What is the Best Diet?
I have been working with tens of thousands of migraine sufferers from all over the world for nearly 8 years. During this time, a great many migraineurs have learned to become migraine free by following nutritional and lifestyle changes, that is, the Stanton Migraine Protocol. The process of recovery starts with understanding the migraineur’s health condition prior to implementing any changes. For instance, I request all new members to provide me with a specific list of blood tests.
Over the years I have looked through a tremendous number of blood tests. Two of the standard items on the test list are fasting blood glucose and the lipid panel—a.k.a. cholesterol. More often than not, migraineurs need to entice their doctors to order basic tests because doctors are suspicious of anything their patients initiate.
So, imagine when one of my migraineurs suddenly popped into my Facebook group to post a 7-year-long history of her blood glucose and lipid panel results. What instantly caught my attention was how clearly her stages of dietary changes were documented by her test results: first on the SAD (Standard American Diet), then on a vegan diet, dropping all meat and dairy, and finally on a very strict version of a vegan diet with 80% carbohydrates, 10% protein, and 10% fat. Let me show you what I mean.
Blood Glucose and Cholesterol Refresher
Most people are quite familiar with what cholesterol and blood glucose tests are but there is confusion about what they mean.
Blood glucose is often measured because it is easy to check (even at home) health status about how one’s body can handle carbohydrates. Carbohydrates turn to glucose and all plants and their processed derivatives have carbohydrates. So foods such as bread, cereals, pasta, pizza, all fruits, and all vegetables—including salads, beans, and nuts—convert to glucose. Of course, sugar, honey, and any syrups and sweetened drinks all show up as an increase in blood glucose.
The ideal blood glucose range is 70-99 mg/dL at all times, though there is some allowance given for a short period after consuming a meal. It is recommended to never go past 140 mg/dL. Fasting blood glucose, tested on typical laboratory blood tests, is based on 10-12 hours of fasting, meaning not eating anything prior to the test, not even vitamins.
As already mentioned, fasting blood glucose between 70 and 99 mg/dL is healthy; between 100-125 mg/dL is considered to be prediabetic, and 126 mg/dL or over is diabetic (see here).
Cholesterol is a bit more difficult to interpret. The standard lipid panel that is supposed to test cholesterol actually can’t give any real information about cholesterol—the test itself lacks the kind of sensitivity that would be able to measure cholesterol.
Cholesterol is a most essential substance in the human body, to the point that if we don’t get enough of it from our food, we make what we need on our own. Since Wikipedia has a great description of everything you ever wanted to know about cholesterol, I only discuss the very basics here.
Cholesterol is a waxy substance that gives integrity to cellular membranes, is the building block of our hormones, and also makes up a very large part of our brain. Over 25% of all the cholesterol in your body is in your brain (see here), which together with fat take up over 65% of the brain (see here).
In the lipid panel blood tests we can distinguish several elements: HDL, LDL, Triglycerides, Total cholesterol, and often some residual factors.
- HDL: not cholesterol but a lipoprotein ball—a vessel, which contains cholesterol that it picks up from cellular activities. It is the “cholesterol recycler” and so it is known as the “good cholesterol” even though it is not cholesterol.
- LDL: not cholesterol but also a lipoprotein ball—a vessel, which carries cholesterol to cells for support. In addition to cholesterol, it also carries triglycerides, and all fat-soluble vitamins, such as vitamin A, vitamin E, vitamin D3, and vitamin K2, all of them extremely essential for our health. LDL is referred to as the “bad cholesterol”, though note it carries important fat-soluble vitamins, so it cannot be all that bad.
- Triglycerides: not cholesterol but a fatty acid, created by the liver as a form of storage for excess energy we have consumed—converted primarily from excess carbohydrates.
- Total cholesterol: this is the sum of the good cholesterol HDL, the bad cholesterol LDL, and one-fifth of the triglycerides. Total cholesterol is not very meaningful, it may be high simply because the good cholesterol is high and so it is often flagged for no reason.
You may have noticed that none of the lipid panel components is really cholesterol, this fact plays a large part in the general confusion about cholesterol.
The current generally accepted guidelines recommend that for optimal health the following should be met:
- LDL should be <100 mg/dL.
- HDL should be >40 mg/dL for males and >50 for females.
- Triglycerides should be <150 mg/dL.
There may be some variations on the above, depending on the laboratory where the tests are done.
From Good to Bad to Ugly
Start: The SAD Diet
Let us now follow the actual test results of our migraine group member through her dietary changes. Her starting test results from (3/10/2014), while she was on the SAD diet, were:
- Fasting blood glucose: 90 mg/dL, perfect.
- HDL: 67, so way above the minimum recommended, very good.
- LDL: 139, slightly higher than recommended.
- Triglycerides: 60, well within the recommended range, very good.
Just looking at these data, she was actually quite healthy at this time. The modern cardiovascular risk analysis is based on the triglycerides/HDL value (see here). This only works in mg/dL so if your cholesterol test results are in a different unit, they need to be converted first. The cardiovascular risk is scored as follows:
- Ideal 0.6 -< 1
- Good 1 -< 2
- Barely acceptable 2 -< 3
- Heart attack is waiting at the door if > 3
Our migraineur’s score was 60/67 = 0.895. As you can see, on the SAD diet her risk score was well within the best score possible. Nevertheless, her doctor—a cardiologist—still recommended a change to a plant-based (vegan) diet, seemingly based on the slightly elevated LDL test result.
Change in Diet
The Vegan Diet #1
It is difficult to not hear and read everywhere today how great the plant-based diet is. In fact, some European countries don’t allow children to take animal-based products for their school snacks (see here) and others simply dropped all meat options in the canteens of schools (see here). In the US too (and in 40 other countries), there is “Meatless Monday”, and also a huge push elsewhere for increased prices and taxes on meat products referred to as “sin tax”.
Vegetarianism and veganism are strongly encouraged in most of the Western world. People assume that they must then be good for health, but is that really so? Or is the benefit of the plant-based diet a myth?
Our migraineur followed her cardiologist’s direction to the T. She dropped all meat and dairy, turned vegan… and then… well… her blood test showed something unexpected.
Her first 4-year vegan-period values are as follows:
| Date | HDL | LDL | Triglycerides | CV Risk (triglycerides/HDL) |
| 3/18/2016 | 56 | 113 | 105 | 1.875 |
| 7/20/2016 | 61 | 134 | 103 | 1.688 |
| 10/20/2016 | 64 | 152 | 131 | 2.047 |
| 5/17/2018 | 71 | 162 | 139 | 1.958 |
| 1/10/2019 | 65 | 176 | 119 | 1.831 |
| Average | 63.4 | 147.4 | 119.4 | 1.88 |
Since she started the vegan diet to improve (reduce) her LDL, let’s compare her cholesterol results on the SAD diet against the vegan diet for which I averaged the 5 tests:
| Type | HDL | LDL | Triglycerides | CV Risk (triglycerides/HDL) |
| SAD | 67 | 139 | 60 | 0.895 |
| Vegan | 63.4 | 147.4 | 119.4 | 1.88 |
As you can see, every marker that should have gone down (LDL and triglycerides) increased and the one expected to increase (HDL) dropped while following the vegan diet. Her cardiovascular risk score increased and was no longer in the ideal range, though it was still good.
Her fasting blood glucose has also been recorded, and she shared her 5 test results:
| Date | Fasting blood glucose in mg/dL (ideal 70-99 mg/dL) |
| 3/18/2016 | 88 |
| 7/20/2016 | 113 |
| 10/20/2016 | 116 |
| 5/17/2018 | 122 |
| 1/10/2019 | 122 |
| Average | 112.2 |
Her fasting blood glucose increased from the ideal of 90 mg/dL that she had during the SAD diet to prediabetic at 112.2 mg/dL on 4 years of a vegan diet. So her fasting blood glucose too moved exactly opposite of what the doctor was hoping to see.
The Vegan Diet #2
Consequently, the cardiologist told the migraineur that she needed to double down because the markers moved in the undesired direction. So the migraineur restricted her fat and protein to the absolute minimum of 10% each and increased her carbohydrates to 80% of her calories. She followed this extreme vegan way of eating for nearly 3 years religiously. Here are her 5 blood test results for cholesterol this period:
| Date | HDL | LDL | Triglycerides | CV Risk (triglycerides/HDL) |
| 4/25/2019 | 70 | 173 | 111 | 1.586 |
| 5/15/2020 | 42 | 134 | 121 | 2.88 |
| 8/14/2020 | 46 | 134 | 121 | 2.63 |
| 12/4/2020 | 51 | 172 | 155 | 3.039 |
| 3/14/2021 | 52 | 146 | 158 | 3.0385 |
| Average | 52.2 | 151.8 | 133.2 | 2.552 |
So let’s compare now her cholesterol on all three diets: the SAD, vegan, and extreme vegan:
| Type | HDL | LDL | Triglycerides | CV Risk (triglycerides/HDL) |
| SAD | 67 | 139 | 60 | 0.895 ideal |
| Vegan | 63.4 | 147.4 | 119.4 | 1.88 good |
| Extreme Vegan | 52.2 | 151.8 | 133.2 | 2.552 barely acceptable |
Wow! Everything was heading in the wrong direction! Her HDL, which should have increased, decreased further after she went nearly fat and protein-free. Her LDL and triglycerides were supposed to decrease but both have increased, extremely so on the extreme vegan diet. But by far the worst news was her cardiovascular risk score, which went from a completely normal level on SAD to approaching serious cardiovascular risk for damage and possible heart attack! And all this happened by switching from an unhealthy SAD diet to a “very healthy” vegan diet???
And what about her blood glucose after she tightened her belt and moved to the extreme vegan diet?
| Date | Fasting blood glucose in mg/dL (ideal 70-99 mg/dL) |
| 4/25/2019 | 128 ==> Diabetic! |
| 5/15/2020 | 104 |
| 8/14/2020 | 111 |
| 12/4/2020 | 115 |
| 3/14/2021 | 124 |
| Average | 116.4 |
Her fasting blood glucose changed from excellent to bad to worse as she changed to the vegan and the extreme vegan diet! From 90 mg/dL to 112.2 mg/dL to 116.4 mg/dL, meaning from healthy to pre-diabetic to worse pre-diabetic (closer to diabetic). In the extreme vegan set of blood tests, she even managed to acquire a clearly diabetic fasting blood glucose value (128 mg/dL) at one point in time.
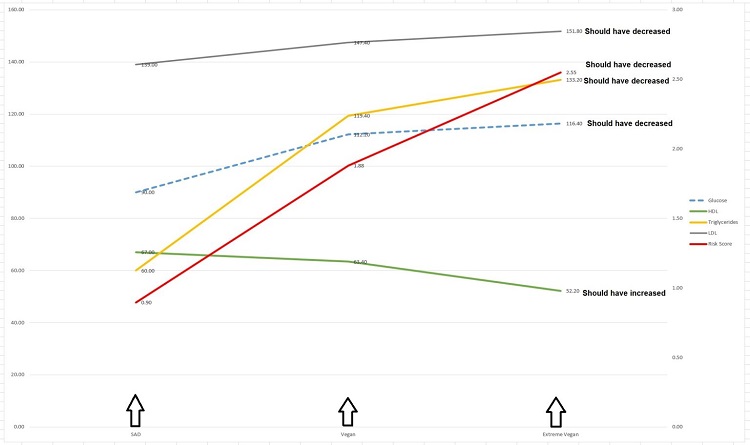
The graph above summarizes the outcome of the three different ways of eating over the seven years of testing.
Over the 7 years of vegan dieting, a completely healthy individual turned into a sick person with type 2 diabetes and the risk of a potential heart attack. And all this on the advice of her cardiologist. Lovely.
Conclusion
This migraineur joined my migraine group a couple of months ago and started the carnivore diet approximately 5 weeks ago. In the migraine group we run a Kraft in Situ mimic test where the migraineur measures blood glucose and blood ketones fasted, pre-meal, and then starting 30 minutes after the last bite of food, the migraineur takes blood samples every 30 minutes for 5 hours. On her first test, shortly after she joined, she showed all the signs of prediabetes. Only a couple of weeks into the carnivore diet her fasting blood glucose was back to normal at 89 mg/dL.
On the carnivore diet, she has cut out all plants and only consumes animal foods high in protein and animal fats. She now eats meat, poultry, fish, seafood, organs, animal fats, dairy, and lots of eggs. The only non-animal foods that those of my group members who are advised to be on the carnivore diet can eat are mushrooms (fungi) and seaweed (algae) as these are not plants.
As for this migraineur, it is too soon to see major improvements in her health after 7 years of serious damage. Her fasting blood glucose is already back to normal and we have yet to see her cholesterol results. Based on my experience of over ten thousand migraineurs in my Facebook migraine groups, and the many blood tests I have seen over the years, the expectation is a complete reversal of her HDL to be high again, triglycerides to be low again, and with that her cardiovascular risk score to drop back to normal. Her LDL will likely increase because it will be carrying lots of fat-soluble vitamins and minerals that are only found in animal products.
I hope that this shows you the importance of eating the appropriate human species foodstuff, which includes—as it always has included during human evolution—lots of animal products. The vegan diet is clearly not the way most people’s health will improve. There might be some individuals for whom the vegan diet is harmless, but it is dangerous for the majority of people.
Don’t follow a diet because your friends do. Unfortunately, you also have to be skeptical of the advice of many healthcare professionals. Follow the data and how you feel. Eat the way that is healthy for you.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, and like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
This article was published originally on June 24, 2021.













Yes vegan diets are healthy for our heart. I am having vegan lifestyle since 2007 and still my heart is in great condition. So, I believe veganism is best for heart health.
I’ve been vegan for over 10 years, vegetarian many prior to that.
My blood metrics have always been excellent.
Inflammation about zero.
Testosterone high.
Research shows the best diet is plant based or largely plant based.
Dear Robert,
The plant-based diet research–all of them, with the exception of 1–showed no such benefit whatsoever. They only studied if cholesterol was lower or higher but we all know by now that lower cholesterol doesn’t represent better health. The one study that ran a real clinical trial, messed up by giving education to those on the plant-based diet leg to not smoke, exercise, etc. So the benefit(s) of the diet in this clinical trial was the result of: food? Not smoking? Exercise? We haven’t the clue, because that was not tested. The clinical trial was deliberately mishandled to tilt the benefit to what appeared to be the plant-based arm, but which was the non-smoking and exercise arm.
The most highly rated so called Mediterranean diet also has absolutely nothing to do with the real Mediterranean diets they are referring to. I know. I was there in those years when they ate the foods that made the Mediterranean diets famous: lots of pork (salted, think prosciutto and similar), lots of cheeses, lots of fish, butter and cream in and on everything, almost no desserts only seldom, and very little salads–usually only antipasto, which is mostly veggie-like fruits. I didn’t see a single person eating salads and plants as a meal prior to my arrival in North America in the 1970s.
By contrast, throughout human evolution over a few millions years, humans were scavengers and meat-eaters. Had it not been for your meat-eating ancestors, you would not be here to comment on this article. Whether you are an individual who gets good results from the plant-based diets is largely based on genetics becuase a very small percent of the population have adapted to plants. Perhaps you are in that very small percent. Still, you are only here on earth becuase your ancestors ate meat. And so you cannot exclude that from your life history, even if you wish it didn’t exist or weren’t true very hard.
In addition, we shall see as you get very old and then compare. Shall we?
Best wishes,
Angela
Angela you are a gem! I went the vegetarian/vegan route and am still paying for it so I think it’s great to have as many spreading these truths as you have, as possible. I see it all the time in my practice and the most unfortunate part is muscle loss. You can usually tell when a grown adult is a vegan because they typically look emaciated if doing it for any significant amount of time and the amount of muscle on our body is one of the greatest defenses we have against death and disease. And don’t even get me started on what plant based diets are doing to our planet and the humans inhabiting it. I think one could argue that the majority of us are plant based now based on our consumption of overly processed plants foods and seed oils and look how much we’re (NOT) thriving.
Thank you for this article! We need to spread this message like wildfire!
Dear Troy,
Thank you for your support. Indeed! Don’t get me started either on what damage plant-based dieting does to our plant!
Stay strong and healthy,
Angela
Very informative.
I emailed ADA and asked, can T2D or pre-diabetes, be reversed.
They replied
“There is no known cure for diabetes, so once a person is diagnosed with type 1 or 2, it cannot be reversed. However, with a good treatment plan, one can live a long healthy life”.
Just crazy.
I was wondering how vegetarians coped with T2D, before insulin was produced,
Vitamin B12 etc.
Did they eat meat or how did they supplement nutrients missing?
I was just wondering if you know about that.
regards
OMG thanks Glyn. You got a hilarious response, as expected. I recommend you read the explanation why you got that response here.
In terms of your question about vegetarians and vegans:
Vegetarians:
There are many types of vegetarianisms. In older countries of vegetarianism, people drink milk and eat cheese, so they receive their important nutrients that way. India, for example, has such long history of doing that and also raw milk has all the nutrients one needs, including B12.
Some vegetarian societies eat eggs and some also fish. So these people get all their nutrients because egg is a whole animal and fish, fish oil, etc., have all they need.
Other types of vegetarian system, where they eat nothing of animal origin, I would classify as vegan.
Vegans:
There are no known vegan cultures on the planet. Veganism is relatively new. The term “vegan” is less than 100 years old. There have always been small groups of people who ate no animal products dating back to about 900 A.D. It was usually reserved to people of special faith. The lack of B12 can create weird sensations in brain and body. It can make them sick such that they may interpret it religiously as a calling. As a child when I ran out of B12 to dangerously low (I was 19), I was experiencing very weird sensations that I could very easily have interpreted in a religious way! It places one into a strong trans that requires lots of meditations to come over so long as B12 isn’t available–or isn’t known to be missing. So from my personal experience, severe B12 deficiency does feel like a serious religious inspiration. 😉
There is another trail of thought, in terms of how people who ate vegan yet got their B12, and that’s through the soil. The plants were eaten without washing. Washing veggies and fruits is a Western Civilization invention starting in the 20th Century. Prior to that no one washed anything. The earth around veggies is full of microbiome and they provide the necessary nutrients, including B12. This biome is so vital of a nutrient that our closest ancestors, the chimps, eat their own feces for B12. B12 is generated by the gut flora and those animals with hind fermentation (including humans) only can access it via eating their feces or eating meat. Chimps, by the way, eat meat, so they aren’t vegetarians either. There is no known human vegetarian ancestor.
In terms of the other nutrients, such as iron, DHA/EPA, and other primarily animal origin nutrients, vitamins and mineral, these can be created from plants via conversion. Humans are really bad at converting ALA found in flax seeds, for example, to DHA. The average conversion in males is less than 1% and in females it is a bit better, I think 4-5% or something like that. So vegans must eat a ton of flax to get the necessary DHA for their brain. Our brain is over 85% fat (DHA) and cholesterol. Luckily cholesterol is so essential that humans make their own and we need not eat it.
And here we also need to look at health and longevity. People in all cultures prior to now lived shorter lives–except in tribal cultures where they predominantly ate animal products, but even there parasitic diseases as well as having been killed by predators was the cause of taking lives at an earlier age. Today we live much longer and have no parasite issues (usually) and our longer life is also enhanced by supplements and medicines. While deficiencies in B12 would have likely killed a person prior to reproduction in earlier societies if they were fully vegan and washed their veggies, and we don’t know if they have lived long or healthy lives, today we have a problem of washing everything and so no chance for earth flora to help with B12.
One of the documentaries of Tribes (Amazon Prime) I saw a person with D3 deficient genes. Although the person was on the sun all day long of his life every day, still D3 deficiency showed severe bone deformities and was bent over with a strongly curved back and major rounded out legs to the side. I have no way of knowing how old that person was but didn’t look old–though in tribes like this the only sign of aging is white hair because the elderly remain as youthful and agile as the young through their death. It is likely that a person like this may not reproduce in a tribe, preventing future problems in later generations. This type of deficiencies may not be clearly evident to a modern society with the possibility of supplementing and so we may have a lot more people today who are unable to absorb B12 or D3 animal-only vitamins.
In terms of “how vegetarians coped with T2D, before insulin was produced”: I think type 2 diabetes (T2D) rarely existed prior to the discovery of insulin and the few that did, were all placed on the low carbs diet–see the original Banting diet, see “Letter on Corpulence” in a digital edition. Originally published in 1869. Likely prior incidents of T2D–if existed–ended with death. Insulin’s discovery was a lifesaver for T1D rather than T2D.
I hope this answers your great questions,
Angela
Great comments, Dr. Stanton.
The reply that Glyn Williams received from the ADA is laughable. Moreover, it’s wrong — which makes their response tantamount to malpractice.
On a lighter note, I recently had to go to the ER for an issue and had to endure a lengthy intake with many questions that seemed unrelated. When I was asked about my religion, I responded “I’m Pescatarian.” The young girl typing the responses into her computer responded “I never heard of that religion,” as she scrolled down the list looking for a match. I told her “It’s not very popular.”
Although I can’t recall for sure, I believe I stole that from George Carlin. If it wasn’t Carlin, then it sounds like something he would have said.
Lol Hugo, at least they care to ask so you don’t get served chicken breast for your meals, should you end up in the hospital for some reason. 😉 Can’t blame her for being honest. 😉
I hope you are well and didn’t end up staying in the hospital.
Angela
Very interesting case study. Thank you!
When I was starting to read, Dr. Kraft s book: Diabetes Epidemic & You came in my mind – you have used it already…
FBG (Fasting Blood Glucose) should being measured always together with insulin, in my opinion.
Dr. Robert Lustig (Sugar, the bitter truth) & Fructose 2.0 on YouTube was talking about another important LDL fraction:
Small Dense LDL. It is small enough to cause arteriosclerosis. The big and light fractions of LDL are not dangerous, but small dense LDL is.
I wonder, why cardiologists are still not using W/kg body-weight at 1.5 mMol lactate (OXPHOS) , (equivalent to eco-mode in your car), but try to prove that nothing is wrong by measuring ECG at lactate 7 , or maximal risk blood-pressure, hypoxia , or pseudohypoxia/Thiamine deficiency/Other co-factors deficiency) (red zone in rotations per minute in your car)
By the way, Aecg.ch are doing better ECG s. TT Schlegel at Karolinska Institute YouTube
Above 2 Watts/ kg bodyweight at lactate 1.5 is the lowest acceptable in my opinion, and it should being differentiated further between TOFI (tight outside , fat inside the organs) , and FOTI (fat outside, tight inside the organs)
Riboflavin deficiency / functional deficiency, can lead to migraines too, I did read in some study’s.
Or am I wrong?
Thank you!
Benjamin Kramer
Thanks for your comment Benjamin. Indeed, my 5-hour postprandial is based on Dr. Kraft’s Diabetes in Situ test, which is a 5-hour blood glucose and insulin test based on an oral glucose solution consumed. I don’t use oral glucose in my test because drinking 75 gr (I think he may have used 100 gr) glucose is major unhealthy, so why do it. I completely agree with you that fasting blood glucose and fasting insulin should be measured together but most doctors cannot ask for insulin. They have to follow the protocol of the institution, which normally doesn’t include preventive tests! Checking a fasting insulin would be a preventive test.
Yes, I am familiar with Dr. Lusting and his points–I think it actually originates from Dr. Malcolm Kendrick’s book “The Great Cholesterol Con: The Truth About What Really Causes Heart Disease and How to Avoid It“, which is a great book and I recommend you read it. There is a test called NMR (Nuclear Magnetic Resonance), which measures the different cholesterol densities–it is the only technique patients have access to inexpensively. It is not usually covered by insurance (again, it is preventive), so people have to pay out of pocket at places like where I order mine: ReqquestATest but it’s available in other organizations as well.
But even this way, the meaning of the results is dependent on understanding metabolic health. So one can order the NMR with lipoprotein markers for insulin resistance. This is a bit more expensive, but it also provides an LP-IR score, and also some additional markers, like HDL size as well, which are very important.
I think the reason why cardiologists aren’t using the W/kg body-weight at 1.5 mMol lactate (OXPHOS) is primarily because they aren’t familiar with it–it is really used for sport evaluation and not for general medicine–and also because even if they are familiar with it and may even have it available to them, the results may be ambiguous, given the population and the type of people who looked at by a cardiologist. There are also limitations that are beyond the scope of full understanding. For example, you can get a great understanding of this analysis of an endurance athlete but not that of a weightlifter, yet they both may be very healthy, but the weightlifter may have such tight and large volume of muscles even over the chest that getting enough oxygen for this wouldn’t be possible. VO2 max is a great way also, but again, it has some limitations. For example, I have way better VO2 max than average for my age but I would probably flunk the bicycle test because I don’t have the right muscles in my legs to carry me through!
And lastly, riboflavin deficiency: I have not seen deficiency in any of my migraineurs so far, including me. With this said and done, all of my migraineurs are recommended to supplement riboflavin, TTFD type B1, and magnesium, without testing if they need it or not. For all other supplements we test and see.
Best wishes,
Angela