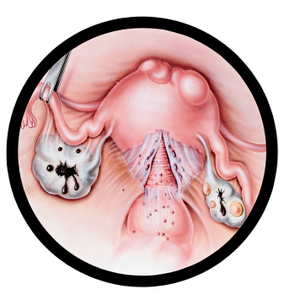
Twenty-Five Years for the Correct Diagnosis: Endometriosis
My name is Angela Wice and I am 35 years old. I had one child with natural birth in 2003 and was diagnosed with Stage IV endometriosis June 2006. My Journey has been long, depressing and still not over 25 years later. Here is my story.
Early Childhood and Early Troubles
I was a very busy active, athletic, child growing up. I would say besides being born with jaundice, I was healthy until I turned 7 years old. I was rushed to the hospital because I started bleeding rectally. I was operated on within hours of being at the hospital for intestinal volvulus and appendectomy. They sewed my bowel to the pelvic wall so it wouldn’t happen again.
By the age of 10, I started to get chronic headaches and was told to stay away from chocolate, peanuts and cheese.
The Pain of Endometriosis
I got my first period when I was 13. The second time I got my period is when the pain started. I had the worst cramps ever, my legs would go numb, I was nauseated, I was bloated, and I was in so much pain I would vomit. I remember them saying that you should only bleed 1 TBSP a period and I was like “Are you kidding me, I do that in an hour!!”
My mother took me to the doctor the same year. The doctor did an ultrasound and a transvaginal one as well. The pain was so bad on the left side when she inserted it inside me but other than that nothing showed up but she did say that I possibly had endometriosis. That was at 14 years old, nothing was done about it. I was given Naproxen and that was that.
Endometriosis and Migraines
My first migraine happened when I was working at around 16 years old. My whole right side went numb including my tongue. I went to the hospital and they said it was an Aura Migraine.
By 17, I was far beyond constipated and the rectal pain I had was so severe and sporadic. To be honest, I never really put two and two together because I could just be driving and all of the sudden it felt like was being stabbed with a knife in my rectum. That never went away. It was constant.
I knew I was getting my period because I would, all of the sudden, not have constipation and I mean literally evacuate all my bowels at one time. That was my sign to start taking the Advil, and by the next morning or the middle of the night there it was. Sometimes if I didn’t take the Advil in time it was too late, nothing would work. I would pump my system with so much of it until my period was over. During my period I could not have a BM at all until my period ended. It was excruciating. I got fed up went to see a gastrologist. I had a colonoscopy and was told it was IBS, which I did not believe. That was the first of over 40+ doctors/specialist I was to see until I was diagnosed.
Endless Misdiagnosis
For the next 15 years it became a blur. I was depressed, angry, frustrated, disappointed, rejected and in so much pain that never seemed to end. I went to doctor after doctor only to be diagnosed with fibromyalgia, chronic fatigue syndrome, restless legs syndrome, thoracic outlet syndrome, TMJ, irritable bowel syndrome, chronic pain, cluster migraines, complicated migraines, neuropathic pain syndrome, overactive bladder, depression, anxiety and I developed an eating disorder (Bulimia).
I was at the end of my rope in 2006 and had another ultrasound only to find out my results were misplaced until I called 3 months later to find out that I had a 10cm complex cyst. I was sent to an oncologist who took blood work CA125 to see if I had cancer. The first test done was 37 on my period and 78 when I was ovulating. He felt positive it was endometriosis and sent me to a local gynecologist who told me nothing could be done about the Endo and to take Lupron. I refused, as I had done my research. She then put me on Marvelon21 and sent me on my way. One thing changed for sure right away from taking the birth control pill and that was the chronic nausea was gone within a week, acne cleared up and my mind was right. I really felt like I got a new lease on life.
The Power of Patient Groups
I ended up on Medhelp and found a great group of women that to this day we still talk. We have a private group of about 20 women on Facebook called the BBBC (Bulge Battling Battalion Cysters). Some of the women had cancer, some were in remission, some had Endo etc. They were my support and still are, without them I would have surely not been here today.
I did my research and found the best Endo doctor in Ontario. It took 3 minutes for him to find the rectovaginal cyst that had caused me so much pain all of these years. I was in tears, tears of relief that finally, finally someone knew what was going on. He couldn’t do the surgery because I had previous bowel surgery so he sent me to his protégé and he operated on me a month later.
My story continues. More next week.









Thank you so much for sharing! I am shocked at how similar your story is to mine. I am also 35 and am constantly battling endometriosis and chronic migraine pain. After giving up for several years and just dosing myself with as much pain meds as possible every month, locking myself in my apartment, missing work and missing life, I’m now trying to find help again and have been looking at support groups online and found a new GYN.
Dear Angela,
Reading this I felt like I wrote it. I’ve sent it to my parents, best friend that is a PA and boyfriend and they all were shocked to read an account so similar to mine. My issues started as a 12 year old when I got my first period. After my “emergency” gall bladder removal in 2008, I’ve been on a roller coaster of a diagnosis game. I was diagnosed surgically with Endometriosis in 2015, and had my second lap this past July. Additionally I’ve been diagnosed with OAB, IBS, Depression, Anxiety, ADHD, Restless Leg Syndrome, possible IC, anal fissures, insomnia and hemorrhoids. Recently I suffered the miscarriage of an unknown pregnancy because my IUD was shifted after my surgery. I know that I’m reading this a few years past your posting, but I am located near ON and I’m wondering if you could contact me privately. I’m looking for a new doctor, preferably a specialist, because I do not trust the judgement of my doctors. I’m 24 years old and I’ve spend the entirety of my adult life chasing this around. I can’t help but to feel that my life revolves around my pain and my pain only. I worry about my career, life goals, the possibility of having a family, and my overall health constantly.
I hope to hear from you,
Susie
Dear Angela,
Thank you so much for sharing your experiences and inspirations.
I would like to know which pills did you taken for your migraine?
Just marvelon BCP continuously. It seemed to be the only thing that stopped them for me. So mine must have been estrogen or progesterone driven as I haven’t even had one since my hysterectomy either.
Just be careful. The chemistry is such that it is not a matter of if, but when.
Hi Angela, I have migraine with aura and Adenomyosis, but I’m convinced I have endo as well. My entire body is in excruciating pain all the time and I suffer from period cramps all month long. I’ve been told I can’t be on contraception due to my headaches. I have a one year old at home and don’t know what to do. I’m in constant pain and it’s affecting every aspect of my life. When you had a hysterectomy, did you have your ovaries removed as well? Has your pain stopped? What specialist did you see? I’m in Toronto and looking for someone to help me.
I have been reading that a hysterectomy can actually make migraines worse. Was this ever a concern?
Not sure if you still respond on this, but I’m wondering about taking BC as a migraine sufferer? I was taken off them because of the stroke risk.
There is a big risk for stroke in migraine sufferers from hormonal birth control. We’re beginning a research project on the topic very soon. We’ve begun writing posts about blood clots and birth control and sharing personal stories of women who have had strokes (brain clots) while on birth control. Both of the stories we have so far had migraines and in fact, were given migraine meds during the stroke which made them worse. Do the research, take a look at our posts on the topic. We’ll have more of them in the coming weeks and months.
Jennifer
I am so sorry that you are going through this. My main concern was the migraines after my hysterectomy. I know since being on the pill the migraines stopped and I only had one in 8 yrs and since my hyster in May 2014 I have not had one yet. Crossing my fingers. It is painful and yes I would say more harder to deal with than Endo in my opinion. Are you on any HRT? What did the neuro say? Mine chalked it up to “Complicated Migraines” since he couldn’t figure it out. Mine was def hormonal in my opinion it might just be that yours is not. Its trying to find out what triggers them is what is the hardest thing to do. I only noticed mine gone after I started taking the pill but I know others start to get migraines while on the pill. Have you seen an Endocrinologist before? I am wondering if you can have a thyroid panel testing done.
I’m crying as I read this because I’m fighting the same battle with no resolution. My option has continually been, “Which is worse? The migraines or the endo pain?” When the endo pain was unbearable after 3 laparascopies, I had a radical hysterectomy at age 36 a few months ago. Since then, my “well managed” migraines have been out of control and I am having to take imitrex almost daily. I’m at a loss. I feel like I will never be normal again. Honestly the migraine pain is worse than the endo pain because at least pain killers could help the endo pain. Unfortunately, here in the States (and probably everywhere), it is so tough for doctors to be able to get around new legislation re: painkillers (amt. prescribed), that I HAD to have a hysterectomy because I couldn’t continue to function on painkillers 2 weeks per month like I was doing. I got a misdiagnosis of IBS at age 22 also… and have been diagnosed with Stage 4 endo. each time I have had a laparascopy. Now here I sit trying to teach school with a migraine. I’ve had a migraine almost every single day since my hysterectomy in June. No joke. My doctor doesn’t know what to do for me. I’ve been to neurologists…
I am at a loss and I am so discouraged. Thank you for sharing your story because it gives me hope.
I wish I knew how you were doing now I am in this same boat…
***Dr.Kay Lie** sorry spelled that wrong
Kim, I saw two. The first one was Dr. Kay Lei in Toronto but he pushes the Macrobiotic diet, tai chi and natural stuff which isnt bad either but he knew I had a rectovaginal cyst so he sent me to his protege Dr Nicolas Leyland he now works out of McMaster university. Have your doctor send a referral over to him. He has no bedside manner but he knows what he is doing.
I live in Ontario as well – would you mind giving me the name of the dr you saw that found your cyst? I am certain I have endo but am having a hard time convincing my current doctors to explore further. Thanks!
So glad you found a good doctor. Endometriosis specialists are too far and few between. Here’s a great one who wrote this great blog on what it’s like to have endo: http://www.vitalhealth.com/blog/endometriosis/what-it-really-means-to-have-endometriosis/ He gets it.
I totally agree
The first step in dealing with this problem is that there has to be a phase shift in the model used to explain and diagnose these two debilitating disorders of oestrogen metabolism. There seems to be a mind set amongst Gynaecologists that refuses to accept the major role sex hormones play in the body’s metabolism outside of the uterus.
The first step must be the development of a “safe” range of estradiol within the current lab range which is just representative of 80% of the range of values seen in that lab. We know with blood cholesterol levels that the ideal range is only a tiny window inside that 80% range seen in the lab. and billions of dollars are spent trying to achieve that “safe” level. But ask any Gyno what the “normal” blood levels of oestradiol at day 21 is, then you will be told that it is anywhere in the 80% range, which of course it is not!
The second step is to concede the role that natural progesterone (and also realise that artificial progestogens have a completely different biochemical reaction in the body) has in the regulation of estradiol levels. And then to recoginise its use as a valid theraputic agent.
The third step is to realise that estradiol is very much like thyroxine and that while its total body blood levels are important, it is its metabolites that are the active molecules that actually produce the physiological effect. It is the hydroxylated metabolites of E2 that produce the physiological effect in the body, ie 2 alpha, 4 alpha and 16 alpha hydroxy estrone. Disturbances in the ratio of these 3 metabolites will be a non invasive way of diagnosing the above 2 conditions.
But there are a lot of rigid minds out there!