I went to the doctor in early January 2008 and during the consultation was asked if I’d had my Gardasil shot. There was no discussion about possible side effects and I was urged to have it while it was still free. So I had the first shot then, just before my 26th birthday. I had the second shot at the end of February.
I was healthy, fit and enjoying life. I was working in retail and there was talk of promotion and management training. My long term plans included a career change so I was training at the gym regularly to get my fitness level up. I passed a thorough preliminary medical examination in early May.
A Delayed Reaction to Gardasil?
In mid-May, I broke out in a rash. Originally I thought it might have been bed bugs or a reaction to laundry powder but it persisted and the doctor thought it was an allergy of some sort. I was put on antihistamines but the rash continued. One day my eyelid was swollen. Another day my lip swelled up. It seemed random and puzzling.
In June, I had my third Gardasil shot and then things really started to rev up with the symptoms escalating in frequency and severity.
It was then, that I started keeping a health diary to track what I was eating, what medication I was on, and what symptoms I was experiencing. After a few weeks I realised that it was not related to what I was eating, so just recorded medication and symptoms being experienced.
By July, the rash was all over my torso, legs, and arms and my face. It would sometimes come up in great welts. One night my thighs were blood red and so itchy I thought I’d go mad. One day I woke up and my entire face was so swollen, I looked like I’d been beaten up and I could barely recognise myself. My hands and feet would swell up and be so painful I could barely walk. My wrists and ankles ached and I had trouble sleeping because every time I moved I was in pain. I had strange bald patches on my tongue.
A Post Gardasil Inflammatory Condition
I had so many blood tests I felt like a pin cushion. In early July the doctor rang back to say my recent blood tests showed elevated CRP levels (an inflammatory indicator). I went back for weekly blood test, and the CRP levels continued to be elevated and rising higher each week. Up until then I had been seeing different doctors at different clinics so my mum suggested I see her doctor, Dr R, so there was some overview perspective.
By this stage I had taken so much time off work that I ran out of sick leave and went onto sickness benefits.
Dr R tried to get me an appointment with an Allergist but the waiting time was 10-12 weeks, and I was put on the cancellation list. In the mean time I went gluten-free and cut down on processed foods. Nothing worked.
Idiopathic Urticaria and Angioedema
On the 24th July my tongue started to swell. My mum drove me to the Emergency Department of The Alfred Hospital. I thought it will be just like on ‘House’ or ‘All Saints’ and the doctors will solve the riddle, provide a diagnosis and cure me. But no such luck. I was told I had “idiopathic urticaria / angioedema”. They couldn’t say what caused it and all they could do was try to control the symptoms. After spending hours there I was eventually sent home with a script for high dosage antihistamines – I was on 2 x 24 hr strength tablets twice a day. One thing I learnt was that I was meant to be taking 2 different types of antihistamine, R1 and R2, for the urticaria.
The doctors assured me this would control my symptoms. It didn’t.
Connective Tissue Involvement
I managed to get an appointment at short notice – there had been a cancellation- to see Dr S, a Specialist Physician (specialising in diagnosis), on 25th July. He took thorough notes of my history and symptoms. He said clinically it looked like connective tissue involvement suggestive of rheumatoid arthritis or a lupus-type condition. He ordered more blood tests, including a specific one for lupus. He also said not to worry too much as clinicians had recently being seeing patients presenting with what they were calling ‘pseudo lupus syndrome’. Could these pseudo lupus syndromes be related to the Gardasil vaccine or other medication reactions? I wonder.
Swollen Tongue
On 14th August, exactly three weeks after my previous visit, I was back at the Alfred Hospital Emergency Department. Three weeks of the treatment had not controlled the symptoms, but had left me physically weaker – I was nauseous, tired from lack of sleep and in pain. I went to the Emergency Department at 10.15 pm as the back of my tongue was swollen and there was a strange feeling in my throat. I felt like I had a large bubble in my throat and it was difficult to swallow. The Alfred Hospital staff were spectacularly unhelpful – I was told to report back to the desk if unable to breathe. Over the next hours the swelling seemed to stabilise in that it wasn’t getting worse. I left The Alfred at 12.30am having not been seen and I got home at 2.30am. At about 6.30am the swelling suddenly started to increase and I had difficulty in swallowing. My mum came and collected me and we went straight to see Dr R. She said in over 30 years of practice she had never seen or heard of anything like it. I was put back onto cortisone.
On 20th August I had my revisit with Dr S. The blood test for Lupus was negative, so I was one of the ‘pseudo lupus syndrome’ patients. He recommended I see a Rheumatologist rather than an Allergist or Dermatologist. He said that, in Melbourne, Immunologists tended to be research rather than clinical, and that Rheumatologists were the autoimmune specialists. So, onto another waiting list to see a yet another specialist – an appointment was made with Dr A for 9th September.
On the 2nd September I finally got to see an Allergist. He recommended a very restricted “elimination diet” which, by that stage, I didn’t have the energy or inclination to follow. I had worked out weeks earlier that the swellings were not related to what I was eating. However, I did buy some allergy free soap, toothpaste and shampoo. And he provided a list of foods/drinks to avoid because of preservatives.
A Heart Murmur
On the 9th September I saw the Rheumatologist Dr A. Like Dr S she took a comprehensive history. She ordered an extensive battery of blood tests – for HIV, Barmah forest virus, Ross river virus etc. On examining me she detected a heart murmur and ordered a chest CT scan and echo cardiogram. One thing I was sure about was that I had no heart murmur when I passed the comprehensive medical back in May.
Still No Answers
It was the same old story: Dr. A as a Rheumatologist was a connective tissue specialist, not an autoimmune specialist. She suggested seeing a clinical Immunologist, Professor H, and appointment was arranged for 13th October.
So I spent months on high-dose antihistamines and intermittent short courses of cortisone. The cortisone initially controlled the rash, but as soon as I stopped the treatment the rash came back. Eventually the rash appeared even when I was on cortisone. So the recommended treatment didn’t work. What was worse was that the doctors seemed mystified and perplexed by my multitude of symptoms.
By this stage, based on my diary, I was seeing some emerging patterns: The symptoms appeared more severe around the time I got my period; and also after exercise, if I went to the gym or personal training. I also had the feeling that the antihistamines may have been actually exacerbating the symptoms, particularly the swellings. The most striking instance occurred on the evening of 14th August within 15 minutes of taking the histamines, my lip suddenly started swelling up and then the swelling progressed to my tongue and throat.
Unstable Mast Cells
A breakthrough of sorts came when a colleague gave Dr R an information sheet about Ketotifen – a mast cell stabiliser – that seemed to explain and (hopefully) treat my symptoms.
Apparently people with chronic urticaria and angioedema do not suffer from specific allergies, but rather an unstable mast cell system. According to the fact sheet, the unstable mast cells leak histamine, prostaglandins and leukotrienes, which result in other associated symptoms, such as headaches, tiredness, lethargy, irritability and difficulty in concentration. It can also affect the gastrointestinal tract causing cramping, bloating, indigestion, regurgitation, flatulence, intermittent diarrhoea and constipation. Many patients suffer from joint pains and muscle pain. These symptoms are due to the inflammatory properties of leaked histamines, prostaglandins and leukotrienes. I was unable to see the doctor who wrote the information sheet, as he only saw asthma patients.
Also, Ketotifen was not available in tablet form in Australia and we had to send to New Zealand for it. Ketotifen is only available in Australia as eye drops. A friend sent me an advertising leaflet for Zaditen “the only triple action, anti-allergy eye drops for symptomatic short term treatment of seasonal allergic conjunctivitis available over the counter without prescription.” Strangely, it was titled Zoe’s Dilemma and featured a cartoon of teary-eyed Zoe “I’ve got minutes to pull myself together!” being ZAPPED with Zaditen by a handsome young white-coated healthcare professional, saying “Only I can give you a quick solution”.
By the time we sent to New Zealand, received the tablets and found a doctor willing to oversee it, I didn’t start the Ketotifen until September. Gradually the swellings became less frequent. The rash remained but became more “normal”.
Back to Urticaria
When I saw the Clinical Immunologist, Professor H, on 13th October he was the first health professional I’d seen that wasn’t mystified by my many and varied symptoms. He diagnosed severe chronic urticaria and, when shown my photos, said they were classic of severe urticaria. In terms of severity, my condition was in the top 5% he had seen.
He went on to explain that an unstable mast cell system was the basis of all autoimmune conditions. Researchers were just starting to unravel how the immune system works, particularly autoimmunity. He said that researchers had recently discovered that unstable mast cells leaked many chemicals, much more than previously thought (i.e. many more than mentioned in the Ketotifen information sheet). He was currently supervising a PhD student researching this topic.
I queried how it was strange I should, within a two month period, be so badly affected -particularly as I had been so fit before. Professor H said that, for some reason, the fittest people were often the most severely affected by autoimmune disease. It was as if their immune systems were also super fit, and turned in on the body with extra zeal. He also said that there was evidence in support of my intuitions – that symptoms were often worse after exercise; and, for women, worse around the time of menstruation.
The only recommended treatment was a long-term course of high dose cortisone. He explained that long-term cortisone use had some nasty side effects. Although he couldn’t guarantee it, he was confident that the treatment would get rid of the rash. He couldn’t say how long I would have to stay on cortisone. I was to think about the pros and cons of this, and decide whether to start the cortisone when I came to my next appointment in December.
Alternative Therapies
On 28th November I consulted a Traditional Chinese Medicine practitioner, Dr Z. He was the first health practitioner I had seen who was confident that the rash could be treated successfully. He said there were acupuncture and Chinese herbs specifically for it. I had the treatment and the rash disappeared.
I don’t know whether it was the acupuncture or a combination of acupuncture and the Ketotifen, but something finally worked. I was still having intermittent swellings, but at least the rash was gone.
When I revisited Professor H on 2nd December, the rash was gone. I decided to stick with the Ketotifen for another 4 months as recommended on the information sheet.
I did remain rash free taking just the Ketotifen, and then remained rash free when I stopped it in March 2009.
The whole experience left me exhausted, I felt as if my life had been put on hold for months. I had to take time off work and could only work part time after that. Not only did it cost me a lot financially in terms of being off work, I had to spend a fortune on antihistamines, Ketotifen, painkillers, indigestion tablets, and assorted other drugs.
In March 2009, just after finishing the Ketotifen and possibly as a result of all I’d been through, I experience for the first time ever an episode of acute anxiety and panic attacks for which I had treatment and counseling.
And Now Cervical Cancer
The biggest shock occurred in March 2011 when I went for my regular pap smear and was diagnosed and treated for cervical adenocarcinoma in situ (AIS). This was 17 months after my previously normal Pap smear, and three years after the first Gardasil shot. All of my previous pap smears had been clean.
I went for my regular pap smear with Dr P. early March 2011. A week later he rang me to say the report was showing glandular-cell abnormalities and I was to come in the following Tuesday for an assessment. [There are two main types of cervical cancer: the more common squamous-cell abnormalities and cancer (squamous carcinoma); and the rare but more aggressive glandular-cell abnormalities and cancer (adenocarcinoma)].
The following Friday I was in surgery and had a cold knife cone biopsy. The results came through the following Wednesday that the margins of the cone biopsy were clear.
I am very aware that I was fortunate – having my screening with a specialist colposcopist and having the surgical procedure within 10 days of the results being received. As a result of this, the cancer was detected early, at the in situ stage.
I have to have a follow-up screening every 6 months to make sure the cancer doesn’t return, and so far so good. I’m reassured that I’m having reliable and expert follow-up
So not only did I experience severe adverse reactions to the vaccine, it is obvious that Gardasil does not even protect against the serious cervical cancer: glandular cell cervical cancer. As AIS is thought to be caused by HPV 16 and 18, the exact viruses the Gardasil vaccine is supposed to protect against. Since I didn’t have the either HPV or cancer a mere 17 months prior to my vaccination, I have to wonder whether the Gardasil vaccine introduced the virus and the cancer into my system.
Recurrence of Urticaria and Angioedema
In June 2011, maybe as a result of stress, I had a recurrence of the urticaria/angioedema, including swelling of my tongue and throat. This time I was touring around Cornwell, UK so it was a little scary not knowing where to locate the local doctor or hospital.
When I saw Professor H a couple of months later, he said researchers in Australia had now developed a new version of the mast-cell stabiliser. It was being trialled with impressive results and they were trying to get the government to approve its use in Australia. He suggested that, as the Ketotifen had worked for me before, I go back onto it. When I eventually got the capsules for New Zealand and started taking them, the symptoms gradually subsided.
When I was telling Professor H. about being in Cornwell at the time of the recurrence, he said “Just as well your tongue didn’t start to swell.” On hearing that I’d had episodes of my tongue and throat swelling both recently and in 2008, he immediately wrote out a script for an epi-pen and told me to carry it at all times. As my mum later commented, it would have been helpful to know this three years earlier in 2008.
Six Years Post Gardasil
So how am I, six years on? I am still struggling with the aftermaths of Gardasil.
Although the urticaria / angioedema haven’t reoccurred for 3 years, I am struggling with an “invisible” legacy of insomnia and fatigue.
My sleep pattern is extremely disrupted. I have had a problem with insomnia since a teenager but, post-Gardasil, this became much more severe. I have been experiencing the strange situation of having no energy, being extremely fatigued, and yet I can’t get to sleep.
In 2010, I made the decision to return to study and relocated to Geelong (about an hour away from Melbourne) to attend Deakin University. Distance, work and university commitments made it impossible to have consistent follow-up treatment with Dr Z. TCM seems the best prospect to help with my sleep/energy problems, but unfortunately wasn’t an option for me at the time. I didn’t have the energy to go another round of finding local doctors, explaining symptoms, having more blood test, etc. So I battled on as best I could – herbal tea, Valerian, prescription sleeping tablets – nothing worked.
After the 2011, recurrence of symptoms my sleep patterns were even more disrupted. Early in 2012, I saw Dr M., a sleep specialist, and did a sleep test. I was awake all night and was officially diagnosed with sleep narcolepsy – falling asleep during the day due to exhaustion from insomnia.
A more visible legacy of Gardasil has been with my skin. Post-Gardasil my skin has been shocking with acne much worse than I’ve ever experienced, even when I was a teenager.
On reading Gabriella’s story I realise that maybe I can finally find some answers to regaining my health… it’s just a matter of knowing where to start and who to see.
However, the main message I want to get out to other Gardasil women – and all young women – is the need for annual pap smears. Dr P, who diagnosed and treated me for cervical adenocarcinoma, says there has been an increase in the number of young women developing this type of cancer, and that annual Pap smears are essential to monitor for it. Again, I have to wonder if the Gardasil vaccine and the increase in cervical cancers in young women are connected.
Pap smears saved my life, not bloody Gardasil.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Image by manseok Kim from Pixabay








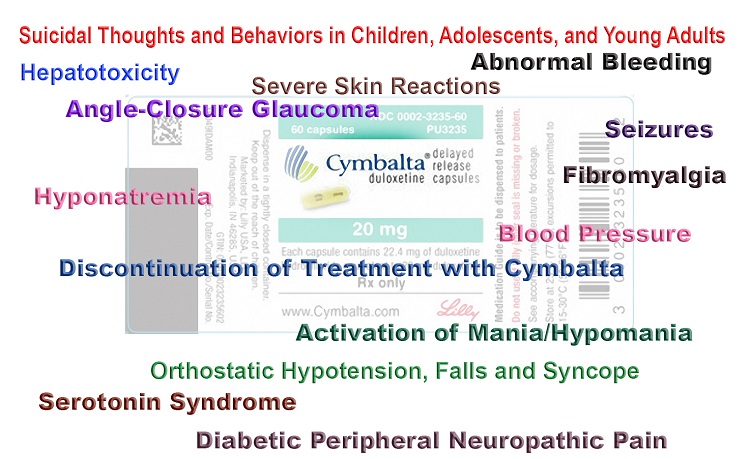



Our body is equipped with a powerful set of tools for resisting invading microorganisms such as viruses, bacteria, and parasites. Unfortunately, these set of tools, or the immune system, sometimes goes awry and attacks our body. These misdirected immune responses are referred to as autoimmunity. In case you are experiencing any abnormalities in your body, go seek autoimmune specialist ASAP.
Same here! I don’t have hpv but have AIS and have received the guardisil vaccines I wonder the same thing
Good on you for speaking up Zoe. It isn’t fair you went through all that trauma whe you were only trying to protect yourself and following doctors orders. Hoping your symptoms have eased now and you feel better. Xo
Thank you for sharing your story. My daughter received Gardasil at age 11 and this is her story. I have seen that rash many times. There are pics of Autumn with it here,
http://vaccineimpact.com/2015/the-gardasil-vaccine-after-life-my-daughter-is-a-shadow-of-her-former-self/
Thank you for sharing your story. It is very scary, and very heartbreaking. Pharmaceutical companies should not get away with releasing products that are obviously not tested enough. I am very sorry to hear about all of your problems and wish you well.