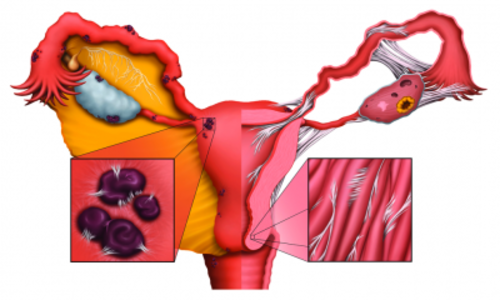
While doctors disagree on the exact cause of endometriosis, theories include heredity, environmental problems, or retrograde flow of endometrial tissue from the uterus, out the fallopian tubes, and into the body. Whatever the cause, most doctors agree that endometrial implants and adhesions (internal scars) are frequently found together. Adhesions are tiny but powerful structures that act like straight jackets wherever they form, causing pain or infertility – or both; because adhesions do not appear on any diagnostic test (x-ray, MRI, CT scan), they can elude even the most savvy physician. Thus, our patients often tell us “my doctor says he can’t find anything” or even “he says it’s all in my head.” The truth is, the pain is exactly where you are feeling it.
Endometriosis Pain
While there is no consensus as to the cause of endometrial pain, increasing evidence from the studies published from our clinic and elsewhere indicates that the pain is caused, or significantly increased by adhesions – internal scars that form where endometrial tissues attach to underlying structures. In the past, the only method to treat endometrial adhesions was surgery. However, physicians and their patients are stymied by the fact that, no matter how skilled the surgeon, surgery to decrease endometriosis or adhesions tends to cause more adhesions to form as the body heals from surgery. A large retrospective study of post-surgical outcomes [Digestive Surgery, 2001] reported that between 50% and 100% of all pelvic an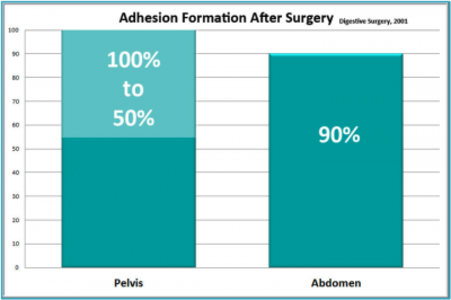 d abdominal surgeries created additional adhesions.
d abdominal surgeries created additional adhesions.
Thus, while the surgery may help some women, the relief may be temporary; recurring, and sometimes greater pain can appear as the body forms internal scars to heal from the surgery. Some evidence indicates that endometrial implants tend to recur with greater frequency at the surgical site.
Endometriosis and Pelvic Pain
In our own published studies, we have come to understand that the pelvic, abdominal, hip or back pain often associated with endometriosis comes from the pull of tiny but powerful cross-links, the building blocks of adhesions. Where endometrial implants appear, adhesions tend to bind the foreign tissue to the underlying structure. As the tissues swell with each menstrual cycle, the adhesions pull on the delicate underlying structures, causing pain. Our manual physical therapy appears to detach the adhesive bonds so endometrial tissues can expand and contract naturally, without pain from the adhesive bonds.
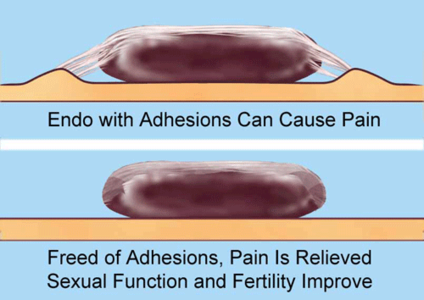 Hormone medications such as birth control pills can stop the menstrual cycle totally. Since the endometrial tissue does not swell, it does not pull on the adhesions and pain is relieved. However, if the woman wants to have a child, she has to stop the birth control pills and the pain returns. Thus, the medications address the symptoms, but not the cause of the pain.
Hormone medications such as birth control pills can stop the menstrual cycle totally. Since the endometrial tissue does not swell, it does not pull on the adhesions and pain is relieved. However, if the woman wants to have a child, she has to stop the birth control pills and the pain returns. Thus, the medications address the symptoms, but not the cause of the pain.
Pain with Sexual Intercourse: Definitions and Therapies
Our patients tend to report three different types of intercourse pain:
- Pain with initial penetration
- Vaginal pain during intercourse
- Pain with deep penetration
The body creates adhesions (tiny internal scars) wherever we heal – whether due to an infection (e.g., bladder, bacterial, yeast, STD), a trauma (abuse, fall onto the tailbone or perineum), or a surgery (abortion, C-section, laparoscopy) – or due to inflammation from the endometriosis itself. These adhesions can be small enough that they form between muscle cells, causing pain when your partner pushes on them.
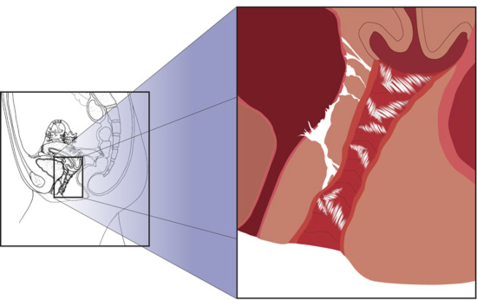 Because of its unique position in the body, a woman’s vagina is subject to numerous traumas in life. Falls onto your bottom cause adhesions to form. Once your body heals, the adhesions remain there for life, causing tiny but powerful straight-jackets that can cause pain when pressure is exerted on them – such as during intercourse.
Because of its unique position in the body, a woman’s vagina is subject to numerous traumas in life. Falls onto your bottom cause adhesions to form. Once your body heals, the adhesions remain there for life, causing tiny but powerful straight-jackets that can cause pain when pressure is exerted on them – such as during intercourse.
With the warm, moist environment, the vagina tends to be a perfect place for bacterial infections. Again, adhesions form as the first step in the healing process – to help contain the infected area so your body can heal more easily. Once you have taken antibiotics or are otherwise healed, the adhesions that formed remain in the body for life – unless removed by a skilled physical therapist who specializes in work in this delicate area.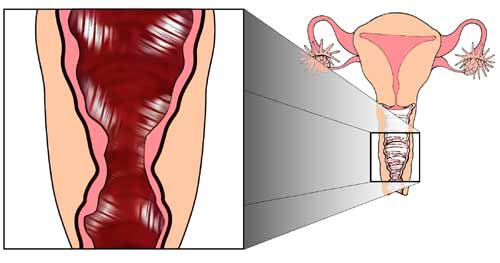
Women who have pain with deep penetration say “it feels like my partner is hitting something,” – and he is! The usual cause for this deep pain is either a stenosed (adhered) cervix caused by adhesions following a healing event (shown in the drawing below), or a forward tailbone – caused by a fall, trauma, abuse or surgical scars.
Physicians are generally stymied to cure intercourse pain. Their prescriptions generally consist of any of a combination of therapies that address the symptoms, but not the cause. Physicians may suggest:
- Abstinence
- Pain relievers
- De-sensitizing drugs
These approaches do not help a woman get the pleasure or function (desire, lubrication, orgasm, pain relief) that should be hers. Many of our patients feel their lives deeply impacted; some are concerned that the pain will impact or even end their relationship with their partners.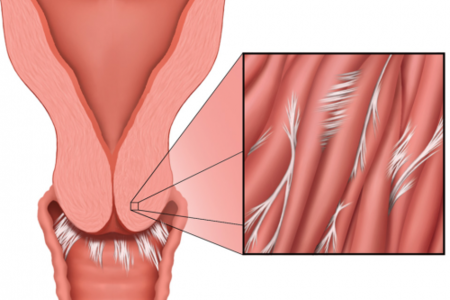
Fortunately, there is now a non-surgical, drug-free treatment for endometriosis pain. The Clear Passage Approach® has been examined for treating pelvic, menstrual and intercourse pain associated with endometriosis for decades. In a recent study update in the Journal of Endometriosis, this therapy was found as effective as surgery – even a year after therapy.
Besides studies in that journal, studies on this work are published in WebMD’s Medscape General Medicine, and housed in the U.S. National Library of Medicine (see study results below). In all of our studies, the treatment is a manual physical therapy that can feel like a deep massage. A brief look at the results are provided below. Learn more about treatment for endometriosis pain.
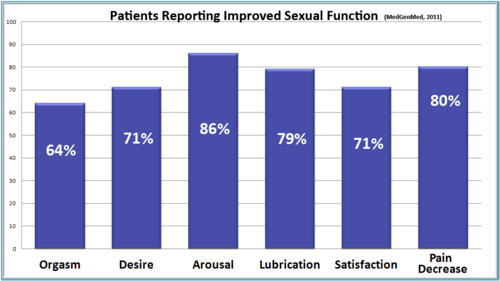
Pain Decrease and Function Improvements from a study on the Clear Passage Approach, Published in WebMD’s Medscape General Medicine, 2011.
We are glad to provide 30-minute phone consultations to interested women, at no charge. Simply visit the website www.clearpassage.com.
Join us for our next posting on endometriosis and Infertility.