Over the last several weeks, I have been preparing a report regarding our research on birth control and blood clots. In doing so, I have been reviewing past work and stumbled upon my notes for the presentation that landed the grant allowing this research to begin. The talk was filmed, but the video is behind a paywall. So, I decided to post the notes and the presentation. Enjoy.
Birth Control, Big Money and Bad Medicine: A Deadly Trifecta in Women’s Health
As I considered how to put this presentation together, I struggled with where to begin, what to leave in, what to leave out. There is so much that needs to be understood about contraceptives that we could fill a week of lectures and discussions. What I kept coming back to, however, is the notion that if I can teach you how to think about contraceptives, or for that matter, any medical treatment, if I can teach you how to question and evaluate the research, how to find the answers that you need; if I can give you a foundation and a framework for understanding the science, the economics and the politics of this medication, then each of you can find your own answers, and perhaps, if you are so inclined, contribute back to the knowledge base, so that we all have a better understanding of these issues. And so it is from that perspective that I have decided to approach this discussion. I want to give you a foundation and a framework from which to build your own house of knowledge. Sounds a little corny, doesn’t it, but bear with me, learning how to think critically about medical science might just save your life or the life of a loved one.
The Framework of Knowledge
I have a background and a natural inclination towards philosophy. In other words, I tend to think about things a bit more deeply than perhaps I should. This gets me into trouble sometimes.
One of the questions that plague my thinking is ‘how we know what we think we know’. I find that more often not, pondering from where and from whom the knowledge, the science, the politics, even the historical interpretations come from, tells us a lot about what it is we know exactly and what we really have no business claiming knowledge of.
With hormonal contraceptives, and indeed, the entirety of women’s health, when we deconstruct what is known and detach it from how we know it, or at least how we think we know it, it becomes very clear, very quickly, that our knowledge is severely limited.
For example, did you know that most of the science on contraceptives was developed over 50 years ago before the thalidomide tragedies changed FDA regulations regarding women’s health? Did you know that after thalidomide, research involving women of childbearing potential was all but prohibited until the late 1990s?
The post-thalidomide regulations, when combined with the political quagmire that is female reproduction, all but eliminated research and development on hormonal contraceptives, with the large pharmaceutical industries preferring to make only slight changes to dosage or delivery method and focus almost entirely market saturation over all else.
Probably not, unless you study this stuff. But knowing this, understanding how we know what we know about hormonal contraceptives can tell us a lot about these products, even if you don’t know the science.
So, hormonal contraceptives didn’t get the safety research they deserved. Indeed, they did not and continue not to because of the perceived economic and political costs associated with contraceptive science is greater than the perceived benefits.
Why fund new science, when the old science is already approved and the market is mature, in the sense that women and physicians alike consider hormonal contraceptives safe, but more importantly, a necessary component of reproductive health?
The Objectivity Bias
Back to the topic of how we know what we know, not only do we have to consider the science behind these drugs, but we also must consider in what context the science emerged and whether and how that context introduces a bias that impedes our understanding.
I would argue that bias is inevitable, even fundamental to the scientific endeavor, even though we claim objectivity. Consider, for example, the process of research design. What questions are asked and not asked are dependent entirely on the researcher’s individual constructs about what the problem is. Defining the problem, or even whether there is a problem to be investigated, is informed by education, culture, society, advertising, marketing, and in more modern times, by research funding availability. In many ways, bias permeates every aspect of the scientific endeavor. And yet, we hold tightly to this notion that delineating science from every other pursuit of knowledge, is its objectivity, its lack of bias.
In science, in particular, we have exalted the notion of objectivity above all else. The experiments we do are meant to eliminate subjectivity, to eliminate chance and the variables that might confound our data so that we can say with some confidence that this or that treatment is safe and effective.
While these are laudable goals that have contributed largely to the great advancements we have in all fields of science and technology, I think, in some ways, we have taken this reliance on objectivity too far, so much so that we have lost the humanity, and indeed, the humility in our scientific endeavors. This fealty to what I would argue is a contrived reliance of objectivity, to controlled but abstracted data calculations, not only severely limits the scope of our understanding but also poses real risks to human and organismal health. We see evidence of this every day, when human illness mediated by a particular drug or environmental toxicant is viewed only in terms of averages. That is, when a drug evokes a reaction in only small fraction of those who use the medication, but appears not evoke that reaction in others (though I would argue that it evokes other reactions that we are simply not recognizing), then those reactions, those costs, are viewed as inconsequential. They are not statistically significant and because we forget that statistical significance is different that clinical significance, because supplant statistical significance, a mathematical abstraction for clinical and human significance, we fail to recognize the dangers of a particular medication.
And so when I approach medical science, or really anything, it is always with those two things in mind – how we know what we think we know, and how biases, mine and others, influence that knowledge. It is from that perspective, we’ll take our foray into the contraceptive conundrum.
My Biases
Because I believe biases are so important – let’s begin with my biases. We’ll then look at the biases in modern medicine and statistics and how those biases have informed how we know what we know about hormonal contraceptives. Finally, we’ll tackle what is known and what is not known about what hormonal contraceptives do and do not do to the body.
You already know a little about me from the bio I submitted and from the brief introduction. But let me insert myself into the research, give you some idea of the lens through which I understand medical research in general, and hormonal contraceptives, in particular. I stand here today as a woman who has used oral contraceptives and experienced side effects from them (but at the time had no clue about the connections between my health issues and the contraceptives, nor did any of the physicians I sought help from).
I am mom of 21 year old twins, a wife of 26 years and a lifelong jock (even at the ripe old age).
I am as a research scientist. I love figuring out how things work, and to me, figuring out how things work means not only going to down to the smallest possible unit of function – the molecule, the chemical pathways, but mapping the systems involved, not just of the target organ but across the entire body. I think I was an engineer in a former life.
I am writer, as I mentioned, with philosophical tendencies.
I am business owner, whose business involves understanding women’s health and healthcare.
Finally, I am fierce women’s health advocate. For too long, questions about women’s health have been ignored. I want to change that.
I should also mention, as someone who is involved in medication adverse events research, listening to patient stories, seeing the devastation that some of these medications can evoke, and then investigating the mechanisms by which these reactions can occur, I have become increasingly wary of pharmaceutical promises. Admittedly, in that regard, I am probably more biased than others. It is difficult not to be.
So it is this totality of experiences that color, not only my interpretation of data, but I think more importantly, the questions I ask about any given medication. When I look at the safety and efficacy of a drug, I want to know in real terms what the benefits versus the risks are to an individual.
Unfortunately, we don’t have that information for majority of medications on the market, especially for women, and most especially for hormonal contraceptives.
With that long introduction, let’s dig into the topic at hand.
Birth Control, Big Money and Bad Medicine: A Deadly Trifecta in Women’s Health from Hormones Matter
Add Your Experience to the Conversation
As a result of this presentation, we were awarded a grant to investigate the health risks associated with hormonal contraceptives. Some of the early results of the pilot study can be found here and here. You can help us delineate those risks further by adding your experiences to our growing database by taking part in the Real Risk Study and, if you are so inclined, sharing your health story on Hormones Matter.
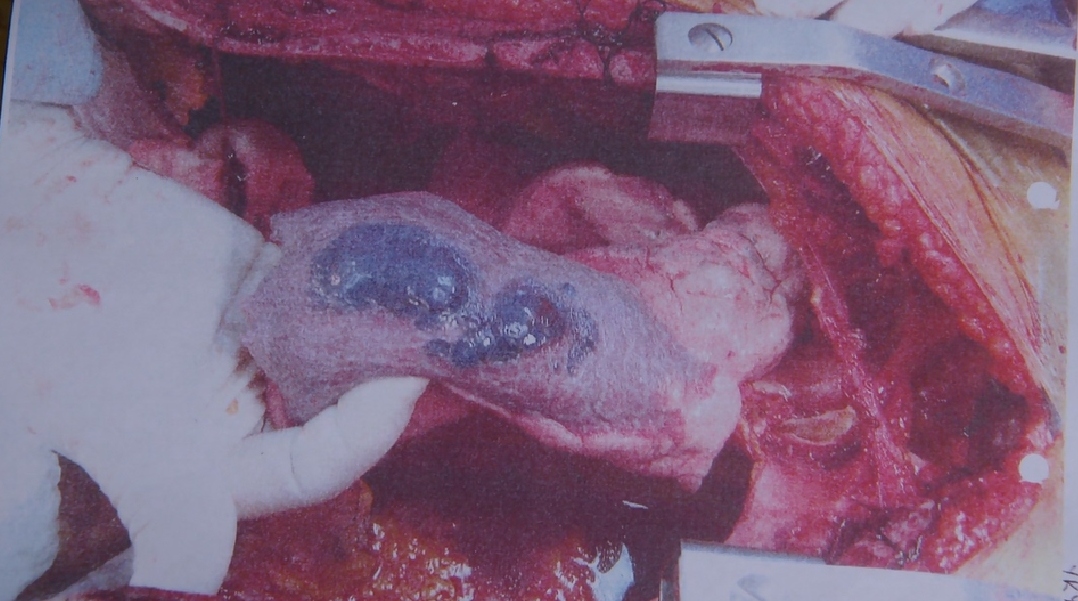
Real Risk Study: Birth Control and Blood Clots
Lucine Health Sciences and Hormones Matter are conducting research to investigate the relationship between hormonal birth control and blood clots. If you or a loved one have suffered from a blood clot while using hormonal birth control, please consider participating. We are also looking for participants who have been using hormonal birth control for at least one year and have NOT had a blood clot, as well as women who have NEVER used hormonal birth control. For more information or to participate, click here.