary spasming of the muscles that prevent penetration. It can be associated with hypersensitivity of the skin and muscles so that even light touch in the genital area causes pain. Vulvodynia refers to chronic pain of the vulvar area without a known cause. It is often accompanied by tight pelvic floor muscles.
Deep Pain with Sex
Pain is often reported with deep penetration, and may be described as a deep ache, cramping, or as if a woman’s partner is “hitting something” in her pelvis.
The sensation of something being bumped or hit with penetration is often related to uterine positioning. The uterus may be tilted (which in some women is their normal anatomy, or in other women may be related to tight ligaments, scar tissue, or fascial structures). The uterus may also not be mobile enough to shift comfortably during sex. There may be scar tissue deep in the vagina that restricts vaginal or uterine mobility. Fibroids at the uterus may make it larger, asymmetrical, or less mobile and more prone to discomfort. Finally, the cervix may be sensitive due to fascial restrictions, surgical interventions such as colposcopy for abnormal cells, or irritation from IUD placement. In these cases changing sexual position or angle of penetration sometimes improves the discomfort, although in severe cases there may be no position of comfort.
Due to the proximity of the bowels to the vaginal canal, constipation or bowel irritation may result in pain with deep penetration. A sensitive or infected bladder may also be irritated for the same reason. Bowel pain may feel like cramping or a deep ache. Bladder pain may feel like a deep ache above the pubic bone, burning, or a painful bladder pressure.
Finally, active infections in the abdomen and pelvis may also cause pain with deep penetration. Acutely, infections and accompanying irritation can cause direct sensitivity and pain. In addition, chronic processes can cause pain due to adhesions that are formed with chronic inflammation. Endometriosis is an example of this. Adhesions restrict the movement of tissues and can put pressure on pain-sensitive structures. Unfortunately, adhesions are challenging to see on imaging, but they are palpable to trained therapists and physicians and are often visible when investigated surgically.
Pain with Orgasm
This type of pain is less common, but from my experience, it may indicate decreased mobility of pelvic structures, spasm or trigger points in pelvic floor muscles, or inflammation and irritation of pelvic structures.
Pain after Sexual Activity
Pain after sexual activity is often a response to irritation and trauma caused by the activity itself. In these cases, patients may experience pain or discomfort during activity and have it continue or worsen afterward.
In the case of a deep, heavy aching discomfort after sexual activity, pain may be related to venous congestion in the pelvis. During activity, blood flow into the pelvis increases, but for these women, the blood flow out cannot keep up just like swelling or varicosities commonly found in the legs. This may be directly related to inefficiencies of the veins themselves, but in many cases is related to scar tissue and fascial restrictions that restrict blood flow.
Clearly, there are many causes of discomfort with sexual activity, but for each cause, there are treatment strategies! There is no reason to accept discomfort as normal or inevitable. The first step in addressing pain is to visit a gynecologist well versed in sexual pain to rule out infection, fibroids, cysts, hormonal shifts, or other issues and to discuss treatment strategies. One strategy may be physical therapy, as specialized women’s health PT has excellent results in treating pelvic and sexual pain. In my next article, I will discuss which types of sexual pain can be treated with physical therapy, and what treatment may entail.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, and like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
This post was published originally on Hormones Matter on September 21, 2015.