Chronic lower back discomfort. Stiff neck. Pelvic floor dysfunction such as pain with intercourse or urinary incontinence. Inability to sit squarely or for long periods of time. Pain with bowel movements. These are symptoms I see commonly grouped together in patients coming for treatment. What is the connection?
The tailbone.
Although it is a common site of injury, often taking the brunt of our many childhood and adult slip and falls, the tailbone is unfortunately an under-evaluated source of pain and dysfunction in both men and women. Once injured it can cause pain in sitting, pain with bowel movements, pelvic floor dysfunction, such as pain with intercourse, or even cause reactions up the spine, all the way to the neck and head.
What Is the Tailbone?
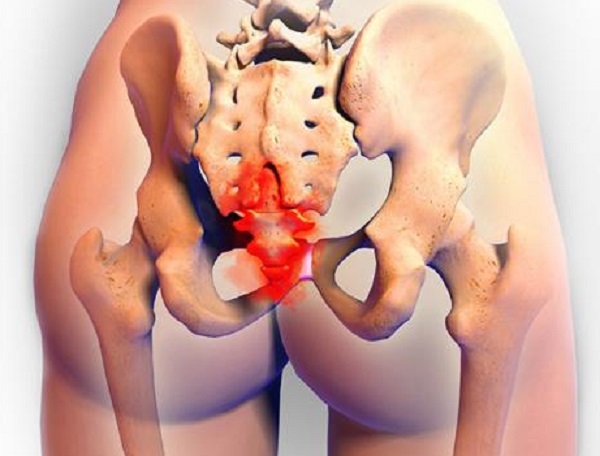
The coccyx, or tailbone, is the last piece of the spine. It is shaped like a triangle, and attaches to the sacrum by ligaments that run front, back, and both sides. To find your tailbone, just feel down your back, between the buttocks, until just above the opening of the anus.
In a healthy alignment it is mobile (moves slightly when pressed upon), center line, pain free, and continuous with the sacrum. However in a dysfunctional alignment it may be painful to touch it or the tissue around it, immobile, and even noticeably off-center. It may feel like it “points” deep into the body, rather than continuous with the rest of the spine.
How Does Tailbone Injury Happen?
Some patients know the moment they injured their tailbone. It is often a slip and fall, resulting in pain in sitting, and requiring the use of a donut pillow for some time until the irritation subsides. Usually, though, patients arriving with tailbone dysfunction cannot pinpoint a particular time that it was severely injured. They recall a multitude of childhood falls, none of which were particularly notable. And yet the tailbone is out of alignment and causing dysfunction.
Because the tailbone is attached to the rest of the spine by ligaments, it can be sprained just like any other joint. It can also be moved out of alignment. In many cases, a fall to the buttocks jams the tailbone forward, spraining the ligaments surrounding. As they heal the ligaments may scar down around the misaligned tailbone, effectively holding it rigidly out of place. Whether the fall was 2 months ago or 20 years ago, the tailbone may still be out of alignment.
What Are the Problems Associated With Tailbone Misalignment?
The most obvious symptom is coccydynia, or pain at the tailbone. However often patients have no pain at the tailbone until it is directly touched, and occasionally have no pain around it at all. This symptom may manifest as an inability to be comfortable in sitting. Often patients find themselves shifting from buttock to buttock in search of a comfortable position.
Pelvic floor dysfunction is common, as the pelvic floor muscles attach around the tailbone. Their ability to function optimally is affected by the positioning of the bones around them. Problems may include pain with intercourse, sensation of “tightness,” or pain with bowel movements. Bladder leaking may be aggravated by the inability of the pelvic floor to contract optimally.
Pain or tightness further up the spine is often a secondary symptom that patients don’t realize is connected. Since the spine and its contents are continuous from the skull to the tailbone, a tailbone out of place can affect alignment all the way up to the head. The most common two places I see this are the lower back and the suboccipital region, or area just below the skull on the back of the neck. Chronic nagging pain or tightness in these areas that shifts but never resolves despite care may be traced down to misalignment of the tailbone.
Treatment
The only way to treat most tailbone dysfunction is to work internally to mobilize the soft tissue around it and the joint itself. This is most directly done rectally, but sometimes can be accomplished vaginally. Pelvic floor physical therapists can do this, and some chiropractors and osteopaths may be trained to do it as well.
Why does this only work internally? Since the most common dysfunction of the tailbone is to be pushed forward by a fall to the buttocks, it needs to be mobilized in a posterior direction. This involves putting pressure on the front of the tailbone to move it back into place. In most cases the only way to access this angle on the tailbone is internally.
The therapist treating you should have specialized training to work internally, and have worked with tailbone issues before. As with all internal treatment, it is important that you feel comfortable and informed about what is happening. The practitioner will use a gloved and lubricated finger to mobilize your tailbone. You should be in a private room, draped for your comfort, and educated on what is found during evaluation and being done during treatment. Many patients are very anxious about being treated at or around the rectum. A skilled practitioner will be able to make your treatment as comfortable possible.
Does It Stay Fixed?
Usually, yes! Once the tailbone is mobilized it will not scar itself back into the old position unless there is a new injury. However, it is important to treat the ligaments, muscles, and bones around it as well, which may be contributing the dysfunction. Without treatment, these areas might pull the coccyx back out of alignment over time. The same concept applies to areas such as the lower back and the neck. Once the pressure of the misaligned tailbone is resolved, it is important to also treat the rest of the spine as it may have become tight or weak over time.
Often patients describe a sensation of “lightness” and ability to stand taller after being treated for tailbone dysfunction, as if a pressure was released. If you suspect that you have tailbone dysfunction, it is worth it to have an evaluation. You may find a connection piece in the puzzle for other symptoms you didn’t think were related.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
This post was published originally on Hormones Matter on September 10, 2014.













i slipped on the ice when i was 12, and landed right on my tailbone and i couldnt tell anyone beacuse i was off school property i suffered for weeks of pain and hovering over the deskseat, now whenmy back goes out i move my legs outward like a sumo and it pops back into place
Yes this is very true, also spiritually it related to kundalini and is related to the grounding of energy from the spine into the earth. And misalignment also causes issues with psychology and an inability to feel connected to the earth, which manifests as fear. If you use your voice tone of “TINNNNN TNYNNNNNG” in your most powerful vibration tone resonance (men low and women higher) basically whatever register works best – for me will be lower register for example, it will naturally move into place as these vibrations relax the muscles of the coccyx and allow it to find its natural placing. More extreme misalignment needs physical push. But this also works quite well and is a powerful method a friend taught me. Do this while standing relaxed. You will feel it if you get the tones right. Other ways to help alignment is to squat poop or use a cushion with hole around the coccyx in your car as western poop sitting actually causes the feces to push against the coccyx and squat pooping is an amazing natural healing technique as the defecation method allows for the coccyx to find its natural alignment. Some will scoff at this but it really works. I promise.
I’m miserable. I slipped and fell on May 22. 2022 and still suffering. My boyfriend and I have attempted intercourse based on my suggestion I was on top. It seemed to be the most comfortable however the next 10days I was in horrible pain at the end on my day. My spine in the lower back region feels like it’s swayed I have sharp zings of intense pain and my legs struggle to allow me to stand or walk. I m scared I won’t be able to make love to the love of my life. It’s been months and I should be able to have my sex life back by now. It was vaginally sex so why am I having such trouble ?
Steven Becker, D.C. is a chiropractor in Los Angeles, California and specializes in treating tailbone injuries. Dr. Becker has been in practice for more than 30 years and treats multiple tailbone cases each week. Dr. Becker focuses on providing quality personalized care to resolve pain, restore function and mobility and allow patients to return to their daily activities as quickly as possible. If your coccyx pain has become chronic (persisting for more than 3-6 mo), you should know that it may be less likely to resolve by natural recovery alone and, therefore, is more likely to continue indefinitely. If this is the case for you, Dr. Becker would encourage you to try internal chiropractic tailbone manipulation. You can read more about it here: https://drstevenbecker.com/coccyx-pain-tailbone-pain-coccydynia/
Wow, this article was an answer to prayer this morning. I was starting to think I would always have tailbone pain. I woke up 6 months ago with random tailbone. I was completely fine the previous day, and did not fall or do anything to injure. I’ve done general physical therapy with no improvements, and the chiropractor I went to actually made it worse. Thank you for this information. It’s such a relief to find out I’m not the only person who has gone through all this, and that there is a treatment. I am hoping there can be an effective external treatment, but at this point, I would do anything. It is also nice to know that my pelvic pain is also linked to my tailbone pain, and not a separate issue!
I’m in high school and I play a lot of sports. One or two years ago my tailbone started to irritate me, it feels fine when I am just running, laying or sitting up, but when I lay back on the tailbone or do an exercise where I need to put pressure on it, I can’t hold it for long because of the pain. Also I can feel a bump there that hurts when you press on it. Also I have minor pectus carinatum which just is a defect where my chest bones protrude. I’m wondering if those are related and also if I need to get treatment to prevent back pain in the future.
I am feeling same issue recently after I fall on ground please tell me what to do next
Good luck with getting treated by any orthopedist. I went to an orthopedist who ordered an x-ray. The x-ray technician commented that my tail bone was misaligned but it was up to the doctor to give me a diagnosis. The doctor said he found nothing. When I asked him about the tail bone he said that was not part of his investigation.
i have had a long-standing problem with purported gout, only recently to find it is with oxalates (brain fog, fatigue, dehydration, joint pain, bloating, etc. My GP doctor said I was fine and would live to 100 because my arteries were clear. I told her they were clear because I couldn’t eat anything without all the above symptomatology. Blood tests were not helpful because my reaction to oxalates was after I ate, not when fasting before a blood test.
Moral of story: you are on your own when it comes to chronic health conditions or something like tail bone mis-alignment.
Thank you for leaving that comment. Everyone needs to know or be reminded that doctors don’t look at everything and a lot of times totally look past things, not always aware of doing such. We all think “professionals” look at every possible factors. That word “professionals” causes us to easily forget, that they are still people, and are no different than anyone, we all make mistakes or sometimes don’t put two n two together.
It’s not that at all the culture with drs is not to listen and brush ppl off. If they would listen and care to investigate together with the patient. Less ppl would suffer for years and years with their lives wasting away.
i have exactly the same problem, can also see mine let alone feel it :/ makes all my clothes sit funny (which makes me paranoid since i have no butt to try hide it :/) wondering if anyone will reply to the questions asked :/
Hi I was wondering if you could advise. I had a back injury way back in 1994, when i was 17 and bumped my way down about 12 stairs after losing my footing, i was in severe agony and bad bruising, i finally went to my gp after about a week to be told id probably cracked the tailbone and itll heal by itself, just to rest as much as i could (i was a trainee hairdresser so standing was my normal day :/ ) anyway it did heal but instead of being inwards it sticks out lots to the point i have a bump where there shouldnt be a bump (makes me self conscious to wear tight fitting clothes, as i am slim its very noticeable).
I have suffered years and years of back pain,sciatica, and neck pain (even sometimes when i yawn its like the top of my spine cracks ) A couple of yrs ago a physiotherapist was checking my back and pushed down so hard on my tailbone i thought i was going to snap, the pain was unbelievable for her to then claim (oh its not going to move is it – yeah i coulda told you that) Anyway any advice on what to say to the doctor or what can be done? Id love to be able to wear normal clothes with confidence, but mostly to be able to sit properly or lie flat on my back (which i cant do, i have to slightly turn my pelvis so im resting on one butt cheek)
Sorry for long post. YIA
I’ve had issues off and on for years now. I will say that having a good chiropractor has helped tremendously. Everytime I start having pain in neck, back, hips, I know I need an alignment. Key though is to keep your core strong to hold it all in place
I’ve been having severe pain with my tailbone since at least September, 2018. I recently had a CT scan it showed that my tailbone is angled more than normal. Is this an issue that is fixable?
Is it possible for this to result from pregnancy? When I was pregnant with my youngest, I had terrible pain on my coccyx. It felt as though his head was crushing my tailbone for the entire third trimester. He ended up being 2 weeks overdue and delivered by emergency C-section because I wouldn’t dilate (even with an induction and having had 3 children prior to him) and the pressure of contractions was putting too much strain on his head. Since then my tailbone has been severely pointing to the left. They never mentioned his head positioning as a reasoning for the difficulties with his birth, but that is when the pain and my symptoms began. Could this occur without an impact? Could the prolonged pressure of his head have moved it out of alignment?
Hi WS ,
The excellent informative post you have shared on this page about the injured rarely treated tailbone injury with starting of proper treatment by the concerning of therapist treating you should have specialized training to work internally, and have worked with tailbone issues before. As with all internal treatment, it’s important that you feel comfortable and informed about what is happening. The practitioner will use a gloved and lubricated finger to mobilize your tailbone. You should be in a private room, draped for your comfort, and educated on what is found during evaluation and being done during treatment. Many patients are very anxious about being treated at or around the rectum. A skilled practitioner will be able to make your treatment as comfortable possible.
Thanks.
I fell on stairs 5 and half weeks ago. I was bruised bad so put off going to the dr. Went this week and xray did not show any sign of fracture but my tailbone area and back directly above butt crack is still sore. As I am now also having some episodes of sciatica pain down left leg. An anti inflammatory shot and steroid shot didn’t help so I am now on oral steroids. Should this help? What should I do?
About a year ago I had issue to empty completely my stool in the rectum area.
Stool got stock, I got bloating stomach, with a lot of gas when laying down sitting is giving me pain as I have the impression that something is pushing against my rectum or lower colon.
There a strait mark on my stool also.
We did many exam, never really find anything.
One of the pain Management doctor that I so mention to me that my tail bone was all crok when doing a injection into it.
I never really believed that could be the cause of my issue.
I am doing physical therapy right now work on my pelvic muscle which doesn’t help.
I leave in Corona 92883 California. I am with Kaiser.
Do you anyone in my area who could fix my tail bone ?
Please let me know
Thank you
Did you ever get clearer results of what might have caused this? Sounds a bit like my problem.
Have you looked into something called Disinersia? It’s a pelvic floor problem possibly caused by a fractured tailbone, but could be the result of other issues.
I’m curious if any studies have been done to look at spine, hip and tailbone “abnormalities” in women who have had hysterectomies. The severing of the uterine ligaments / pelvic support structures causes the spine to collapse and the hips to widen which is why women’s figures change after hysterectomy. This is all explained here – https://www.hormonesmatter.com/post-hysterectomy-skeletal-anatomical-changes/. Not long after my unwarranted hysterectomy, I noticed that my tailbone looked bruised and it still does 11 years. I now know that it’s because my whole spine collapsed causing the hysterectomy belly and loss of the curve in my lower back.
I am amazed at reading these symptoms and identifying with them all, Although I see all the comments are pretty much women it applies to men too I guess, I have been in intense pain on and off last 6 months with all the described symptoms, had MRI today after all other tests and xrays really didn’t show much will see what that shows. I had my issues start ten yrs ago when I tripped and didn’t even fall down, but jerked something really good, I had intense symptoms within hours, suffered over a year before it subsided but never to the point that I wasn’t aware of it mildly, didn’t have insurance at the time so just rode it out, then it started all over around 6 months ago only no outward indicators and kept saying that it feels internal and it seems to creep from mild low pain below the belt until I’m experiencing all symptoms described lasting for weeks with shorter periods of experiancing some relief only to reoccur and around I go again! This post has convinced me to persue this issue with Dr. as the likely cause of all my trouble, thank you so much for sharing this information.
my mother is 87. She broke her right hip December 3, 2017 out of the hospital December 9, 2017. I brought her home. She suffered a significant bed sore which we healed up and she was discharged from the wound clinic at the hospital the first of April 2017 and the skilled nursing for the bedsore and in home health PT. April 13, 2017 my mother fell straight on her bottom and the first dew days she voiced no pain suddenly she started with the pain. X rays showed no breaks. Is my mother too old for internal manipulation. One of my mothers main problems is urine comes out like a flood when she stands
I fell several times (after back to back pregnancies in 2002 & 2003) with the falls occurring between 2005 and 2010. I found unrelated DDD, stenosis, sciatica and a bulged disc, seemingly for no reason. Around 2012, I began to have Sacral/tailbone pain. I had xrays where they found my sacrum was tilted to the right. The PA I saw did NOTHING. I never even saw the xrays until last month. I was furious to see this abnormality but also that my coxxyx is curled inward completely. Finally, I was referred to Ortho. Next move is nuclear bone scan to look for fractures missed on xray. Thank you for sharing!
FYI I have everything you described. I have been in pain for 10 to 15 yrs. I have always complained about my tail bone area more then anything and was always told there was nothing there. After pain management treatments shots and several test and scheduling surgery. 1month prior to surgery I went to a different chiropractor and she found my tail bone was totally been pushed forward. After her straightening it and one more treatment. It has been the first time in 15 years I have been able to walk with no pain in that area. All those years and people and know one else found it. I couldn’t believe it.
Are you still with out pain?
Omg.. Thank you for this. Your knowledge. I broke my tailbone when I was 18. I found out when I was 30 and having pelvic pain. I am now 52. I’ve had a lifetime of headaches, pelvic pain, and pain in general from my waist down for most of my life. Only the last 3 years the pain has gotten unbearable. I currently have sciatica pain running down both hips.
Drs have never figured out that it’s my tailbone. It was a chiropractor who xrayed me when I was 30. I never thought much of it then. Never ever thought all my headaches could be from it. Thank you
What type of treatment u took for the pain relief sir??
I have the exact opposite problem. My tailbone actually is so posterior that you can see it poking out. The x-ray tech was truly fascinated. My chiropractor worked on pushing it antierior with no luck. I did have injections from my pain management doctor which lasted about a year. The ones I had this year haven’t helped at all. I’m considering having surgery to have it removed. The pain is unbearable and I can’t sit for any length of time, even with coccyx cushions without being in a lot of pain.
I believe this may be from a car accident, because I can’t recall any other injuries that it could be related to. I also have daily, chronic migraines (mostly occipital) that started about the same time. I’m curious if there’s a connection there?
What do you do in a situation like this when the tailbone is going the wrong way? It’s so prominent you can even feel it through a pair of jeans!
I HAVE A BROKEN TAILBONE AND MIGRAINES AS WELL! I never thought they would be connected, have you figured this out?!
My physical therapist was able to straighten my tailbone externally. She did not have to go internal to do this. She is a Physical Therapist with a lot of specialty training in women’s issues.
Yay! This gives me hope!
I broke my spine last year….cannot operate,I limp everywhere,take loads of medication,now the tailbone has started to give agony and cannot walk,what can i do, devastated… what do I DO ß
A three weeks ago I came down with a bad case of bronchitis. A week into the bronchitis on a Thursday I coughed and had instant pain in my tailbone. By the next day I went into the e.r. The pain was soo bad. Reminded me of just having a c section and not wanting to cough which was not, not going to happen with the bronchitis. E.r. Dr. Gave me a shot of toradol , a narco 7.5 , and more meds for the bronchitis. I’m about to go into week 3 and still hurt when I sneeze, cough, sit, or go to stand from a sitting location. Should I go back to see my Dr. Or wait it out?
Brook, you should see a physical therapist or doctor with lower pelvic floor expertise. Your coccyx is connected with muscle, tendons and ligaments to the other abdominal areas. Coughing may have caused muscles to spasm and essentially dislocate the tailbone. A pelvic floor PT can release the muscles and realign the coccyx to a proper position. A little ice will help immediate pain near tailbone. Treat right away as time can cause scarring.
Hi Leslie, thanks for the great article and for your prompt replies to the many questions! I have one of my own. I fractured my coccyx and have read numerous articles suggesting an 8-12 week healing period. However, I have yet to find any specifications of what to do and what not to do during those 8 to 12 weeks. I am 10 days into my healing. Can you please help provide insight as to what type of activity would be most beneficial during this healing.? Should I be slow paced, resting and extremely gentle going about my daily business, or do you think more movement could actually aid in healing? As this is not my area of expertise, I am pleading for an answer and would really like to know what is likely to be most beneficial… slow and extremely cautious or proceed at a normal pace, but listen to my body, as to not over do it? Thank you in advance for your timely reply!
I broke my tailbone 5 years ago, to my knowledge it healed fine and I had no issues, until this year. In January 2016 I started experiencing a strain in my hip while running that after a few months turned into severe pain. When stretching didnt help, I went to the doctor, chiropractor and got myofascial release. All together I’ve spent over $1,700 in therapy/massage/doctors visits. I’m at the point where I’m desperate for relief of my pain and strains. After finding this website though I have renewed hope that this is the root of my problem and that I can get it addressed with a pelvic floor PT! My pain has been in my lower back, sides, glutes, tailbone, hips, and constant tightness in my leg muscles when I used to be very flexible. Any information or advice would be appreciated!
Hi, I’m 26 and I can’t recollect if or when I hurt my coccyx. My pain started about 8 months ago I thought I had prostatitis as I was having pain,spasms and tingling in my perinium area and pain during and after intercourse. (I didn’t know about the pelvic floor then. ).. All tests for that came back clear, since then I’ve had more symptoms, chronic lower and upper back pain, an overall heaviness in my legs? Sore knees, an awful cluncking popping feeling in my low back/sacrum area everytime I get up from sitting
I’ve had a different scans on my back(2 MRI’s, CT and normal xray) all didn’t show anything of significants,….
I’m desperate for answers I’ve been doing PT for months with no relief ,the pain in my groin and all the other symptoms have made me severyl depressed and am going to lose my Job.
Could this possibly be my tailbone out of alignment as it also feels quiet tucked under.
Sorry for the long post.
I have been having coccyx pain for 5 months. I recently had X-rays & MRI. I have a traumatic anterior dislocation of the lower 2 coccygeal segments (segments are at about a 90 degree from the rest) Also, L5-S1 of my lumbar have early signs of degenerative changes with a tear of the posterior annulus & minimal central focal bulge. I cannot find anyone to see or treat me. I live in Oklahoma. Do you have any recommendations?
Thanks for this good article about tailbone treatment. Since 7 years, I am suffering extremely from my tailbone misalignment. I did a trek at high altitude and one day we descended around 1200 mts (and maybe at some moment I did a bad movement). Next day, I was unable to descend all the day because of extreme pain in my right knee but had no problem while ascending. First, I thought it was a problem in my knee but in 3 years, I got to understand that it was my right pelvic which had come sightly outwards which I can feel when I sleep on a hard bed or when kneel down to touch my feet or some other movements too. I can feel it by touching and comparing both sides too.
Now this pain is radiated to left knee, one of the thighs or on pelvic too. I have visited several orthopaedics and physiotherapists who have prescribed some exercises for pain but told me as well that this misalignment cannot be removed. I have myself tried pushing right pelvic inside on my own by doing exercises or by sleeping on hard bed since 2 years but all in vain. Reading this article gives me a great hope. Can you please tell me what I can do to align it. Otherwise, I am too far and lives in India.
I broke my tailbone well I think I broke my tailbone 20 years ago. I couldn’t sit and was in tremendous amount of pain try to sit and literally sat on one butt cheek for very short periods in time. I never went to the doctor of anything, I just got it cracked or readjusted as they would say. Well I would always feel it rubbing and shifting and was uncomfortable. After a while all that went away but when I sit I would always slouch which is bad posture to accommodate. Now I am having extreme pains with my fibular head and hamstring issues as well as pinched nerves and I can barely walk on my right leg. One day I can walk normally and others I cannot put pressure at all. Does all these pains and irritations may be a cause from possible breaking my tailbone? I also got in a car accident in 2002 in which I had muscle damage and possibly 2 slip disc in my back.
I have had sever pain for the last 6 months. I’ve had two MRI’s, an xray, sonogram, 4 cortisone shots, and about 15 PT appointments. Nothing has helped. Nobody can figure it out. How do I find a Dr. who does internal therapy? I live in Austin, TX. I don’t remember any injuries, it just started hurting one day.
Dr Jamie Inman in Fort Worth (D.O.) helped me a few years ago.
Hi I have an old fracture to sacral/coccyx join so most of coccyx normal except for this part which protudes. I’ve had neck pain for last 4 years which has become shoulder /back pain. The coccyx injury happened about 16 years ago and although painful at the time I didn’t pay too much attention to it but realised over time that my coccyx stuck out so couldn’t lie flat. Could that be the sole cause of other pain? I have had 2 kids also since injury which I have found stressful and a difficult family life which I thought also was a big contribution to holding myself badly and so causing neck pain. I am now having cranial sacral therapy /Alexander technique sessions which is helping to release area around coccyx as well as rest of back but am scared I’m always going to have this problem. Any advice? Thanks, Lucy
I banged my bum 3 years ago on a ride it still hurts if I sit down to long or ride a bike but since then I ve started with planture fasitus is it connected at all
My life has been a living hell for the last 6 years, I have pain 24/7 on my tailbone, my pelvis, my glutes, the pain also radiates all the way up to my neck on the left side of my spine, my left lung can’t fill up with air all the way from the compression. I’ve had multiple X-rays, MRIs, CT scans, seen more than 6 chiropractors, been through physical therapy, acupuncture, cupping, massage, I do stretching, yoga and use the foam rollers every day, but nothing seems to help. What made everything worse was the decompression machine, which is when my severe tailbone pain started.
All the doctors always say the same thing, “yes your lumbar spine is compressed, your tailbone is not fully straight, but this is very common and shouldn’t cause severe pain, nobody has a fully straight spine”. I need help, if you’re reading this comment and know of any specialist in the Northern California area that can help me PLEASE, PLEASE let me know.
Hi Ady,
I’m so sorry to hear how much trouble you have had these past 6 years. Check out the practitioner directory on coccyx.org- it is divided by state. There is also a group called Clear Passage who can treat this condition, and they have clinics in Portland and San Francisco. I have worked with them in the past and care safely say that their program is EXCELLENT: http://www.clearpassage.com/who-we-are/locations/
I wish you the best of luck and hope you find relief soon.
All the best,
Leslie
Thank you very much for your quick reply Leslie, it means a lot to me. I went through the list of practitioners in my area and none of the places I’ve called so far do manual tailbone adjustments, I haven’t contacted the one you mentioned, but it gives a lot of hope to know that you highly recommend them, I will give them a try.
Thanks again!
Ady.
Hi Ady,
There is a Ayurvedic physiotherapist in Trivandrum, India who is excellent in slipped disc, bent spine and tailbone issues. My sister after going through severe pain and a lot of medication which didn’t help, went to her and is healed completely now. The doctors name is Justina. Let me know if you need full address and her details by dropping an email at sharhn@icloud.com
Hope you are recovered now.
Thanx
That triangular plate is NOT your tailbone! However, your tailbone IS connected to this plate. The plate is the sacroiliac and it has a joint. Who knew we had a butt joint? This joint is NOT controlled by anything. However, the surrounding muscles play a HUGE part in its health. Relief does not come from internal adjustments but by toning the right muscles. Takes FOREVER! Been dealing with mine for 5 months now. Can’t get my glute to loosen though. Which is causing severe IT band pain.
I had severe pain in the tailbone area. My regular doctor sent me to an osteopathic doc who then sent me to have an x-ray, an MRI, and physical therapy. Nothing worked. Finally a friend suggested I see Dr Jamie Inman in Fort Worth who performed a slight internal adjustment. It was miraculous. I felt a “click” and iimmediately was relieved of about 80% of the pain and the rest gradually diminished over time. I suspect the remaining pain was the sore ligaments that needed time to heal. So, yes! An internal adjustment can work. Just depends on your issue. 🙂
It’s actually called sacrum; not sacroiliac. The sacrum has what is called the sacroiliac joint. The joint DOES move and can develop arthritis and can be injured with or without injury to the coxxyx (tailbone), which is attached to the bottom of the sacrum.
Hi,
I have just started (within the past 5-6 days) to notice that I can now feel my tailbone when I sit on a hard surface, such as the floor.
I don’t feel any pain really, I just feel like my tail bone is longer all of s sudden? And that if I sit on a hard surface, it will end up hurting..
I don’t know what to do and whether it’s worth a trip to the doctor or I’m just overreacting. Any help would be much appreciated. Thank you 🙂
Hi Lucy,
I have some patients who start noticing their tailbone more when they have been chronically sitting in a slouched position. A good sitting position is upright with your weight on your ‘sit bones’… when the pelvis rolls under it can transfer the weight towards the sacrum and tailbone. Check your sitting position and be careful to always sit upright. If it continues it may be worthwhile to seek out a practitioner who can evaluate your pelvic and coccyx alignment. Coccyx.org is a good resource.
All the best,
Leslie
Ive had chiropractor hit my left pelvis down put me on drop table used his palm hit it hard cause he said 18mm high,3 epordorials ,pt nothing is helping.Its been years same constant pain in groin,lowerback,middle of left pelvis,hamstring,behind knee,back of ankle,and second toe in under that toe feel like walking on rock or staveing,pins and needleswith leg weaknwss,do you thinj myofacial release,or pushing tailbone out from inside will,help?I have ddd,annual tears bending back right shoulder lower then left.Please help.
Hi Leslie
I have had an mri scan and shows I have a misaligned coccyx…the physiotherapist subjects I have steroid injections to hopefully ease the pain. Do you think this is the correct treatment?
Hi Lynnette,
The injections may make you more comfortable temporarily, but will not address the tailbone misalignment. I’d recommend seeking out a physical therapist, DO, or chiropractor who can treat the tailbone alignment specifically. Coccyx.org is where most of my patients find practitioners near them. If you still need additional relief then perhaps an injection is something to consider.
Hi,so i had went to a water park and jumped of a 40 foot height into the water & my whole leg had went numb, from my tailbone down to my legs. I got a bruise from it, & its all healed the only thing im having problems with is ny tailbone, ive been getting alot of pain from my tailbone since that day. What do i do? Because the doctors couldnt do much for me.
Hi Tiffany,
Check out coccyx.org to find practitioners in your area who can treat the tailbone.
Best of luck!
Leslie
Wow. This is such a long story but will try to shorten it.
12 years ago I thought I had a UTI – felt like I had to pee constantly. It came on with abdominal pain and constipation. It got worse. Did every bladder test known to man. Bladder was fine. Also came with some pain in the tailbone in sitting. Got better over time but got WAY worse before it got better.
The symptoms are back now. Out of the blue: horrible urgency to pee, abdominal ache, constipation. Actual peeing never hurt or impeded. A friend asked me about any injury early in life and Yes, I had tobogganed down a hill at 12 and hit a rock full blast with my tailbone. A gyro/urologist years ago said it could be deferred pain from somewhere else as my bladder and region are fine. Could it be that this tobogganing injury has messed with my taibone area, ergo, playing with the nerves that effect my bladder?
Any help will do. I’m stuck and I can’t go back to this discomfort again.
MUCH appreciate it.
HI Sam,
I’d definitely go back to your GYN or a gastroenterologist to make sure that there is nothing systemic going on. If all tests and imaging come back clear, then you can look into a musculoskeletal cause.
Best of luck!
Hi Lesley, I fell down the stairs about 7 years ago and hit my tailbone coccyx on every step. I got up and was in a lot of pain went to hospital an they said that they couldn’t do anything for me. Was put on oxy-contin and oxy-norm for a month and was told to rest for 6 months. I had rested for 2 months and in between this i was seeing a physio therapist then had to go back to work. Since then i have had bouts of pain now and then and some rest, painkillers and hot water bottle did the trick. But recently i feel like my bum is about to fall out of my trousers and have pain going up my spine and down both legs. Pain killers does nothing and not sure if the doctors can do anything for me. Do i need a MRI scan to determine what is going on or something?
Go and visit a physio who is qualified in spinal a pelvic realignment. I did as I was referred to one by my physio, cos she wasn’t strong enough to do it , I out weighed her by ten stone. Lol. Recommend if in Manchester area, Howard hunter , wilmslow physio.1st appt – approx £75 for assessment and treatment. Then £55 for each visit. For me and the results I got , worth every penny.! I had about 5 visits after the 1st. But he does give you a full body exam and found things that an X-ray didn’t pick up.
Good luck.
Thanks Graham, AM going to see a spine specialist and just waiting for an appointment. Thanks for replying to my message, but i live in Aberdeen.
I had an accident at work I was a cleaner in an aged care facility. The accident was over 5 & 1/2 years ago, I moved a bed to vacuum underneath and as I was moving bed I twisted and there was a sharp pain in my right side and lower back. I only found out yesterday that nothing can be done for me as the injury is in my tail bone.
I hurt my tailbone. Is that affect pregnancy?
Dear Leslie,
I am a dentist, and have had hemmoroid issues in the past 3 years. I have a small one that only worsened this year due to constipation from pregnancy. My friend recommended I get one of this inflatable donuts and sit on it as much as possible along with preparation H to get rid of my hemmoroid. My pregancy was awesome, no nausea/vomiting, pain, except for minor round ligament pain until 1 month before I was due. I gave birth May 20, 2016 (4 days ago!). My pain started April 11, 2016. Around the same time or a little before it I started using the inflatable donut, which felt by the way ok the first day, but then I felt like I was trying to find a comfortable position on it after that. I was constantly adjusting or just not using it. I found my pelvic/inguinal or groin pain started then. It was always a lingering pain on the left, and I just said ok it’s the baby pulling down and pinching or pressing on something, so I ignored it! Well it got worse to the point where I could barely walk 2 weeks before 5/13 which was my due date. I suffered so much pain, and told my OB and she said lets do an MRI. Well I went to get that and I couldn’t do it, I was 9 months pregnant and very cloister phobic! I then ended up going to acupuncture and that provided limited relief. Then I went to an orthopedic who checked to make sure I didn’t have pubic symphysis dysfunction and according to his testing he said go home and exercise, stretch, walk on it and you will be ok. He thought it was just the baby pressing on my pelvic floor. So this motivated me to move more and do squats which actually made my pain even worse! I eventually stopped moving around too much used a heating pad at all times and set up shop on my couch until the end of my pregnancy. I did manage to see a chiropractic who is great for my psychological well being however, he too did not help much. Once I gave labor my pain felt a little better, but the week before and now both sides of my groin hurt like a 9/10 on the pain scale. I’m so depressed I can’t walk that it’s started to effect my everyday life. My husband found a pelvic and breast rehab center, but just wanted to see if you have heard anything like my story before? By the way I did have a natural delivery with an epidural. Of course the epidural took away my pain on the left side, but for some reason it didn’t even work on my right side. I got what I call a unilateral epidural injection :/ Please help with any advice, I am up late doing research for the 100th to see if anyone suffers the way I have been.
Hi Sarah,
I too have the same issues you have for the past 5 years. My journey began when I could not identify where the pain was exactly coming from, being that my groin, low back, right hip and the constant bloating brought me so much pain that I had no clue what was causing it. The doctors put me through every test imaginable, to the point I lost faith in every single one of them. One day I was doing some research of my own and found this OBGYN here in Michigan that did tailbone adjustments, since it did hurt when I sat I figured I would give it a try. What the hell right?
To my surprise, My first adjustment I felt some relief but then a couple of days went by I went out again. I went back for 2 more adjustments after that and went out with in a couple days. Again, as I sit here writing you, I am in some pretty bad pain. I still have faith in this doctor, however, I have been doing some more research this evening and it turns out that since I have been out of alignment for about 5 years. I may have some pretty severe muscle imbalances, now I work out with a trainer, so, I’m conflicted as to what to do. Keep working out or go another therapy rout.
Keep me posted on your journey to perfect health, since you seem to have the same symptoms that I have. And I will do the same, maybe together we can figure this tailbone thing out. So we can get back to living life. 🙂 good luck!!
Lesley
I suffered for over 2 years with the same described pain. It started in my 3 rd trimester and continued for a yr and a half after that. I saw 8 specialist and had every test/procedure imaginable. I finally got relief when I started seeing a PT who specialized in women’s pelvic health. I had a large amount of scar tissue around my tailbone and from shifting from side to side for over two years most of the muscles in pelvic floor had knots that needed to be released. What really did the trick was getting my Pelvis aligned everyday and wearing an SI joint belt. Since I was misaligned for over 2 years there was damage to the piriformis and coccygeal muscles. These had to be stretched daily and toned back to health. The process took about 6 months but I am 80-90% pain free. I was in so much pain before that I literally didn’t sit for months. I couldn’t unless I was on a heating pad. Your experience may be different, but if you are in pain and as desperate as I was after more than 2 years, its worth a try. Find a PT that specializes in women’s health.
Hi Sherri, who was your PT?
Tess
I also have tailbone misalignment and live in Michigan, please may I have or be referred for a call, i fell on ice last December and had hip surgery but am now having bladder leakage and back and neck pain
Help! I have seen my doctor but he has no knowledge of this. I feel exactly that. Can I perform the re-alignment back on myself? In case I can’t get an appointment soon enough? Also – does this procedure involve a high degree of pain (such as moving a dislocated shoulder back to place, or less than that?)
I’d appreciate your answer
Hi Shirley,
While you may be able to do self treatment later on, it is typically challenging and requires training from your PT. While treatment may be uncomfortable due to the sensitive nature of that area of the body and inflammation that may be present, it should not highly painful. I recommend checking coccyx.org for their directory of practitioners.
All the best,
Leslie
Shirley, I am a health coach and yoga instructor and have had falls in childhood and most recently a car accident that moved my tailbone sideways and inwardly.
You can do the adjustment yourself, I did it myself for my car accident because I none of my chiropractors did this kind of care! Although “Network chiropractic” will do this kind of adjustment if you can find one near you.
The pain level is not anything like putting a shoulder back into its shoulder girdle! No way.
But it can be sensitive like a tender spot after an injury.
Here is a link to this website that explains how to do it yourself: http://www.dynamicchiropractic.com/mpacms/dc/article.php?id=46070
In my case my tailbone was so turned under that it is taking me several days/weeks of adjusting once or twice a day until I could feel the tip of my tailbone in my finger. I did the external approach.
Slow and steady gets you to have mobility in the tailbone until you can actually hold it and pull it back. It works. In combination of yoga, massage and chiropractic care your spine will restore its natural alignment as you keep adjusting your tailbone.
I fell down the steps about a week ago. And my tailbone hurts really bad,now when I sit it feels like something is there.is my pelvis out of place? Thank you
Hi Shyla, unfortunately this is not something that can be determined without an examination. I suggest you find a physician who is familiar with the tailbone- coccyx.org has a great directory of practitioners organized by location.
Best,
Leslie
I slipped and fell while ice skating about 7 years ago and fractured my tailbone. Since then my tailbone “pops” out of place… Sometimes it hurts a lot and sometimes not at all. I can normally pop it back by applying pressure or by squeezing the muscles around it. After I fractured it the doctor told me part of it didn’t heal right and is blocking my birth canal but to fix it they would need to rebreak it, which they deemed too risky.
Is this something I should get checked out? Also, what kind of doctor is best for this?
You should do research on which doctor is the best. When they say rebreak it, it is a 50/50 chance of something going wrong. Yet I’m just a kid, but I also have a issue with my coccyx and I feel like it’s misaligned. So I’m gonna go take a FREE x ray hopefully and we will see how that goes. I heard when they remove the coccyx (tailbone) you will have to bare pain usually 3 months to a 1 year. Overall you will feel more relieved.
About three months ago a friend hit my tailbone with a barstool as hard as he could trying to be funny. After this there was a slight amount of bruising. As the time has gone on it has healed slightly but still causes minor pain when sitting or transferring from standing to sitting. Then just recently it has started to make a popping sound if I apply pressure. Is this normal or do you think I should get it looked at by my doctor.
Yes, I would have it looked at. Good luck!
i have a very bad coccyx subluxation (its 90 degree inwards) and i tried myself pulling it
internally in a correct position but it doesnt move very much (even with much pressure on the coccyx). X-Rays show that the coccyx is not fused together but it doesnt seem to move.
is there a possibility do realign the coccyx when it seem to be stuck in that position (90 degree inwards)
Yes, there is still the possibility to improve the tailbone position, even if to your touch it seems very rigid. You will need to find a therapist who specializes in this type of work, and preferably someone who has been trained in myofascial release. They should do a thorough evaluation and let you know how much improvement you can expect to see with treatment.
All the best,
Leslie
About 2 weeks ago I was walking down the steps from upstairs and missed the last step and fell very hard on my left hip. Yes, it is painful while sitting, which includes driving. Feels like the pain is in my lowest part of my spine. Advil and Alieve help very little. It hurts when I have a bowel movement. I don’t feel like anything broke but unknown of any internal injuries.
I have had sciatica before but this seems to lasting longer. The pain goes down my legs a bit, just a tingling pain, as I am to walk ok. If I see the doctor how will they evaluate my injury…MRI, XRAY, etc. Opinion please.
Hi Fred,
How you are evaluated will depend on your physician, but I presume that they will at the very least want to take x-rays. I suggest starting here. If x-rays show that there are no fractures you can go to to investigating whether you are experiencing pain due to the coccyx, sacrum, lower back…
All the best,
Leslie
This is it!! I have been complaining about my lower back for a couple of years now. Im not sure what caused this but i had a daughter feb. 2013. I immediately got birth control. The copper IUD called paragaurd. I bled heavy for about 1 week. Then i stopped bleeding and no more periods so of course i wad happy! Then i got into a relationship and noticed i was having chronic pains during intercourse and it never went away and i bleed every single time we had sex. So i went to get my iud checked and DEAR GOD it hurt so bad. It wad stuck. I got it surgically removed and i still have not had a period to this day. I now have a soft tissue lump on my lower back. And right under that soft lump, i can feel what im sure is my tail bone. When i sit on a hard chair it really really bothers that bone. I cant ever get comfortabe laying or sitting. When i lean my chin closer in toward my chest it feels so good. I cant stand, sit, lay, walk….NOTHING for longer than 10 mins without irritation. The first day at a job i had, i stood in the same spot for 7 hours. I left crying cause i could hardly move. I got in my car and coughed and it felt as if my back had just snaped in half. HELP PLEASE!
Hi Casey, I’m so sorry to hear that you are having these issues. It definitely sounds like you would benefit from evaluation by a physical therapist specializing in pelvic rehab, preferably one with experience in myofascial release, visceral manipulation, pelvic floor treatment, and coccydynia. I’d also recommend checking back in with your gynecologist, since you still haven’t resumed your menstrual cycle. Check out coccyx.org for info on practitioners who treat coccydynia or https://hermanwallace.com/practitioner-directory for pelvic floor PTs. You can also google search ‘women’s health physical therapy’ or ‘pelvic floor physical therapy’ in your area. Once you have a list of practitioners, call and discuss your case with a few to see who seems like the best fit. Good luck!
when the coccyx is misaligned and show to the left side will the muscles that are attached to it move along the direction that the coccyx is facing to?
(i hope u understand that question and sorry for my bad english)
Hi Mary,
Unfortunately it’s very hard comment on individual situations since every patient is different and presents differently. In general, though, the muscles of the pelvic floor can be affected by tailbone misalignment, and depending on what other issues are present there may be hip, leg, or lower back muscle involvement as well.
Can you die if you don’t fix it
Hi Gabriel,
I am not aware of any cases of someone dying due to a tailbone injury.
What happened when your tailbone injury and the misaligned of the coccyx is
causing you problems with Urination and bowel movement., and causing retaining water in the uterus.
I think I injured by sitting down on a concrete floor for prolonged time fixing my water heater it’s been about a month and a half can I take anti inflammatory pills and what they help or fix the problem?
Hi Alex, as a physical therapist I cannot recommend medications. I would recommend an evaluation by a physical therapist or orthopedic physician to assess whether you are feeling pain from your coccyx or somewhere else, as well as learn treatment options for your specific issue.
I have suffered from a twisted pelvis for years I finally met a doctor who realised what my issue was. We solved my pelvis issue with exercises and sugar shots, but I still can’t do lots without causing it to go back to being twisted, left or right. I have for the last 10 years have always had swelling on my tail bone. Yet never really worked on that, and I accepted what pain I was having even when my pelvis was correct I gauged my swelling on my back as to take the next day off or not. I hurt if I carry ,lift.etc I think I have finally realised that its my tail bone that’s the issue. I was taking tylenol for a tooth ache I normally take no pills at all. The swelling went down and I bent over wrong and it felt like a knife went into my back. The next thing I knew was the lumborum spazed and I could’nt use my upper body to help my tail bone to get up or sit down. Today I have relaxed the lumborum but my tail bone is really sore. My pelvis is correct now as well. but my tail bone swelling is half a grapefruit size and very stiff on movement.
My daughter fell on her coccyx yesterday and it seems to be sticking out a little and she is having problems seating down , she is fine walking , do you think I should get her to see a doctor or could it correct itself in a few days . She is 12 years old by the way, thank you
Hi Beka, if in doubt have it checked out. Certainly if you can see a problem with the bone then it should be looked at. If it’s simply a little bruised but not sprained or broken then I’d recommend getting a donut pillow for her until the soft tissue heals up. Hope this helps!
Is it possible for your lower back and tail bone to be realigned and you have the urge to go frequently for a while. My back was injured for years and I just for the first time saw a chiropractor and got it aligned and now it feels like I need to go frequently.
Hi Chri, Thanks for your question. I would definitely direct this question to the chiropractor who treated you.
I injured my tailbone a few months ago doing repetitive rolling/balance movements on my basement floor. The pain subsided, but recently returned after sitting on the floor for a prolonged period… The pain is fairly constant now ranging from a dull ache to sharp, shooting pain. I was planning on contacting a chiropractor on Monday- but now I’m very hesitant. Are there any exercises or stretches I can do in attempts to realign my tailbone on my own? I am a COTA so I work with a few DPTs but obviously I would never have a friend/coworker attempt to reposition my tailbone with these methods! 🙂
Are there surgical solutions to this problem? Ongoing too long with my wife. What surgical specialty should we be looking for? She has tried traditional PT for this. Injury from slip and fall on ice. She has to sit on a coccyix pillow to prevent worse flare ups.
Thanks for your help.
Hi John,
Traditional PT will not likely resolve coccydynia. I would recommend looking up “pelvic floor” or “women’s health” physical therapists in your area and asking each if they can treat coccydynia.
It is possible to do injections around the tailbone, or remove it surgically. Surgical removal is a typically a last resort, following conservative care which includes pelvic floor physical therapy.
Hope this was helpful!
The surprising thing is i manage to adjust my tailbone to its original position by stretching. Will it prolapse again?
Hi Alex,
That depends on the type of stretching you use- if you are using a fascial-release technique it may stay adjusted for quite a while or permanently. However if there is pelvic floor spasm, sacral dysfunction, or other commonly seen associated dysfunctions, it may be pulled back out of alignment.
In my experience, standard stretching (holding a stretch for 10-60sec) typically will not permanently resolve this issue.
Hope this was helpful!
Hey alex,
I am suffering from tailbone misalignment from 2 years, i need your help, please can you drpp me an email so that we can connect.
Thanks for the good article and detailed information about tailbone misalignment. My teenage daughter has been suffering from a lot of tailbone discomfort and pain since a slip and fall almost two years ago. She is now receiving PT treatment, but may need to go to a more advanced treatment of internal mobilization. How many treatments are typically required? It is a pretty extreme treatment for someone of her age, and I want to make sure it is not a prolonged treatment. Also, we have had doctors tell us to get an MRI. What would this accomplish?
Unbeknownst to most women (and men for that matter), the tailbone as well as the entire spine and pelvic anatomy is compromised by hysterectomy. The first indication of these changes was a bruised looking tailbone around 1 year post-hysterectomy. Not long after, my rib cage started falling and my hip bones began widening. I am now 8 years post-hysterectomy (which never should have been done in the first place) and my figure looks far different than it did prior to surgery despite no weight gain. Not only is this extremely distressing appearance wise, it causes back, hip, and rib cage pain that I never had before my organs were needlessly removed. You can read about the hysterectomy induced skeletal and anatomical changes here – http://www.hormonesmatter.com/post-hysterectomy-skeletal-anatomical-changes/.