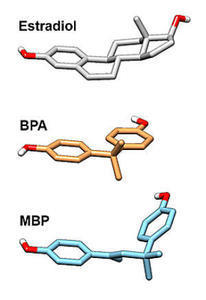
Bisphenol A or BPA is the ubiquitous estrogenic compound used to create plastics. It leaches into our food stuffs and because of its hormone-like qualities elicits a myriad of health issues in adults but especially in children and most especially when exposed in utero or during key developmental phases.
As we cover the expanding research base on BPA, it becomes increasingly clear that traditional methods of toxicology do not work for understanding endocrine disruptors – the man-made chemicals that alter our hormone pathways . A case in point, the latest research on BPA.
Exposure in Adults
A report published online in June of 2011 and presented at a prominent toxicology conference in February 2013, measured BPA exposure levels over a 24-hour period in adults fed a high BPA diet (lots of canned food and water from plastic bottles). The report showed that the concentration of BPA measured from blood was below the level of detection in most of the study participants, even though urine concentrations were extremely high and indicated exposure levels above the 95th percentile of the US population.
From urine tests, researchers were able to detect an average 84% – 97% of the dosed BPA and its metabolite, BPA glucuronide – indicating a high rate of clearance from the body. The ranges varied widely by time of day (morning tests showed significantly less clearance) and gender of participant (women did not process the hormone as well as men).
The researchers argue that their failure to detect BPA in blood, combined with the high concentration in the urine meant that risk was minimal. Their reasoning, even though BPA exposure was high, most of the BPA was cleared from the body rapidly and efficiently; no harm, no foul.
Medical and science marketers latched on to this and soon every major and minor media outlet was reporting that risks were minimal. Here are just a few headlines.
No Ill Effects Found in Human BPA Exposure, says the Wall Street Journal
Majestically Scientific Federal Study on BPA has Stunning Findings: So Why is the Media Ignoring it? – says Forbes
No toxic effects from controversial food packet, says expert – the Guardian
Ahh, where to begin?
Flaws in the Research
Conflicts of interest. Always look for industry sponsorship of for research, see my previous post on evaluating endocrine research for details. The relationship between the investigators in the present study and industry are muddled, but they do exist. For more information, click here.
Below the level of detection. When researchers report that their tests are unable to detect a visible pathology or measure a particular compound that any reasonable person would expect to be present, the test is likely at fault. Below the level of detection, means just that. It does not mean the compound was not present or that it was not exerting effects, only that the tests were not sensitive enough to measure the compound. This was case here and I suspect as testing methods improve, we’ll see higher detection levels in blood.
High clearance is not the same as never exposed. In this study, not all of the hormone was recovered in the urine, only an average of 84% – 97%. That sounds like a lot. With hormones, however, small amounts do great damage. Why? Because steroid hormones are stored in fat (and other tissues). They accumulate over time and metabolize into a myriad of different hormones (metabolites), some more potent than the parent compound. After the initial exposure and certainly after repeated exposures, our bodies become little (or big) hormone factories, storing and creating more and more hormones and hormone metabolites.
Metabolites matter. Hormones are shape shifters. Every time they meet an enzyme, the interaction between the enzyme and the hormone creates a new, similar, but differently shaped hormone. Hormones are never ‘one and done’ metabolizers. Even though a large percentage of the original hormone and its primary clearance metabolite were measured from urine in the present study, one cannot assume that there were not still other metabolites circulating within the body and wreaking havoc.
BPA has metabolites. This is critical and often ignored in toxicology research. BPA is a hormone like substance and as such, it metabolizes into many different forms. BPA has metabolites that are more potent than BPA itself. New research shows that BPA metabolizes into a compound called 4-methyl-2,4-bis(4-hydroxyphenl)pent-1-ene or MBP for short. MBP is 1000-fold stronger than BPA in its estrogenic effects. MBP binds strongly to both types of estrogen receptors (ERa and ERb) and may change the activity of the cell, displacing native or endogenous estradiol. So within that 3%-16% range of BPA not cleared, comes a compound 1000 times stronger than the BPA itself. As the research progresses, who knows how many other active and potent metabolites from BPA or MBP we’ll see. With hormones, nothing is simple or straightforward.
What this Means
Avoid medical marketing, it’s usually incorrect. Learn how to evaluate endocrine disruptor research. Once you get the hang of it, you’ll be able to dismiss faulty research at a glance. More importantly, learn about hormone systems and environmental hormone disrupting chemicals. Otherwise, our children will bear the brunt of our ignorance.
A good review article: Bisphenol A and the Great Divide: A Review of Controversies in the Field of Endocrine Disruption.