In December 2015, I was given Lexapro. I had taken Lexapro previously for 12 years, but because of abnormal blood chemistry and building side effects, my doctor suggested that I cease taking the medication. After five months without the drug, I was improving slightly, but because of life events, my doctor and I decided to begin taking Lexapro again. During the reinstatement of the drug, I immediately began to experience serious neurological reactions that I have come to describe as a brain kindling of sorts. It felt like my head was on fire chemically and electrically. Some of the symptoms that developed included: fatigue, confusion, eye pain, leg weakness, headaches, visual processing disturbances, coordination difficulties, lack of concentration, and short-term memory problems.
Within a few weeks of taking the medication, these symptoms were worsening but my physician was not concerned. In fact, he suggested what I was experiencing was normal and that I continue taking the medication. I did, for a while, until the side effects were so bad that I decided to stop. I published my story on Hormones Matter a year ago. You can read it here: A Kindled Brain: Long Term Lexapro Use Reactions. A year and dozens of doctors later, I have become completely disabled. This is a follow up to my story, told with much help from the editor of Hormones Matter.
Two Years Post Lexapro Damage
I no longer take Lexapro or other medications but the damage was done. I still cannot work, watch TV, read, drive or walk more than a few feet. I have had what seems like a two year long headache and severe vision processing issues. It is going to be another great Christmas at my house.
Though I received diagnoses of Chronic Fatigue Syndrome (CFS) and Fibromyalgia they really were just symptoms of something bigger. Shortly after the CFS diagnosis, an MRI revealed white matter lesions and demyelination. The neurologist dismissed a Lexapro connection. Research suggests otherwise. In the summer of 2017, I was finally given a provisional diagnosis of Lexapro induced neurotoxicity. Just recently, the extent of the brain damage was shown on both on a quantitative electroencephalograph (QEEG) and single-photon emission computed tomography (SPECT) brain scans. Both neurotoxicity and brain injuries were identified by both tests and later confirmed again by additional physicians who reviewed the results independently.
QEEG Results
The QEEG is an EEG with a visual mapping component. It measures the electrical activity or signal transduction between electrodes placed in specific locations on the brain. My test results showed that in certain areas of the brain there was very little organized electrical activity and other areas where there was unusual amount of high activity. What that means is that in some areas of my brain, the signals are very low and essentially not sufficiently strong for the activities that need to be performed but in other areas of my brain, there was way too much electrical activity. Specifically, the report said:
“The patient was found to have a significant amount of low frequency (8-9 Hz) in the right posterior temporal (T6) area. There is an extreme amount of low beta (12-15 Hz) predominantly in the prefrontal and frontal areas that may interfere with executive functioning, organizing, decision making and may also account for fatigue. There is a very unusual amount of high activity for all measured frequencies (1-50 Hz) in the right posterior (O2) area, specifically in the right inferior occipital gyrus (Broadman areas 17, 18, and 19). This may result in sub-optimal functioning in visual processing of color, form, movement, visual perception and spatial processing…
…The analysis of amplitude asymmetries were found to be abnormal for low frequencies (1-12 Hz) stemming from right posterior temporal (T6) area. Also, there are abnormalities for high beta (18-30 Hz) stemming from primarily the right posterior area (02). Both findings are substantiated by LORETA analysis and resembles TBI or other brain damage…
…The TBI index indicated that there was an 85% probability that the patient’s brain is functioning as if there is a TBI 0.95 on a scale of 0-10.”
This was the first confirmation of the cognitive dysfunction that I have been living with for the last few years. Doctor after doctor told me that my symptoms were not real and somehow made up (and some still do, as the QEEG is used mainly in research circles and not always accepted in conventional medicine). The QEEG clearly showed the abnormal electrical activity underlying my symptoms. Next up, the SPECT scan, a test I had to fight for, because again, no one seems to believe that a drug like Lexapro could cause such damage.
SPECT Scans
SPECT imaging shows brain activity (blood flow, which represents local brain metabolism and energy use). The technology uses radiolabeled isotopes that are then reconstructed with algorithms to display in color 3-D images of brain activity. The images below are some of my brain scans. Regions displayed in blue represent a state of very low activity called hypoperfusion and those in red represent hyperperfusion – excessive activity.

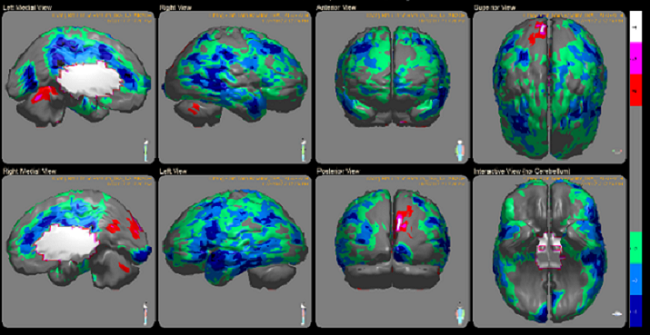
From my images, you can see several areas of both abnormally low and abnormally high activity with very little normal brain function anywhere. From the report:
- At rest, the overall cortical activity was reduced in a diffuse, decreased, patchy pattern.
- Focal areas of abnormal cortical hypoperfusion were noted in the bilateral anterior frontal (L>R), left posterolateral frontal, left orbitofrontal, right dorsolateral prefrontal, bilateral anterior and medial temporal (L>R), bilateral superior parietal and bilateral occipital areas.
- Focal areas of abnormal subcortical hypoperfusion were noted in the anterior aspect of the pontine portion of the brainstem, bilateral caudate and right lentiform areas.
- Focal areas of abnormally increased cortical perfusion were not noted.
- Focal areas of abnormally increased subcortical perfusion were noted in the bilateral thalamic and left lentiform areas.
The doctors conclude:
“The nature (diffuse, patchy), location (cortical and subcortical), and pattern (involving all lobes of the brain) of these abnormalities is primarily consistent with the scientific [literature] pertaining to a toxic/hypoxic/neuroinflammatory process and the patient’s clinical history, as obtained, of a medication reaction which was received after the blind review. These results agree in large part with outside EEG data showing hypofrontality and NM report showing left frontal abnormality, likely not to be artefactual.”
What This Means
My brain is a mess. According to the Hormones Matter editor, the areas of low activity in the various regions of the prefrontal cortex would explain my difficulties executive function, things like planning, decision-making and lack of concentration, while the reduced activity in the temporal and occipital lobes would explain my memory and vision difficulties, respectively. The reduced brainstem activity would connect to my walking and balance difficulties, but also, poor to autonomic regulation (the autonomic nervous system controls all automatic bodily functions including things like breathing, heart rate, temperature control, digestion, sleep/wake cycles, etc.). The areas of my brain on hyperdrive may reflect compensatory reactions, last ditch efforts to kick start some of the underactive regions. The thalamus (plural thalami), in particular, acts as a relay station between the brainstem and the rest of the brain for motor, sensory signals and ‘emotional’ signals via its connections to the limbic system. Mine seem to be screaming ‘wake up’ to the rest of the brain.
Please be careful using these medications, particularly psych meds and especially when prescribed for minor issues like a fear of flying or work-related stage fright. If I knew then what I know now, I would have never taken Lexapro.
*TBI: traumatic brain injury
Update: Neurocognitive Testing
In October 2017, I had a battery of neurocognitive assessments. The results have only recently become available (March 2018). According to the report, the decrements in cognitive ability were consistent with the QEEG and SPECT results indicating probable neurotoxicity with brain damage. Some of the findings included:
- An approximately 9 point drop in IQ from premorbid (pre-medication reaction) levels.
- Impairment of perceptual reasoning, working memory, processing speed, and full scale IQ (FSIQ), which is now at the 7th percentile.
- Significant declines memory function including auditory memory, visual memory, visual working memory and immediate memory (2nd percentile).
- Significant decline in manual dexterity with performance below the 1st percentile.
- Severe decline in executive functioning.
According to the doctor’s assessment:
“The neuropsychological testing indicates disability from gainful employment for the foreseeable future. The results of this work is a diagnosis of Toxic Encephalopathy (ICD 10 G92); DSM-5 Substance/Medication Induced Major Neurocognitive Disorder (ICD F13.97).”
He also indicates that
“…the abnormal neuropsychological findings consistent with neurotoxicity; personality testing consistent with neurotoxicity; abnormal advanced brain imaging and QEEG findings; and no other reasonable explanation for the claimant’s illness and resulting disability, in my opinion, Lexapro and associated drug interactions caused this neuropsychological decline.”
Again, I cannot stress strongly enough how dangerous these drugs are. Please consider my story before taking these medications.
Postscript: In 2020, I had an evaluation by an independent forensic medical examiner. She concluded:
Within a reasonable degree of medical certainty, it is my opinion that the decline in your health has been caused by the combination of DNA variants for several CYP450 genes, with reduced metabolic capacity together with prescription psychoactive medication which caused drug-gene, drug-drug and drug-drug-gene interactions leading to severe toxicity and consequently brain damage.
Share Your Story
If you have suffered from a medication reaction and would like to share your story, contact us.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.


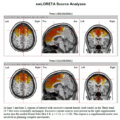












Here the same – but after cold turkey from duloxetine. I took 20mg for 10 years.
I stopped in august 2023 and I’m still in horrible condition – can’t live, only trying to survive from day to day. Lost my job, often bedbound. It’s so sad looking at old pictures, like a time travel in an other part of my life.
My worst symptoms: anxiety, panic, derealization, depersonalization, dystonia, tremor, tinnitus, teeth chattering, crying spells, brain zaps, depression, suicide thoughts, back pain and so on.
Is this still active? If so, could you please email me CF, I want to know if you have recovered and how.
Thank you
The study you cite (https://www.ahajournals.org/doi/pdf/10.1161/STROKEAHA.107.498097) in “:Research suggests otherwise” as evidence of white matter lesions from Lexapro only found evidence for lesions associated with Tricyclic Antidepressants (TCAs), which do not include Lexapro. The SSRI finding (which would include Lexapro) was “statistically insignificant”, meaning not mathematically different than random.
There are numerous studies linking SSRI’s to brain lesions.
“ University of Pittsburgh Study
Researchers at the University of Pittsburgh explored the cerebrovascular effects of a variety of antidepressant drugs in 47 patients, age 60 or older.53 In order to be eligible for the study, participants had to be suffering from at least moderately severe depression. Treatments consisted of one of three serotonin-modifying drugs: escitalopram, duloxetine, or venlafaxine. Brain scans were performed at baseline and again following 12 weeks of drug exposure.
Two sets of findings were significant. Among the 24 patients whose depression failed to remit (as defined by a score of 7 or less on the Montgomery-Asberg Depression Rating Scale), antidepressant treatment was associated shrinkage of the hippocampus. Among both sets of patients (remitters and non-remitters), all three antidepressants were associated with an increase in the volume of white matter hyperintensities.”
I took lexapro for 4 weeks and my symptoms were horrible. I’ve been off 4 months and still struggling. First mri in March showed spots in white matter. Another mri tomorrow, let’s see what that shows. Neuro will probably call it MS but we all know what it is.
I was one of the first “triers” of Prozac during the early 90s. I was 17 years old. I was put in one of those adolescent psych hospitals which was one of the worst experiences of my life and I can tell you I didn’t belong there. It was abusive. I wore the same underwear and socks for a week before I was “allowed” to wear clothes. I could write a novel about how wrong these places are to people but I won’t do that here. I hesitantly agreed to Prozac and after weeks it wasn’t helping me but they told me to stay on it. 3 months later I almost died from what I was going through and was admitted as a study patient at a hospital because our insurance ran out. I was probably among the first studies showing how awful these medicines are, and instead of being justified as being called medication damaged I received every diagnosis under the sun and my life has never been the same. I’m not the person I was. At that time I had tried psychedelics and cannabis a few times as did all my friends, but NOTHING was as bad as what Prozac did. None of them were on SSRIs and none have ruined lives like mine. I want justice, and the world will never provide it.
Same story here. Was prescribed Lexapro after what seemed like an episode (just one) of anxiety. Right away developed abnormal thoughts of hurting myself and others, severe anxiety about nothing and visual issues. Doctor insisted it’s normal and will go away. I battled for 6 months but it only kept getting worse. Once so tapered off real horror started. Now I’m unable to watch TV, vision is blurred, have constant memory issues, can barely walk as my legs feel like they are going to collapse, I am unable to feel any type of pleasure, can’t focus, can’t remember simple words, all the intrusive thoughts became even worse and added suicidal thoughts. It’s been over two years since last dose and I’m starting to lose hope. Two years of being bedridden horror and visits with tens of different doctors. Two opthalmologist confirmed they’ve seen it before but neither had a solution. It either will get better by itself or not. Of course I spoke to a psychiatrist (not the same one that prescribed Lexapro) and she has seen it as well. No solution other than “let’s try this drug”.
I’m wondering how many of people that are homeless were damaged by this drug.
Why would you be out on ssri due to one episode? Very weird. Sorry to hear your struggle. I had chronic GAD And Lexapro has been god send
i took only a few lexapro and my brain has been deteriorating since for the last 10 months, non-stop ear worms, head tension/pressure, cognitive impairement, insomnia , unable to work and function, totally bedridden and homebound.
does anyone has similar symptoms? will it improve? im feeling sicker physically and mentally
Yes Carol. I’m in the same boat. Took it for 4 weeks, been bed bound for 4 months. Cognitive decline, mental fog, balance problems, vestibular disorder, vision problems (not corrected by glasses)
Hello,
Have any alternative diagnosis been made since then? One that comes to mind is multiple sclerosis given the white matter lesions, which could explain the symptoms you were experiencing at the time of increased stress (which is typical for an MS flare up).
If I had MS do you think I would have taken the time to write these articles that specifically describes my condition being caused by Lexapro? My medical history, symptoms and the diagnostic tests verified my diagnosis and ruled out any other cause.
If you did not have brain imaging prior to taking Lexapro, how is it that you can conclude that these abnormalities were not present beforehand and have just been worsening with time with no correlation to the medication?
Why would anyone get brain imaging when they have no symptoms? Medication injuries are diagnosed by “cause and effect” and by abnormal tests supporting that effect. All other considerations of what caused my decline were ruled out.
I have been on Lexapo for about a year and did not like the side effects so I tapered off. I have brain zaps constantly throughout the day. I am worried I will not get back to normal.
I have been taking lexapro for 10 years. From the first day I developed Visual snow. The doctor insisted that I had another problem and you were already laughing as I explained the syndrome to him. There have been countless researches that this pill does. I have dizziness, migraines with aura and I spent many years with a lot of paracetamol. I made many attempts to cut it. I was convinced that I got it 3 years ago before I took the pill from a little cannabis use. I have only cut it for a month. I do not have a headache. Eyebrow pain left. my head feels burning and it hurts due to the many years of migraine. everyone thought I had all this stress.even now they do not even know the syndrome that the doctors developed here. we do not have good doctors in my country. I have a strange feeling in my head as if something is going very wrong. I’m waiting to see if I have any improvement. I did 4 magnetic the last few years because of headaches they came out clean. I have not done this year.I’m looking for a doctor to understand me, I’m alone. only my boy understands and has stood by me well. i have stronge memory issues. I dont even remember names. I think i destroy my life. i wish all the byrning sesnsasion go away. How long did it take to you to the very bad withdraws go? Last 5 years i took 10mg. Today is day 29.
HI,
IM SO SORRY,
I HAVE BEEN ON SERTRALINE FOR 6 YEARS BUT AFTER STOPPING, I AM SEVERELY DEPRESSED AND HAVE TRIED EVERTHING. I FEEL LIKE MY BRAIN IS DAMAGED BECAUSE OF IT.
PLEASE CAN YOU SHARE ANY INFORMATION ABOUT:
WHAT DID YOU DO TO GET BETTER? IS THERE A TREATMENT, A WAY OUT OF THIS? TELL ME THERE IS ONE….
Thanks for the story and all the comments. Now for my friend: total of 30 years on anti-depressants starting with minor ones including 16 years on Lexapro. Her ophthalmologist told her point blank if she stayed on Lexapro she would go blind. That was a PTSD event a few years ago. Now the glaucoma specialists she sees tell her that it’s not correct. I went and listened and when it looked like I was going to say something the specialist gave me a very cold look.
I also went with her to the cardiologist. He also understands anxiety and said there are patients who stop exercising due to heart anxiety, then get weaker and thinner in a spiral. So he said to do 10% more exercise per week. I am encouraging that and 10% more eating per week. She is 92 pounds.
Back to the meds. Went off Lexapro, onto something else for a year (long name which I forgot). That didn’t work for anxiety though. Back on Lexapro but only for a month or so because it was causing major anxiety. Now her GP has her on 5mg of Paxil and wants to increase that. Is that a good idea? I honestly can’t see how she can function being panicked 90% of waking hours. Paxil should help reduce panic. Talk therapy is probably helping bit by bit, but that will take a long time.
I thought her case was like another friend of mine who took a psycho-active med for the length of time it took to become functional (one for just two months) and get the therapy to overcome the acute clinical anxiety. Now after reading all this I now think her case is different. Her sister thinks she needs to drop all meds. Is her sister correct? I am here and her sister is far away, and my friend can’t function much of the day. The anxiety overwhelms all other thought processes. What can we do about this?
Ok, I talked with her some more and she said it was Zyprexa. She says “I should have stayed on the Lexapro, I was doing better”. Me: “you were getting worse”. Her: “I was getting six and a half hours sleep”. Me: “you were on Atavan”. Her (angry): “You are supposed to be positive”. Every now and then she says she should have stayed on the Zyprexa and then admits that wasn’t working either.
White matter lesions found on the MRI last week. There weren’t any last November. Using a video chat by someone who doesn’t know the patient to announce that finding is very poor policy. Needless to say it didn’t help with her anxiety. She immediately assumed she had been having “mini-strokes”. Otherwise reading here and watching her is like the short story Flowers for Algernon.
This week she sees the academic psychiatrist at a well-known local university. I have written two pages filled with medical history including most of the past two years of experiments. I am hoping they can use the information to get a head start on their own diagnosis and recommendations. I have no idea what they will recommend.
I think that mainly continuing with her current psychologist counseling for anxiety (rooted in health anxiety) will slowly improve her situation. For example she believes at times that she can’t walk because her legs and/or heart have gone bad, and therefore doesn’t walk and deteriorates. The last two cardiologists and a PA have said her heart is “fine” or “healthy”. Have to continue to press on in that direction.
Were the white matter lesions listed as hyperintensities in the MRI report? My new MRI listed scattered hyperintensities.
Sorry, I don’t know. The announcement was via video chat which I listened to, and I don’t recall them using that term. If there’s a written report I have not seen it.
The edict: 20 mg Paxil and specific therapy for illness anxiety. I asked them if they would use the Paxil as a means to get through therapy and then taper off. They said yes. In my mind, a year is optimistic even without any setbacks. They also insist in her specific case: no tests due to illness anxiety. That may apply to nobody else writing here and few people in general. But if you have that type of anxiety, consider avoiding medical tests including neurological.
research “niacinamide for anxiety” it will give you some valuable information and you can talk to her about trying it – it is a form of the B vitamin Niacin but does not have the flushing and other side effects that Niacin does. Therapeutic dose is 1500 mg. in am. and 1500mg later in the day but not at bedtime. Actually, Valium is a patented medication for anxiety that basically was chemically patterned after niacinamide plus what things they had to add to it to make it enough different to get it approved for a patent since niacinamide is a natural substance and cannot be patented. if she agrees to try it, have her start with 500 mg. morning and late afternoon and if it does not cause her gastric or any other problems up it gradually until she is taking the therapeutic dose. if she makes it to the highest dose, she would then have to add in a good B complex of 50 mg. twice a day also to balance out the B vitamins, since they are synergetic. It is a very cheap supplement and can be found on Vitacost.com for around $8 per month – that would be for two bottles, as at the therapeutic dose it would take two bottles a month. You can use the Vitacost brand and you would be fine. I wish her luck
I’m in the same boat as the author. Horrible APRN (not even a psychiatrist or physician) had me on 30mg of Lexapro that I had to go off cold turkey because of problems with scheduling an appointment with them. Ended up on a psych hold due to intense anxiety and paranoia.
My problems really started though when the APRN’s solution was to try and put me back on 10mg of Lexapro, I had to end it about a week in, and the APRN basically washed their hands of me, first saying they’d only treat me again if I saw a therapist, and then when I finally did, said that “we” decided to see somebody locally instead. The APRN lives out of state (used to live here), probably to avoid certain regulations.
My symptoms since October of last year have been brain fog, memory loss, numb emotions, trouble breathing, bad cough, sinus issues, ear ringing, neck/face nerve problems and pain, nausea, high blood pressure (my blood pressure is better now which makes me think maybe I had a slight case of serotonin syndrome), throbbing headaches, extreme fatigue (flushed, red face), dry mouth, and probably a ton of other stuff I can’t remember.
The symptoms that haven’t gone away at all are the numb emotions, face/neck problems, sinus problems, memory loss, and brain fog. I’d love to find out Lexapro didn’t cause this, and it was stress from other things in my life, but I’m pretty sure Lexapro caused it. It’s been a year of feeling like a cripple, and most of the doctors I’ve seen have been useless. The neurologist I saw completely dismissed notions of Lexapro causing this, and didn’t order any tests. Basically said “sorry you feel bad, good luck”.
If the author’s willing to help me and respond to me, I’d really appreciate it. I feel like some legal action could be taken here, since it was an APRN that lives out of state overdosing me with a non FDA approved dosage of Lexapro, and then abandoning me after a bad reaction to reinstating me on 10mg of Lexapro.
Thank you.
How is it possible that I only took this drug for merely 2 months for GAD, and yet I relate to everything you described here and you were on it for much much longer at 10+ years? Everything you said exactly described my current situation, I’m 3 months off of it now and I still can’t seem to return to normal yet.
Hi C F and everyone,
It is truly insane we found each other here, because I also took escitalopram for ~8 years starting age 21 (male). I quit 4 years ago and my brain has never been the same ever since… I legit feel handicapped mentally, as though part of my brain is missing. It’s tragic because albeit subjectively, I was a brilliant person.
Currently in my state, I am unable to handle stressors like a normal person. My cognitive function, organization, and coordination sharply declined and am showing signs of early dementia at the age of 33. I have a severely hard time controlling my emotions like anger and sadness.
All this to say that when I experienced these moments early in my adulthood pre-escitalopram, I was able to handle these issues without feeling like I’ve been traumatized every time like I do now.
I truly feel that I’ve been severely debilitated from this medication, and the fact that these corporations allow patients to take this long-term is truly.. ridiculous.
I wonder how long until the world finds out that we were all guinea pigs of these neurotoxic drugs, and whether people would remember us as victims as opposed to people with mental disorders. Because I can say with confidence, we would have all faired better if we never took these meds in the first place.
I will look into some neuropsychological assessments done as CF suggested. But the worst feeling currently is to know there is no way to save our damaged brain from these meds…
Thank you so much for sharing your experiences with the world. For 10 tot 11 years I took Escitalopram and, if necessary, Oxazepam 10mg. For the past 2 years I have become more and more convinced that I suffer from brain damage. Last year I completely stopped taking oxazepam from which the withdrawal lasted for 6 months. For 8-9 years I have taken 20 MG Escitalopram and the last 2 years I have continued to withdrawal to lower doses. From 5mg to at the moment: 1,25mg to 2.5mg. Unfortunately, I suffer from intense spams around my jaw. Not every day thankfully, but today it lasted around 5 hours. It is very tiring to deal with. I have also lived on 30% percent energy for years. As a result of this I could no longer work and often lay in bed for several years.
I have not done an MRI scan but did had that chance last year with my health insurance, but as I experienced more often, I felt that I was not taken seriously enough from the beginning and the specialist was already expressing his pessimism to be able to find something. I then let it go because it hurts again not to feel taken seriously enough. My blood test were fairly normal. I have to add that I took 2 overdoses in my life a few years ago but I’m no longer suicidal.
I feel that my chronic lack of energy has influenced these decisions in that time and have often felt over-stimulated in my brain.
I find the intense spasms (convulsions) difficult to deal with and I have also experienced countless of other unpleasant symptoms, but what especially influenced my life quality was the fatigue syndrome which unfortunately has never officially been confirmed. I hope my story adds something, to you or possibly for others. I’m going for full healing of my brain and believe in this.
Marjolein
I feel like I have brain damage too. I was on Lexapro for six years.
Also, for those interested in being evaluated for neurotoxicity I suggest finding a Neuropsychologist familiar with the condition.
You may also want to consider finding the original source of this medical text book chapter for additional information.
“Among commercial and industrial chemicals, cosmetics, food additives, pesticides, and medicinal drugs, there are more than 50,000 substances distributed. Of these, approximately 600 have standards set by Occupational Safety and Health Administra- tion (OSHA) and approximately 200 have been regulated for neurotoxic effects.1–3 The major categories of neurotoxic insults to the brain include: (1) heavy metals, (2) indus- trial toxins and solvents, (3) venom bites, stings, and plant poisons, (4) bacterial toxins, (5) addictive drugs such as opiates, and synthetic analgesics, (6) sedative hypnotic drugs, (7) antidepressants and antipsychotic drugs, (8) psychoactive drugs and stim- ulants, and (9) antineoplastic and immunosuppressive drugs.3 Any of these may pose neurotoxic effects that can incur cognitive impairment, especially with prolonged exposure. Accordingly, a systematic method of tracking cognitive changes is pertinent to clinical practice. As bedside neurologic examinations may be insufficient in tracking more subtle cognitive sequelae of neurotoxic exposure, extended neurocognitive testing is proposed to better understand individual clinical presentation.
CLINICAL MANIFESTATIONS OF NEUROTOXICITY
There are two broad categories of neurotoxicity: neuropsychological impairments and elementary neurologic impairments.3 Neuropsychological impairments may include declines in attention/concentration, memory (especially short-term memory), executive functioning, processing speed, language, visuospatial skills, depression, and anxiety. Elementary neurologic presentations may include toxic neuropathies, myopathies, tremor, parkinsonism, myoclonus, dystonia, ballismus, and tics, to name a few.3
Given the myriad of possible symptom presentations, a formal neuropsychological test should be viewed as an extension of the neurologic examination. These tests are particularly useful in assessing for particular toxin-derived syndromes. Most patients with neurotoxicity present with impairments in the cognitive domains of attention, executive functioning, and memory.3 However, it has been documented that other clinical syndromes may be correlated with toxic exposure, further complicating the cognitive sequelae beyond that of a mechanism exclusive to acute neurotoxicity.“
https://pubmed.ncbi.nlm.nih.gov/21803211/
Hope you are doing at least somewhat better this year. I’d like to contact you and get advice on what to do for my own struggle with this.
Hi Christian,
I’m afraid I might have experienced the same thing as you have. Is there anyway I can contact you for more insight? Thank you.
Hi Christian,
We talked briefly before, but unfortunately I lost the email thread. Would you be able to reach out to me again? I’m struggling with similar issues and have another question. Thank you.
Every now and then I see my story being posted on social media expressing doubt on the validity that psych meds can cause the conditions and severity of what I was diagnosed with. So I am including this link so I can disappoint the doubters.
“Introduction
Subacute toxic encephalopathies are challenging to identify due to their often insidious tempo of evolution, nonspecific manifestations, relative infrequency as individual entities, and frequent lack of specific diagnostic testing. Yet they are crucial to recognize—in aggregate, subacute toxic encephalopathies are a common problem that can lead to severe, irreversible harm if not diagnosed and treated efficiently. This article reviews the clinically relevant aspects of some of the more important subacute toxic encephalopathy syndromes caused by inorganic toxins, carbon monoxide (CO), antibiotics, antineoplastic agents, and psychiatric medications.“
https://www.sciencedirect.com/science/article/pii/S073386192030058X
how are you doing today?
Wow, I took Lexapro since 2004. My brain is a mess. Like some others I need to find a doctor that agrees that Lexapro is responsible. I annot afford the costs of the tests either. I need help so very bad. Also, is there lawsuits against Lexapro, not that it will help me, I just want people to know about the serious damage Lexapro has done to me and so many more.
I was working for a managed care company when my supervisor told me that if I didn’t start taking an SSRI she would recommend that my position would be terminated. The reason for her suggestion is that I was working with a caseload of over 300 patients that had to be reviewed monthly under extreme pressure to get them off benefits. I was not a good fit for the job because I am too much of a patient advocate to have such a job which I long since left. Anyway, while I was still there, I started Lexapro. Some of the other nurses and social workers were also taking SSRI’s and they told me that you have to push through the initial side effects and in time they would subside. When I first started taking Lexapro, I felt like there were stick figures dancing around in my brain and my skin got a funny texture to it. Then, slowly but surely, I started gaining weight. I was always thin or average and became obese. I also started having severe nosebleeds and had to go to the ER via ambulance. I started seeing an integrative physician and she suggested that I taper off the Lexapro. I did. I’ve been off it since around 2013. But, my life has never been the same. I was once very active and now I suffer from hot and cold sweats, pain in all muscles, burning sensations, vertigo, balance issues and some autoimmune diseases. I don’t know if this is from the Lexapro but, after reading the above, it very well could be. So, the thing that I am trying now is Annie Hopper’s Lymbic system rebooting. I hope this works for me because I have not been told, by anyone, what else would stop this brain damage.
Hi
I took this SSRI – Escitalopram as well – but even worse, a cheap generic version of it for 13 months. Upon withdrawal – 8 weeks of debilitating symptoms and I have never been the same since. For the last 4 years since coming off – brain fog, fibro symptoms, pain, inability to function properly. I have no money to get fancy tests done to prove damage and I live in a 3rd world country. It’s terrible.
hey if you wanna talk im also injured I have the same symptoms as you from antidepressants you can email me at lydrooney@protonmail.com
I am really really suffering from the effect of Lexapro. No issues for a while – went from 10 mg to 5 mg. Then 5 mg to 2.5 every other day. Then tried to go to zero and totally F****me up. So I went back to 5 mg but STILL my brain feels full of pressure, I don’t feel well, I always feel lightheaded. I get panic attacks from not taking it because my brain feels so off. I just want to feel better.
Hey Lisa, have you improved by any chance ?
I really need a neuro who did the scans and test like CF. Please share with me any neurologists i could turn to for help and answers
I use medications but I also have hormonal problems due to a premature menopause ? Do more women here have hormonal problems. I think this can also cause some of these symptoms.
You need growth hormone to increase your healing, read up on healing braindamage with hGH.
Hello I got the same symptoms you have after ssri use. Im now 4 months off and my memory and sense of time is terrible.
Do you also have visual snow?
And the symptoms did they come gradual?
Can you please reply.
This is also a good article that is good evidence of what happened to me and maybe some of you. It links to studies and scientific data.
https://www.karger.com/Article/FullText/447034
This article comfirmed all psych Meds cause mitochondrial Damage including all the conditions I was diagnosed with.
https://www.ncbi.nlm.nih.gov/m/pubmed/18626887/
Ok I will post one more. Here is a a compiled article of multiple antidepressant induced dementia studies. It’s rather convincing. There are many other studies verifying SSRI induced dementia. All of which prescribing doctors will deny.
https://www.hindawi.com/journals/bn/2018/5315098/
Maybe it is the condition that is treated with SSRI’s that gives a higher change at developing dementia.
No, that is not it. The pharmaceuticals cause damage.
I was criticized on a website that I did not link my injury to scientific evidence that SSRIs can cause brain damage. There is a lot of info online that is legit and not “ghost written” by pharma or a paid off doctor. Such as this article that is probably best piece of info proving all my damage. It’s on the reliable NIH.gov website who is known to frown on pharma written articles. Also google SSRI induced dementia or medication induced mitochondrial Damage and much more will appear. Look up DrGrace Jackson’s book Drug Induced Dementia that links SSRIs to brain and Miri damage through brain scans and testing references and prior published research.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3334530/
Wow
Who performed these tests for you? I suspect I am suffering from lexapro neurotoxicity and like the others I would like to prove it. Thank you
I am considering taking Lexapro and am wondering if you ever tried weaning off of the medication during the years that you took it?
Weaning off of it? Did you read the story, I have a brain injury from taking it. If you are considering taking it you missed the entire point of this story. Good luck.
Why isn’t the name of the author/injured patients name noted anywhere? I fully, 100% believe all of it. I hope you sued the manufacturer and every doctor who pushed it on you over the years. Do no harm. Period.
Hello, I have the same symptoms and the same Image on the spect scan.
main was started after use of marijuana, three years ago. can you contact me somehow? maybe on facebook?
I would like to hear about your prognosis, and whether there is any improvement or not.
my name is oren gavish. ty
Hi C.F. I was on Lexapro for 10 years and Identify a lot with your story. I’m sure I have brain damage I just don’t know to what extent. I’m a writer and putting an article together has become next to impossible. (I’ve had to request help) Also I have most of the symptoms Kary Smith points out. I’d please like to ask you a couple of things. Where could I message you?
Hello Cf I am in the same boat, how did you manage to get disability since antidepressant long term side effects are not aknowledged at all by conventional medecine? Also Qeeg are not aknowledged by doctors here in France. Thanks for your reply….
I, too, would like to know what doctor or specialist did these studies and attributed the damage to the drug. I’ve suffered severely and have been disabled by Zoloft since 2001. MRIs show lesions. I have been diagnosed with all sorts of physical disorders and diseases, but no 2 doctors agree A few doctors have very subtly hinted that the drugs are the problem, but none will really follow up on it. I suspect they don’t want to be involved in a potentially litigious or messy case. The Cleveland clinic brain center turned me away as a patient when I gave a bit of my history.
I’m down to 75lbs and bedridden.
Thanks for sharing your story.
I am suffering from neurotoxicity due mainly to the benzodiazepine Klonopin. I took this medication as prescribed for 16 years. I want to know what type of dr eventually got you to these tests. I have seen multiple specialists in the past few years. I suffer from terrible cognitive impairment and emotional deregulation with violent panic attacks and trauma due to iatragenic injury. I am currently on SSDI for psychiatric illness that is actually trauma and neurotoxicity based. I am a single mom. I want these tests so I can prove what I have known for quite some time. How do I find the right specialist? Would it be a neuropsychiatrist? I’m lost in my search…
I will message you directly.
Could you please message me? Ive been on ssris for 22 years…even going down 1mg a month triggers horrible insomnia, anxiety, ocd….just desperate…im on disability…
Would you message me also about where you had your testing done please? I am desperate for answers. Thank you
Knutsent@aol.com
Can you message me I have been suffering with the same symptoms
did you get an answer? same symptoms..
Any improvement
Another example of drugs going wrong and doctors unwilling to admit (or even recognize) when this happens. When you speak with family and friends, stories begin to surface, people having the same exact experiences with drugs and the medical community’s lack of understanding when it comes to adverse drug reactions–how doctors use gaslighting as a form of silencing their patients’ concerns. It’s very sad, I’ve been there–but it’s good to know that at least we, the patients, and certain doctors and researchers know just how potentially dangerous medications can be.
Thanks for putting your story and your travails out there, CF.
This is yet another page in the Mad Mad Mad World of the druggies writing chapter after chapter of our world out of sync — those white lab coat wearing, PhD and MD bearing, know all/know nothing men and women foisting drug after drug onto a Western Culture that precipitate a culture that is so out of balance; all the way down to the family unit we have nowhere, seemingly, to run but to the drug store and managed for-profit medical delivery system for help.
I am quoting you kind sir to ramify my points:
“One year ago, I was living the American dream, a father of two young sons, active, social, traveling sales person. All of that was taken away from me because of a pill. I never had any history of mental illness or even anxiety for that matter. I “sold myself to the devil” as they say by taking a medication that I was told would help me with some fears with public speaking. I am now paying the price for that decision.
….
I went to see the psych for only three weeks but he changed the course of my life with just a couple of strokes of a a pen on a piece of paper. This doctor prescribed a pill. A pill that many say “re-wires” the brain. The medication he suggested was Lexapro. I had never heard of Lexapro, but back in 2001, anti-depressants were taking off. You may recall the TV series, The Sopranos. It was a hit cable series that featured characters that as soon as anyone had any issue pop up, the doctor prescribed an antidepressant. It seemed to me that they were making a joke of the concept that everyone on the show needed a medication to function.
In 2003, during the peak of that wave, I started Lexapro. Within weeks, I was transformed into someone who feared nothing. Everything became much easier for me. I could present to large audiences. My fear of flying disappeared. My career took off. I became even more social, feeling confident in any setting. I enjoyed being the center of attention. I then started making changes in my life. I got divorced. At the time, I felt that I did not need to put up with anything if I didn’t want to. It was hard, as I had two young sons, but I felt it was the right move for me at the time. Looking back it was a cold move (and I handled it poorly) but I was laser focused on what I wanted to do. I became much more comfortable and flirtatious with women (not in an obnoxious way). At the time, I wanted to be free. In so many ways, in my mind, I was an improved person. It wasn’t until the last year that I realized how wrong I was. I took Lexapro for 15 years. I never looked back. Until now.”
###
Wow is all I can say, and, unfortunately, I’ve been a teacher since 1983 who has seen so many fine people suffer GAD, general anxiety disorder, fear of presentations, and panic and severe depression — at colleges, universities, alternative high schools, military bases, prisons, refugee centers, retirement facilities, day centers for memory care patients and those living with developmental disabilities.
Your story is not unusual, and many people grab prescribed and other chemicals and other systems of coping to cope. Man, how the drug industry and the medical industry are nefarious, cold, and they too are stealth and focused: money-money-profits-profits at all and any costs!
Here, lawsuits against the manufacturer of Lexapro. Mothers, no less, tied to birth defects!
Lexapro was given a grade C by the Food and Drug Administration for its level of safety when used during pregnancy. Research shows that the drug had adverse effects on the reproduction of the animals being tested. Though the medication may be harmful to the fetus, the benefits of its usage may outweigh the risks therefore allowing approval for use in expecting mothers.
Mothers of children born with birth defects have filed numerous lawsuits against Forest Labs for the injuries as well as the failure to alert users of these potential risks. In one case in St. Louis, Missouri, in which three mothers filed Lexapro lawsuits, the mothers argue that if they had been aware of these potential side effects that they would not have taken the medication and would have chosen a safer alternative.
Birth defects caused by Lexapro include:
Persistent Pulmonary Hypertension of Newborns (PPHN) – PPHN is one of the most life threatening side effects of the birth defects. PPHN affects a newborns heart and lungs by causing difficulty adapting and breathing outside of the womb. Infants born with this condition are often admitted into intensive care and require supported ventilation and heightened supervision.
Cleft Palette and/or Cleft Lip – Cleft palette is occurs when the body’s natural structure does not properly fuse together while in the womb. There then becomes a gap that can often be surgically corrected but otherwise requires special care and attention. Cleft palates can lead to speech impairment, difficulty breathing and ear infections and hearing problems.
Heart Defects – The use of any SSRI imposes a heightened risk of heart defects in newborns however, expectant mothers that are prescribed Lexapro are at nearly double the risk of obtaining heart defects including, but not limited to, atrial septal defect, hypoplastic heart syndromes, tetralogy of fallot and transposition of the great arteries.
Neural Tube Defects – Fetuses exposed to Lexapro while in the womb are at twice the risk of obtaining anencephaly, a neural tube defect. Anencephaly is a fatal disorder characterized by the absence of a large portion of the brain and skull.
These defects are among several others including limb defects, spina bifida and cranial defects. Mothers should be aware that the chemicals in Lexapro can travel through the placenta and the use of this drug puts themselves and their unborn child at risk of defect or even death. Expecting mothers should consider their health as well as that of their child and contact a physician about possible alternative medications.
https://www.drugdangers.com/ssri/lexapro/lawsuit.htm
Thousands of payouts for violence, murder and suicides attributed to SSRI’s like Lexapro.
Amazing, if we go down the Physicians’ Desk Reference (PDR) of all the drugs, and then do a Google and LexisNexis search on lawsuits and injuries tied to those drugs. Again, the cure is worse than the disease is the unfortunate reality of so much in our society tied to not only health, but other aspects fueling the engines of capitalism.
Unintended consequences. Tipping Points. Lag Time. The Tragedy of the Commons. Your story is so linked to what does go wrong in our First World Developed Society, from the individual in society to the society in the culture, to the culture in the world.
Thanks for your stories.