Lucine Health Sciences and Hormones Matter launched an important new research project one month ago. The Real Risk Study: Birth Control and Blood Clots is a multi-phased project designed to assess the breadth and depth of blood clot risks and other side effects associated with hormonal birth control. The current phase of the research involves collecting survey data and case reports from women who have suffered from blood clots while using hormonal birth control. Although data collection is still in the early stages (we have data from 42-50 participants, depending on the question), some important trends are already beginning to emerge.
Are Newer Users Really More At Risk?
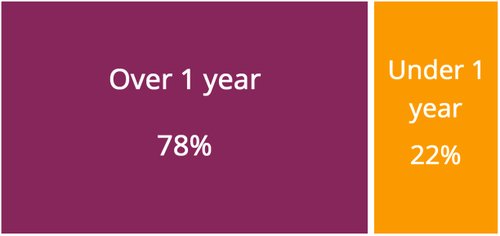
One of the statements often made in medical publications, and even stated in the pharmaceutical companies’ own package inserts, is that the risk of developing a blood clot on hormonal birth control is the highest among new users or those restarting (within the first year of use or re-use). In our study, we are asking the question “How many total or cumulative months or years had hormonal contraceptives been used prior to the clot?” In our preliminary data set of 50 women, only 22 percent developed blood clots within the first year of use. The majority of women, 78 percent, developed blood clots after the first year. From our data, it does not seem true that the risk of blood clots is highest within the first year of use.
Seventy-Eight Percent of Hormonal Birth Control Induced Blood Clots Develop After One Year
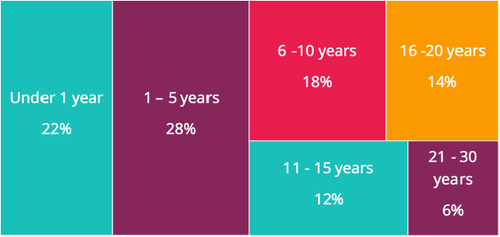
We further analyzed the data set to refine our understanding of when blood clots were developing relative to length of time on hormonal contraceptives. The chart below shows the percentage of women in our preliminary data set that developed clots after various lengths of time. The size of each box is proportional to the number of women in that group. Because the data is preliminary, and the number of women in each group is still small, we cannot really compare the sizes of the groups to each other until we have more data. However, we can say that women are developing clots after a wide range of time on hormonal contraceptives, even after up to 21-30 years on the medication.
Hormonal Birth Control Induced Blood Clots Develop More Frequently in Years 1-10
Cigarette Smoking as a Risk Factor for Blood Clots
We are also asking survey questions about known risk factors and possible risk factors, to try to get a clearer picture of all of the factors contributing to a woman’s risk of a blood clot while on hormonal contraception. Cigarette smoking is known to increase the risk of developing a blood clot, and it is referenced in the package inserts that come with birth control pills. In the information for Yaz, the most popular birth control pill in the U.S., the warning states:
WARNING TO WOMEN WHO SMOKE: Do not use YAZ or Beyaz if you smoke and are over age 35. Smoking increases your risk of serious side effects from the Pill, which can be life-threatening, including blood clots, stroke, or heart attack. This risk increases with age and number of cigarettes smoked.
However, it has been pointed out that the risk communication by pharmaceutical companies in these inserts employs language that is misleading about the true level of risk, and the message most women who read the inserts come away with is that if they don’t smoke and are not over age 35, they are not really at risk.
In our survey we are asking the question: “Were you a smoker at the time of the blood clot(s)?” So far we have collected data from 42 participants for this question. In our data set, 79 percent of women who suffered from blood clots while on hormonal contraception had never been smokers. Another 12 percent had smoked previously, but were not smokers at the time of the blood clots. Altogether, 91 percent of women in our study were not smoking at the time when they develop the blood clot(s). This means that women cannot be confident that they are not at risk just because they do not smoke.
While these results are very preliminary and will have to be confirmed with the larger sample pool and the additional validation studies we anticipate, the data collected thus far seem to suggest that risks described by the industry do not correspond to the reality of what women experience. Although some women develop clots soon in the weeks and months after initiating hormonal birth control, the vast majority do not. Similarly, although smoking is certainly a risk, not smoking does not equate with lack of risk. So what causes the blood clots in some women and not in others? That is what we are trying to determine with this study.
Birth Control and Blood Clots Is about the Chemistry
We know from the basic chemistry that hormonal contraceptives skew coagulation factors in favor of blood clotting in all who take them. The research on this is pretty clear. These synthetic hormones increase the coagulation factors by 170%, almost three times their normal levels. Simultaneously, hormonal contraceptives decrease the anti-clotting cascades by 20%. This alone is sufficient to create blood clots and yet, not all women who take hormonal birth control develop clots or develop them very quickly. In some cases, it is years before the clotting becomes problematic.
What causes some women to develop clots soon after starting hormonal contraception, versus those who develop clots after many years? What causes some women without any known risk factors to develop massive DVTs and/or massive bilateral pulmonary embolisms, and die in their twenties? Is it determined by genetics, by medication interactions, by lifestyle variables, or by various combinations of risk factors? We do not know. No study to date has been sufficiently comprehensive to determine those risks. The Real Risk Study is.
Participate in Research
Lucine Health Sciences and Hormones Matter are conducting research to investigate the relationship between hormonal birth control and blood clots. If you or a loved one have suffered from a blood clot while using hormonal birth control, please consider participating. We are also looking for participants who have been using hormonal birth control for at least one year and have NOT had a blood clot, as well as women who have NEVER used hormonal birth control. For more information or to participate, click here.














I love your work. This is exactly the kind of information that needs to get out there to women AND men. In my own experience it’s men prompting women to get on birth control because they “hate the feeling of condoms”.
Also I feel that a better hormonal free alternative should be adviced on this page. (I’m sorry if there already is, in that case I missed it!) For example the Fertility Awareness Method were the woman tracks her physical symptoms to know when ovulation occurs (and thus is fertile).
I feel that there is so much information only on hormonal contraceptives (at school, doctors office) all the while women are taught nothing about how their body and ovulation actually works. If only doctors would advice patients to start FAM, no side effects, but also no money to big pharma.