In a sense, my complicated health history began a decade before I was born. In 1951, on a chilly pre-dawn morning in Nevada, my father-to-be crouched in a trench with his Army comrades and shielded his eyes with his hands. Moments later, an atomic blast was detonated with a light so brilliant that he could see the bones in his hands through his eyelids, like an x-ray. The soldiers were marched to ground zero within an hour, exposing them to massive amounts of radiation. My father suffered many physical issues and died of chronic lymphocytic leukemia at 61 – a far younger age than usual with this disease.
Many of the soldiers exposed to atomic tests and military radiation cleanup efforts paid dearly with their health, and the legacy was passed on to their offspring in the form of miscarriages, stillbirths, deformities, retardation, childhood cancers, and chronic health issues. I never wanted children, in part because I was concerned that my own genes were affected by my father’s radiation exposure.
Early Markers of Ill Health
Physically, I didn’t feel right as a child. I had mononucleosis as a baby and needed a prednisone shot to get well. I was sick often and lacked stamina. I had mono again in high school and relapsed in college.
I fared well as a young adult, but then hit a wall in my mid-30s when I suddenly became chronically ill with digestive issues, insomnia, brain fog, and fatigue. A hair test revealed off-the-charts mercury poisoning, so I had ten fillings replaced and detoxed. All my hormone levels crashed, so I went on bioidentical hormone replacement therapy for a time. I recovered quickly but adrenal and thyroid hormone support were still necessary. I even fared poorly with the ACTH cortisol stimulation test to assess for adrenal insufficiency (“adrenal disease” beyond so-called “adrenal fatigue”).
In 2001, a DEXA scan revealed I had osteopenia at just 40 years old and I tested positive for elevated gliadin antibodies, a marker for celiac disease, the likely cause of the bone thinning. I went gluten-free and began lifting weights – thankfully, my bone density resolved. I shifted away from a vegetarian diet and gained muscle mass and energy.
Over the next several years, I had bouts of “gut infections,” resolving them with herbal antimicrobials. About a decade ago, the dysbiosis flares became more frequent and difficult to resolve. I tested positive again for mercury. This time I did the Cutler frequent-dose-chelation protocol and reduced my mercury burden to within normal levels according to hair tests.
A Labyrinth of Health Issues
My health issues were becoming more numerous, complex, and difficult to manage as I grew older. Besides the persistent sleep and digestion issues, I often had fatigue, pain, bladder pain, urinary frequency, restless legs, migraines, Raynaud’s, chilblains, and more. Managing all these symptoms was a real juggling act and rare was the day that I felt right.
As I searched for answers, I turned to genetic testing, starting with Amy Yasko’s DNA Nutrigenomic panel in 2012 and then 23andMe in 2013 to learn which “SNPs” (single nucleotide polymorphisms) I have. A Yasko-oriented practitioner helped me navigate the complexities of the nutrigenomics approach – that is, using nutrition with genetic issues.
I learned that genes drive enzymes that do all the myriad tasks to run our bodies (which don’t just function automatically), and that certain vitamins and minerals are required to assist the enzymes, as specific “cofactors.” Genetic SNPs require even more nutritional support than is normal to help enzymes function better. So my focus shifted toward using basic vitamins and minerals to support my genetic impairments. I now understood that I needed extra B12, folate, glutathione, and more. I began following Ben Lynch’s work in elucidating the MTHFR genetic issue, as I had MTHFR A1298C.
Also in 2013, given my struggle with diarrhea, I was diagnosed with microscopic colitis via a biopsy with colonoscopy. In 2014, I learned about small intestinal bacterial overgrowth (SIBO), which gave me a more specific understanding of my “gut infections,” and tested positive for methane SIBO. I worked with a SIBO-oriented practitioner on specific herbal treatments with some short-lived success.
At the end of 2014, I learned that I have Ehlers Danlos Syndrome (EDS, Hypermobile Type), confirmed by a specialist. I came to understand that my “bendiness” likely had implications in terms of chronic illness, and I saw my bunion and carpal tunnel surgeries in a new context, as part of this syndrome.
Even with these breakthroughs in understanding, I still relentlessly searched deeper for root causes.
Genetic Kinetics
In 2018, Ben Lynch published Dirty Genes, focusing on a number of common yet impactful SNPs.
I learned that I had NEARLY ALL of these SNPs – NEARLY ALL as “doubles” and even a “deletion.” (Deletions are worse than doubles; doubles are worse than singles.) Researching further, I had doubles in many related genes with added interactive impacts. Typically people might have just a few of these SNPs.
Understanding my “dirty gene” SNPs revealed that I could be deficient in methylation, detoxification, choline synthesis, nitric oxide synthesis, neurotransmitter processing, and histamine processing. Each of these SNPs could potentially impact sleep, digestion, and much more in numerous ways. Now I potentially had a myriad of root causes.
Lynch warns people to clean up their health act before supplementing the cofactors, whereas I’d cleaned mine up years prior. Sadly, I found only limited improvements in adding his nutritional protocol. Suffice it to say I felt rather overwhelmed and disheartened.
But at the same time, I gained vital and necessary insights. I now understood why I had mercury poisoning twice: detox impairments. I understood why I had Raynaud’s, chilblains, and poor circulation: nitric oxide impairments. My migraines could be histamine overload. I needed high levels of choline for the PEMT gene to prevent fatty liver disease and SAMe for the COMT gene. Much was yet still unexplained. So I relentlessly soldiered on, following every lead, clue, and a new piece of information.
Later in 2018, a friend who also has EDS encouraged me to learn about Mast Cell Activation Syndrome (MCAS), as many with EDS also have this condition. A few weeks later, I had a three-day flare of many issues, which prompted me to delve into the MCAS world, which was just as complex as the genetic approach. In working with an MCAS specialist, I honed in on three supplements, quercetin, palmitoylethanolamide, and luteolin, to help stabilize mast cells, which improved my bladder pain, bone pain, migraines, fatigue, and generalized pain. This was the culmination of months of research and work. All of this points to further genetic involvement, even though I lack specifics.
Downward Spiral
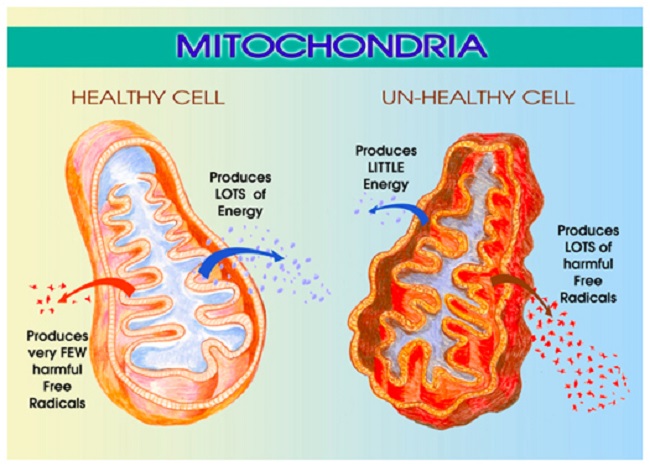
Twenty-nineteen brought further insights. I integrated circadian rhythm entrainment work. I tried a low-sulfur diet, suspecting hydrogen sulfide SIBO, which made me feel worse; and I began taking dietary oxalates somewhat more seriously after testing positive on a Great Plains OAT test. I did glyphosate and toxicity testing, which provided a picture of my toxic load. Testing also indicated high oxidative stress and mitochondrial issues (very interrelated). Hair Tissue Mineral Analysis (HTMA) testing, with the assistance of a specialist, helped me understand my mineral status and to begin rebalancing and repleting.
In 2020, I took a hiatus from all this effort, during which time I turned my attention towards personal matters, but 2021 has been a doozy in redoubling my health efforts. My digestion had worsened, so I focused on this area. I learned about sucrase-isomaltase deficiency, a lack of certain enzymes to digest sucrose and starch. I hadn’t tolerated sugar and starch for years, and I found I had a SNP for this condition. In January, a zero-carb trial diet helped me feel much better, so I continued. I tested positive for hydrogen sulfide SIBO, and I wrestled with this “whole-other-SIBO-beast” – in February trying again the low-sulfur diet and again feeling worse. Combining the zero-starch and low-sulfur diets left few options. Despite all my best efforts, I experienced a downward spiral with a loss of appetite, nausea, and vomiting every few days.
Discovering Thiamine
Around this time, I read an article about low thiamine (Vitamin B1) lowering intracellular potassium – I had been trying unsuccessfully to raise my potassium level in my HTMA work. I began following author Elliot Overton’s articles and videos on thiamine deficiency and oxalates. I was finally persuaded to take oxalates seriously. I then read the definitive book “Thiamine Deficiency Disease, Dysautonomia, and High Calorie Malnutrition” by Drs. Derrick Lonsdale and Chandler Marrs. I learned how B1 was key in many processes involving energy, digestion, and much more. I found that I had multiple SNPs in the B1-dependent transketolase gene, which is pivotal in several pathways. I gained some understanding of how all this related to some of my other genetic impairments, and why I might need high dose thiamine to overcome some issues.
All this was quite a revelation for me. It fit perfectly with my emphasis on vitamins and minerals to assist genes…but why hadn’t I learned of B1’s significance sooner?
In early March, I began my thiamine odyssey with 100 mg of thiamine HCL, upping the dose every couple of days. At 300mg HCL, I added 50 mg of TTFD, a more potent and bioavailable form of B1, then continued to up the TTFD dose every few days.
Similar to my experience with other vitamins, I was able to proceed rather quickly in dose increases. Many other people are not so fortunate and must go much more slowly. I already had in place most of thiamine’s cofactors (such as glutathione, other B vitamins, and methylation support) – so perhaps this helped me proceed more readily. Without these cofactors, peoples’ thiamine efforts often fail.
Magnesium is one of the most important thiamine cofactors, and for me, the most challenging. My gut cannot handle it, so I must apply it transdermally two or more times a day. At times, I had what I interpreted as low magnesium symptoms: racing and skipping heart, but these resolved as I continued.
Additionally, one must be prepared for “paradoxical reactions.” Worse-before-better symptoms hit me the day after thiamine dose increases: gut pain, sour stomach, headache, fatigue, and soreness.
My symptoms improved as I increased the dosing. When I added 180 mg of benfotiamine early on, my bit of peripheral neuropathy immediately cleared. This form of B1 helps nerve issues. As I increased my thiamine dosing, the nausea abated, my appetite came roaring back, and gastritis disappeared. Diarrhea, fatigue, and restless legs improved. I was able to jog again. My digestion improved without trying to address the SIBO and inflammation directly; the strict keto and low oxalate diets may have also helped.
In June, I attained a whopping TTFD dose of 1500 mg but did not experience further resolution beyond 1200mg, so I dropped back down. At 1200mg for a month, a Genova NutrEval test revealed that I was not keeping pace with TTFD’s needed cofactors, especially glutathione and its substrates. Not too surprising, given my malabsorption issues and my already high need for these nutrients. I dropped the TTFD to 300 mg, but quickly experienced fatigue. I’m now at 750 mg, which is still a large dose, and clearly, there is more to my situation than thiamine can address. I still have diarrhea and insomnia, and continue working to address these.
The Next Chapter
With TTFD, its cofactors, and my new gains in place, I’ve turned my attention towards a duo of genetic deletions that I have in GPX1 (glutathione peroxidase 1, one of Lynch’s dirty genes) and CAT (catalase). Both of these enzymes break down hydrogen peroxide (H2O2), a byproduct of numerous bodily processes. This unfortunate double-whammy causes me a build-up of damaging H2O2 and lipid peroxides – in other words, oxidative stress, a major factor in mitochondrial impairment, many diseases, and aging. This might be one of my biggest and yet-unaddressed issues, and I am digging deep into the published medical literature. This new chapter is currently unfolding.
I believe these two deletions are related to my father’s radiation exposure, for reasons beyond the scope of this article. But what about all the other SNPs? Many questions remain unanswered.
All my gains have been so hard-won, involving much research, effort, and supplementation. Yet what other options do I have, besides playing whack-a-mole and spiraling downward? Looking back, my improvements have been substantial, given the multitude of issues I’ve had to deal with. Perhaps now at 60, my life can start to open again to more than just self-care.
I hate to think of where I would be now, had I never come across the thiamine deficiency issue. I believe a number of factors had driven my thiamine status dangerously low earlier this year, such as malabsorption, oxidative stress, and hydrogen sulfide SIBO. I’m forever grateful to Lonsdale, Marrs, and Overton for their invaluable thiamine work that helped guide me back from the brink, and to the numerous doctors and practitioners who have helped me get this far. Perhaps my story can help others struggling with chronic health issues.
We Need Your Help
More people than ever are reading Hormones Matter, a testament to the need for independent voices in health and medicine. We are not funded and accept limited advertising. Unlike many health sites, we don’t force you to purchase a subscription. We believe health information should be open to all. If you read Hormones Matter, like it, please help support it. Contribute now.
Yes, I would like to support Hormones Matter.
This article was published originally on September 23, 2021.












Thank you so very much for sharing your story. You have one more comrade cheering you on.
Phosphorus deficiency, thiamine deficiency, magnesium deficiency, potassium deficiency are most common in refeeding syndrome.
Choline(Phosphatydylcholine), ATP, ADP, AMP, and Creatine Phosphate within the cell can be depleted by the enzyme AMP deaminase and turned into uric acid by XanthineOxidase, which means intracellular energy deficiency and metabolic syndrome.
Uric Acid must be below 5 mg/dl, better 4 1920, 3.5 was average.today the false normal is below 7.
5.5 or above means metabolic syndrome.
On YouTube channel Low Carb Down Under are 3 videos from Dr.Richard Johnson, which explain very precisely the metabolism of energy depletion,(polyol pathway) and how to prevent it.
Don’t drink fruit juice
Drink enough water , fix leaky gut, (can mimic dehydration and switch to polyol pathway)
Reduce salt
No dried fruit
Reduce glucose and insulin (eventually Berberine)
Try Magnesium Phosphate 47 essentials from Austria, enough vit D is required to take in phosphorus
Good luck
I have hEDS and similar issues and cured my horrendous insomnia by blocking ALL blue light after sundown. Either by having no artificial light on or around me or by wearing totally blue blocking glasses (orange lensed ones Blublox are good). Also getting as much natural sunlight as possible especially in the morning and noon. I was lying awake for hours and then falling asleep at 9pm! Just from wearing the blue light blocking glasses and avoiding ALL artificial light. It sounds too good to be true but it was miraculous. Increasing melatonin always a good thing too! Master antioxidant!
As I have indicated in many posts on this forum, I truly believe that lack of cellular energy, particularly in brain, is the key to understanding disease. That is why thiamine deficiency causes the well known (but largely ignored) disease known as beriberi (translation, I can’t, I can’t, severe fatigue is a salient symptom). In its early stages, it affects the autonomic nervous system ((dysautonomia) and in this stage it exactly imitates most diseases. If this polysymptomatic stage is recognized, treatment is easy, even if there are SNPs. Epigenetics is a relatively new science. Ignore these symptoms and the cellular damage becomes irreversible or demanding of high dose vitamin
Glad this was helpful for you, Andrew.
Can not begin to explain how your journey parallels mine. Thank you for your insights.