In September 2015, I published an article called Topamax: The Drug with 9 Lives about the myriad of side effects associated with Topamax. Since then, the article has received thousands of reads and over 180 comments. Given the traffic, I thought an update was in order. Had there been any new indications for which this drug was prescribed? Were there any new side effects recognized or any more research on the drug in general? The answer to each of these questions is yes. Since the last publication, the drug has become even more wildly prescribed with additional indications (10 thru 16 are new). Additional side effects are being reported and the research on mechanisms is growing. Below, I have updated the original article to include the new information.
Is Topamax a Wonder Drug?
Over the past week alone, I have talked to several people about their doctor visits. Each one of them had a different illness and each one of them was prescribed the drug Topamax. I cannot help but wondering, how it is possible that one medication can treat so many disparate illnesses. I suspect it cannot and the overreach is driven more by marketing than medicine. This led me to do some digging into Topamax.
What I found is not good. Topamax is prescribed for a broad scope of illnesses for which there is likely little evidence of its efficacy. Take a look at the list below.
Updated list of conditions for which Topamax is prescribed:
- Obesity1
- Seizures1
- Migraine1,2
- Impulsivity3
- Diabetes with nerve damage4
- Bipolar disorder5
- Depression6
- Alcohol addiction7
- Fibromyalgia8
- Periventricular leukomalacia9
- PTSD10
- Essential tremor11
- Bulimia nervosa12
- OCD13
- Idiopathic intracranial hypertension14
- Cluster headaches15
As you can see, there are very few commonalities in the conditions Topamax is prescribed for; some have no connection at all. Does Topamax really treat so many disparate conditions that doctors prescribe it for everything? Topamax is prescribed for many of the above conditions off-label, without sufficient information about the drug effects and without the real informed consent of the patient. I think, off-label prescribing has gone too far.
What is Topamax?
Topamax is one of the most dangerous drugs in the prescription market today. Not only is it a diet pill made from sugar derivatives (actually a sugar substitute), but it uses two dangerous methods (blocking both voltage dependent calcium and voltage dependent sodium channels at once) to achieve what several classes of drugs normally do separately; and thus, with one medicine it affects and damages two circuits that are critical for brain function.
Topamax (an anticonvulsant under the generic name Topiramate and in time release Trokendi XR) is important to discuss because it was initially formulated as a diet pill. Yet over 50% of the new members who join my migraine group arrive with Topamax on their prescription list. I have yet to find a single person on this drug who is not seriously considering dropping it due to its adverse effects, not to mention that it does not appear to work as a pain killer or migraine preventing drug. From what I see in several fibromyalgia groups, it also doesn’t work for that.
Topamax is difficult to quit. The most difficult problem is that doctors are under the false impression that a drug that blocks the voltage dependent calcium and sodium channels can just be easily stopped by a few days of reduction. However, since the voltage dependent calcium channel is a high voltage channel, for some people the discontinuation may end in seizures.
Evidence is also accumulating that Topamax can cause brain damage4. Personally, I have heard of many cases where it has done just that.
Topamax is a sugar substitute that failed as a diet pill but is somehow permitted by the FDA to be used for epileptic seizures. It also received approval for use against migraines. The reasons for such a turn of events is unclear; how can a drug that fails approval for a diet pill suddenly be a perfect match for seizures and migraines? Don’t we all wish for sugar pill to be a pain killer? Unfortunately, sugar or sugar substitutes have different serious adverse effects as Topamax (they cause metabolic disorders).
Adverse Effects of Topamax
If we look at the list of adverse effects associated with this drug (as provided by Wikipedia – Topamax), it is clear that Topamax is not very safe. Indeed, the list is very long.
Dizziness, Weight loss, Paraesthesia (pins and needles), Somnolence, Nausea, Diarrhea, Fatigue, Nasopharyngitis – common cold, Depression, Weight gain, Anaemia, Disturbance in attention, Memory impairment, Amnesia, Cognitive disorder, Mental impairment, Psychomotor skills impaired, Convulsion, Coordination abnormal, Tremor, Lethargy, Hypoaesthesia, Nystagmus, Dysgeusia, Balance disorder, Dysarthria, Intention tremor, Sedation, Vision blurred, Diplopia, Visual disturbance, Vertigo, Tinnitus, Ear pain, Dyspnoea, Epistaxis, Nasal congestion, Rhinorrhoea, Vomiting, Constipation, Abdominal pain, Dyspepsia, Dry mouth, Stomach discomfort, Paraesthesia oral, Gastritis, Abdominal discomfort, Nephrolithiasis, Pollakisuria, Dysuria, Alopecia (hair loss), Rash, Pruritus, Arthralgia, Muscle spasms, Myalgia, Muscle twitching, Muscular weakness, Musculoskeletal chest pain, Anorexia, Decreased appetite, Pyrexia, Asthenia, Irritability, Gait disturbance, Feeling abnormal, Malaise, Hypersensitivity, Bradyphrenia, Insomnia, Expressive language disorder, Anxiety, Confusional state, Disorientation, Aggression, Mood altered, Agitation, Mood swings, Anger, Abnormal behavior, Crystal urine present, Tandem gait test abnormal, White blood cell count decreased, Bradycardia, Sinus bradycardia, Palpitations, Leucopenia, Thrombocytopenia, Lymphadenopathy, Eosinophilia, Depressed level of consciousness, Grand mal convulsion, Visual field defect, Complex partial seizures, Speech disorder, Psychomotor hyperactivity, Syncope, sensory disturbance, Drooling, Hypersomnia, Aphasia, Repetitive speech (stuttering), Hypokinesia, Dyskinesia, Dizziness postural, Poor quality sleep, Burning sensation, Sensory loss, Parosmia, Cerebellar syndrome, Dysaesthesia, Hypogeusia, Stupor, Clumsiness, Aura, Ageusia, Dysgraphia, Dysphasia, Neuropathy peripheral, Presyncope, Dystonia, Formication (the sensation of insects crawling under the skin), Visual acuity reduced, Scotoma, Myopia, Abnormal sensation in eye, Dry eye, Photophobia, Blepharospasm, Lacrimation increased, Photopsia, Mydriasis, Presbyopia, Deafness, Deafness unilateral, Deafness neurosensory, Ear discomfort, Hearing impaired, Dyspnoea exertional, Paranasal sinus hypersecretion, Dysphonia, Pancreatitis, Flatulence, Gastrooesophageal reflux disease, Hypoaesthesia oral gingival bleeding, Abdominal distension, Epigastric discomfort, Abdominal tenderness, Salivary hypersecretion, Oral pain, Breath odour, Glossodynia, Calculus urinary, Urinary incontinence, Haematuria (blood in urine), Incontinence, Micturition urgency, Renal colic, Renal pain, Anhidrosis, Hypoaesthesia facial, Urticaria, Erythema, Pruritus generalized, Rash macular, Skin discolouration, Allergic dermatitis, Swelling face, Joint swelling, Musculoskeletal stiffness, Flank pain, Muscle fatigue, Metabolic acidosis, Hypokalaemia, Increased appetite, Polydipsia, Hypotension, Orthostatic hypotension flushing, Hot flush, Hyperthermia, Thirst, Influenza like illness, Sluggishness, Peripheral coldness, Feeling drunk, Feeling jittery, Learning disability, Erectile dysfunction, Sexual dysfunction, Suicidal ideation, Suicide attempt, Hallucination, Psychotic disorder, Apathy, Lack of spontaneous speech, Sleep disorder, Affect lability, Libido decreased, Restlessness, Crying, Dysphemia, Euphoric mood, Paranoia, Perseveration, Panic attack, Tearfulness, Reading disorder, Initial insomnia, Flat affect, Thinking abnormal, Loss of libido, Listless, Middle insomnia, Distractibility, Early morning awakening, Panic reaction, Elevated mood, Blood bicarbonate decreased, Neutropaenia, Apraxia, Circadian rhythm sleep disorder, Hyperaesthesia, Hyposmia, Anosmia, Essential tremor, Akinesia, Unresponsive to stimuli, Blindness unilateral, Blindness transient, Glaucoma, Accommodation disorder, Altered visual depth perception, Scintillating scotoma, Eyelid edema, Night blindness, Amblyopia, Calculus ureteric, Renal tubular acidosis, Stevens-Johnson syndrome, Erythema multiforme, Skin odour abnormal, Periorbital oedema, Urticaria localized, Limb discomfort, Acidosis hyperchloraemic, Raynaud’s phenomenon, Face edema, Calcinosis, Mania, Anorgasmia, Panic disorder, Disturbance in sexual arousal, Feeling of despair, Orgasm abnormal, Hypomania, Orgasmic sensation decreased, hyper pigmentation.
The FDA Black Box on Topamax
According to the FDA and their listed label update in 2014, Topomax includes a black-box warning that has the following known adverse effects:
- Acute myopia and secondary angle closure glaucoma: Untreated elevated intraocular pressure can lead to permanent visual loss. The primary treatment to reverse symptoms is discontinuation of TOPAMAX as rapidly as possible (5.1)
- Visual field defects: These have been reported independent of elevated intraocular pressure. Consider discontinuation of TOPAMAX (5.2)[i]
- Oligohidrosis and hyperthermia: Monitor decreased sweating and increased body temperature, especially in pediatric patients (5.3)
- Metabolic acidosis: Baseline and periodic measurement of serum bicarbonate is recommended. Consider dose reduction or discontinuation of TOPAMAX if clinically appropriate (5.4)
- Suicidal behavior and ideation: Antiepileptic drugs increase the risk of suicidal behavior or ideation (5.5)
- Cognitive/neuropsychiatric: TOPAMAX may cause cognitive dysfunction. Patients should use caution when operating machinery including automobiles. Depression and mood problems may occur in epilepsy and migraine populations (5.6)
- Fetal Toxicity: TOPAMAX use during pregnancy can cause cleft lip and/or palate (5.7)
- Withdrawal of AEDs: Withdrawal of TOPAMAX should be done gradually (5.8)
- Hyperammonemia and encephalopathy associated with or without concomitant valproic acid use: Patients with inborn errors of metabolism or reduced mitochondrial activity may have an increased risk of hyperammonemia. Measure ammonia if encephalopathic symptoms occur (5.10)
- Kidney stones: Use with other carbonic anhydrase inhibitors, other drugs causing metabolic acidosis, or in patients on a ketogenic diet should be avoided (5.11)
- Hypothermia has been reported with and without hyperammonemia during topiramate treatment with concomitant valproic acid use (5.12) (FDA Topamax Label)
- Suicidal Behavior and Ideation (FDA warnings update)
According to the label, Topamax is only indicated for seizures as a secondary medication in support of a primary kind and for migraines and nothing else (not even for weight loss). Yet, I see people being prescribed this drug for all types of off-label use that are unrelated to either seizures or migraines. The migraine group I run on Facebook had over 4000 migraineurs pass through and end up without migraines and, of course, without Topamax or other migraine medications in the past over three years.
Because I have found that Topamax is the #1 prescribed medicine to migraineurs when they join the group in despair and hopelessness, I have decided to designate Topamax also as the #1 medicine discussed on the series titled drugs of shame that is a chapter in my upcoming book—expected date is August 2017. This is apt because it affects (and often damages) the neurotransmitters (hormones of the brain) and thereby puts the whole hormonal structure of the body in chaos. As far as I can tell, the damage is often permanent.
The Problem: Brain Slowing
Topamax may cause brain function slowing. Why? Topamax is a voltage dependent calcium channel blocker (also called voltage-gated calcium channel blocker), which is a key channel for neuronal communication via neurotransmitter release. Topamax is systemic, meaning it doesn’t just act on a particular type of neurons but all neurons; it cannot differentiate between voltage dependent calcium channels of the many cells. This means that neurons that are responsible to organize how the heart beats, how the lungs function, how you blink, and how you digest your food are all affected by Topamax in a negative way: the neurons cannot release neurotransmitters and so the communication between hormones of the brain and the hormones of the body are broken. Many of the side effects of Topamax are so strong that a lot of migraineurs who start Topamax stop within weeks (some on day 3) of taking this medication. The drawing below shows how voltage dependent calcium channels work and what happens when they cannot work because they are blocked.
Voltage Dependent Calcium Channel Blockers
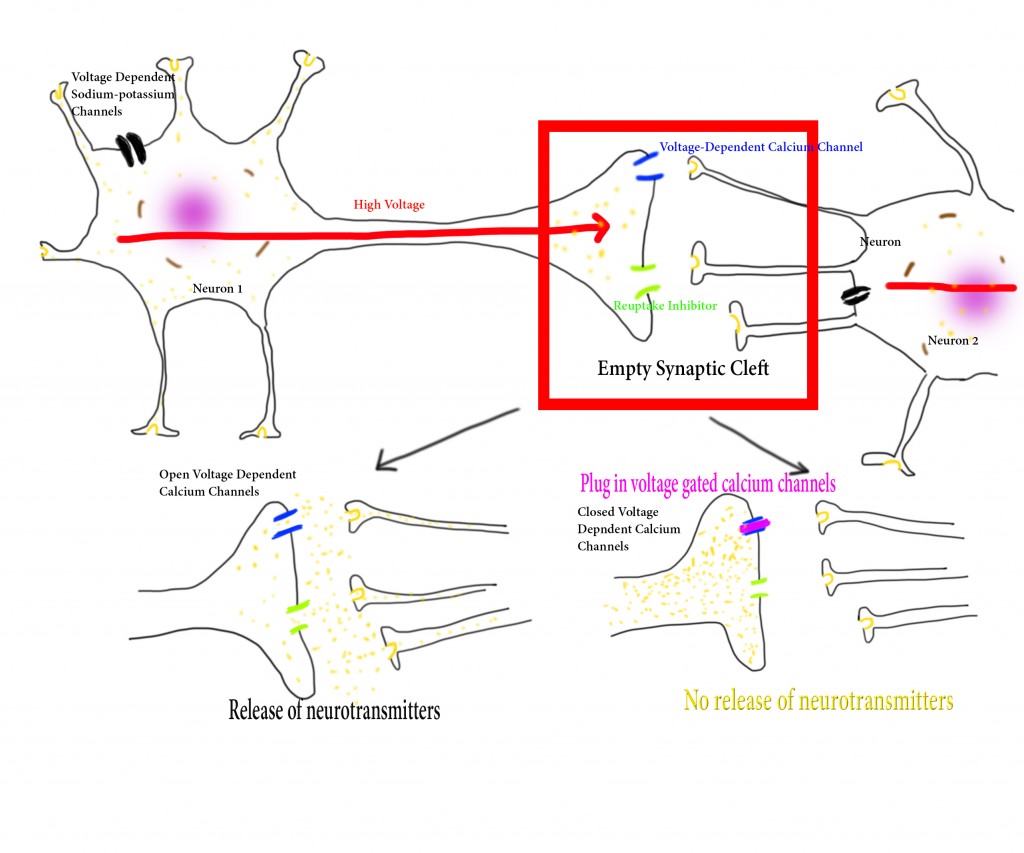
Figure 1. How Voltage Dependent Calcium Channels Work
In figure 1, you see a simplified neuron on the left and the axons of another neuron on the right. In the synaptic cleft, normally neurotransmitters work like a domino effect. One neuron receives a signal from a sensory organ that stimulates the release of neurotransmitters that are specific to the type of stimulus. The neurotransmitters then get to be picked up by the neuron connected to the releasing neuron and pass the signal along. When the signal volume, intensity, frequency reaches a particular threshold, the brain sends a command to the body: it’s hot, cool the body, for example.
Blocking the voltage dependent calcium channels from firing means that no neurotransmitters can be released and thus no message is passed on to the necessary number of neurons to reach the threshold. One of the most often noted adverse effect is the inability to stay on the sun since the body is not able to control its temperature in the heat. Since Topamax is systemic, every function of the body is hampered to some degree.
Neurons have five types of voltage dependent calcium channels based on voltage requirements:
- L-type that directs skeletal muscles, cardiac related muscle cells, endocrine cells, adrenal, etc., associated with contraction, hormone release and synaptic integration (neurons working together)
- P/Q-type that activate neurons and neurotransmitter and hormone release
- N-type works at the nerve terminals similarly to P/Q for neurotransmitter and hormone release
- T-type think of it as the pacemaker of the brain for firing with a particular frequency
- R-type that works with cerebral cells and some neurons
For each of these, the current required is different so fine-tuning is necessary. The calcium channel must go through all stages of voltage levels to be able to perform all five types of actions, as the body requires all of them. Note that when the voltage gated calcium channels are blocked, none of these 5 types of actions can properly function. The body will utilize its reserves to maintain vital functions. People who take Topamax can still breathe and their hearts beat – but they have serious issues with body cooling, which is a pretty basic, built-in automatic motor function. Most interestingly Topamax prevents the very functions a migraine brain needs for relief the most because it blocks those channels that would instruct the brain to cool the body.
In addition, Topamax blocks both voltage dependent sodium-potassium channels. I have written extensively on voltage dependent sodium-potassium channels in previous articles so here I just present a short summary. Voltage dependent (or gated) sodium-potassium channels have the critical function of sodium and potassium exchange in the cell to ensure that proper voltage differential is generated between the inside and the outside of the cell membrane to generate action and resting potentials. Proper voltage is required so that the channels can open and close their gates, nutrients can enter and waste products can leave. Neurons cannot manufacture neurotransmitters without the availability of various minerals, many of which must be able to enter the neuron via voltage dependent channels. When these channels are not able to generate the proper action or resting potential, nothing moves in or out of the neuron. By blocking voltage dependent channels, the high voltage needed to release the neurotransmitters is reduced as well.
Topamax robs the brain from its most important vital roles: making neurotransmitters that transmit messages and regulate brain and important autonomic body functions such as, cooling the body when it is too hot, maintaining and appropriate heartbeat, or simply making a decision. I think, Topamax is one of the more dangerous drugs on the market. From what I can gather from the research and my work with migraineurs, Topamax does not appear to work for pain. It only slows brain function. I would not be surprised to see researchers soon showing a connection between Topamax use and dementia. Until then, proceed with caution.
Share your Story
If you have a Topamax story, please consider sharing it on Hormones Matter.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
Sources:
- Sommer BR, Mitchell EL, Wroolie TE. Topiramate: Effects on cognition in patients with epilepsy, migraine headache and obesity. Therapeutic Advances in Neurological Disorders. 2013;6(4):211-227.
- Nelles G, Schmitt L, Humbert T, et al. Prevention of episodic migraines with topiramate: results from a non-interventional study in a general practice setting. The Journal of Headache and Pain. 2010;11(1):33-44.
- Navarrete F, Pérez-Ortiz JM, Manzanares J. Pregabalin- and topiramate-mediated regulation of cognitive and motor impulsivity in DBA/2 mice. British Journal of Pharmacology. 2012;167(1):183-195.
- Garvey WT. Phentermine and topiramate extended-release: a new treatment for obesity and its role in a complications-centric approach to obesity medical management. Expert Opinion on Drug Safety. 2013;12(5):741-756.
- Geddes JR, Miklowitz DJ. Treatment of bipolar disorder. Lancet. 2013;381(9878):10.1016/S0140-6736(1013)60857-60850.
- Campayo JG, Sobradiel N, Alda M, et al. Effectiveness of topiramate for tobacco dependence in patients with depression; a randomised, controlled trial. BMC Family Practice. 2008;9:28-28.
- Paparrigopoulos T, Tzavellas E, Karaiskos D, Kourlaba G, Liappas I. Treatment of alcohol dependence with low-dose topiramate: an open-label controlled study. BMC Psychiatry. 2011;11:41-41.
- Pereira AG, Michael J.; Gross, Robert A.; Posner, Kelly; Dworkin, Robert H. Suicidality associated with anti-epileptic drugs: implications for the treatment of neuropathic pain and fibromyalgia. Pain. 2013;154(3):345-349.
- Follett PL, Deng W, Dai W, et al. Glutamate Receptor-Mediated Oligodendrocyte Toxicity in Periventricular Leukomalacia: A Protective Role for Topiramate. The Journal of Neuroscience. 2004;24(18):4412-4420.
- Andrus MR, Gilbert E. Treatment of Civilian and Combat-Related Posttraumatic Stress Disorder with Topiramate. Annals of Pharmacotherapy. 2010;44(11):1810-1816.
- Chang K-H, Wang S-H, Chi C-C. Efficacy and Safety of Topiramate for Essential Tremor: A Meta-Analysis of Randomized Controlled Trials. Medicine. 2015;94(43):e1809.
- Hoopes SPR, Frederick W.;Hedges, Dawsom W.;Rosenthal, Norman R.;Kamin, Marc;Karim, Rezaul;Capece, Julie A.;Karvois, Debra;. Treatment of Bulimia Nervosa With Topiramate in a Randomized, Double-Blind, Placebo-Controlled Trial, Part 1: Improvement in Binge and Purge Measures. The Journal of Clinical Psychiatry. 2003;64(11):6.
- Van Ameringen M, Patterson B. Topiramate augmentation in a patient with obsessive–compulsive disorder. Journal of Psychiatry & Neuroscience : JPN. 2015;40(5):E31-E32.
- Çelebisoy N, Gökçay F, Şirin H, Akyürekli Ö. Treatment of idiopathic intracranial hypertension: topiramate vs acetazolamide, an open-label study. Acta Neurologica Scandinavica. 2007;116(5):322-327.
- Láinez MJA, Pascual J, Pascual AM, Santonja JM, Ponz A, Salvador A. Topiramate in the Prophylactic Treatment of Cluster Headache. Headache: The Journal of Head and Face Pain. 2003;43(7):784-789.
[i] This particular adverse effect was listed on the package at the first publishing time but since has been removed. It can still be located in various sites
Image source: Pixabay.
















I was prescribed to topiramate 25mg 8 days ago for migraine. I have been taking it just from 8 days. Im realizing that my periods are delayed – its 32nd day of my cycle now. Im 34 years old, mother of 2, i have always been on regular cycle my whole life. Its never been late more than one day ever! Im concerned.im not used to having irregular periods and its giving me anxiety. Do you think its the side effect of topiramate? I had been pmsing from 5 days already.
Dear Alisa,
Topiramate is a serious medication that changes how your brain works. I don’t know what condition you were prescribed Topiramate for. If it was prescribed for migraine, you can do way better by joining my Facebook migraine group here and learning how to become migraine and medicine free. We can help you there completely free.
Best wishes to you,
Angela
I have IIH. I had an allergic reaction to Diamox and can now only take Topamax. I am at 300 mg now because just as I was almost in remission, I learned that heat was a trigger for me- the pappiloedema is back at a grade 3 & 4. What do we do when we have no choice but to take Topamax? The alternative is risk blindness for me.
Dear Angel,
I am sorry that you have IIH (pseudotumor cerebri). While the cause of IIH is unknown, one way to prevent it from harming you and your eyes is to have a surgery with a shunt built into your brain to release the cerebrospinal fluid 24/7 ongoing. IIH is associated with obesity and thus metabolic disease. This would suggest that working on your metabolic health may be helpful. This is just an association, not a causation–at least as far as I know. If you are heavier in weight than your ideal and/or have metabolic disease, you should consider a change in lifestyle and incorporate a low carbohydrate diet. If you are not overweight and have no metabolic disease, consider to have a discussion with your doctor about a shunt.
Best wishes to you,
Angela
I was prescribed 300mg of Topomax as a mood stabilizer, weight loss, pain management and migraines.Within a months time, tinnitus and insomnia hit me like brick in the head! I stayed on it for over year and am currently on a 3 week taper, ordered by my doctor, because of hair loss. He never made the connection to tinnitus or insomnia. The tinnitus seems to be resolving, even before the end of the taper. Sleep maintenance insomnia has been horrible! Have you heard these conditions being related to Topomax? Any thoughts about how long it will take to resolve the insomnia?
Dear Karen,
Insomnia was among the most common side effects of Topamax–even in the original clinical trial. See here under “Monotherapy Epilepsy” for adults.
I am not sure how long it will last, but first you will have to come off of the medication completely and be off for some time for most of the normalcy to return. I am glad that some of the problems are already reducing. That shows hope of full recovery. Please join my Facebook migraine group and we will help you there.
Best wishes,
Angela
Hello Angela,
I too feel I have permanent damage from Topamax, after only being on it for a few weeks about a year ago at a smaller dosage. I believe it may have impaired my language center as I can no longer spell, type, or articulate things like I used to. Furthermore I can’t think as deeply or immerse myself in ideas the same as I could prior to Topamax. You seem convinced that the keto/low-carb protocol can fix these symptoms, but I’m unable to find any evidence here or elsewhere that absolutely supports this position. Could you provide links to a few peer-reviewed studies that provide more info on how keto and intermittent fasting might reverse cognitive impairment from Topamax? Also, what is the precise mechanism by which it would do this? Also, you mention that Topamax damage is primarily because it blocks voltage-gated calcium and sodium channels. But there are many drugs that do this that do not seem to have the same permanent effects. Does Topamax do something different? Does it do something other than permanently block neurotransmitter pathways? I’ve heard it may inhibit AMPA and NMDA receptors.
I tried joining the facebook group, but I’m unable to set up a facebook account for some reason.
Dear Dave,
There are no studies that show specifically how the ketogenic diet helps cognitive damage or impairment from Topamax, but there are hundreds of studies out there on how it helps nearly all brain conditions. There are literally hundreds of peer reviewed academic articles out there on various brain conditions and the ketogenic diet, some even explain the mechanism. Here is one on seizures, here is one for Alzheimer’s disease, and one for multiple sclerosis.
A new book is about to be released: “Ketogenic: The Science of Therapeutic Carbohydrate Restriction in Human Health”. It is a textbook with multiple authors–I am one of them. This book will explain to you all of the methods, why and the how for all neurological disorders and the benefits of carbohydrate reduction.
In terms of why Topamax causes such terrible permanent damage even though other drugs use similar mechanism without such damage: I don’t know the answer to that. Topamax may just be a very badly designed drug. It isn’t supposed to permanently block anything but because it does, that is the trouble and the mechanism that is not working right. In my personal opinion, any drug that aims to “block” or “inhibit” a function essential to neuronal operation is a bad drug to take.
I am sorry that you are unable to set up a Facebook account. I have never heard of such problem. Perhaps you are in a country that is not permitted? I am not sure.
Best wishes to you,
Angela
Thanks for the prompt reply. Having tried keto and low-carb regimens in the past, I find it severely limits my functioning to the point where I simply couldn’t sustain them. Perhaps because I’ve been stuck on SAD so long and the abrupt change is just too much? I’ll plan to progressively go at it this time around, taking it month-by-month until I get to mostly fat & protein with few-to-no carbs lifestyle.
Re: the facebook group, I don’t know what the issue is but when I try to set up an account the platform won’t let me on, telling me that I’m “suspended.” That said, can you attest to the success rate of individuals who’ve responded favorably to your protocol, specifically those who’ve been on Topamax and feel as if the damage is permanent? Have they gained their functioning and language skills back?
Dave,
Switching to keto or carnivore at your speed is ideal. Just know that carbs are addictive. Studies show that carbs release the exact same neurotransmitters as heroin and alcohol, this is why tapering off slowly often backfires.
In terms of the success of the Stanton Migraine Protocol(R), yes. Since every single migraine sufferer who applies my protocol fully recover and is medicine free, even without knowing how many of them were taking Topamax, I can say the Protocol is 100% successful. There is a “Wall of Testimonials” I recommend you read. These posts are either posted there by me with the permission of the author in the group or they posted it themselves on the wall. There are many more testimonials, but I have limited time to post them all. And all migraine sufferers have gained back their functions–again, I don’ know how many of them were taking Topamax, but the recovery is magical.
In my group the migraineurs use the carnivore diet rather than the ketogenic. I found that the carnivore diet works better and faster and is also quite foolproof. The carnivore diet does not contain any plant stuff, only animal products.
Best wishes,
Angela
I was placed on toprimate two years ago at about 200 mg every night and now I am down to 50 mg. I was prescribed it because an MRI done on my brain and spine after being hit by a car while riding by bike showed that I have osteoarthritis of the atlanto-axial joint, mild spinal canal stenosis and bone spurs in my neck. In my back I also have osteoarthritis and bulging discs. Since osteoarthritis is not an autoimmune condition, I was wondering if there is a diet I could follow because I think the toprimate has affected my appetite where I don’t feel very hungery anymore.
Dear Margaret,
Thanks for reaching out. Indeed, osteoarthritis is not considered to be an autoimmune condition and in reality the literature refers to it as “wear and tear” but the trick here is the cartilage that starts to break down, causing the problem. So while it is not believed to be autoimmune, I had worked with many people–including myself–with osteoarthritis that went into remission after starting new nutritional ways. Based on this alone I venture the thought that while not known to be autoimmune, I personally think it is!
It didn’t reverse per se. For example, I had several finger joints that were disformed already and most disappeared but two are still visible. So the degeneration stopped where it was and didn’t get worse in some of my finger joints, but reversed in others and is invisible. And, zero pain, of course.
The nutritional changes I made were–in order of importance and most benefit:
I stopped the following:
1) grains–all grains, not just gluten. I found this to be the most important in reversing not only my osteoarthritis but also asthma, allergies, psoriasis, diabetes (T2)
2) seed/veg oils–all plant-based oils were removed from my diet–including olive and avocado oils and all other plant oils. This was a HUGE change for the better. If today I go to a restaurant and they use some veg oil, it gets that sticky feeling in my mouth for days and I usually end up with gut issues
3) all processed pre-packaged foods are gone from my life. Exceptions are dairy, which I love and eat a lot of cheese, butter, sour cream, ricotta cheese, etc., and I drink milk. These are the only processed foods I eat.
4) vegetables–I eat no vegetables at all. I do eat some fruit-type veggies: tomatoes, peppers, quash, pickles, avocado, and similar. but zero true vegetables except onion and garlic for seasoning
5) all sweeteners are out of my life as well. Maybe a couple of times a year, on some birthdays, I will eat a small scoop of ice cream. That’s all the sugar I eat a year, and I don’t use any zero calorie sweeteners at all.
7) all tropical and high fructose fruits are also all gone
8) my choice was to also go coffee free. Time to time I enjoy a decaf with a lot of cream, but seldom
When I started to implement these, the changes were amazing. All my health conditions went away. I came off of over 10 daily medications.
The foods I eat now: I most eat an animal-based diet with some seasonality–like in the summer I will include some berries but in the winter no. All animals: wild or not, red meat focus, followed by eggs, fish and seafood, poultry. Basically every day at least one serving of red meat–usually beef or bison–and another meal may be chicken or fish or seafood or pork or organs. I eat only twice a day and eat very well, full of nutrition. I am now healthier than I have been when I was 30 (I am 69 now).
In sum: yes, I strongly recommend you try and change your diet and allow you body to heal from the nutrients you eat. Your collagen needs to strengthen up and that needs protein–not collagen powder but full protein.
Good luck to you!
Best wishes,
Angela
Thank you so much for this article! Topomax & Topiramate are dangerous drugs. My mom was prescribed Topiramate for weight loss 9 years ago in early 60s. Around her 70th birthday, she had sciatica & a pain doctor upped her dosage from 75 to 100 mgs to 250 for pain. At one point, a primary care doctor told her she could adjust the dosage as she saw fit, which was not good advice. Back in September, my mom decreased her dosage by 100 mgs & experienced some feelings of depression. Then, in December, she stopped taking it completely w/o proper monitoring by a physician & she developed a full blown anxiety disorder. For several weeks, she could not function & it was terrifying. It was a total personality change. She had to see a psychiatrist & it took about 4 months to get her “back.” I could go into more detail, but I wanted to share our experience here b/c none of the docs we talked to really believed that Topiramate was the cause of her depression & 4 month long total personality change. She was never depressed in her life! I put this here just in case another person out there is dealing with a sudden personality change and is on this drug and/or recently changed dosages, please be aware that the drug could be the culprit. Docs who prescribe this all the time don’t really understand the potential side effects. Docs kept telling us “We never see this with Topiramate.” But they simply refused to admit it! I noticed her getting a little “kooky” in her 60s. Now that is completely weaned off of the drug, she seems back to the way she was in her late 50s. I understand some folks might really need this drug, but for weight loss and/or pain management, what my poor mom went through was not worth it. What an unnecessary nightmare to lose 30 lbs.
Dear Lori,
Thank you for your comment and the story about your mother. I sure hope she is doing better now and that she will see a full recovery from Topamax.
Indeed, it is hard to accept how doctors prescribe these drugs like candy, without true understanding of their adverse effects. I am glad to hear your mom is no longer taking it!
Best wishes for her and thank you for sharing her experience.
Hugs,
Angela
I am a single mom of two boy who both have autism n I recently went thru a break up I do you know what has happen to my brain seems like I can’t get anything done since I have been taking tops ax simple task such as cleaning my house which I did daily before taking care of my kids just the most simple things have become very huge task to the point I don’t know what to do people say I look like I’m in a zone will I get my brain back please help
Dear Amber,
Thanks for reaching out. May I ask why you are taking Topamax? Is it for migraine or seizures? I recommend you join my Facebook group where I can help you better.
Hope to see you there,
Angela
I have debilitating migraines 4-6 days a week, to the point of my hair hurting. I have been prescribed countless medications. I am on round 2 of topamax. I stopped taking it last time due to the side effects, however, it is one of only 2 medications that has worked for my migraines and the other medication causes me to experience extreme anxiety and uncontrollable weight gain. While I’m not a neuroscientist, I have to recognize that, as with most things in life, it isn’t for everyone, but some of us actually do need it to function. While I have experienced some pretty crazy side effects, I would not be able to get out of bed without it. That is the reality for me.
Dear Jamie,
The true reality for you is what several thousands of migraineurs–many originally on Topamax–have done. Please join my FB migraine group and/or read my book in order to understand the cause of migraines.
Big pharma and the medical industry, in general, will look for a pain treatment, something that will stop the pain. But ultimately if the cause of the pain can be prevented–which can be–then there is no need for the medications. So far, of the over 10k migraine sufferers I have worked with over the past 6+ years, all have been able to learn to prevent their migraines. It only takes a bit of work to understand the cause. Once you understand it, the prevention is very simple.
Join us and try–it is free and you need not stop your medicine. Just try a lifestyle change to learn why you are getting migraines. 🙂
Angela
I am trying to find out if Topamax taken during pregnancy could cause a child to have brittle or soft bones?
My 4 year old grandson has broken bones since the age of 1. His brother, although he was born with a club hand, mother used Epilum in the first six weeks of pregnancy, thereafter Topamax until after her youngest was born 3 years later. I’m concerned about the ease with which my youngest granson breaks bones.
Dear Renee,
I went online to search for this adverse effect and bam, on Topamax website:
from here
So clearly Topamax could have caused the problem. In terms of how to fix it, I am not a medical doctor, so I cannot advise. But you do need to understand a bit about bone formation and that may help you help your grandson. Bone is over 40% protein–and it is important that this protein come from animal products, because plants contain incomplete protein, except for soy, but too much soy is a major goitrogen (destroys the thyroid) and plants have the wrong ratio of various amino acids in the protein. So to build the scaffolding onto which the calcium can deposit, the diet must be rich in proteins. And the next things are fats and calcium. Calcium in the human body needs fat to be absorbed, and so taking just calcium won’t do. Whole milk–and plenty of it–would help anyone grow stronger bones.
Best wishes,
Angela
Dear Angela, I have had hormonal migraines for over 20 years, twice a month for 3-4 days, increasing in severity. I have also been diagnosed with Cervicogenic headache. Now I’m not sure which it is but around the time of my period and ovulation the neck pain begins to flare and within days the migraine follows. I have tried all types of acute medications, which initially worked great but now no longer work and have tried various preventatives also. Six weeks ago my GP prescribed Topamax 25mg. Whilst the medication helped with the migraines I suffered severe neck and lumbar spinal pain and joint pain in my hands and elbows daily for the six weeks of being on the medication. I presented to the emergency department three times. The last was when I’d decided to stop taking the medication as I couldn’t put up with the new ongoing daily pain and would rather go back to migraines with some relief in-between. After I stopped taking the Topamax within two days I was back in hospital, I had experienced one of the worst migraines plus the neck and lumbar pain, vomiting and pins and needles throughout. I have mild mid cervical spondylosis and was wondering if this medication might have caused this to flare up. My GP believes it’s not the case and also one of the hospital doctors. My kidney specialist is with me and agrees I should stop taking it as I have reduced kidney function. It has been nearly three days since I have stopped taking this medication and my neck and back have improved considerably. I have had MRIs, X-Rays and about to go through the whole process of Neurologists, Rheumatologists and Musculoskeletal specialists. I would love to hear what you think and intend to read your book as I’m starting to rethink medications! Thanks, Maria 🙂
Dear Maria,
Thank you for reaching out. 🙂 Indeed, your hunch is correct and quitting Topomax just cold turkey is not the right way to go. I am unsure why your GP didn;t realize that because Topamax is really an anticovulsant medication, meaning it is to prevent seizures, by its very functions, when stopped abruptly, major chaos–even seizures–may follow. I think you are very fortunate that you didn’t end up getting a seizure and “only” got a monster migraine!
Let me briefly explain why you ended up with a monster migraine after you quit the medicine, and then you will also immediately see why you may never want to take it. In the article above I described the process by which it works, but to be very specific:
The only reason your body functions at all is because of the communications among neurons. Neurons communicate in order to pass on instructions in response to stimulus. For example:
A very primitive example but I want to make a point clear: the neurons communicate from one to another via neurotransmitters. To release neurotransmitters for such communication, voltage gated calcium channels must open and let calcium into the neuron in order to kick the neurotransmitters out from one neuron into the synapse, which is where the next neuron picks the neurotransmitters up. Neurotransmitters are the messages! So if there is no neurotransmitter release, there are no messages, and you have no reaction to reach for your sunglasses.
The problem here is that Topamax is a voltage-gated calcium channel blocker! This is very important. So, in essence, Topamax blocks neurotransmitter release by blocking the action of the calcium channels. Therefore, there is a neurotransmitter buildup in the neurons that would like to release these neurotransmitters, but they cannot. This does several things, none of which is desired:
1) The buildup of neurotransmitters damage the neuron
2) In the brain, neuronal communication is the meaning of life. No neuronal communication means the neurons disconnect!
3) Neurons disconnect by trimming their connections–that is: they degenerate
4) Drugs like this are brain degenerative as a result
5) If you stop taking the drug, calcium can enter through the voltage-gated calcium channels and kick way to much neurotransmitters out and/or kick them out too often
6) Such huge voltage release all of a sudden can lead to seizures!
There are many comments already how Topamax is labelled as Dopamax because it makes everyone feel doped and dumb… This is why.
Since you will be reading my book, you will see link to my Facebook migraine group in the book, but here I provide it for simplicity. Please join my group and we will help you learn how to become migraine free without a drop of medications by feeding your brain the right way. 🙂
I am looking forward to seeing you there,
Angela
Wow. Thank you for writing on this. My husband seems to have Cyclic Vomiting Syndrome, and he just started seeing a neurologist for the first time, and had requested a plan to get off of his 75 mg of amitriptyline (which he started in the fall of 2019 at 10 mg and slowly titrated up). Chandler Marrs shared with me that amitriptyline blocks thiamine. My husband is taking 150 mg lipothiamine a day for a week now (was taking allithiamine since beginning of May, but I switched him because lipothiamine is enteric coated and is apparently absorbed better and causes less digestive distress). But the amitriptyline seemed to be causing him faintness, Raynaud’s, diarrhea, etc. He never had Raynaud’s before it. But anyways, neurologist wants to switch him to topiramate. He is also eating carnivore, which is technically a ketogenic diet (I saw your warning about that). I’m going to encourage my husband to wait on the topiramate and see if the lipothiamine and magnesium will cure his cyclic vomiting syndrome. He is also taking l-carnitine, coq10, b2, and b-100 tablet and will continue that as well (those are recommended by Dr. Richard Boles). Topiramate sounds scary. But I understand my husband’s desperation. He doesn’t want to puke. Or feel dizzy. Or have the room spin (right-beating nystagmus). Or get terrible headaches. Or have random swollen joints/tendons.
Dear Sarah,
Thanks for reaching out. Indeed, Topiramate interacts with ketosis and there is an FDA warning on the drug against its use in ketosis. I am not sure what your husband needs the medicine for since the ketogenic diet will cure his cyclical vomiting syndrome and just about everything else he has, which seem all to be autoimmune to me. I would stop the B-100 because it has all Bs in that and we don’t know if he needs those and we also don;t know if he can even absorb the non-methylated form. I am not in support of supplementing most Bs without first checking for blood test. The Bs I fully support taking are B1 (thiamine, which he takes) and B2 (riboflavin). I would not take the other Bs without a blood test, since supplementing the rest may cause trouble if he has enough or cannot methylate–and thus may have too much.
L-carnitine is taken if one cannot metabolize protein and fat well enough. It is not something I would recommend takign long term–particularly not if he starts the ketognic or carnivore diets, both of which have more than plenty carnitine. CoQ10 is fine though may not actually help; but the Ubiquinol form is the most absorbent. I would recommend your husband to join my main migraine group on Facebook for help and guidance.
Best wishes,
Angela
He attempted a traditional ketogenic diet, and was unable to stick with it. Then in April 2018, he began carnivore, and has been able to stick with that. He went from 330 lbs own to 250 lbs, reversed his prediabetes (A1C down from 6.4 to 5.1), and reversed his NAFLD. But his CVS episodes did not stop. Then in September 2019, he got a 2 week long episode (longest ever). He began the b vitamins, coq10, and l-carnitine because CVS is believed to be a mitochondrial disorder. I have been reading Dr. Lonsdale and Chandler Marrs work, it’s possible subclinical beriberi and he need high doses of thiamine (TTFD). Unfortunately, carnivore alone did not cure my husband.
Sarah, it takes quite a bit of time for the body to heal–several years for some. I went keto and hypercarnivore (that’s carnivore with a very small amount of carbs time to time) over 5 years ago and I still discover improvements showing up now after 5 years! It is important to stick with it. However, mitochondrial disorder needs help in addition to the proper diet. I am facing the same. Still, had I started to supplement a multi B vitamin, I would be in trouble, because some of my Bs are high and some low! And that means that it requires individual Bs to be picked for supplementing.
I use Allithiamine for my B1 and currently am takign 350 mg (7 times 50 mg throughout the day. This seems to work for me but it’s a moving target. Upon testing my blood, I discovered I needed to supplement a host of other things, which your husband may also need to supplement. Some things really require a blood test. We really haven’t the clue otherwise, and vitamin/minerals can be harmful if supplemented incorrectly.
Another thing: if he is on the carnivore diet the right way–and for that he should join my group–he can take medications–like Topiramate. But it need modifications to how one conducts the carnivore diet.
Angela
Thank you! It is very difficult to get blood tests right now in Nova Scotia. But once we are able, I will be sure to get him to request a test of the B vitamins. And I just made a request to join your group, “Stanton Ketogenic Protocol for Migraines.” In my husband’s defense, he was basically, “I’ll do/take anything. I must stop puking.” He didn’t and doesn’t want to lose his job and miss more work. So I understand his desperation. He went from April 2018 to September 2019 eating carnivore without taking those supplements, but his episodes did not get better or less frequent. But you’re right, we don’t know whether he is high or low in some of those B’s (though he was on the low side for B12 prior to supplementing; don’t know now). Looking forward to learning more in the group! I hope it’s okay that I join. It’s mainly me that learns all this stuff as he is very busy, and many times doesn’t feel well and up to absorbing any kind of information. Plus he doesn’t really go on Facebook (maybe once every couple of months he’ll pop in for a look at his feed).
Sarah, it is difficult to get anything done now anywhere because of Covid restrictions. Feel free to join the group yourself for him. We have other people just like that: in for their spouse or child. 🙂
Angela
Are there any neurological drugs that don’t have awful side effects? I’m currently taking 200mg of topamax for grand mal seizures (I know they have been reclassified but I can’t keep up). I have tried so many different drugs and they all have terrible side effects. It makes me mad to have to take anything to be honest. My EEG is always normal. My MRI is normal. The neurologist is only interested in the big seizures not the ones that I suspect may also be seizures but I don’t “twitch” so they don’t count. No one can give me any answers so I live my life in a foggy haze. It is extremely frustrating to have doctors tell you “the brain is a mystery -take this drug” and then read on a random blog how dangerous this drug is. I just want my life back.
Dear Terri,
Unfortunately all neurological drugs have awful side effects. Drugs of any kind have awful side effects because we were not meant to supplement our diet with drugs. Have you tried to change your diet to the one that kids with seizures are placed on? It is the ketogenic diet. A very large percent of kids (over 60%) can completely stop their meds for life. It seems the brain merely needs healthy foods… and that excludes most carbs.
Best wishes,
Angela
I am pretty sure the topomax I am prescribed caused me to lactate. I am 49. peri-menopausal. I now am being treated for mastitis as result. Any other women producing breast milk when they shouldn’t be because of tomomax?
Wow Karen! I have not heard that adverse reaction before. Very scary. You may want to talk to the doctor about that and stop taking it–with your doctor’s directions.
Best wishes,
Angela
Hi Karen,
I have the same situation. I’m 42 and it’s been 11 years since I breastfed my last child and I’m still lactating too! I have no idea why, but this is the first time I might have an answer: Topiramate! I’ve had breast milk since taking the drug for migraines. I’m now going though some AWFUL withdrawals since I took my last pill last Friday ?.
Terri, can you help with ideas on how to survive the withdrawals?
I’ve been on Topimax/Topiramate for 11 years. I went down slowly from 75mg to 25mg over a month, and have now stopped altogether.
The symptoms Include experiencing are that I have a permanent scorching headache, occasional migraines, insomnia, brain zaps, dizziness, emotional, and I feel like my heart skips a beat every so often which is rattling to say the least! I’m determined to stick it out though! I’ve heard that Brenedryl can help.
Any advice would be soooooo appreciated.
Thank you ?
Dear Sascha,
Coming off of Topamax without changing your lifestyle–meaning remaining in the same health situation for which your doctor prescribed it the first place–will likely cause trouble and delay your recovery. I think also that your tapering after 11 years may have been too fast. It seems you tapered the “standard” way and that is definitely not sufficient for someone on it for 11 years.
Can you talk to your doctor and go back on 25 mg once a day and then taper slowly from there by cutting the pills? Ask first if the pill can be cut–from what I understand it can be but best to confirm. Please contact your doctor and reduce it slower. Some of the side effects you feel are caused by the nature of the drug. It prevents neuronal communication, and thereby it degenerates the brain. All of a sudden, when the drug stops, firing is on again but the neurons are not connected properly and the communication is off. That is what you feel.
So tapering must be slow enough to allow some brain regeneration.
I wish you the best,
Angela
You didn’t really update the article with any new information at all. I am on Topamax and it does indeed suck. But I need some more.
Colin,
I updated only the FDA information about it and more adverse reactions. Nothing else. Topamax is a nasty medication. What are you taking it for?
Angela
Hi Angela,
I came across your article while researching (again) more info on Topamax and being very fed up. I took it in 2009 for migraines & dizziness. I took it for 6 months or so. I noticed my vision changed (I had lasik eye surgery in 2006 so my vision was great until Topamax). Now my vision keeps getting worse. I also started experiencing brain fog, slow thinking, lack of concentration, etc. It has been 10 years and I’m still dealing with these symptoms and I feel they have gotten worse. The doctors don’t want to listen and claim the Topamax should of been all out of my system & it must be something else (but of course none of them can explain what, can’t give me any answers). I keep telling them I know how I was before Topamax and I’m struggling with these side effects because of this medicine. I don’t care what they say, this medicine is the cause. My life has become an embarrassment for me because I can’t think or function like I used to or like the average person. Others my age (46) are sharp, smart, you name it. This has brought me so much anxiety and heartache. I hate I was ever introduced to it!
Dear TJ,
I am so sorry what you have to go through. <3 I totally agree: your symptoms likely relate to your having had taken Topamax. Few doctors understand–and the fact that most individuals don’t know that they should report the adverse effect to the FDA–doesn’t help. have you reported your adverse effect? You can do it any time. Here is the link where you can report it by one of 3 methods: online form, print out the form and mail in the filled out version, or call via a toll-free number. It is the most important thing to report all adverse events, so that the FDA can make the proper adjustment to label warnings.
Today the label contains eye damage warning as the first symptom and it can be permanent. I know several people who had lost their eye sight in that one eye. At least it seems you still seem to have vision. Though you have brain fog. There is a good chance that can be reversed nutritionally. The cause of such brain fog is likely from the inhibition that Topamax uses. It is a voltage gated calcium channels blocker. These channels are used for neurotransmitter release. In the brain, all communication between cells is via neurotransmitter release and reception. When the calcium channels are inhibited/blocked, the communication stops. Communication between neurons is what keeps neurons connected. When the communication stops, the connections reverse and neurons disconnect. This is an equivalent statement to brain degeneration.
Brain degeneration may not be permanent–it takes a lot of work and a change in nutrition to go after changes. Most people who remove most/all carbohydrates and replace vegetable oils with animals fats experience amazing clarity and the lift of brain fog. These diets may go under the name LCHF (low carbs high fat), ketogenic, MAD (modified Atkins diet), or carnivore diet. I doesn’t really matter which version you try. The brain regenerative process occurs from fasting over 16 hours–fasting, meaning no food of any kind but you must drink water and supplement salt to maintain your electrolyte. These diets place you into ketosis, a metabolic form where the primary fuel for your body is ketones and fat and not glucose. Ketosis requires that you are not taking daily prescription medications, since some interact with ketosis.
You are welcome to join my LCHF migraine group to learn more about our approach and why we all are migraine and medicine free, and if you can move into ketosis, we will move you over to my ketosis migraine group.
Looking forward to seeing you there,
Angela
Thank you so much Dr. Stanton for you thorough and prompt reply.
I found your reply for thought provoking and am considering seeking a full body re-assessment. For years I have seen an Internal Medicine Doctor but she has never taken a complete approach to the extent that you just did.
I’m 55 yo and yes, over weight. I wear a size XL/16 so not huge but yes, over weight none-the-less.
My struggles with depression/anxiety have been more then 25 years and it has been the source for most of my medical care prior to AS. I have been hospitalized, tried ECT’s and the past two years have had good success with TMS. (Thank God) Way less invasive and holds way less stigma.
When my thyroid issues first began my depression tanked. It leveled off a tad once I was medicated with Synthroid. I have always felt the all of my struggles are related. Even with the newly diagnosed AS I struggled to accept the label. I can’t help but feel it’s all from something else.
You have my mind going in a completely different direction. You have my mind returning to years ago back to following my gut.
Diana
Hi Diana,
I am glad I got you thinking more in terms of “whole body” rather than just individual parts. Everything is connected in our body so there is no reason to suspect that one has a health condition specific to that organ and it is not associated with anything or everything else. 25 years ago, when your depression started, we knew much less about the importance of nutrition. Actually, 25 years ago we knew less than we knew 40-50 years years ago! And while this may sound weird, we have a nutritional movement based on no scientific evidence. It has bee–and still is–the greatest scientific experiment in human history, in which we don’t even know we are part of an experiment.
This experiment is officially called the “Heart Health Movement”, which had nothing heart or health about it, and that is why, today, half the world is ill with various health condition: metabolic diseases (your heavier weight than normal for you is part of that), depression and various other brain health condition are also nutrition related, asthma, arthritis, PCOS, psoriasis, allergies, IBS, urinary incontinence, Crohn’s disease, most autoimmune diseases–including thyroid–and a host of other very common health conditions are all nutritionally exacerbated or nutritionally created condition, all of which can either be completely prevented, reversed, or at least put to remission by changing one’s diet. I am walking the talk so I know.
I hope you will give some action to your thoughts once you are ready. The change is huge and requires lots of willpower. I find that those who got sick from modern Western nutrition in any shape and form and have discomfort or pain, have amazing willpower and can completely change their lives, as I changed mine. 🙂
Good luck!! Keep us posted!
Angela
Hello…..I stumbled on your site this morning by chance. I found it very interest, thought provoking and disturbing.
Many years ago, ten maybe I was put on Topamax for petite seizures. I remember losing some weight on the drug but not much else except I wasn’t on it for a long length of time as I didn’t find that I fully trusted the doctor that Rx the drug.
Two months ago my psychiatrist Rx Topamax for my daily struggles with anxiety. I’m currently taking 200mg x 2 a day. With in days the anxiety was much better. I have also lost 14 lbs. (much needed)
I have a medication list a mile long….high blood pressure, hypothyroid, high cholesterol, 4 meds for depression/anxiety/sleep. Six months ago I was diagnosed with AS (Ankylosing Spondylosis) and have been been taking high doses of anti-inflammatories and the past two months have been receiving Enbrel injections.
Besides all of my AS symptoms….Over the past two months (coinciding with both the Enbrel injections and the Topamax, I have had a nasty cough and have been throwing up initially every 6 days and last week three times. I also have right ear pain and have seen an ENT and have nothing wrong with the ear. He did a balance test of which I did horrible on the eyes closed/cushioned stability test. I feel unstable at times, dizzy at times. I recently reported these side effects to the Enbrel support nurse and she feels it is unlikely the Enbrel.
Until reading your site…It never dawned on my that it could be from the Topamax.
On top of all of this I had my yearly blood work done last week to check my thyroid function. My TSH w/reflex to FT4 is quite low (0.29). I’ve yet to hear from my doctor that ordered the test but if I’m researching it correctly that means that it is now the opposite of what I’ve always been taking meds for….Hypothyroid. Now it is low pointing to Hyperthyroid.
Again….Can this change be from the Topamax??
If I’d never started the Topamax would I still be losing weight, throwing up?
Was the initial anxiety increase actually from my change in the thyroid/pituitary?
I know you wont have these answers but you see where my mind is going.
I wanted to post so that you could add one more item to your list of reasons doctors Rx Topamax. ANXIETY
Diana
Hi Diana,
Quite a story you have! So let me try to see if I can understand what your doctors did.
First, Topamax is specifically for seizures but it is supposed to be only used as a secondary drug–meaning it is not considered to be sufficient on its own to be used alone as a seizure medicine. So your first doctor who prescribe Topamax for your petite seizures had the right idea but I think he/she should probably have had to prescribe Gabapentin or Pregabalin instead of Topamax, though if you had infrequent and small seizures, the Topamax may have had been enough.
The psychiatrist prescribing Topamax for anxiety is malpractice–if indeed he/she said that the prescription was for anxiety. Anxiety is very specific to a certain brain region where anxiety peptides are released. Topamax is a voltage dependent calcium channel blocker, which blocks all neurotransmission between neurons systemically across your whole brain–also affecting the heart, which works on voltage, and whose contractions are even more depending on calcium than the brain is, where it is merely used to kick neurotransmitters out of the neurons. The fact that your anxiety was better at that time hints at Topamax blocking those neuron regions as well that release neurotransmitters for anxiety, but it unleashed a torrent of other problems for which now you are taking a ton of medications.
Your high blood pressure, anxiety, hypothyroidism, and high cholesterol are likely induced by your diet. The standard American diet (SAD) is full of grains and carbs, reduced fat, reduced salt, not enough water, not enough meat and healthy fats, all of which add up to bad health. The dietary recommendations are slow to change but are now starting to change. Eating a lot of carbohydrates (fruits, vegetables, grains, starches, juices, sugar, etc.,) generate a lot of insulin. The brain is extremely sensitive to glucose and insulin. Too much variation in glucose is an anxiety cause and too much insulin prevents the brain from getting enough glucose (like in the case of Alzheimer’s disease). Also, both glucose and insulin damage the myelin–the myelin is the white matter in the brain, a wax-like element made from cholesterol, which is supposed to insulate your neuron’s axons so they can communicate well. Glucose and insulin damage this layer and thereby increase seizure activity.
In sum, your current condition is a result of over-medication and the likely under-nourishment by nutrition-poor foods, and too much carbohydrates in your diet. All of the symptoms you described above cab be related to these two factors. It is not one drug, like Topamax. It is the combination of all the drugs and your diet. I would recommend you read online–or perhaps some trustworthy books–about the benefits of a reduced carbohydrate diet, be it the Mediterranean or LCHF (Low Carb High Fat), and the increased healthy fats, such as the use of animal fats for cooking, eating olive or avocado oil (cold), and trashing all processed vegetable or seeds oil, all sugar, processed foods, drink plenty of water and eat healthy. No medication can undo the damage the wrong foods can cause.
How your thyroid is working cannot be evaluated by the TSH alone. You also need to get free T3 and free T4 tested–I know that these are not always covered by insurance, but without knowing all three, a correct diagnosis cannot be made. For example, a decreased TSH can mean hyperthyroid but it can also mean hypofunction of the anterior pituitary… we cannot tell from the TSH alone what it means. If T3 and T4 are increased and TSH decreased, you likely have hyperthyroidism and I would then go further and get another test to see if you now are heading towards Grave’s disease. However, this is an autoimmune disorder, which is completely resolvable by the correct nutrition.
I hope you find this helpful.
Bets wishes,
Angela
I have been on 200mg of Topamax for two years. I use to have horrible memory problems, foggy head, speech problems and my fingers felt like a pin cushion. My neuro told me about a supplement on amazon called Euphasia that eliminates the side effects of topamax. I now order it from their website because it is cheaper but all of my side effects are gone.
Robby, that supplement is nothing but calcium and vitamin C. Might as well just take a cheap calcium and vitamin C product. There is nothing special about this combination so if it works, just get its cheap equivalents separately.
Angela
It’s $24.00 to buy the calcium carbonate and vitamin c separately and $20.00 to buy the Euphasia. 🙂
Dr. Stanton, do you have guidelines for tapering off of Topirimate? I need help. Pharmacists, FDA and MDs are worthless. I need to get off. My kinesiologist is helping me and identified this as the #1 worst of the worst right now. I’ve been tapering off of Lyrica and Cymbalta also. I have been on Topamax/Topirimate for over 20 years for migraine. The others for almost 5 years for depression and fibro from a trauma life event. I also take imitrex when I still get migraines. Which lately is too often. Former Psych had increased Topirimate to 200mg at some point when he had me really drugged up (klonopin, Abilify, rexulti +) I went CT from those not knowing better. I quit sugar in Oct 2017 and slow tapered. I eat clean. The rest of my story is sad, and happy because I am still alive.
I’m at 100mg 50/50 Topirimate until now Going to 50 at pm today, per testing with my kinesiologist. What next though? I have been told mixed things on breaking these tablets? What about alternate days? How long do I hold and how long should it take to get off.
I will finish Lyrica taper after Topirimate and then finish Cymbalta.
I am grateful to find your articles. Thank you.
Hi Jill,
Thanks for your post. I do have guidelines but I cannot provide them on a blog–a blog is not a place to give such guidelines. Please join the Stanton Migraine Protocol(R) migraine group where your membership forms a contract such that I can provide you with a guideline that you can apply with the support of your kinesiologist’s support. The group can also give you support while you tapering off and teach you how to become migraine free without the need for any medicines. 🙂 It is a win/win by joining the group. There are three questions at the virtual door of the group. Please make sure you mention you responded to this article. Looking forward to seeing you there,
Angela
I was looking for a report I read years ago on the link between Aphasia and Topamax and came across this site. It was a pleasure to read this article and the previous one.
In my case I took eleven tablets over nine days and my world as I knew it ground to a halt. I have thought for many years that this drug is dangerous and am horrified at how each year it seems to be the new wonder cure for another condition. There is so much risk in how this drug has progressed to be the new cure all it scares me.
Sadly I see it as a potentially Thalidomide type scenario in years to come.
I am UK based.
I had to battle so hard to get help. It took months to get into Speech Therapy and even longer to get the Pain Management Consultant to acknowledge the ‘chain of events’ and refer me to UCH, and then he simply referred me into nowhere and it was picked up thankfully by an Canadian Professor who worked with an American Professor from Kings who specialised in Speech and they knew exactly what had happened and what had caused it.
They referred me into the National Neurological Centre , and for two years I went up and down as an Outpatient where initially they tried to prove my issues were dementia and then some rare neurological disease. Eventually I came under the care of Professor Warren and the end conclusion was that the chain of events most likely burst a very small blood vessel in my brain and he emphasised that brain scans were only as good as the person who reports on them and some things are just to small to see.
Strangely though on talking quietly to some of the European Associates/trainees they were very aware of the drug and how dangerous it is.
Well on the upside I lost two dress sizes in the first two weeks and still years later have zero interest in food. It’s like an enforced anorexia. I have learnt to talk again, and know it will always be inappropriate at time. Word blindness and back tracking on conversation is easy once you realise that people do not listen properly. The cognitive issues are manageable if I make lists.
Reading and writing remains an issue and hand eye co-ordination is often a problem, but I have learnt to live with my defects with good humour. Tiredness is my enemy as it makes it worse………..but among close friends there is always a competition going to see who has had the most wackiest unreadable text from me.
Thank you for such a well written article. Yvonne x.
Dear Yvonne,
I read your story with great familiarity (I am sorry to say that). Not just because it is Topamax you are dealing with but because of the UK medical system. I deal with many migraine sufferers from the UK and I know it is utterly impossible to get help there for most things. I am very sorry to hear about your suffering. I enjoy your humor at the end but I shared a tear with you for that.
What was the original reason for your starting Topamax?
It is indeed prescribed for everything from seizures to broken nails to reduce hunger and many more. There is a reason for that. It is one of those medicines that provides no direct treatment for anything specific; it merely closes all doors that may open to prevent anything from going through. Hence the horrible side effects. It inhibits voltage dependent sodium and calcium channels, effectively inhibiting neurotransmitter release, systemically in your whole brain, affecting every single region of the brain, operating everything from temperature maintenance, to speaking, tasting, logic, thinking, talking, seeing, smelling, hearing, etc. It cannot distinguish between areas that may benefit from those that don’t.
However, if you started taking Topamax for some neurological conditions, there may be hope of recovery–age dependent and also how long you have taken the medicine.
The brain is an adaptive system and can recover from many injuries, provided the systemic damaging stops and recovery is given a chance. In my migraine groups, there are hardly any members who were not taking Topamax at one time or another–some may not even be migraineurs. The key is to change lifestyle such that it is regenerative to the brain and taper off Topamax.
The UK has different regulations for this than the US so find out what you can or cannot do. Like, will your doctor label you non-compliant if you taper off Topamax and kick you out? (I heard stories like that.) In the US doctors have no such rights. So look into your rights. Look to see if your doctors would support a program that will help you taper off and recover otherwise–provided you are not taking it for seizures.
Please let me know. You are welcome to join my migraine group, which is no longer just for migraineurs here.
Best wishes,
Angela
I never did come back to you, and just put all my effort into improving my own life quality…….but I did start a support group online. Which took a while to get going but is now growing so fast it is quite scary to see so many worried people looking for help. The site draws a lot of negativity from members and we support and suggest and persuade them to seek help if it looks more than standard side effects. And we also see some good success stories which raised peoples hopes.
We recently did a poll on what conditions they suffered with and why they were taking the drug……and it was worrying at how far this drug has slid sideways into treating some really random conditions……….age never seems to matter and recently a mother joined us because her four years old had been prescribed the drug.
Six years down the line, I still think that this drug is a ‘wild card’ with the potential to be an international disaster. It has as time has gone by simply lost its way from the original license.
Dear Yvonne,
I couldn’t agree with you more! I find the same: children placed on Topamax together with some other very “adult” medicines like Amitriptyline, Nortriptyline, Propranolol, and others. Very scary indeed. Particularly Topamax, which is a brain degenerative drug–breaks connections. Yet a child’s brain is still developing. Very scary and very sorry to hear.
Congratulation for your online support group! I very much appreciate your care and concern for others and honor your time spent helping them. <3 Little by little we will change the world. <3
Hugs,
Angela
I found your website while looking into my blood test results which have been indicating low sodium levels. I started taking Topamax in 2008. At first it was 50mg daily, then 75mg daily for a couple more years, then in 2013 my doctor bumped the dosage up to 200mg daily. He also put me on Wellbutrin which I took for 9 months before discontinuing it. I went back on SSRI’s in 2017, this time he prescribed Zoloft and also Oxybutynin. Over the last 5 years I have been increasingly sick with various upper respiratory, sinus & ear infections (or so I thought) due to almost constantly running an elevated temperature between 99.2 – 100.00, pressure in my head and pressure & popping in my right ear. For a couple of years I woke up and went to bed with a headache, interspersed with migraines monthly. During that time I was prescribed a few rounds of Levaquin, 1 of Cipro and 1 of Avelox. Even though half the time the doctor couldn’t see any evidence of infection. They also prescribed Prednisone to take along with the antibiotics. I never seemed to get any better, my energy and sense of general well being continued to decline.I was also very dizzy (vertigo effect), I couldn’t tilt or lay my head back without getting nauseous and would even get car sick. I also had a far amount of tingling in both hands and feet as well as restless leg. In October I went to the hospital thinking I was having a heart attack or stroke. While my bp was elevated to 160 I wasn’t having either of these. Although my heart was racing, I was short of breath, dizzy, my left side had a loss of sensation compared to the right with my left thigh being very numb. They did however find that I had inflammation in my brain and a tumor/lesion. I was kept for 3 days and treated with high doses of prednisone. When I got home I felt and acted like I was an elderly recovering stroke patient (I’m 48). I’ve seen 3 neurologists, been tested for every possible autoimmune & had a spinal tap. All my tests come back negative or clear. The doctors say they aren’t sure what’s going on as even the abnormal area on my brain doesn’t look or act like anything they’ve seen before. In the meantime I’ve gone back to the ER 3 times since October feeling as if I was again having a heart attack or stroke, only for everything to be fine. My heart pounds & races, my bp goes from high to low, my temperature goes from hi to low. I’ve been having cold sweats, hot sweats, chills. My eyesight has been affected – very blurry, but will clear up some through the day only to blur again. I have a heavy, weighted feel to my left leg and lower back. I struggle to have the energy to get through a normal day, napping quit a bit. My memory is compromised, I struggle to keep my train of thought. I have extreme anxiety constantly. My husband says my mood is all over the place, crying, angry, happy, from day to day it changes, I know mostly because of the anxiety. Shortly after coming home from the hospital, I quit taking the Topamax, Oxybutynin & Zoloft, pretty much cold turkey because when I took them I seemed to have another ‘episode’ like the one that sent me to the ER initially. The 1st of January and then again 3 weeks later I was treated with 250mg Levaquin and 750mg Levaquin for sinusitis. But was unable to finish the 2nd round of antibiotics because it was also making me feel ‘episodic’ like the other meds did. I’ve seen the articles you’ve published, it seems to me that maybe a serotonin attack is what sent me to the hospital but all the residual effects are from a combination of Topamax, steroids and being Floxed. My question at the point is can this combination cause an abnormal MRI, I haven’t seen where anyone else has had this issue. Where do I go from here.
Dear Suzanne,
You could very well have had serotonin syndrome–particularly at the time you also had fever–but you managed to survive that and so likely recovered from that. I am certain that all these medicines have left quite a bit of nerve damage–no question about that. Then to top it off you took quinolones, which floxed you–I am certain about that. They flox healthy people with healthy immune system and you were definitely compromised before you even started to take them. Prednisone is also a monster as it ends up in diabetes. So you have a list of what I call “killer drugs”. I am glad to see you can write and think and that you are alive actually! Happy that you are because with proper treatment (nutritional treatment) nerve damage can be repaired. Yes indeed, damage can be caused by these drugs such that it shows up on the MRI. The chemistry is complicated and I don’t want to get this comment be a sleeping pill, but all the meds you toook, some doing opposing things, blocking various voltage dependent channels, block the clearance of junk from your brain plus those nerves that were damaged or died may also show up as such and not yet cleared out of your brain as it is shut down from functioning the way it should.
Your didn’t mention what the cause of all these medicine takign was–did you have migraines? Fibro? Something else? Do you have now health condition–in addition to all the drug-caused ones? Are you still takign any of these drugs?
It would be great to get your life back by a change in lifestyle: quitting all grains (not just gluten but all grains), all sugars and sweeteners, all starches, juices, smoothies, shakes, all high glycemic index fruits and veggies. Stick with the foods that are not inflammatory: low carbs and high fat (high animal fat) diet, with moderate about of good quality grass fed, free range animals of any kind and fatty fish. Your brain is over 80% fat and cholesterol, which provide protective functions. If you don’t have that functioning, your brain is compromised. The brain is made from DHA fat–this can only be found in animals. Vegetables have ALA version that converts very poorly to DHA. So start eating meat, fish, take cod liver oil to rebuild vitamin D and DHA. Start a healing diet.
Best wishes,
Angela
Thank you Angela for replying. I started taking the Topamax for migraines, then after having upped the dosage to 200mg daily, I also started having incontinence that I & my doctor thought was due to menopause so he started me on the Oxybutynin.. I now know it was from the inflammation on my brain as I had a marked increase in October when I went to the ER and a huge decrease after my spinal tap, seems it relieved some of the pressure on my brain. I took the Wellbutrin & Zoloft for short term intense stressful family situations. I didn’t intend to stay on Zoloft as long as I did but the situation didn’t resolve and is still ongoing…Within 3 weeks of leaving hospital back in October I stopped taking the Topamax, Zoloft & Oxybutynin, as I noticed a correlation between taking them and recurring episodes of what sent me to the ER in the 1st place…I continued to have flair ups but they were minor in comparison & I got tired of running to the ER every time only to be told they couldn’t do anything, wait for my appointment with a neurologist. But it did at least give me a good graph of all my lab work since they ran it every time…The neurologist tried me on a very long round of prednisone(2months) hoping it would help. Now that I’ve tapered off all the symptoms are coming back quickly and more extreme than before in October. Clearly the doctors I’ve seen so far have not been helpful or knowledgeable on this subject. Would you know of any doctors you could recommend who are familiar with these issues in NC or even Virginia or SC. I’d be willing to travel to the next state if necessary to get help for all this. It’s really impacted my life severely.. I have been looking into your Keto diet recommendations. If you could also recommend which group to join that would be great!
I really appreciate you getting back to me and all the research/work you’re doing! I called my mom to let her know about your website. She’s been on Topamax as long as I have for migraines also and just started on Wellbutrin the past month. She’s tapering off the Topamax now and holding off on taking the Wellbutrin until she’s off the Topamax.
Hi Suzanne,
Incontinence is not caused by menopause–millions of women go around without it after menopause–including me. Incontinence is caused by electrolyte imbalance–the water if going through you and your kidneys are not able to push water back in since nothing is holding it in. At the same time, this is also a sign of dehydration. This could have been caused by Topamax, which is both voltage dependent calcium AND sodium channel blocker and sodium (part of salt) then is not able to function properly to form electrolyte.
A spinal tap that releases pressure in the brain tells me you have some major health concern–perhaps caused by the many medicines you are taking. All these meds and medical treatment for migraines? You really need to read my book on how to prevent and abort migraines without a drop of medicines. This is a link to the 2nd edition that was released a few months ago, which will teach you how. The e-book is only available through amazon but paperback everywhere.
I would recommend you look into many changes in your life, starting with your nutrition since the wrong nutrition to the person can make or break health! Going from drugs to drugs will not cure a health condition that is likely caused by nutritional mismatch to your body. It is important to ficus on the underlying cause and not on symptoms.
Hugs,
Angela
2nd try posting, first try ended up with a few others in the write for us area somehow. Here goes, and am writing on a Kindle finger picking on tiny keyboard, hoping it doesn’t “fix” anything it doesn’t understand.
My husband had/has TBI over a decade ago, migraines and constant tension headaches started nearly right away but VA ignores TBI aspect, and he has been on so many meds successively and or concurrently to make life less painful for the migraines, headaches, & other post knocked off a 2 story building type injury things he deals with now. They started him on Topamax about 2 years ago, & his migraines really slowed @ intro dose of 50mg a day, but still had headaches and occasionally taking the only last chance med when he gets that premigraine feeling (1600mg ibuprofen yuk), so a neurologist said wow just double your dose, and suddenly migraines & headaches were gone-happy days.
Then a few weeks later he noticed a discoordination in one hand (the side he isn’t already slightly paralyzed), and within a few weeks he developed a tremor in that arm, and it sort of dread to the leg eventually. We contacted the VA repeatedly about it but between “that’s not something that topiramate can do” and “I’ve never heard of that” and your doctor has retired and we are still months away from finding a replacement so you can hope for any continuity in treatment…etc it was 6-8 months before we brought him down to 75 mg from the 100 and the tremors never left his arm. Also got all headaches & some migraines back… He did the AT over the summer (DISABLED DOESN’T MEAN UNABLE just means more determined!) and had finally talked with the new doc about tapering off the med while hiking-hiking has always made him feel better so it was a good time to try. So after about 3 months from coming off the med, he has the migraines back at full misery (5 trips to DR from them in about 50 days) and adventures in doc prescribed B vitamin overdose misery he is back off meds and miserable, but now with tremors… oh and finally they’ve done some scans, found he has partial empty sella syndrome (pituitary is squashed), optic nerves are a bit bulged, and now a dat scan suggest parkinsons (which tbi can possibly predispose one to, and I am wondering if may also be possibly partially drug induced, as the only symptom displayed is tremors, which turned up suspiciously after suddenly doubling a med known to most internet info pages on it but not known to the va to cause tremors…dreaded topiramate)…I know the tremors seem to have left the leg since perhaps dropping to 75, and surely since going off, and I keep thinking the energy behind and magnitude of the hand tremors seem weaker some times now…
Anyway, long story short, I have had it up to my eyeballs, and am going to start spraying this info on the net, because hopefully the info can help someone doing research, or maybe there are others out there who have had similarscissues and we can point to y’all when we try to shove the VA into everything their act together and say “we are not the only ones to experience that, we are not nuts, be responsible for the mess you have caused!”
… best of luck! If you are interested in his info for research or similar, find us at fixedbydoc.com
Thanks Adda for the horrific story of your husband (and of your family of course). I know of others who got tremors from Topamax so it is not unheard of and similar side effects are listed among the adverse effects. I agree with you. The lack of proper care and understanding about this (and many other) drugs is scary and a lot of people will be hurt unless more information is out there. So thank you for sharing your thoughts here and everywhere else you spread it. You should also post an adverse effect reporting at the FDA, which you can find here. The more people report it there, the louder our voice.
Hugs to you and to your husband!
Angela
Oh and what do you think of the book ‘Grain Brain’ from the neurologist David Perlmutter?
Hi Lonneke,
I liked Grain Brain but I have a preference for another book “Wheat Belly: Total Health”. I found it much more informative and while the Grain Brain is great, I felt that it was pushing very much toward keto. At the time I read that, I was not yet ready for the ketogenic diet so it left me a tad disappointed but the Wheat Belly didn’t try to push me in any direction, only made me see how bad grains were. I quit grains after that book and eventually ended up with the ketogenic diet so I ended up at the goal of Grain Brain anyway–I just found the other book more enjoyable.
In either case, they both are great book.
Hugs,
Angela
I’ve also read that l-tyrosine would be helpfull. Have you heard of it? I would try anything to get back to normal again!
Hello Angela,
I responded to your previous article about topamax some months ago. Ik still feel like my brain is more numb, not functioning as it used to before topamax (i used 50 mg a day for 7 months in 2016). In this revisited article you speak of possible permanent damage. I’m worried that the damage done by topamax is permanent. Ik tried the ketogyn diet and exercise to recover. But i still find myself in derealisation and slow thinking, numb body. Is your conclusion about recovery from topamax less optimistic then before? Probably hard to say but i wanted to ask anyway! Thanks in advance!! Kind regards, Lonneke
Hi Lonneke,
Sorry for all the trouble you are having post Topamax. You took Topamax for such a short time and in such a small dose that your recovery outlook is quite positive. Could it be possible that you have not found the right ketogenic diet process for you and hence it didn’t help you? Let me cover the basic steps in the ketogenic diet since there is so much misinformation about it out there–I am working on a book about it.
Steps:
1) Before you do anything, you really need to check if you have insulin resistance, especially hypoglycemia (reactive hypoglycemia) in particular, since if you do, you cannot start keto with fasting. Whatever I write here assumes that you don’t have hypoglycemia and you won;t faint from fasting.
2) Prior to the ketogenic diet, train your body for drinking proper water amount and eating more salt–both of which are essential for the ketogenic diet. To calculate how much water you need, take 55% of your weight, divide that by 8 to get it in glasses, and add at least 1 extra glass to that in keto. So if you weight 150 lbs, that is 150*0.55=82.5/8=10.313 glasses +1 = 11.3 glasses of pure unflavored water a day. Don;t include anything else you eat that has water in it. You need a lot of water for keto
3) salt: salt is measured as sodium. You need to consume at least as much sodium as potassium–you need to use the USDA database to find the potassium value of foods and match that with sodium 1:1. For reference, 2300 mg sodium is 1 very finely ground teaspoon of salt.
4) Quit all sweeteners–including honey, naturals, sugar substitutes and all things sweetened by them. Stop all juices, smoothies, shakes, alcohol
5) Quit all grains, all vegetables that grow below the ground (except for onions and garlic), all fruits (except for raspberries and blackberries, all legumes, all milk
6) Quit all cooking oils and switch to animal fat for cooking. You can enjoy olive oil, avocado oil, or coconut oil but only cold
7) Don’t take MCT oils. They only burn as ketones, which is great, except they will prevent your own fat from burning so you will not get the full benefits
8) Once you understand the principle of the ketogenic diet, start by purchasing either urine ketone measuring sticks (cheap but inaccurate) or blood testing kit to make sure you are at a range you need to be
9) Start the ketogenic diet by fasting for as many days as you can–5 days usually but if you are a migraineur, join my keto mild group instead since this doesn’t work for migraineurs. Fasting means only water and salt please–you can have broth if you wish or some butter if you are starving but hunger is what will get you into ketosis.
10) Keep on measuring your blood ketones–you want to be between 0.5 and 3.5 measuring beta hydroxybutyrate–and hold it steady. If the numbers go past 3..5, stop the fast.
11) once you are in ketosis, you may get cramps in your legs or heart palpitations. When this happens, take 1/8th teaspoon salt with a glass of water.
12) avoid any heavy exercise while your body is getting keto/fat adapted.
13) There will be no therapeutic benefits from the ketogenic diet unless you start intermittent fasting regularly. For example, I practice the 16:8 (fasting 16 hours and eating within an 8-hour window) every day and once a month or so I do a 24-hour fast. Fasting ability is the reason for the ketogenic diet in your case. When you get hungry and you don;t eat, your body starts to optimize its energy. It removes cells that don’t function optimally and replaces them with new one–particularly mitochondria. This is your way to recovery.
Supplements are not necessarily helpful… no idea. I am not a supplement supporter. But I am a definite ketogenic diet supporter but I find most people do it wrong.
Hope you find this helpful.
Hugs,
Angela
Dear Angela,
Thanks again for your comprehensive answer. I’m going to start the ketogynic diet (with your advice) in a month with 5 days fasting in order to get in ketosis. In preperation of the 5 day fasting i wil start with your 16:8 fasting guideline (except for the big christmas dinner i suppose ;-)).
Some questions:
-Do you, beside quitting stuff like potatoes and legumes, also have to stop eating pumpkins and other vegetables that are rich with starch?
-What does the ketogenic diet do with your pH value? My body didn’t get in metabolic acidose due to the topamax but still doesn’t have a healthy pH value. My body got pretty acidic.
-What does the ketogynic diet do with excitatory neurons? I feel like i’m missing excitatory stimuli even a year after quitting topamax. Feels like having a slow brain function. Will a ketogenic diet, by increasing the GABA receptor have a damping affect on neuro-excitation or will it help my brain ‘wake up’ again? I miss that ‘brain sensitivity’/incitements.
-Does the ketogynic diet (besides a change in sodium/potassium levels) also have some effect on electrolytes?
-Currently i’m using supplements every day, these are: magnesium, multivitamin, fish oil and bee propolis. Is it okay to use them while trying to get in ketosis? Maybe not the bee propolis?
Thanks a lot for your time, really appreciate your help and expertise.
Kind regards,
Lonneke
Hi Lonneke,
You are asking a lot of great questions. Let me address them one by one.
–yes you need to quit all starches (at least at the beginning until you are not fully fat adapted. Once you are, you can take small servings but always test each food you add back to make sure you are in ketosis. I use blood ketone testing, which is essential–though expensive.
–The ketogenic diet makes your entire body a bit more acidic, so the pH lowers. Each organ always has different pH values and the human body must be acidic, because most pathogens cannot live in an acidic environment. The only alkaline organ we have is our blood, and that is why blood infections are so often fatal. Because every organ has different pH value, there is really no such a “a healthy pH value”… there are many healthy pH values within the human body.
–he ketogenic diet allows the neurons to recover in every which way. It seems to relax the brain but increase alertness. My focus now is better than it has ever been (I am in my 60s) and I don’t ever get tired. It increases the brain without becoming excited–so it is more efficient.
–the ketogenic diet is quite neutral in electrolytes since it contains too little carbohydrates to be able to disrupt electrolyte balance.
–you will find that the only supplement you really need in the ketogenic diet is magnesium, and not much else. Since you eat fish and meat, your omega 3 fatty acids are covered; you don;t need any multivitamin since meats are richer in vitamins than plants, and the little vitamin C you need you can from the green veggies you eat
I don;t think the bee propolis is anything of importance–frankly no person on the ketogenic diet takes that so you are not likely to need that. However, some people tend to end up with too light color bowel movement. That is a sign that your body lack carnitine to metabolize fat properly. If so, the supplement you need is Acetyl L Carnitine–but wait and see the color of your stool. It works right away.
Hope this helps,
Angela
What do you think of a toxicology report showing 3000 ng/ml of topiramate drawn from peripheral blood? Seems like a ton imo. How could someone consume this much and is there a taste? Could it be given to a person intravenously?
Mason, that appears to be a very large amount of Topiramate because you got the measures in ng. However, 1 mg is 1 million ng, so 3000 ng is 0.003 mg. This may or may not be a big amount–I am not sure since Topiramate come dosed 300 mg twice daily, etc., so depending upon how it was given and when it was taken, and what dose was taken/given, this may be a big amount or may not be. Intravenous application is also possible but everything depends upon liver clearance quality. A compromised liver may not work so well and drugs like this–especially in combination with other drugs, particularly herbs, could be big trouble.
Hope this helps.
Best wishes,
Angela
Thank you for your quick reply! I tried to respond but my last comment didn’t go through for some reason. Do you have an email where I could ask an additional related question?
Hi Mason,
Your comments should come through–I see none so perhaps it had a glitch somewhere. I have very little time to respond to emails since I work with thousands of migraineurs and have a backlog of emails and other things. Questions here on the blog are great because other people can learn from them. I would much prefer a conversation here if that’s OK.
Thanks,
Angela
What do you think of the Kenneka Jenkins story? She was found to have the 3000ng in her system.
Mason I know nothing of the story other than that a dead body was found in a hotel freezer. Really far from my expertise.
Thanks,
Angela
I was originally brought to this website for the content on Lupron ( I also have endometriosis and was given a single injection) but saw this and had to comment. I am sure there are many people with negative life altering experiences caused by taking Topiramate, and do not want to diminish that, but my experience has been good. Let me explain.
In 2010 I began to have chronic dizziness, along with a few other symptoms. was tested for everything my Dr could think of, then shuffled off to specialists- Neurology, ENT, Rheumatologist, had CT scans, MRI, electronystagmogram, you name it. everyone was stumped and the dizziness continued to worsen and got to the point that at times I couldn’t walk, and would almost fall down just standing still or fall off the couch when an attack occurred. I had to stop driving when an attack almost caused an accident and sent me to the hospital where they diagnosed me with ” vertigo”- Ha! So not helpful.
Finally as a last ditch effort I was sent to a Neurologist at the University of Michigan who immediately knew that I was suffering from atypical migraine, I think then he said some people called it MAV or Migraine Associated Vertigo. I was prescribed a low dose of topiramate and my life slowly got back to normal. I don’t know what went wrong with my brain, but I do know that the only thing keeping me from daily vertigo attacks is topiramate. It saved my life.
I agree there are side effects- I lost weight, and my brain definitely slowed down. It was significant at first, but is not really too noticeable now. Sometimes I have trouble finding words. At first my sense of taste was severely altered ( probably part of why it causes weight loss?) which was a problem since I work as a Pastry Chef- but that wore off after about 5 months, as did the inability to sense carbonation. The Paresthesia was strange and bothersome at first- a weird tingling in the fingertips and hands. But that too wore off soon and instead of being a daily occurrence only happens rarely. All in all, I feel like the side effects I experienced are easily balanced out by my ability to walk a straight line, drive to work every day, and just live normally without having to worry about when the next attack will come. Thank you for posting the other side of the story.
Dear Amber,
There is nothing atypical about MAV (migraine activated vertigo). Quite common and many migraineurs have it. There is a non-medicinal solution that has worked for over 4000 migraineurs and would work for you as well if you tried. The problem is that while most researchers believe migraine to be a “disease”, it is not. It is a variance of many functions of the human brain that I wrote about on this blog, explaining how the sensitized “migraine brain” is the default humans brain and all without migraine have adapted to modern life.
Just as one need not medicate red hair or blue eyes, so there is no need to medicate migraine. Understanding the cause and modifying nutrition to that of what a migraine-brain can metabolize and live on healthily can prevent all migraines. If you want to learn more about it, please read my book or join my migraine group or better yet, do both.
Best wishes and looking forward to having you in the group,
Angela
Just wanted to comment because Topamax ruined me. I took a single dose, 25mg and had over 15 different side effects. I couldn’t think, sleep, coordinate movements or even breathe (I was suddenly very congested, like I had a cold).
The last 24 hours have been hell and I cannot wait for it to exit my system. A neurologist prescribed it to me as the go-to medication for my cluster migraines but i’d much rather deal with the pain than with such an impairing and ruthless drug.
Dear Ana,
That sounds horrific. You are not the first one I hear with such incredible side effects! Why don’t you join our migraine group to learn what we do. There are several cluster headache migraineurs in our group. Cluster headaches improve from the use of oxygen but not every doctor knows that. You should ask and see if your doctor is willing to prescribe a test dose to see how it works for you. In the migraine group though we can help. So please join us.
Hugs,
Angela
I was prescribed 25mg 2x per day and took this for just over 2 weeks. I didn’t quite feel like myself and decided I wanted to stop. My neurologist said I could stop cold turkey and wouldn’t have problems. 3 days after stopping completely most of my days didn’t really feel real to me, and my anxiety skyrocketed. Since i had these episodes at home i was causing myself more anxiety about going home after work because I was afraid I’d have another episode of “unrealness”. My neurologist said these responses are not related to Topomax at all and that my anxiety must have gotten worse from some other cause. (Nothing I can think of). I went and saw my family physician and she said I may have had a rebound response to topomax making my anxiety better and then removing it caused the rebound. The topomax should be out of my system at this point (today is day 9) but I still feel anxiety. My doctor said IF it’s related to topomax the effects should be gone in 2 weeks. Does this sound right for others’ experiences you’ve read about? I just want to be back to myself, this stuff was a nightmare. My doctor upped my Sertraline to 75 mg last night but so far it’s not made a difference today. 🙁
Dear Kaitlin,
Topamax can cause damage to the brain–it is a voltage-gated calcium dependent channel blocker. Each person is different and these voltage-gated calcium channels may slightly differ. Perhaps the Topamax damaged some of these channels. Whether this damage is temporary or not, only time will tell.
The best way to help your brain repair the damage is by eating the right food for your brain, and this includes a change in diet that is heavy in saturated fat and cholesterol, and is mostly meat-based. Most people eat a heavily plant-based diet, and that, unfortunately, works against brain health.
Best wishes,
Angela