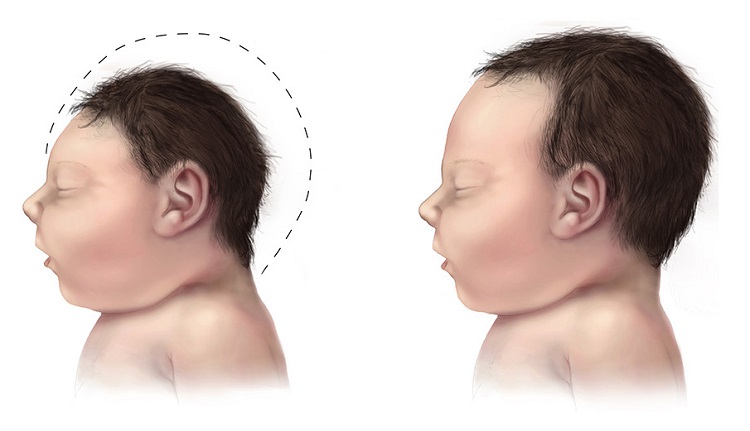
A wise midwife recently told me that in 1960’s the B vitamins were part and parcel of a healthy pregnancy, not just folate (vitamin B9), that we stress now, but the entire complex of B vitamins, including: thiamine (vitamin B1), riboflavin (vitamin B2), niacin (vitamin B3), pantothenic acid (vitamin B5), pyridoxine (vitamin B6), biotin (B7), folate (B9) and the cobalamins (vitamin B12). Thiamine (also referred to as thiamin) was viewed as critical for maternal and fetal health and used within the midwifery community to ensure not only a healthy pregnancy, but a healthy postpartum. In many non-industrialized regions, thiamine is still supplemented for maternal and fetal health and maternal thiamine deficiencies are still recognized as critical impediments to health. Not so in the Western, industrialized world. Here, most resources and education seem set on prenatal folate; so much that it is difficult to escape folic acid supplementation in everyday foods. Despite heavy fortification and regular use of prenatal vitamins, we see increasing evidence of nutrient deficiencies in pregnant mamas and most especially, in their children. Some of these deficiencies are visibly obvious, as least to those who look, such as the increased incidence of neural tube defects in children of women who are low in vitamin B12, but sufficient, even abundant in folate or B9. While other deficits are not so obvious, at least not immediately.
Maternal vitamin B status is important to the pregnancy at hand but also for the child’s long term health, as many of the B vitamins are capable of activating or deactivating gene programs in the children. Maternal vitamin B deficiencies can induce long-term epigenetic changes in the children, and likely, grandchildren. Maternal (and probably paternal too) vitamin B deficiencies silence genes in their off-spring that significantly increase the risk of insulin resistance, high blood pressure and a host of metabolic disorders through adulthood. Nutrition, in addition to its vital role as a source of energy for our cells, is the guidepost for DNA activation and inactivation. The balance of nutrients tell our cells how to function or not function, as the case may be. This information is carried from parents to offspring, across generations. It is this genetic control derived from lifestyle and nutrients that forms the basis of health for our children, and so it becomes something as parents we must pay attention to.
The B Vitamins are Important for Mom’s Health
For the moms, latent deficiencies in core nutrients will become unmasked with the increasing energy demands of pregnancy as many nutrients are shuttled preferentially toward placental and fetal needs, depleting maternal stores. Following delivery, the demands of lactation will further deplete maternal nutrient status and depending upon the vitamin in question, adversely affect her health and/or her child’s health. Reports link maternal thiamine deficiency to hyperemesis gravidarum – severe vomiting across the pregnancy, in some instances leading to a full blown Wernicke’s Encephalopathy. Maternal vitamin B12 deficiency is linked to an increased risk of developing preeclampsia, intra-uterine growth retardation, preterm labor, but also, low vitamin B12 puts mom at risk for developing a myriad of neurocognitive, neuromuscular and psychiatric symptoms associated with B12 deficiencies both during pregnancy and postpartum.
How Prevalent is Maternal Vitamin B Deficiency?
Since there are few reference ranges for vitamin status during pregnancy, with most ranges based upon non-pregnant women, and since much of the research in nutrition is conducted in non-industrialized, poorer countries, it is difficult to assess how many outwardly healthy, western women carry nutritional deficiencies into pregnancy and postpartum. A 2002 study reported the vitamin profile in 563 pregnant New Jersey women at different points across the pregnancy. They found a trend towards too much folate, riboflavin, biotin and pantothenate (vitamin B5) and too little niacin, thiamin, vitamins A, B6, B12, suggesting that prenatal vitamins neither appropriately nor sufficiently address maternal nutrient demands.
A study of healthy pregnant women in Spain found that 32-68% of the women tested were deficient in thiamine, riboflavin or pyridoxine. Interestingly, the severity of deficiency correlated with oral contraceptive use, specifically with the length of oral contraceptive washout period prior to becoming pregnant. That is, when the woman became pregnant shortly after stopping oral contraceptives, she was more likely to exhibit a vitamin deficiency than if she had to waited to become pregnant and allowed her body to readjust to the non-oral contraceptive state. Additionally, the researchers found that if the woman was deficient in one of these nutrients, she was more likely to be deficient in each of them. Although not measured in this study, we know from other studies that many medications, including oral contraceptives, metformin and statins, decrease vitamin B12 significantly.
These reports, combined with the current trends in obesity, type 2 diabetes and the inherent nutritional shortcomings in the Western diet, suggest that it is likely that nutritional deficits and even nutritional imbalances are more common than are recognized.
Maternal Vitamin B Status Before Pregnancy Affects Health of the Male Offspring
A study carried out in sheep found clear evidence linking maternal vitamin B9 and B12 status pre-conception to the health the male offspring later in life. This particular study compared the offspring from sheep fed a nutritionally normal diet to those fed a slightly deficient diet, but one that was still within accepted nutritional parameters, from eight weeks before conception, throughout the pregnancy and six days postpartum. While the pregnancy proceeded normally in both groups and both male and female offspring appeared normal and healthy at birth, continued monitoring across the lifespan of the sheep, showed remarkable changes in the health of the adult males conceived on the nutritionally deficient diets. These males were heavier, had significantly disrupted immune function, impaired glucose metabolism and increased blood pressure, than the females and in comparison to the offspring whose moms had more nutritionally sound diets. This slight change, towards the lower end of what is considered a nutritionally normal diet, had significant influence on long term health in the male offspring. This study also identified clear epigenetic markers in the offspring conceived with dietary deficiency.
Maternal Vitamin B Status, Breast Milk and Infant Health
Maternal vitamin demands do not end postpartum. Lactation increases the demand for maternal nutrients. Deficits in maternal vitamin status impacts infant health and development as well as maternal health and recovery. It should be clear that maternal vitamin deficiencies negatively affect maternal health. Even so, there has been some contention regarding the relationship between maternal vitamin status, fetal development, the quality of breast milk and subsequent infant health and development.
A review of studies assessing vitamin status in breast milk found widespread deficiency, with levels below what is considered adequate intake for proper infant development in most of the samples. The B vitamins (thiamine, riboflavin, B6, B12 and choline) were particularly inadequate.
What was particularly interesting about this study is that researchers found that nutrient deficiencies affect maternal health more so than infant health. Nutrients can be categorized into two groups, those that respond favorably to maternal supplementation with higher milk concentrations (Group 1) and those that do not (Group 2). Group 1 nutrients included thiamine, riboflavin, B6, B12, choline, retinol, vitamin A, vitamin D, selenium and iodine. These nutrietns are secreted into breast milk and depleted rapidly in breast milk when maternal nutrient status is low. Deficiencies in these nutrients can be supplemented and passed on through the breast milk. In this way, maternal nutrient status directly affects the quality of the milk. Group 2 nutrients (folate, calcium, iron, copper and zinc), on the other hand, do not respond as well to supplementation. Breast milk concentrations of these nutrients remain relatively unchanged by maternal status, even when maternal status is declining. Supplementation with Group 2 nutrients affects maternal health more so than infant health.
Take Away
Fetal and infant health and development can be severely impaired by maternal nutrient deficiencies during pregnancy and during breastfeeding. The period across which maternal nutrient status affects the health of her offspring should be extended to well before conception. The B vitamins are especially important to proper development and long term health and appear to regulate genetic expression via epigenetic mechanisms. Recognizing and treating the potential nutritional deficiencies in modern, western diets, may go a long way towards reducing maternal illness while improving fetal, infant, child and adult health for generations. A growing body of evidence, and indeed, common sense suggest that while vitamin B9 or folate is critically important to maternal and fetal health, deficiencies in the remaining B vitamins and other nutrients may be equally important.












What would treatment protocol for a breastfeeding mother with suspected thiamine deficiency look like? I know thiamine, magnesium and a good multi but would dosing be delicate with balancing the nutritional needs of the mother without having excess in the breast milk?
and the anti gluten movement has removed many of the fortified vitamins out of the daily diet and planning is required to replace that